Research Article - (2016) Volume 1, Issue 1
Urethral Mucosal Prolapse in girls in Abidjan (Cote dIvoire)
Received Date: Jul 01, 2016 / Accepted Date: Jul 09, 2016 / Published Date: Jul 15, 2016
Copyright: ©Adeneye AK. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: Urethral Mucosal Prolapse is a benign condition that is observed particularly in black girls. The benign nature of this disease contrasts with the anxiety of parents who attribute it to sexual abuse. This survey reported exclusively results of medical management of Urethral Mucosal Prolapse.
Patients and Methods: This retrospective study was conducted in CHU of Yopougon during 15 years from January 1998 to December 2012. All the patients in whom the surgical treatment was indicated at the outset of the disease were excluded from the study. The treatment consisted of the daily application of a dose of estrogen cream on the lump about the size of a hazelnut at the hypogastric region combined with a local antiseptic treatment as well as an antibiotic and a non-steroidal anti-inflammatory coverage.
Results: The patients were black Ivorian in 52 cases. They mean age was 4 years 8 months (1-11 years). In 87% of cases, genital hemorrhage was the telltale sign. In 36 patients the PMU was grade 4 (40.7%). The diagnosis was confirmed by clinical examination in all cases. Five cases were formally attributed to a rape. The total regression was observed before one month in 37 patients (68.5%). The average duration of treatment was 21 days (15-45 days). Two recurrences after early discontinuation of the hormonal treatment and 3 failures were identified; with a persisting residue of non-inflammatory ridge. The proposed surgical indication was rejected by parents in these 3 cases.
Keywords
Urethral Mucosal Prolapse, Blackgirls, Serous vagi¬nal discharge, Mastodynia, Gynecomastia.
Introduction
Urethral Mucosal Prolapse is a benign condition that is most often observed particularly in blackgirls. It produces an eversion of the urethral mucosa, characterized by a ridge which is more or less large, pink to purplish in color, necrotic-hemorrhagic and which bleeds continuously. Moreover this bleeding is the main mode of revelation [1-3]. The benign nature of this disease contrasts with the anxiety of parents who very often attribute it to sexual abuse [4] thus causing serious medico-legal issues. Several methods are proposed for its management: surgery and manual and medical reduction [3,5]. The results of medical management of Urethral Mucosal Prolapse are reported exclusively.
Patients and Methods
This is a retrospective study in the pediatric surgery department of CHU (University Hospital Centre) of Yopougon over a period of 15 years from 1 January 1998 to 31 December 2012. Fifty four (54) girls were received in the consultation services as well as in our emergency services and these girls are the subject of this study. All the patients in whom the surgical treatment was indicated at the outset of the disease were excluded from the study.
The treatment consisted of the daily application of a dose of estrogen cream on the lump about the size of a hazelnut at the hypogastric region combined with a local antiseptic treatment as well as an antibiotic and a non-steroidal anti-inflammatory coverage. Only hormonal treatment was continued for 3 weeks after the regression of inflammatory signs.
Results
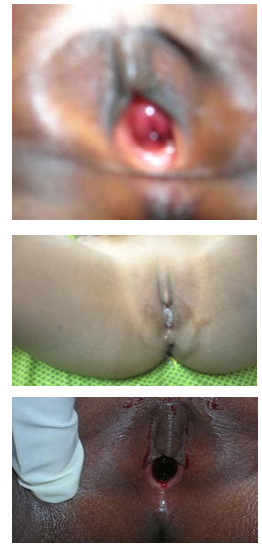
In 52 cases, all the patients were black and Ivorian. They were aged from 1 to 11 years with a mean age of 4 years 8 months. In 87% of cases or 47 times,genital hemorrhage was the telltale sign. Twelve patients (22%) were consulted in 24 hrs, 11 (20%) in the past 7 days. The prolapse was necrotic-hemorrhagic with blood in the vulva in 36 cases (40.7%) (grade 4) (Figures 1-3) is 67%. We did never received grade I. An acute urinary retention was mentioned. The diagnosis was confirmed by clinical examination in all cases. Five cases were formally attributed to a rape and resulted in a sentence of an alleged guilty. Another presumed guilty was compelled to pay all costs of consultation and medicines.
The total regression was observed before one month in 37 patients or 68.5% of cases. The average duration of treatment was 21 days (15-45 days). Gynecomastia associated with breast pain and serous vaginal discharges were observed respectively in 4 and 5 cases. Two recurrences after early discontinuation of the hormonal treatment and 3 failures were identified; with a persisting residue of non-inflammatory ridge. The proposed surgical indication was rejected by parents in these 3 cases.
Discussion
Urethral Mucosal Prolapse is a beginning condition characterized by an eversion of the urethral mucosa, in form of a pink, hemorrhagic, cyanic or necrotic-hemorrhagicridge of variable volume. All the authors agree to emphasize its appearance in the pre-pubertal period [1,3,6] 1-11 years in our series with a mean age of 4.8 years, in accordance with data from the literature [1-3]. This rare pathology [5,7] is occurring essentially in young black girl as shown in all our cases (1,2) although the studies include white girls [8]. This rarity (3-6 cases/year) is the basis of its ignorance, thereby leading to its assimilation to a sexual assault instead of the genital bleeding [1,10]. In fact, usually asymptomatic [3], its mode of revelation is a fortuitous discovery by parents when they find traces of blood in the underwear of their daughters [1,3].
For us as well as for other authors this bleeding has been the principal sign [1-3]. History has seldom found any associated signs such as vaginal discharge or pruritus of genital organs [1,9] and this bleeding is often attributed to a sexual assault which can have dramatic consequences, such as the imprisonment of an innocent person in our series. In general, no obvious cause is highlighted. Furthermore, an involvement of several contributing factors i.e. hypoestrogenism, infection and trauma is suggested [1,3].
Based on the experience of two previous studies in our department [1,7],the clinical diagnosis was without recourse, neither to the para-clinical examinations nor to the examination under anesthesia like some authors [11], against the characteristic ridge protruding below the clitoris and centered by the urethralmeatus. The radical treatment by resection-suture or by the method of Doria requiring hospitalization has long been promoted with satisfactory results [7]. However some involvement of different contributing factors authorizes the medical treatment associating anti-inflammatory, antibiotic, local antiseptic baths and principally the estrogen gel [3,9].
Unlike da-Silva [7] and Fiogbe [2], we used this medical treatment in all our patients, irrespective of the type [3] even in grades 3 and 4. Although longer, 3-6 weeks, it gave us good results. Then, we have to be very attentive to the rare side effects of estrogen such as the serous vaginal discharge, mastodynia and gynecomastia, which disappearupon discontinuation of treatment [9].
According to our experience, the parents now adhere more to the medical treatment which avoids the anesthesia and hospitalization even if it is short. Similarly, the manual reduction may cause bleeding, turning grade 1 to grade 4. Moreover, the surgical treatment next to the failures was challenged by the parents in three of our cases because of the prolonged persistence of a partial ridge residue even after 2 months due to the asymptomatic nature of the disease.
Conclusion
The management of the urethral mucosa prolapse is a benign condition and should receive simple medical treatment, avoiding anesthesia and hospitalization.
Acknowledgments
The authors thank parents and the headmaster of CHU Yopougon, for their help.
References
- da Silva-Anoma S, Bertin KD, Ossenou O, Gaudens DA, Yao D, et al. (2001) [Prolapse of the urethral mucosa in young girls from the Ivory Coast]. Ann Urol (Paris) 35: 60-63.
- Fiogbe MA, Hounnou GM, Koura A, Agossou-Voyeme KA (2011) Urethral mucosal prolapse in young girls: a report of nine cases in Cotonou. Afr J Paediatr Surg 8: 12-14.
- Lang ME, Darwish A, Long AM (2005) Vaginal bleeding in the prepubertal child. CMAJ 172: 1289-1290.
- Aprile A, Ranzato C, Rizzotto MR, Arseni A, Da Dalt L, et al. (2011) “Vaginal” bleeding in prepubertal age: a rare scaring riddle, a case of the urethral prolapse and review of the literature. Forensic Sci Int 210: e16-20.
- Park BJ, Kim YW, Kim TE, Lee DH (2009) Urethral prolapse in a premenarchal Asian girl. Obstet Gynecol 113: 506-507.
- Falandry L (1994) [Prolapse of the urethra in black girls. Personal experience in 11 cases]. Med Trop (Mars) 54: 152-156.
- da Silva-Anoma S, Aguehounde C, Ouattara O, Dieth A, Keita A, et al. (1996) The urethral prolapse in girls: a rare condition in pediatric surgery. Our experience of 22 cases observed at the University Hospital of Cocody and Yopougon. Prog Uro6: 392-397
- Rudin JE, Geldt VG, Alecseev EB (1997) Prolapse of urethral mucosa in white female children: experience with 58 cases. J Pediatr Surg 32: 423-425.
- Sherry Boschert (2001) Topical Estrogen Soaks Heal Urethral Prolapse. OB/GYN News.
- Agarwal S, Lall A, Bianchi A, Dickson A (2008) Uro-genital bleeding in pre-menarcheal girls: dilemmas of child abuse. Pediatr Surg Int 24: 745-746.
- Essiet A, Ikpi E, Essiet GA, Nkposong EO (2007) Uretralprolapse: A case report and commentary on management. African Journal of Urology 13: 1.


