Research Article - (2022) Volume 7, Issue 2
The Efficacy of Probiotic Supplementations on Glycemic Control, Lipid Profile, In-flammation Biomarkers and Anthropometric Measurements Among Type 2 Diabetes Patients
Received Date: Apr 08, 2022 / Accepted Date: May 20, 2022 / Published Date: Jun 02, 2022
Copyright: ©Louay Labban. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Labban. L. (2022). The Efficacy of Probiotic Supplementations on Glycemic Control, Lipid Profile, Inflammation Biomarkers and Anthropometric Measurements Among Type 2 Diabetes Patients. Adv Nutr Food Sci, 7(2), 217-222.
Abstract
Background: Probiotics was defined as living organisms by the World Health Organization. These organisms when consumed as in food items or in the form of supplements, can lead to improvements in the health status of the host. Disturbances of intestinal biology contribute to the development of DM. Many trials have shown that the gut microbiome plays a role in the etiology and progression of type 1 and type 2 diabetes and its complications. This trial was designed to identify the effects of multi-species of probiotic supplementation on fasting blood glucose, lipid profile, inflammatory biomarkers, and in type 2 diabetic patients. Participants and methods: 65 type 2 diabetics were divided into 2 groups T (trial) and C (control) or placebo. The T group received daily one capsule of 14 differnt species of probiotic and C group received capsules filled with roasted ground chickpea. Fasting blood glucose, Serum Tumor Necrosis Factor alpha (TNFα) and C Reactive Protein (CRP), HDLC, LDLC, TG, TC levels were measured and anthropometric measurements such as weight, height, waist circumference and BMI were recorded at beginning and the end of the study which lasted for 10 weeks.
Results and discussion: In the probiotic group, fasting plasma glucose decreased significantly (P <0.05) compared to the control group, 131.1 ± 10.1 vs 145.7 ± 9.8 (mg/dL). Furthermore, a significant reduction was also apparent TC level in the trial group before and after supplementation (184 ± 31 vs 199 ± 21 ) the difference was significant (P < 0.05). The group which received probiotic also showed significant reduction in TG (P < 0.05) compare to control group ( 128 ± 23 vs 1 1 ± 32 respectively). Also, the LDL value, significantly reduced in the probiotic compared to the control group 137 ± 30 and 149 ± 31 ( P < 0.05). Probiotic supplementation significantly increased HDL 41 ± 13 vs 29.8 ± 12 (P < 0.05). Significant differences (P <0.05) in the serum levels of inflammatory markers at the end of the study were observed. Probiotic supplementation decreases CRP (mg/dL) levels and TNFa (pg/ml) (2.11± 4.3 vs 1.68 ± 3.33 and 2.51 ±2.3 vs 2.31 ± 3.6 respectively).. A significant reduction in TNF-α level was observed. The level was 6.8 5.6 ± at the beginning of the trial and reduced to 5.4± 5.1 whereas in the control group TNF-α levels were 5.6 ± 7.6 and 5.6 ± 7.8 at the beginning and at the end of the study respectively .Probiotics supplementations reduced significantly (P <0.05(BMI of participants in trial group (27.6 ± 5.2 vs 33.8 ± 10.1).
Conclusion: The results obtained from this study suggest that probiotic supplementation may have positive effects and can be considered as method to control glucose levels, lipids, inflammatory biomarkers, and reduce body weight in type 2 diabetic patients.
Keywords
Probiotics, Bifidobacterium, Lipid Profile, Glycemic Control, Crp, Tnfα, Bmi.
Introduction
Probiotics was defined by the World Health Organization as func-tional foods. These microorganisms when ingested may support the health status of their host beyond their normal basic nutrient content [1]. The gut microbiome (GM) does not plays a role in the development and progression of diabetes type 1 and 2 only but also in their complications. Disorders in gut biology contribute to the pathogenesis of DM. GM has been shown to affect drug effectiveness. Prebiotics, probiotics and synbiotics, may improve glycemic control as well as DM-related metabolic profiles. There is preliminary evidence that it may even help treat the cardiovas¬cular, ophthalmic, neurological, and renal complications and even aid in the prevention of DM. The role of gut microbiota in con¬trolling diabetes has been demonstrated. Several trials investigat- ed the effects of probiotics and prebiotics, which are widely used to alter the gut microbiome, inflammatory factors and biomarkers caused by oxidative stress in diabetic patients [2]. However, the findings have been contradictory. They are naturally present in a variety of foods such as fruits, raw vegetables, dairy products (es¬pecially fermented products), they are an important part of the gut microbiota as part of the common flora. Main probiotic bacteria can be used in the human nutrition are lactic acid bacteria such as Lactobacillus and Bifidobacterium [3,4].
Comparing healthy subjects with patients diagnosed with chronic inflammatory diseases, mainly rheumatoid arthritis (RA) and an-kylosing spondylitis (SpA), patients with these health problems have alteration in their gut bacteria and this is called biological disorder. These alterations in addition to an increased permea-bility allows cellular or bacterial antigens to interact more readily with the immune system of the host [5]. This inflammation of the intestines is associated with systemic inflammation and may be responsible for the development of several autoimmune diseases and affect their severity [6, 7, 8, and 9].
Evidence from studies performed on rats and humans have shown that beneficial bacteria are created locally as well as systemic alter¬ation of the immune system, leading to a decrease in mucosal in¬flammation and proinflammatory cytokines [10]. In another study, probiotics also lessened rheumatoid arthritis in mice [11]. They can access the immune system of the intestinal lining, persist for a while, and start some immune response. The interaction between the types of beneficial bacteria and enterocytes is important for the controlled production of cytokines and chemokines produced by epithelial cells. It has been shown that some probiotic bacteria can alter the in vitro expression of pro and anti-inflammatory mol¬ecules in a strain-dependent manner. Treatment with certain types of Lactobacillus reduces intestinal permeability and reduces the severity of arthritis [12, 13].
Modification of intestinal microorganisms can alter mechanisms that include risk factors for heart disease, including disruption of lipid metabolism [14]. The use of probiotics is linked to a variety of beneficial effects on human health and changes the physiologi¬cal homeostasis of the intestinal microbiota [15].
Beneficial bacteria are often used to protect the host against harm¬ful microorganisms [16]. These probiotics are helpful in prevent¬ing antibiotic-induced diarrhea and traveler’s diarrhea and these probiotics play a role in the control of gastritis caused by Heli¬cobacter pylori bacteria. In addition, the effectiveness of probiot¬ics has been demonstrated in the treatment of infectious diarrhea, IBD, pouchitis and certain food allergies. They can also reduce the severity of IBD symptoms and lactose intolerance. Lastly, it was acknowledged that probiotics play an important role in inhibiting cancer growth and the process of carcinogenesis [17].
The nutritional benefits of probiotics consist of protective and ben-eficial effects against certain health problems have been demon-strated in many randomized controlled trials which support the evidence of its advantages, are growing [18]. The substantiation for the favorable effects of probiotics to ease constipation and treat hepatic encephalopathy has also been shown in numerous studies. In other studies probiotics showed a proof of efficacy, including prevention of colon cancer, intestinal infections, and relapses of IBD [19]. There is strong evidence for the positive effects of the beneficial bacteria or probiotics on improving symptoms of lac¬tose intolerance, antibiotic-induced intestinal disorders and gas-troenteritis [20]. Recent studies have suggested protective effects against occupation of bad gut microorganisms such as Helico¬bacter pylori and Clostridium difficile [21, 22, 23, and 24].
The purpose of this study was to evaluate the effects of probiot¬ic supplements on serum C-reactive protein (CRP) levels, TNF-α biomarkers, fasting plasma glucose (FPG), lipid profile and an¬thropometric measurements changes among diabetic patients .
Participants and Methods
A total of 64 participants (35 women and 30 men) were enrolled in this study. Participants were diagnosed with type 2 diabetes and were randomly assigned among patients to visit a private endo¬crine clinic. The included patients were aged 33 years to 56 years, diagnosed with diabetes type 2. This research procedure was re¬viewed and approved by A’Sharqiyah University ethics committee (code of ethics: ASU 21073). Informed consent was obtained from each participant. The study was a double-blind, randomized study which lasted for 12 weeks. The recruitment of the participants was done by the researchers. Only the supervisor of this study was aware of the content of the capsules provided (probiotics or chick¬pea) filled and patients in both groups and staff were blinded and supplement contents were kept undisclosed until all participants had completed the study.
During this study, all subjects of group (T), received a capsule of probiotic once a day and Group C the control (or placebo) re¬ceived also a capsule once a day. Both capsules had a completely similar appearance. The capsule which was given to T group had the product (Pronutrition Advanced Probiotics 2 X 109 CFU/ per capsule) that contained 14 different bacterial strains: Lactobacillus acidophilus, Lactobacillus. delbrueckii ssp, Lactobacillus bulgar¬icus, Lactobacillus casei, Lactobacillus plantarum, Lactobacillus rhamnosus, Lactobacillus salivarius, Lactococcus lactis ssp , Ba¬cillus subtilis, Streptococcus thermophiles, Bifidobacterium bifi-dum, Bifidobacterium breve, Bifidobacterium infantis, and Bifido¬bacterium longum. The placebo capsule contained ground roasted chickpea capsule. All other types of products rich in probiotic were not allowed to consume during the study for both the trial and con¬trol group.
Anthropometric measurements were also taken from participants in both groups at the beginning and end of the study. The measure¬ments were weight, height, waist and hip circumferences. Body weight and height are measured by the digital beam balance of the Tanita W 3000. BMI was immediately calculated by the same balance. The waist circumference was measured using a standard tape measure and the waist and hip circumference was calculated
by dividing the waist circumference by the hip circumference. The study required 2-day dietary recall and was collected from each patient prior to the start of the study to measure total energy intake. Patients in both groups were given an isocaloric diet consisting of 55% carbohydrates, 20% protein and 25% fat. The total caloric content of the food eaten by both groups is shown in Table 1:
Table 1: Total calorie intake ((Kcal/day) of patients in trial and control diets
|
Total energy intake (Kcal/day) |
T(Trial) group |
Control (C or Placebo) group |
|
|
299.7 ± 1725 |
1805± 349.5 |
Results and Discussion
The study sample included 64 patients with type 2 diabetes. The study group included 36 patients (16 women and 20 men) and the pla-cebo group included 28 patients (13 women and 15 men) as shown in Figure 1
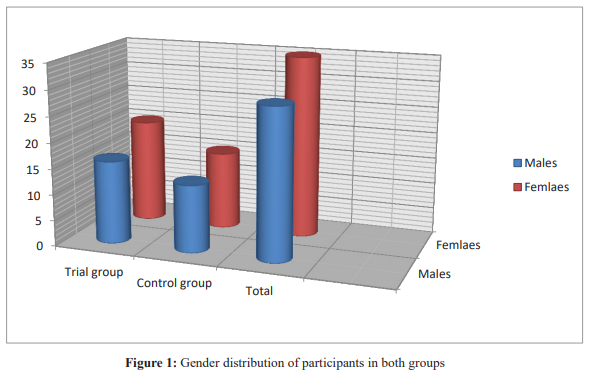
Furthermore, the data such as age, BMI, anthropometric measure¬ments and energy intake of the groups of this study was recorded and there were no significant differences between patients of both groups of this study for anthropometric measurements as demon-strated in Table2.
Table 2: Age and anthropometric measurements of participants in Trial and Control groups
|
|
Trial group |
Control group |
|
Ages (Years ± SD) |
59.4 ± 8.3 |
56.6 ± 8.1 |
|
BMI (W/H2) |
5.23 ± 30.4 |
33.4 ± 9.9 |
|
Weight (kg) |
85.8 ± 9.7 |
87.3 ± 11.3 |
|
Height (cm) |
166.8 ± 27.3 |
161.3 ± 19.9 |
|
Waist circumferance (cm) |
128.9 ± 15.1 |
134.2 ± 15.3 |
|
Hip circumferance (cm) |
99.9 ± 23.5 |
121.5 ± 25.4 |
|
Waist/Hip ratio |
1.3 ± 0.4 |
1.1 ± 0.3 |
The study has shown that supplementation of multispecies pro-biotics has significantly (P <0.05) decreased the CRP and TNF-α in the trial group. CRP level was 4.3 ± 2.11 at the beginning and decreased to 1.68 ± 3.33 in trial group whereas in the control group CRP level was 2.512.3 ± and reduced to 3.6 ± 2.31 but the difference was not significant. A significant reduction in TNF-α level was observed. The level was 6.8 5.6 ± at the beginning of the trial and reduced to 5.4± 5.1, whereas in the control group TNF-α levels were 5.6 ± 7.6 and 5.6 ± 7.8 at the beginning and at the end of the study respectively. These data are presented in Table 3.
Table 3: Alterations in inflammatory biomarkers of both groups at the beginning and at the end of the study
|
Inflammation biomarker |
|
Trial Group |
Control group |
|
CRP (mg/dL) |
Before |
4.3 ± 2.11 |
2.3 ± 2.51 |
|
After |
3.3 ± 1.68 * |
3.6 ± 2.31 |
|
|
TNF-α (pg/ml) |
Before |
6.8 5.6 ± |
5.6 ± 7.6 |
|
After |
* 5.1 ± 5.4 |
5.6 ± 7.8 |
|
|
* Significant difference P<0.05 |
|||
There are many studies which support our findings. Most of these studies confirmed the beneficial effects of probiotics or synbiotics on the circulating inflammatory marker (hs-CRP) in the serum and plasma. Probiotic supplementation reduced hs-CRP the inflam¬mation biomarker (24). In another study which demonstrated that probiotic consumption created a positive outcome in dropping the levels of plasma inflammation markers, including tumor necrosis factor-α (TNF-α) and C-reactive protein (CRP) when compared with the control situation [25, 26].
Table 4: shows that probiotics supplementation of multispecies probiotics to type 2 diabetics significantly reduced their fasting plasma glucose. The effect of probiotics was significant of probi-otics on FPG (P < 0.05). In the trial group, FPG at the beginning of this study was 154.4 ± 11.6 and it was dropped to 131.1 ± 10.1(mg/ dL) whereas the reduction in the control group was not significant (147.7 ± 10.8 vs 145.7 ± 9.8). The data presented in Table 4. It has also showed that supplementation of probiotics to type 2 diabet¬ics reduced their Total Cholesterol level. TC level (mg/dL) was 219 ± 30 at the beginning of the study and decreased to 184 ± 31 and the difference was statistically significant (P < 0.05) whereas this difference was not significant in the control group. There was also a significant decrease in Triglyceride level between Trial and Control group after supplementation. The TG level was 150 ± 39 mg/dL before supplementation and became 128±23 mg/dL and the TG in Control group was 139 ± 33 mg/dL and became 141 ± 32 mg/dL before and after supplementation respectively. The LDL-C had the same pattern as it decreased significantly after supplemen¬tation with probiotics. In Trial group LDL-C level was 158 ± 35 mg/dL before supplementation and went down to 137 ± 30 after supplementation and the LDL-C level in Control group was 151 ± 29 mg/dL before supplementation and became 149 ± 31 mg/dL . A significant difference was observed between the two groups after supplementation (P < 0.05).
The effect of supplementation was strong on HDL-C level. Pro¬biotics supplementation significantly improved HDL-C level in Trial group but not in Control group. HDL-C level went up in the Trial group from 32.5 ± 11.1 to 41.3 ± 13 mg/dL and surprisingly HDL-C decreased in Control group as HDL-C level was 31.7 ± 12 mg/dL before supplementation and became 29.8 ± 12.6 mg/dL after supplementation. The difference was significant (P < 0.05) between groups after supplementation. Probiotic supplementation also improved C-HDL-C ratio . In trial group, the ratio decreased from 6.7 ± 1.8 before supplementation to 4.6 ± 1.1 after supple¬mentation and the difference was statistically significant (P < 0.05). On the contrary, the ratio was not improved in the Control group. However, statistically significant difference was observed between both groups after supplementation with probiotics.
Table 4: Fasting plasma glucose, lipid profile and body weight changes for trial and control groups at the beginning and at theend of this study
|
Indicator |
|
Trial group |
Control group |
|
Fasting Plasma glucose level (mg/dL) |
Before |
154.4 ± 11.6 |
147.7 ± 10.8 |
|
After |
131.1 ± 10.1* |
145.7 ± 9.8 |
|
|
Total Cholesterol (mg/dL) |
Before |
219 ± 30 |
209 ± 27 |
|
After |
184 ± 31* |
199 ± 21 |
|
|
Triglycerides (mg/dL) |
Before |
150 ± 39 |
139 ± 33 |
|
After |
128 ± 23 * |
141 ± 32 |
|
|
LDL-C (mg/dL) |
Before |
158 ± 35 |
151 ± 29 |
|
After |
137 ± 30* |
149 ± 31 |
|
|
HDL-C (mg/dL) |
Before |
32.5 ± 11.1 |
31.7 ± 12 |
|
After |
41.3 ± 13 * |
29.8 ± 12 |
|
|
C/HDL ratio |
Before |
6.7 ± 1.8 |
6.5 ± 1.9 |
|
After |
4.6 ± 1.1 * |
6.7 ± 1.8 |
|
|
BMI changes |
Before |
5.23 ± 30.4 |
33.4 ± 9.9 |
|
After |
27.6 ± 5.2 * |
33.8 ± 10.1 |
|
|
* Significant difference P<0.05 |
|||
Supplementation with probiotics had its effect on BMI. BMI sig-nificantly improved after supplementation in Trial group as it was 5.23 ± 30.4 before supplementaion and became 27.6 ± 5.2 whereas the improvement in BMI in Control group was not noticed. The difference was statistically signifcantly between both groups (P <0.05).
The results of this study were consistent with many other studies regarding the effect of probiotic supplements on glucose levels. In the study of Ostadrahimi et al 2015 found that the favorable outcomes of consuming Kefir (a traditional collection of beneficial microbes) were acknowledged on glycated hemoglobin (HbA1c) readings, and weight loss among diabetic patients. In this study, the patient consumed kefir as an addition of the glucose lowering medication. The results showed that the patient lost about 4 kg of bodyweight, and her HbA1c decreased from 7.9 to 7.1 after 90 days of consumption of kefir. Improvements were also record¬ed in sleep quality as reported by the patient [26]. Similar results have been reported in many studies and comparable to the results that we obtained from the current study showing that probiotics supplements significantly lessened total cholesterol, LDL-c, and triglycerides and increased HDL-c [27, 28, 29, and 30].
We attempted in this study to find out if there was any adverse effect of consumption of probiotic supplements on gastrointesti¬nal health including bloating, constipation, GERD or allergies on participants from both groups even though the patients in the Control group did not ingest any amount of probiotics. We also wanted to know the placebo effect on those patients. In Trial group 13 individual or (36.1%) did not have any symptoms comparing with 14 individuals (50%) in the Control group. As for bloating, 3 individuals in Trial group reported bloating whereas 4 (14.3%) reported the same symptoms in the Control group. The number of individual who had constipation and GERD was similar 5(13.8%) in Trial group but it was 5 (13.8 %) for constipation and 1(2.8%) for GERD in Control group. More people reported allergies in Tri¬al group comparing with Control group. 6 (16.7%) vs 2 (5.6%). For abdominal pain and diarrhea similar number reported in Trial group 1 (3.6 %) and in the Control group 1 (2.8%) for abdominal pain and diarrhea. The number of cases of GI complications is summarized in Table 5:
Table 5: the number and percentage of GI complication after ingesting probiotics supplementation
|
GI complication |
Trial group (Number / %) |
Control group (Number / %) |
|
None |
13 (36.1 %) |
14 (50 %) |
|
Bloating |
3 (8.3 %) |
4 (14.3 %) |
|
Constipation |
5 (13.9 %) |
5 (17.9 %) |
|
GERD |
5 (13.9 %) |
1 (2.8 %) |
|
Allergies |
6 (16.7 %) |
2 (5.6 %) |
|
Abdominal pain |
1 (3.6 %) |
1 (2.8 %) |
|
Diahrrea |
1 (3.6 %) |
1 (2.8 %) |
Conclusion
Probiotics supplements considerably decreased the levels of TC, LDL-C, and TG and improved HDL-C. Other benefits such as gly-cemic control, inflammation, and anthropometric measurements were noticed on the patients. The results of this study propose that probiotic supplements should be pointed out as accompanied man¬agement for diabetes type 2 and dyslipidemias. We recommend that more studies should be carried out to find out any long-term role, as well as their impact with glucose lowering medications.
Acknowledgement
The author would like to thank the staff at the central laboratory for their kind participation in analyzing the blood samples of the patients participated in this study. The author would also like to extend his gratitude for the Dean of Health Science College for his advice and encouragement. The author states that there is no conflict of interest.
References
- Yao, K., Zeng, L., He, Q., Wang, W., Lei, J., & Zou, X. (2017).Effect of probiotics on glucose and lipid metabolism in type2 diabetes mellitus: a meta-analysis of 12 randomized controlled trials. Medical science monitor: international medical journal of experimental and clinical research, 23, 3044.
- Alagiakrishnan, K., & Halverson, T. (2021). Holistic perspective of the role of gut microbes in diabetes mellitus and its management. World Journal of Diabetes, 12(9), 1463.
- Wang, P., Tao, J. H., & Pan, H. F. (2016). Probiotic bacteria: a viable adjuvant therapy for relieving symptoms of rheumatoid arthritis. Inflammopharmacology, 24(5), 189-196.
- Diamanti, A. P., Manuela Rosado, M., Laganà, B., & D’Ame-lio, R. (2016). Microbiota and chronic inflammatory arthritis: an interwoven link. Journal of Translational Medicine, 14(1), 1-12.
- Mielants, H., De Vos, M., Cuvelier, C., & Veys, E. M. (1996). The role of gut inflammation in the pathogenesis of spondy-loarthropathies. Acta Clinica Belgica, 51(5), 340-349.
- Tlaskalová-Hogenová, H., ŠtÄ?pánková, R., Hudcovic, T., TuÄková, L., Cukrowska, B., Lodinová-Žádnıková, R., ... & Kokešová, A. (2004). Commensal bacteria (normal microflora), mucosal immunity and chronic inflammatory and autoimmune diseases. Immunology letters, 93(2-3), 97-108.
- Sartor, R. B. (1997). Role of the enteric microflora in the pathogenesis of intestinal inflammation and arthritis. Alimen-tary pharmacology & therapeutics, 11, 17-23.
- McCulloch, J., Lydyard, P. M., & Rook, G. A. W. (1993). Rheumatoid arthritis: how well do the theories fit the evidence?. Clinical & Experimental Immunology, 92(1), 1-6.
- Danning, C. L., & Boumpas, D. T. (1998). Commonly used disease-modifying antirheumatic drugs in the treatment of inflammatory arthritis: an update on mechanisms of action. Clinical and experimental rheumatology, 16(5), 595-604.
- Delcenserie, V., Martel, D., Lamoureux, M., Amiot, J., Bou-tin, Y., & Roy, D. (2008). Immunomodulatory effects of probiotics in the intestinal tract. Current issues in molecular biology, 10(1-2), 37-54.
- Kano, H., Kaneko, T., & Kaminogawa, S. (2002). Oral intake of Lactobacillus delbrueckii subsp. bulgaricus OLL1073R-1 prevents collagen-induced arthritis in mice. Journal of food protection, 65(1), 153-160.
- So, J. S., Kwon, H. K., Lee, C. G., Yi, H. J., Park, J. A., Lim,S. Y., ... & Im, S. H. (2008). Lactobacillus casei suppresses experimental arthritis by down-regulating T helper 1 effector functions. Molecular immunology, 45(9), 2690-2699.
- Strowski, M. Z., & Wiedenmann, B. (2009). Probiotic carbohydrates reduce intestinal permeability and inflammation in metabolic diseases. Gut, 58(8), 1044-1045.
- Gadelha, C. J. M. U., & Bezerra, A. N. (2019). Effects of probiotics on the lipid profile: Systematic review. Jornal vascular brasileiro, 18.
- Montalto, M., Arancio, F., Izzi, D., Cuoco, L., Curigliano, V., Manna, R., & Gasbarrini, G. (2002). Probiotics: history, definition, requirements and possible therapeutic applications. Annali italiani di medicina interna: organo ufficiale della So-cietà italiana di medicina interna, 17(3), 157-165.
- Kühbacher T, Ott SJ, Helwig U, Mimura T, Rizzello F, Klees-sen B, Gionchetti P, Blaut M, Campieri M, Fölsch UR, Kamm MA, Schreiber S.Gut. 2006 Jun;55(6):833-841.
- Wilhelm, S. M., Brubaker, C. M., Varcak, E. A., & Kaleâ?Prad-han, P. B. (2008). Effectiveness of probiotics in the treatment of irritable bowel syndrome. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy, 28(4), 496-505.
- Marteau, P., & Boutron-Ruault, M. C. (2002). Nutritional advantages of probiotics and prebiotics. British Journal of Nutrition, 87(S2), S153-S157.
- Weese, J. S. (2002). Probiotics, prebiotics, and synbiotics. Journal of equine veterinary science, 22(8), 357-360.
- Saavedra, J. M., & Tschernia, A. (2002). Human studies with probiotics and prebiotics: clinical implications. British Journal of Nutrition, 87(S2), S241-S246.
- Cary, V. A., & Boullata, J. (2010). What is the evidence for the use of probiotics in the treatment of inflammatory bowel disease?. Journal of Clinical Nursing, 19(7â?8), 904-916.
- Yao, K., Zeng, L., He, Q., Wang, W., Lei, J., & Zou, X. (2017).Effect of probiotics on glucose and lipid metabolism in type 2 diabetes mellitus: a meta-analysis of 12 randomized controlled trials. Medical science monitor: international medical journal of experimental and clinical research, 23, 3044.
- Ostadrahimi, A., Taghizadeh, A., Mobasseri, M., Farrin, N., Payahoo, L., Gheshlaghi, Z. B., & Vahedjabbari, M. (2015). Effect of probiotic fermented milk (kefir) on glycemic control and lipid profile in type 2 diabetic patients: a randomized double-blind placebo-controlled clinical trial. Iranian journal of public health, 44(2), 228.
- Zheng, H. J., Guo, J., Jia, Q., Huang, Y. S., Huang, W. J., Zhang, W., ... & Wang, Y. (2019). The effect of probiotic and synbiotic supplementation on biomarkers of inflammation and oxidative stress in diabetic patients: a systematic review and meta-analysis of randomized controlled trials. Pharmacological research, 142, 303-313.
- Ding, L. N., Ding, W. Y., Ning, J., Wang, Y., Yan, Y., & Wang,Z. B. (2021). Effects of Probiotic Supplementation on Inflammatory Markers and Glucose Homeostasis in Adults With Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis. Frontiers in pharmacology, 12.
- Plaza-Díaz, J., Ruiz-Ojeda, F. J., Vilchez-Padial, L. M., & Gil,A. (2017). Evidence of the anti-inflammatory effects of probiotics and synbiotics in intestinal chronic diseases. Nutrients, 9(6), 555.
- Gadelha, C. J. M. U., & Bezerra, A. N. (2019). Effects of probiotics on the lipid profile: Systematic review. Jornal vascular brasileiro, 18.
- Zhang J, Ma S, Wu S, Guo C, Long S, Tan H. J Diabetes Res. 2019; 2019:5364730. Epub 2019 Sep 5.
- Fortes PM, Marques SM, Viana KA, Costa LR, Naghettini AV, Costa PS. Syst Rev. 2018 Oct 17; 7(1):165. Epub 2018Oct 17.
- Labban, L. (2015). The Scope of Therapeutic Use of Probiotics in Management of Diabetes Mellitus. EC Nutrition, 1(5), 254-258.



