Case Report - (2025) Volume 10, Issue 2
Venoarterial Extracorporeal Membrane Oxygenation (VA ECMO) Protected Percutaneous Coronary Intervention (PCI) in Multivessel Disease with Severe Mitral Regurgitation (MR) Ischaemic Cardiomyopathy
Received Date: Apr 08, 2025 / Accepted Date: May 02, 2025 / Published Date: May 08, 2025
Copyright: ©Â©2025 Anand R Shenoy. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Shenoy, A. R. (2025). Venoarterial Extracorporeal Membrane Oxygenation (VA ECMO) Protected Percutaneous Coronary Intervention (PCI) in Multivessel Disease with Severe Mitral Regurgitation (MR) Ischaemic Cardiomyopathy. Cardio Open, 10(2), 01-04.
Abstract
Percutaneous coronary intervention (PCI) or coronary artery bypass graft (CABG) are two methods for revascularizing complicated coronary artery disease, which includes multivessel coronary artery disease, left main stenosis, bifurcation stenosis, and chronic total occlusion (CTO). Patient features, the presence of comorbidities, such as diabetes, LV dysfunction, hemodynamic state, and coronary lesion complexity (by SYNTAX score), should all be considered when deciding whether to revascularize via CABG or PCI. High- risk PCI is being done more often in complicated coronary artery disease with a high risk of periprocedural cardiogenic shock because of higher surgical risk scores and comorbidities in ageing populations. For elective high-risk PCI, mechanical circulatory support (MCS) devices can offer hemodynamic support, averting hemodynamic failure. An intra-aortic balloon pump (IABP) and a coaxial left cardiac support device (Impella device (Abiomed, Danvers, USA)) have been used in a number of trials, however the results have not clearly demonstrated any advantages for IABP. Impella demonstrated certain benefits due to its greater hemodynamic support. An alternative to mechanical support alternatives for patients with possible or current circulation failure is venoarterial extracorporeal membrane oxygenation (VA-ECMO), which offers more comprehensive haemodynamic support. ECMO has the additional benefits of right ventricular unloading and blood oxygenation as compared to IABP and Impella. Therefore, herewith, we report a case of high-risk PCI which we performed under the protection of VA-ECMO.
Introduction
Percutaneous coronary intervention (PCI) or coronary artery bypass graft (CABG) are two methods for revascularizing complicated coronary artery disease, which includes multivessel coronary artery disease, left main stenosis, bifurcation stenosis, and chronic total occlusion (CTO). Patient features, the presence of comorbidities, such as diabetes, LV dysfunction, hemodynamic state, and coronary lesion complexity (by SYNTAX score), should all be considered when deciding whether to revascularize via CABG or PCI. High- risk PCI is being done more often in complicated coronary artery disease with a high risk of periprocedural cardiogenic shock because of higher surgical risk scores and comorbidities in ageing populations. For elective high-risk PCI, mechanical circulatory support (MCS) devices can offer hemodynamic support, averting hemodynamic failure. An intra-aortic balloon pump (IABP) and a coaxial left cardiac support device (Impella device (Abiomed, Danvers, USA)) have been used in a number of trials, however the results have not clearly demonstrated any advantages for IABP. Impella demonstrated certain benefits due to its greater hemodynamic support. An alternative to mechanical support alternatives for patients with possible or current circulation failure is venoarterial extracorporeal membrane oxygenation (VA-ECMO), which offers more comprehensive haemodynamic support. ECMO has the additional benefits of right ventricular unloading and blood oxygenation as compared to IABP and Impella. Therefore, herewith, we report a case of high-risk PCI which we performed under the protection of VA-ECMO.
Case Report
A 68year old gentleman, known case of diabetes, severe LV dysfunction, Chronic kidney disease, paroxysmal atrial fibrillation, CAD-TVD was advised CABG for the coronary artery disease, presented to our hospital with complaints of breathlessness at rest, orthopnea. This was his third admission for acute decompensated heart failure in the last 3 months despite being on GDMT for HFrEF. On admission ECG showed sinus rhythm with no acute ST-T changes and ECHO showed severe LV dysfunction with EF-15% with global LV hypokinesia, severe MR. Patient was stabilised with IV diuretics and other supportive medications. We decided to perform complete revascularisation by performing PCI as patient had high surgical risk in view of his comorbidities and risk of periprocedural hemodynamic instability. Patient attenders were given the option of high risk protected PCI under the support of mechanical circulatory support by using either IMPELLA or VA ECMO. Patient attenders agreed for the procedure under the support of VA-ECMO as it was cost effective compared to IMPELLA.
Figure 1: Pre-Procedure LAD
On 17/3/2025 VA ECMO was inserted via the left femoral route. CAG done revealed LAD-mid 90-95% stenosis, LCX-non- dominant vessel with proximal ulcerated 90% stenosis, Major OM 100% CTO, RCA-proximal 100% CTO. PCI was performed to LAD with 3*32mm GENXSYNC STENT, LCX with 2.75*19mm GENXSYNC STENT and RCA with 3*29mm GENXSYNC STENT. TIMI III flow was achieved. Procedure was uneventful.
Patient was shifted to Cardiac Care Unit and was successfully weaned of ECMO on 18/3/2025. Post procedure ECHO showed that the severe MR was reduced to Grade 1 MR. Patient was discharged on 21/3/2025 with dual antiplatelets, statins and GDMT for HFrEF. After 1-week patient came for follow up and was symptomatically feeling better.
Figure 2: Post PCI to LAD
Discussion
PCI is a crucial tool for irrefutable diagnosis and revascularisation in patients with coronary artery disease. Revascularisation and restoration of coronary perfusion can lower the risk of mortality. High-risk patients with intricate coronary artery disease are more prone to experience significant hemodynamic abnormalities during PCI, which can lead to unfavourable outcomes. Notable adverse events which can occur during high risk PCI include cardiac arrest, reflow. Hence Mechanical circulatory support is required while performing high risk PCI. Because ECMO is independent of the patient's heart rhythm and function during PCI, it can provide the body and ischemic/hypoxic tissues with stable blood circulation and adequate oxygen, as well as reduce acidosis, promote metabolite removal, aid in the autonomic circulation recovery, and minimise functional damage to other organs.
Figure 3: Pre PCI to LCX
Image 1
ECMO may also open the door for rapid myocardial reperfusion therapy, which lowers the mortality rate of critically ill patients. Experts recommend high-risk PCI with MCS devices for patients with specific patient and anatomical characteristics, such as coronary artery disease of the left main, a last remaining conduit, or severe multivessel disease. This is especially important for patients who are inoperable and have a severely impaired LVEF or decompensated heart failure. Our case had complex coronary artery disease involving all the 3 vessels with severe LV dysfunction (EF-15%) and severe Mitral Regurgitation. Our patient showed sufficient revascularization results with limited PCI and ECMO- related complications. While VA-ECMO is not extensively studied for high-risk PCI, studies on alternative mechanical circulatory support devices such as Impella and IABP have been published. Perera et al. found that using IABP did not lower the incidence of MACE following PCI in patients with complicated coronary artery disease and severe left ventricular ejection fraction, but long-term follow-up revealed a reduction in all-cause mortality in patients treated with haemodynamic support.
Figure 4: Post PCI to LCX
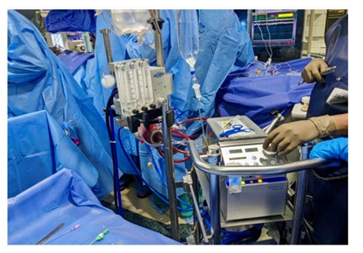
Image 2
Henriques et al. showed the Impella's safety and feasibility, with no procedural or device-related fatalities. In the PROTECT II Trial, 452 patients with severely impaired LVEF and complex three-vessel coronary artery disease, last remaining vessel, or left main coronary artery disease were randomly assigned to IABP or Impella. Both treatment groups achieved satisfactory angiographic results, and there were no differences in the 30-day incidence of MACE (per-protocol analysis: 34.3% for Impella vs. IABP. However, 90-day incidence showed benefit to IMPELLA as there was decreased incidence of MACE. Future studies are needed to compare the results of ECMO and alternative mechanical support devices, such as IABP and Impella, in patients with high-risk PCI, as existing guidelines rely on expert agreement.
Figure 5: Pre PCI to RCA
Figure 6: Post PCI to RCA
Conclusion
The present case showed that high risk protected PCI with VAECMO should be performed in patients with complex triple vessel coronary artery disease and severe LV dysfunction who are at high surgical risk. Sufficient revascularisation and restoration of coronary perfusion improves the patient symptomatically and can reduce the MACE. High-risk PCI with haemodynamic assistance, employing VA-ECMO is a viable therapy option for high-risk surgical revascularisation. Larger, prospective studies and more research is needed to determine the effectiveness of ECMO support in elective high-risk PCI, comparing it to other mechanical circulatory support devices including coaxial left cardiac support devices and IABP.
References
.
- Griffioen, A. M., Van Den Oord, S. C., Van Wely, M. H., Swart,G. C., Van Wetten, H. B., Danse, P. W., ... & Van Geuns, R.J. M. (2022). Short-term outcomes of elective high-risk PCI with extracorporeal membrane oxygenation support: a single- centre registry. Journal of Interventional Cardiology, 2022(1),7245384.
- Ungureanu, C., Blaimont, M., Trine, H., Henin, P., Courcelle, R., Laurent, Y., ... & Huberlant, V. (2023). Prophylactic ECMO Support during Elective Coronary Percutaneous Interventions in High-Risk Patients: A Single-Center Experience. Journal of Interventional Cardiology, 2023(1), 5332038.
- Yan, B., Zhang, G., Huang, C., & Liu, Z. (2023). Successful percutaneous coronary intervention with extracorporeal membrane oxygenation in a patient with acute inferior wall myocardial infarction complicated by electrical storm, cardiogenic shock, and cardiac arrest: a case report. Journal of Cardiothoracic Surgery, 18(1), 47.




