Case Report - (2018) Volume 3, Issue 1
Velamentous Cord Insertion: A Case Report
2Assistant professor obstetrics and Gynaecology, Army College of Medical Sciences New Delhi, India
3Senior Resident obstetrics and Gynaecology, Army College of Medical Sciences New Delhi, India
4Resident obstetrics and Gynaecology, Army College of Medical Sciences New Delhi, India
Received Date: Feb 03, 2018 / Accepted Date: Jan 09, 2018 / Published Date: Feb 13, 2018
Copyright: ©SK Kathpalia, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Normally the umbilical cord is inserted into the central portion of placenta; at times the cord is inserted distally from the margin; onto the fetal membranes, called velamentous insertion. After the insertion the umbilical vessels traverse unsupported for a variable distance between amnion and chorion before reaching the placenta. These vessels can get compressed and torn especially in labour resulting in acute fetal distress and at times fetal death. We report a case where the cause of fetal distress during labour was compression of these vessels. There is a strong case of finding out site of cord insertion when the antenatal cases are undergoing routine sonography. Once abnormal insertion is detected then these pregnancies should be monitored closely as the chances of both antenatal and intranatal complications are higher in such pregnancies.
Keywords
Placenta, Velamentous, Umbilical Cord
Introduction
Normally the umbilical cord is inserted into the central portion of placenta; this insertion is away from the placental margin. At times the cord is inserted near or on the margin of the placenta and rarely inserted distally from its margin; onto the fetal membranes, called velamentous insertion. After the insertion the umbilical vessels separate from each other and traverse for a variable distance between amnion and chorion before reaching the placenta. Unsupported umbilical vessels can also arise as deviant branches of a marginally inserted cord; they can connect lobes of bilobed placenta or succenturiate lobe. The vessels in the membranes are unsupported as they are not covered by protective Wharton’s jelly. Pregnancies complicated by abnormal cord insertion are at greater risk for adverse outcomes, we report one such case where fetal distress occurred in an undiagnosed case of velamentous insertion of cord [1].
Case Report
27 years old second gravida was a booked case, she had undergone emergency cesarean section for non progress of labour three years back. Her postoperative period was uneventful. She had conceived spontaneously in this pregnancy; was doing well antenatally and all her antenatal investigations were normal, fetal growth clinically and on ultrasound appeared satisfactory, placenta was located normally in fundo posterior region. Umbilical cord had normal three vessels. She was assessed in detail for mode of delivery at 38 weeks of gestation. All findings were favorable including pelvic assessment and cervical condition. She reported to hospital after two days with spontaneous onset of labour. Findings were satisfactory; progress of labour was graphically recorded on partograph. Progress of labour was slow and there was fetal bradycardia at 4 cm cervical dilatation. There was no scar tenderness or bleeding PV. She was undertaken for emergency CS, 2.8 Kg baby was delivered through lower segment; lower segment was normal and was not thinned out. After the delivery of baby it was found that placenta had velamentous insertion (Figure-1) of cord; approximately 12 cm away from placental margin (Figure-2). The unsupported vessels were traversing through lower uterine segment but were unruptured. Placenta could be delivered without difficulty. Post operatively she did well and was discharged after four days
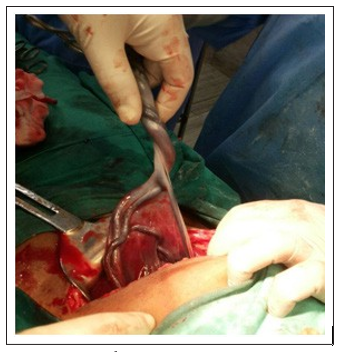
Figure 1: velamentous attachment
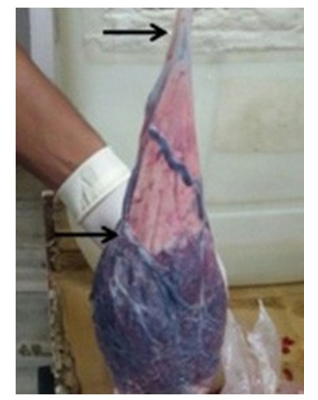
Figure 2: Insertion of cord appx 12 cm away from placental margin
Discussion
Velamentous insertion of cord is not so uncommon; its incidence has been reported as percent, but is observed in as many as 15 percent of monochorionic twin gestations [1,2,3]. Complications commonly associated with velamentous insertion include miscarriage, prematurity, low birth weight, fetal malformation, perinatal death, low Apgar scores and retained placenta requiring manual removal [1,4,5]. The most dangerous complication is vasa previa in which these unsupported vessels run in the lower uterine segment. These vessels are liable to compression and bleeding at the time of delivery and may cause unexpected fetal death due to hypoxia or exsanguinations [6,7]. Rupture of vasa previa is confirmed by differentiating between fetal and maternal blood by acid elution test or alkaline denaturation test which is commonly used [8]. Since the cause for vasa previa is velamentous insertion, early detection of velamentous cord insertion may help in diagnosing this devastating condition [9].
In view of adverse perinatal outcome; routine identification of placental cord insertion both on fetal and placental side should be reported routinely in all antenatal cases undergoing ultra sonography. This abnormal cord insertion can be picked up even during late first trimester or early second trimester as reported by Waldo Sepulveda and followed up subsequently [10]. Women with a prior cesarean section, placenta previa, multiparous women and smokers have slightly increased risk of velamentous cord insertion [11]. Identification of the abnormal cord insertion should be a mandatory part of prenatal ultrasound evaluation [12]. Once abnormal insertion of cord is detected then these pregnancies should be closely monitored, especially in labour, close surveillance could include serial ultrasounds for growth as well as antenatal fetal well being testing.
The mechanisms responsible for abnormal insertion of the umbilical cord are not known, but most probably these events are operative from the first trimester. One theory is trophotropism, in which the chorion frondosum or the early placenta “migrates” with advancing gestation to ensure a better blood supply from a more richly vascularised area [13,14].
References
- Hasegawa J, Matsuoka K, Ichizuka A, Sekizawa, Okai T (2006) Velamentous cord insertion: significance of prenatal detection to predict perinatal complications. Taiwanese Journal of Obstetrics and Gynecology 45: 21-25.
- Tania F E, Yvonne W C, Jonathan S, Susan H T, Brian L S et al. (2012) Velamentous cord insertion: does it affect perinatal outcome? American Journal of Obstetrics and Gynecology 206: 21.
- H Pinar, M Carpenter (2010) Placenta and umbilical cord abnormalities seen with stillbirth. Clinical Obstetrics and Gynecology 53: 656-672.
- Tania F Esakoff, Yvonne W Cheng, Jonathan M Snowden, Susan H Tran, Brian L Shaffer et al. (2015) Velamentous cord insertion: is it associated with adverse perinatal outcomes? The Journal of Maternal-Fetal & Neonatal Medicine 28: 409-412.
- Uyanwah-Akpom P, Fox H (1977) The clinical significance ofmarginal and velamentous insertion of the cord. Br J Obstet Gynaecol 84: 941-943.
- Robert JA, Sepulveda W (2003) Fetal exsanguinations from ruptured vasa previa: still a catastrophic event in modern obstetrics. J Obstet Gynaecol 23: 574-78.
- Jantarasaengaram S, Suthipintawong C, Kanchanawat Thanagumtor S (2007) Ruptured vasa previa in velamentous cord insertion placenta. Journal of Perinatology. 27: 457-59.
- Lindqvist PG, Gren P (2007) An easy-to-use method for detecting fetal hemoglobin-A test to identify bleeding from vasa previa. Eur J Obstet Gynecol Reprod Biol 131: 151-153.
- Oyelese Y, Catanzarite V, Prefumo F (2004) Vasa previa: the impact of prenatal diagnosis on outcomes. Obstet Gynecol 103: 937-942.
- Waldo Sepulveda (2006) Velamentous insertion of the Umbilical Cord. J Ultrasound Med 25: 963-968.
- Yang Q, Wen SW, Phillips K, Oppenheimer L, Black D (2009) Comparison of maternal risk factors between placental abruption and placenta previa. Am J Perinatol 26: 279-286.
- Sepulveda W, Rojas I, Robert J A, Schnapp C, L Alcalde J (2003) Prenatal detection of velamentous insertion of the umbilical cord: a prospective color Doppler ultrasound study. Ultrasound in Obstetrics and Gynecology 21: 564-569.
- Monie IW (1965) Velamentous insertion of the cord in early pregnancy. Am J Obstet Gynecol 93: 276-281.
- AU Kouyoumdjian (1980) Velamentous insertion of the umbilical cord. Obstet Gynecol 56: 737-740.


