Research Article - (2025) Volume 3, Issue 6
Effects of Catastrophic Healthcare Expenditure on Household Labor Supply in Malawi
Received Date: Oct 20, 2025 / Accepted Date: Nov 21, 2025 / Published Date: Nov 25, 2025
Copyright: ©2025 Wellem Ndipo. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Ndipo, W. (2025). Effects of Catastrophic Healthcare Expenditure on Household Labor Supply in Malawi. Int Internal Med J, 3(6), 01-08.
Abstract
Background: The dynamics of labor supply and demand are examined via microeconomic theory at the individual firm and worker levels. A number of factors influence the amount and quality of the labor supply; one such determinant is health status. Research has viewed the connection between household labor supply and health as a two-way causal relationship, with health serving as the deciding factor that influences decisions made in the labor market. The labor supply of a particular household or individual is seen to be affected by a number of factors, with the health status of an individual or a family member being one of them. Households or individuals are forced to either increase or reduce the number of hours they offer to work with respect to the amount of income they spend in trying to cover health care expenses. A household is seen to fall into a health care spending catastrophe if its aggregate health expenditure exceeds a given threshold; thus, in this case, the study uses the 10% and 40% thresholds.
Objective: This study analyzed the effect of catastrophic health care expenditures on the household labor supply.
Methods: This study used the Fifth Integrated Household Survey, which consists of 11,434 respondents. An instrumental variable approach with a binary outcome variable was employed to estimate the causal effect of catastrophic health expenditures on the household labor supply in hours.
Results: The results from instrumental variable regression indicate that the probability of households supplying labor tends to decrease once they are subjected to catastrophic health care expenses at both thresholds.
Recommendation: The study recommends the implementation of policies that enhance financial protection for vulnerable groups. One such measure is the introduction of progressive taxation, which ensures that those with higher incomes contribute more to national revenue that can be in turn used to subsidize user fees.
Introduction
The dynamics of labor supply and demand are examined via microeconomic theory at the individual firm and worker levels [1]. A number of factors influence the amount and quality of the labor supply; one such determinant is health status. Health plays a role in influencing individuals' preferences between work and leisure activities following a health shock [2,3]. Deteriorating health may lead to a heightened demand for leisure, altering decisions connected to work supply, especially given the impact of health on life expectancy [4]. When the direct costs of healthcare services are considerable, generally referred to as out-of-pocket payments, households may experience challenges in covering these charges using their available resources. Studies conducted in Africa and Asia, for example, highlight that user fees significantly impede healthcare access for the most vulnerable individuals, including elderly men and women, widows, and women headed households [5,6].
According to the World Bank, Malawi's labor force participation rate stood at 67.6% in December 2022. The CEIC data also show that the labor force participation rate in Malawi has fluctuated between 67.4% and 80.8% since December 1990. In terms of financing mechanisms, most households in Malawi use out-of- pocket expenses to cover their health-related bills, such that these expenses often lead households to experience health care spending catastrophes [7,8].
As reported by the World Bank (2024), Malawi's labor force participation rate reached 67.6% in December 2022, with a steady increase over time [7,8]. Data from the CEIC also indicate that labor force participation in Malawi has fluctuated between 67.4% and 80.8% since 1990, with a noticeable increase in recent years.
Figure 2: Below Shows How the Labor Supply Trend has Been in this Country Over the Years
Source: Plotted using data from the World Development Indicator Database, World Bank
Despite this increase, many households in Malawi continue to rely heavily on out-of-pocket expenses to meet their healthcare needs [7,8]. This reliance often results in households facing catastrophic health expenditures. The Global Health Expenditure Database reports an increase in out-of-pocket spending in Malawi, from 12.2% in 2019 to 15.8% in 2020, as illustrated in Figure 3 below.
Source: Plotted using data from the Global Health Expenditure Database As individuals struggle to cover these health costs, they tend to respond by increasing their labor supply, working more hours in an effort to increase earnings to cover medical expenses. However, this relationship is complex and bidirectional, as some households may reduce their hours of work following a health shock, such as caring for a sick family member requiring inpatient care.
While previous studies, including Choi et al. (2016) and Lee et al. (2020), have examined the connection between catastrophic health spending and household labor market behaviors, limited attention has been given to how these expenditures directly influence household labor supply decisions [9,10]. This study aims to address the gap in Malawi, where for example, Mchenga et al. (2017) focused only on the impoverishing effects of CHEs in general without specifically pinning them to a narrow sector, such as in this case, the labor supply, by analyzing the causal relationship between the rising labor force participation rates, illustrated in Figure 1, and the persistent increase in out-of-pocket health payments, depicted in Figure 2. The study therefore aims to determine whether these rising demands for labor are the result of households experiencing catastrophic health expenses depicted by the continued rise in out-of-pocket payments in the form of user fees and other health-related expenses [11].
Catastrophic health care expenditure has been identified as a significant factor contributing to impoverishment, contrary to the objectives outlined in Sustainable Development Goal 3 (SDG 3), which seeks to promote good health and well-being. Through an examination of its effects on labor force participation, this study, in alignment with SDG 10, aims at providing insights that can guide the formulation of policies aimed at diminishing inequalities by analyzing how health care costs disproportionately impact distinct income groups, potentially exacerbating preexisting disparities, thus helping reinforce economic resilience at the household level.
Methods
Data
According to the WHO, household income and expenditure surveys are crucial for evaluating whether households face "catastrophic" health costs. Therefore, this study utilizes secondary data from Malawi's fifth round of the Integrated Household Survey (IHS5), which was conducted between April 2019 and March 2020. The survey sampled 11,434 households, which were statistically selected to ensure representativeness at the national, district, urban, and rural levels. The IHS5 employed a stratified sampling design, selecting 719 census enumeration areas (EAs) as primary sampling units (PSUs), with an average of 16 households per EA. Four types of questionnaires were administered during the survey: Household, Agricultural, Fisheries, and Community questionnaires. The key variables for this study-household labor supply, catastrophic health expenditure (CHE), household shocks and demographic characteristics-were derived primarily from the Household Questionnaire, which also includes broader information on household welfare in Malawi.
Dependent Variable
Our variable of interest was household labor supply, which was measured in hours. In the survey questionnaire, the respondents were asked specific questions about the number of hours they spent on different income-generating activities in the previous week, and the hours were aggregated. To improve consistency and precision in the model, the variables were normalized via the minâ??max method. This was necessary, as the raw aggregated labor hours produced disproportionately large values, reducing the precision of the parameter estimates. Proper normalization is critical in econometric models to ensure reliable and economically interpretable results [12]. The normalized variable ranges from 0 to 1, where values closer to 0 indicate lower-than-usual labor supply, and values closer to 1 indicate higher-than-usual labor supply.
Explanatory Variables
The choice of independent variables was based on previous studies that assessed the different health factors that affect the supply of labor for a given household. The variables included gender of the household head, age of the household head, location, education of the household head, catastrophic health expenditure (CHE) and marital status of the household head, among others, with CHE being the main explanatory variable of interest (see Table 1 for a full list of the variables we used). The choice of these explanatory variables is motivated by a number of studies like . This study employs both the 10% and 40% approaches to assess the economic implications of the catastrophic health care spending of given households toward their behavior in the labor market. The calculation for these thresholds is based on the guidelines proposed in several studies that look at estimation methods for the CHE thresholds [13,14]. The use of these different thresholds also helps to understand the extent to which poor households and rich households differ in the way they are affected when health care out of pocket spending exceeds the catastrophic thresholds with respect to their response in the labor market.
Instrument Choice
Endogeneity in this relationship arises from several factors. First, households experiencing significant out-of-pocket healthcare expenses may respond by increasing their labor hours to generate additional income to cover these costs. Conversely, an increase in labor hours supplied by a household may lead to higher income, enabling them to afford healthcare expenses and potentially influencing the extent of catastrophic health expenditures (CHEs) incurred.
Additionally, unobservable household characteristics, such as preferences for health or risk aversion, can simultaneously affect both the likelihood of incurring CHE and labor supply decisions.
This paper followed a number of studies that used shocks to instrument for the relationship between catastrophic health care expenditures and household welfare (Paxson, 1992; Wagstaff, 2007). The study, therefore, uses aggregated health shocks that may influence a household to incur catastrophic health payments as an instrument. The health shocks were computed by summing all the indicators that make up these health-related shocks, including but not limited to, death, birth, pandemics, etc.
Following equation i below, every shock is algebraically represented as:

These aggregated health shocks are assumed to affect the household labor supply (the dependent variable) solely through their influence on catastrophic health expenditures (CHE). These shocks are not expected to directly impact labor supply decisions in ways unrelated to CHE. We assume that aggregated health shocks do not directly affect labor supply decisions because they operate primarily through increased financial burden, captured by CHE. Any direct impact of health shocks (e.g., caregiving or reduced physical productivity) is assumed to be minimal and not systematically correlated with labor supply after accounting for CHE.
Data Analysis
The study used an instrumental variable approach with a binary dependent variable (IVPROBIT) to address endogeneity. Endogeneity occurs when a covariate is correlated with the unobserved error term of the regression. Our IV approach was motivated by concerns around the reverse causality between household aggregate expenditure and labor supply, which could cause endogeneity.
The basic simultaneous equations for estimating the model are represented as:
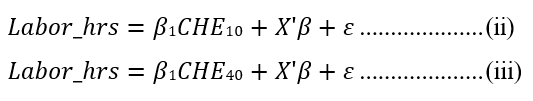

Instrument Relevance and Weak Instruments
To test for the presence of endogeneity in the dependent variable, the wald statistic is used. This statistic examines the null hypothesis that the dependent variable is zero. The Wald test yields a Chi2 statistic of 6.84, which is significant at the 1% level, with a p value of 0.0089. This, therefore, justifies the need to use instrumental variables to control for the endogeneity problem.
The study also performs a first-stage test to determine whether the instrument used is strong enough to capture the variations in the relationships being 0observed. The reported F statistics were greater than 10, with values of 16.7034 and 11.748 for both the 10% and 40% thresholds, respectively.
The model does not suffer from any overidentification issues, as only one instrument was used; thus, the model was identified exactly
Results
Descriptive Statistics
|
Variable |
Obs |
Mean/freq1 |
Std. Dev. |
Min |
Max |
|
CONTINUOUS |
|
|
|
|
|
|
labor hrs |
11434 |
32.553 |
32.213 |
0 |
865 |
|
age head |
11434 |
43.129 |
16.085 |
15 |
100 |
|
BINARY/CATEGORICAL |
|
|
|
|
|
|
CHE10 |
11434 |
2.7% |
.162 |
0 |
1 |
|
CHE40 |
11434 |
0.5% |
.068 |
0 |
1 |
|
chronic condition |
11434 |
27.5% |
.446 |
0 |
1 |
|
Marital status of head |
. |
. |
. |
. |
. |
|
Married |
11434 |
70% |
.458 |
0 |
1 |
|
Separated/Divorced |
11434 |
14.5% |
.352 |
0 |
1 |
|
Widowed |
11434 |
12.2% |
.327 |
0 |
1 |
|
Never |
11434 |
3.3% |
.179 |
0 |
1 |
|
location(Rural=1) |
11434 |
81.7% |
.387 |
0 |
1 |
|
gender(male=1) |
11434 |
69.9% |
.459 |
0 |
1 |
|
Region |
|
|
|
|
|
|
South |
11434 |
46.4% |
.499 |
0 |
1 |
|
Centre |
11434 |
34.6% |
.476 |
0 |
1 |
|
North |
11434 |
19% |
.393 |
0 |
1 |
|
Education Qualification |
|
|
|
|
|
|
none hh |
11434 |
66.4% |
.473 |
0 |
1 |
|
plsc hh |
11434 |
11.2% |
.315 |
0 |
1 |
|
jce hh |
11434 |
8.9% |
.285 |
0 |
1 |
|
msce hh |
11434 |
9% |
.286 |
0 |
1 |
|
postsec hh |
11434 |
4.6% |
.209 |
0 |
1 |
Table 1: Summary Statistics
As given in the Table 1 above, 2.7% of the households incur catastrophic health care spending under the 10% threshold compared to the households that did not incur catastrophic health care spending using the same threshold. Using the 20% threshold, 3.5% of the households recorded catastrophic health care expenditures in comparison to those households that did not incur catastrophic health care expenditures given the same threshold. Thus, the threshold effect is observed as we increase it from 10% to 20%. On average, the number of hours worked per household, thus aggregating the number of hours per working household member, is 32 hours.
On average, most households were seen to be composed of 4 members. The average age of a household head was 43 years, with a minimum age of 15 years and a maximum of 100 years, thus indicating the presence of child-headed households. Male-headed households, on average, account for 70% of the total households in the sample, thus indicating homogeneity in the sample.
Most respondents are seen to reside in rural areas, thus accounting for 81.7% of those households residing in urban areas. With respect to the regional dispersion of household respondents, the southern region recorded the highest proportion of households, with a percentage of 46.4, followed by the central region, with 34.6%, and the northern region, with 19% of the total sample households.
Twenty-eight percent of the households were recorded to have at least one family member with a chronic condition or suffering from a chronic disease. On average, many household heads were recorded to have not attended any school level, representing 66.4% of the total population, compared with those who attended primary, secondary or tertiary levels. Seventy percent of the household heads were recorded to be monogamous or polygamous, indicating that a higher percentage, followed by divorced or separated household heads, recorded 14.5% of the total sample households.
T Tests
The study used t tests to determine if there was a significant difference between the means.
|
|
Yes |
no |
p-value |
|
Labor hours by(CHE10) |
25.35323 |
32.75387 |
0.000 |
|
Labor hours by(CHE20) |
22.54717 |
32.59982 |
0.023 |
|
Labor hrs by(chronic condition) |
30.54045 |
33.31523 |
0.000 |
|
Labor hrs by(location)2 |
27.82391 |
53.67232 |
0.000 |
|
Labor hours, by(gender of head)3 |
36.07234 |
24.36514 |
0.000 |
Table 2: Two-way t Test with Equal Variances
Table 2 above shows that, households experiencing catastrophic health care expenditures in both the CHE10 and CHE20 categories are observed to supply significantly more hours of labor than households that do not incur such expenditures. The magnitude of the differences in mean labor hours is substantial and statistically significant for both categories. There is also a significant difference in the mean number of hours worked between households with at least one member with a chronic condition and those households without a chronically ill member. Households that are headed by males are observed to supply a significantly greater number of work hours than households that are headed by females. With respect to location, households that reside in rural areas are observed to supply significantly fewer hours of work than households that reside in urban areas.
Econometric Results
|
Normalized Labor hours |
Model 14 |
Model 25 |
|
CHE10 |
-4.664*** (0.917) |
|
|
CHE40 |
|
-12.081*** (2.001) |
|
Age of head |
-0.005*** (0.002) |
-0.005*** (0.002) |
|
marital status |
|
|
|
Separated/Divorced |
-0.160*** (0.054) |
-0.144*** (0.056) |
|
Widowed |
-0.192*** (0.067) |
-0.118 (0.075) |
|
Never |
-0.259*** (0.088) |
-0.196** (0.093) |
|
Rural |
0.090** (0.039) |
0.044 (0.037) |
|
Gender of head |
0.151** (0.073) |
0.168** (0.071) |
|
Education of head |
|
|
|
plsc_hh |
-0.025 (0.044) |
-0.036 (0.042) |
|
jce_hh |
0.050 (0.059) |
0.027 (0.058) |
|
msce_hh |
0.092 (0.070) |
0.090 (0.067) |
|
postsec_hh |
0.061 (0.083) |
0.059 (0.079) |
|
Economic shock |
0.094*** (0.028) |
0.071** (0.028) |
|
*** p<.01, ** p<.05, * p<.1 Standard errors in parentheses |
||
Table 4: Results of the Effect of Catastrophic Health Expenditures on the Household Labor Supply
Having presented the descriptive results, we present the results from the estimated IV model. On the basis of the empirical findings from Table 6 above, both models are significant overall at the 1% level, with a p value of 0.000. Catastrophic health spending is seen to have a significant effect on the number of hours a household is likely to offer for both thresholds. On average, when the budget share approach (10%) is used, the probability of households that incurred catastrophic health expenditures to supply labor is reduced by 5 percentage points compared with households that did not experience CHE at the same threshold. On the other hand, incurring catastrophic health costs at 40% reduces the probability of supplying additional hours of labor by 12 percentage points compared with households not incurring CHE at the same threshold while holding all other factors constant. With respect to the reviewed literature, this study finding is in line with those of Cai & Kalb (2006) and Mchenga et al. (2017) [11,15].
Under both thresholds (10% and 40%), if a household is headed by a male, the probability of that particular household offering additional hours of work in the labor market increases by 15% and 17%, respectively, compared with those households that are headed by females.
The probability of a household being headed by a divorced or separated individual offering additional hours of labor is as follows: to decrease by 16 and 14 percentage points compared with households with heads that are married for both the 10% and 40% thresholds, respectively, holding all other factors constant. This is due to the ability of married households to help each other in labor activities, unlike widowed and divorced households, which are, in most cases, female-headed households. Additionally, the emotional and psychological impact of losing a spouse could influence their motivation and capacity to engage in labor activities.
Residing in rural areas is, on average, seen to decrease the probability of a household having additional hours of work for the 10% CHE threshold. Under the 40% CHE threshold, residing in a rural area does not have any significant effect on the probability of a household reducing or increasing hours of work. This can be a result of rural areas having fewer employment opportunities than urban centers do. Limited job prospects may compel individuals in rural households to accept lower-paying or part-time jobs, leading to fewer hours worked overall; thus, most rural households are seen to be engaged in informal labor (ganyu) that is short lived. Moreover, most households in the rural setting rely on on-farm activities, which they mostly perform on their own land, and in some cases, work on other people’s farms for pay. Farm activities are seasonal, thus affecting their overall hours supplied compared with those of urban households.
The education qualifications of a household head under both thresholds are not found to have a significant effect on the probability of that particular household either supplying more or fewer hours of labor.
Discussion
The finding that CHEs reduce the probability of households supplying additional labor solidifies the fact that given exposure to health shocks, household members are constrained by health care giving activities in the case of sickness or injury of a household member making them reduce their hours of work. As CHEs become more severe (e.g., at the 40% threshold), the marginal utility of additional labor income diminishes. This is because the income earned might still not be sufficient to offset the rising healthcare costs, leading households to withdraw from labor markets entirely. This explains the higher reduction in labor supply probability (12 percentage points at 40%) compared to the lower threshold (5 percentage points at 10%).
Male headed households are seen to be more likely to offer additional hours of labor concretizes the idea that there could be disparities in access to employment opportunities or wage differentials on the basis of gender, leading to differential incentives for household heads to work longer hours. For example, if males have greater access to higher-paying jobs or positions with more opportunities for overtime, they may be more inclined to work longer hours than females are. Women often face caregiving responsibilities, such as looking after children, elderly family members, or the sick, which can limit their ability to work more hours. Therefore, even when financial pressures on the household increase, women may be unable to significantly increase their working hours [16,17].
Conclusion and Recommendations
The overall findings indicate that catastrophic health payments affect the number of hours a household supplies in the labor market. The results indicate that the probability of households supplying labor tends to decrease once they are subjected to catastrophic health care expenses at both thresholds. This finding complements the findings of Cai & Kalb (2006) and Lindelow & Wagstaff (2005) [15,18].
At the 40% threshold, households facing CHE are likely to have incurred relatively higher health expenses than their overall financial resources, as most of the households are from rural areas and are not able to earn more with their reliance on ganyu and their on-farm activities, which are mostly seasonal. Consequently, these households may be compelled to offer a significantly larger number of additional hours of labor to cover expenses. On the other hand, under the budget share approach (10%), households facing CHE under this approach may incur health costs that represent a smaller fraction of their overall financial resources. As a result, the additional hours of labor offered by these households may be comparatively less substantial, reflecting the lower impact of health expenses on their budgetary allocations.
The results, and on the basis of the literature, indicate that Malawi’s health care financing system is regressive, as low-income households have to pay more to access health care services, as shown by the introduction of user fees in most health care facilities. This means that, in terms of catastrophic health care expenditures, low-income households suffer a great deal in trying to cover their out-of-pocket health expenses; hence, they require much help and financial protection.
A general implication of these results is that household well-being is heavily influenced by the amount of labor that households can offer in the market, especially when faced with the financial burden of catastrophic health expenditure (CHE). This highlights the need for deliberate measures to protect low-income households from the negative effects of CHE. The study, therefore, recommends the implementation of policies that enhance financial protection for vulnerable groups. One such measure is the introduction of progressive taxation, which ensures that those with higher incomes contribute more to national revenue.
Limitations
The major limitation of this study is the homogenous nature of the data, since a large proportion of the sampled population was from a rural setting; thus, the study is more likely to be dictated by the characteristics of the rural households at the disadvantage of those in urban areas. The researcher also acknowledges that the instrument used may not be sufficiently strong in capturing the effect of CHE on households’ labor supply; therefore, the results of this paper need to be used with caution.
The data used in the study are publicly available at the World Bank website: Malawi - Fifth Integrated Household Survey 2019-2020 (worldbank.org)
References
- Browning, E. K., & Zupan, M. A. (2020). Microeconomics: Theory and applications. John Wiley & Sons.
- Becker, G. S. (1985). Human capital, effort, and the sexual division of labor. Journal of labor economics, 3(1, Part 2), S33-S58.
- Muurinen, J. M. (1982). Demand for health: a generalisedGrossman model. Journal of Health economics, 1(1), 5-28.
- Chirikos, T. N. (1993). The relationship between health and labor market status. Annual Review of Public Health, 14(1), 293-312.
- Balagopal, G. (2009). Access to health care among poor elderly women in India: how far do policies respond to women's realities?. Gender & Development, 17(3), 481-491.
- Onah, M. N., & Govender, V. (2014). Out-of-pocket payments, health care access and utilisation in south-eastern Nigeria: a gender perspective. PLoS One, 9(4), e93887.
- World Bank. (2024a). Analyzing Health Equity Using Household Survey Data. World Bank Institute Development Studies.
- World Bank. (2024b). World Bank Open Data. World BankOpen Data.
- Choi, J. W., Kim, T. H., Jang, S. I., Jang, S. Y., Kim, W. R., &Park, E. C. (2016). Catastrophic health expenditure according to employment status in South Korea: a population-based panel study. BMJ open, 6(7), e011747.
- Lee, H. J., Lee, D. W., Choi, D. W., Oh, S. S., Kwon, J., &Park, E. C. (2020). Association between changes in economic activity and catastrophic health expenditure: findings from the Korea Health Panel Survey, 2014–2016. Cost Effectiveness and Resource Allocation, 18, 1-9.
- Mchenga, M., Chirwa, G. C., & Chiwaula, L. S. (2017). Impoverishing effects of catastrophic health expenditures in Malawi. International journal for equity in health, 16, 1-8.
- Hamilton, J. D., & Waggoner, D. F. (2004). Normalization in econometrics.
- Nguyen, H. A., Ahmed, S., & Turner, H. C. (2023). Overview of the main methods used for estimating catastrophic health expenditure. Cost Effectiveness and Resource Allocation, 21(1), 50.
- Wagstaff, A. (2018). Catastrophic Medical Expenditures: Reflections on Three Issues. World Bank Policy Research Working Paper, (8651).
- Cai, L., & Kalb, G. (2006). Health status and labour force participation: evidence from Australia. Health economics, 15(3), 241-261.
- Bloom, D. E., Mahal, A., Rosenberg, L., & Sevilla, J. (2010).Economic security arrangements in the context of population ageing in India. International Social Security Review, 63(3â?4), 59-89.
- Wagstaff, A., & Doorslaer, E. V. (2003). Catastrophe and impoverishment in paying for health care: with applications to Vietnam 1993–1998. Health economics, 12(11), 921-933.
- Lindelow, M., & Wagstaff, A. (2005). Health Shocks in China: Are the Poor and Uninsured Less Protected? (SSRN Scholarly Paper 2894727).
- Blundell, R., Pistaferri, L., & Saporta-Eksten, I. (2016). Consumption inequality and family labor supply. American Economic Review, 106(2), 387-435.
- Bound, J., Schoenbaum, M., Stinebrickner, T. R., & Waidmann,T. (1999). The dynamic effects of health on the labor force transitions of older workers. Labour economics, 6(2), 179- 202.
- Stock, J. H., & Yogo, M. (2002). Testing for weak instruments in linear IV regression.




