Case Report - (2025) Volume 3, Issue 3
Diaphragmatic Injury with Hemothorax and Gastric Laceration Following Penetrating Thoracoabdominal Injury from Occupational Accident: A Case Report in Buea Regional Hospital
2Department of Surgery and specialties, Faculty of Health Sciences, University of Buea, Cameroon
3Buea Regional Hospital, South-West Region, Cameroon
Received Date: Sep 19, 2025 / Accepted Date: Oct 14, 2025 / Published Date: Oct 31, 2025
Copyright: ©©2025 Quincy-Jones Tchumukong Shumbang, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Shumbang Tchumukong, Q. J., Mokake, M., Tchuisseu Ngapjang, C. D., Lingo, P., Ambassa, M. E., et al. (2025). Diaphragmatic Injury with Hemothorax and Gastric Laceration Following Penetrating Thoracoabdominal Injury from Occupational Accident: A Case Report in Buea Regional Hospital. Ope Acce Jou Dis Glo Heal, 3(3), 01-05.
Abstract
Introduction: diaphragmatic injuries are relatively uncommon and they are life-threatening because of their associated injuries. Thoracoabdominal injuries account for up 15% of diaphragmatic injuries but in Cameroon in particular it is up to 18.1%. work accident related is just up to 14.8% of diaphragmatic injuries. In penetrating mechanism, the lesion is usually small with over 80% being smaller than 2cm. however, complication from misdiagnosis even for larger lesion size can be more life-threatening and as such, thorough initial evaluation with prompt intervention is very important for a better outcome particularly in low income countries.
Case presentation: A 40-year-old male referred with thoracoabdnimal ultrasound report of 2.89cc of homogenous anechoic fluid in the Morrison pouch, from a health facility about 30km to our services after he presented there with a bleeding wound on his left lateral lower chest and left posteriolateral arm following an occupational accident (was pierced by a sickle-shape knife). He arrived at our service in respiratory distress, hemorrhagic shock and generalized peritonitis. Fluid resuscitation was done, and a left emergency thoracotomy done and which collected 300cc of dark blood, analgesics and antibiotics were administered and visible ingested food particles were seen on the chest wound. A clinical diagnosis of acute respiratory distress and hypotension secondary to diaphragmatic injury with hemothorax and gastric laceration folloowing penetrating thoracoabdominal injury was made. He was immediately rush to the theatre for exploratory laparotomy. Which reviewed a 5cm left diaphragmatic injury and 12cm gastric laceration which were sutured and peritoneal and thoracic lavage done. He was transfused 1 unit of cross match whole blood and the chest tube was removed on day 10 post-operation.
Key Clinical Massage: Diaphragmatic injury should be suspected following penetrating thoracoabdominal injury, and life- threatening injuries such as hemothorax should always be address first with simple chest tube or standard thoracotomy. Imaging investigations, should not delay immediate surgical intervention in penetrating thoracoabdominal injury with hypotension/hemorrhagic shock.
Keywords
Penetrating Thoracoabdominal Injury, Diaphragmatic Injury, Hemothorax, Thoracotomy, Gastric Laceration, Occupational Accident
Introduction
Diaphragmatic injuries are relatively uncommon, representing less than 1% of traumatic injuries. However, they are life-threatening injuries because of their rate of associated injuries [1]. However, thoracoabdominal injuries account for up to 15% of diaphragmatic injuries as compared to abdominal contusion which contribute 1% to 7%. In penetrating tharacoabdominal injuries such as stabbed wounds, gunshots or any foreign object, the injury follows the tract of the object and is typically small, with over 80% being smaller than 2 cm to the diaphragm and this may often be undiagnosed and overlooked in the initial assessment [2-4]. Many hollow or solid organ structures can be injured as are in close proximity to the diaphragm because it wraps circumferentially around the abdominal wall. So it is very rare for a diaphragmatic injury to occur in isolation [5]. Complications from misdiagnosis can be life threatening and as such thorough initial evaluation with prompt intervention is very important for a better outcome particularly in low income countries.
This case report talks about an occupational hazard leading to penetrating thoracoabdominal injury with diaphragmatic and gastric laceration, referred from a rural health facility (Muyuka district hospital) located about 30km from our setting (Buea regional hospital).
Case Report
40-year-old male, who was referred from a health facility about 30km to our emergency unit following an occupational accident, he was harvesting palm fruits, when the sickle knife got stock and give way from the woody extension end. While he was attempting to mount another extension on the ground, the stocked knife got dislodges from the palm tree and lacerate his left posteriolateral arm and pierces him on the left lateral chest. With the fright and agitation, the attached distal woody end weighted with gravity and this spontaneously forced the curved knife off his body.
He was rush to Muyuka district hospital where he was administered 1000cc of normal saline 0.9% flush and maintain with 500cc every 8hours. Ceftriaxone 2g injectable intravenously start, then, 1g every 12hours, tramadol 100mg start and diclofenac 75mg start intravenously and intramuscularly respectively. The laceration on the left arm was sutured and that on the chest was approximated with sutures and a circumferential compressive chest dressing was done and no chest tube was placed.
Thoracoabdominal ultrasound was done which reported, 2.89cc homogenous anechoic fluid in the Morrison’s pouch and both left and right plural spaces were free and a rib fracture was suspected and this prompted his referred to our service (Buea regional hospital) on arrival to our services, which took about 3hours from time of the injury.
His airway was patent, oxygen saturation was 97% on room air, respiratory rate was 14 breaths per minutes, his blood pressure was 88/62mmHg, pulse of 95bpm, Glasgow coma scale was 15/15 and glycaemia was 110mg/dl. He had difficulty in breathing with intercostal recession worse on deep inspiration and periumbilical pain. He was calm and moderate pallor on the palms. The was decreased breath sound on left lung field and moderate periumbilical and epigastric tenderness. His last meal was fufu and eru. As initial emergency management, two intravenous lines were set with cannula size 18, he was flush 1500cc of normal saline 0.9%. then 500cc every 6hours.
An emergency thoracotomy was done on the left chest which drained about 300cc of dark red blood. The circumferential compressed chest dressing was removed and an oblique approximated sutured laceration on the 7th intercostal space from the left midaxillary to the posterior axillary line measuring about 8cm. it was draining dark blood and visible food particles (strands of eru) on the wound. The wound was immediate packed and compressive dressing done.
Diagnosis
Blood was immediately collected for full blood count and blood group and cross match 2units of whole blood.
Analgesics; paracetamol 1g intravenously every 6 hours, tramadol 100mg intravenously every 8 hours
Antibiotherapy; ceftriaxone 1g intravenously every 12 hours and metronidazole 500mg intravenously every 8 hours, single dose of anti-tetanus serum 1500IU subcutaneously and the general surgeon was called.
Patient was urgently taken to the theatre for exploratory laparotomy; under general anesthesia. Were a midline incision was made from the xphoid process to beneath the umbilicus. The peritoneal cavity was exposed, the was 5cm left hemi-diaphragmatic laceration (figure 1, video 1) and a 12cm laceration at the medio-lateral side of the greater curvature of the stomach were identified along with contamination of the left hemithorax and abdominal cavity with stomach content of vegetables (eru) and chewed cowhide.
Diaphragmatic injury with hemothorax and gastric laceration following penetrating thoracoabdominal injury from occupational accident: A case Report in Buea Regional Hospital
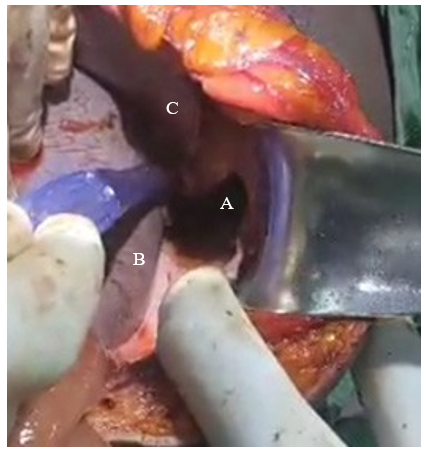
Figure 1: Intraoperative Findings; A) Diaphragmatic Laceration, B) Spleen and C) Liver
The stomach laceration was sutured with vicryl 3-0 and graham patch was done. Extensive peritoneal and thoracic lavage was done. The diaphragm was sutured with silk 0 and abdominal wall was also closed. The traumatic chest wound was opened, washed and closed with silk 0. Intraoperatively, he was transfused 1 unit of cross matched whole blood. The patient was transfer to the male surgical ward for follow-up. Chest tube drain was removed on day 10.
Discussion
The circumstance of the injury and nature of the instruments has an important role to play and much consideration when initial evaluation is being done. They are major two types of injury pattern; blunt or penetrating. G.A. Bange et al in 2022 in Cameroon reported that, diaphragmatic injuries from thoracoabdominal trauma is 18.1%. Penetrating mechanism account for up 59.3% and work accident related is just 14.8%. it is usually not uncommon to have an associated thoracic or abdominal organ injury. It can be a simple lung contusion, herniation of abdominal organs into the thoracic cavity and possible laceration of abdominal solid and hollow viscus with it content leaking into the thoracic cavity which intend worsen the prognosis and increasing the rate of mortality [6]. By using the pathophysiology of occurrence, based on organ injury scaling committee, the American association for the surgery of trauma classify diaphragmatic injury into five grades (Table 1); Grade I with contusion; Grade II with lacerations of less than 2cm; Grade III, more extensive lacerations of 2-10cm; Grade IV that involve laceration greater than 10cm with evident tissue loss of less than 25cm2 and Grade V that involve lacerations with more tissue loss of 25cm2 and above. Literature reveals that penetrating wounds are the most prevalent causes of diaphragmatic injuries, but are often overlooked due to the smaller size of the wounds (about 80% has wound size <2cm) [7]. But this was different in our case as we had a 5cm diaphragmatic laceration (Grade III).
|
Diaphragm Injury Scale |
|
|
Grade* |
Description of injury |
|
I |
Contusion |
|
II |
Laceration ≤2cm |
|
III |
Laceration 2-10cm |
|
IV |
Laceration >10cm with tissue loss (≤25cm2) |
|
V |
Laceration with tissue loss >25cm2 |
|
*Advance one grade for bilateral injuries up to grade III |
|
Table 1: Diaphragmatic Injury Scale (from Moore EE et al. Organ Injury Scaling IV. Thoracic Vascular, Lungs, Cardiac and Diaphragm. J Trauma 1994 Mar;36 (3):299-300)
The clinical presentation of diaphragmatic injury, is sometime difficult particularly for penetrating injuries which majority of them are quite small, hence most patient will present with pleural discomfort, shortness of breath, chest pain due to mostly diaphragmatic hernias and obstructive symptoms in strangulated herniation. But our case was unique with the fact we had a thoracic injury with visible gastric content through it.
Urgent imaging in thoracoabdominal injury is very important as it is used for early recognition and determination of the nature of all injuries. The imaging modality will depend on the clinical findings which is best evaluated with Advanced Trauma Life Support (ATLS) protocol. It is important to note that it is not rare to missed diaphragmatic injury on clinical examination, Extended Focused Assessment with Sonography in Trauma (EFAST) scan or mobile plain chest X-ray [8]. CT scan is the gold standard for penetrating diaphragmatic injury, which can show direct discontinuity of the hemidiaphragm with a sensitivity of 17-80% and specificity of 90-100%. It may be seen with or without intrathoracic herniation of abdominal contents [9]. It is worth noting that, penetrating thoracoabdominal injury with hemodynamic instability warrant and emergency surgical intervention without delay for imaging. Due to recent technological advancements, surgical techniques are invasive and minimal invasive; however invasive (laparotomy and or thoracotomy) remains the emergency plan. Laparotomy is highly recommended as it identify source and stopping intra- abdominal bleeding and peritonitis, suturing wounds of hollow and parenchymal organs as it was in our case, draining the small intestine, and abdominal cavity lavage, however, emergency thoracotomy is indicated when there is damage to the heart and main vessels: large and total hemothorax, hemopericardium and cardiac tamponade, hemomediastium with compression of the airways and main blood vessels. Also with rupture trachea and large bronchi [10].
Conclusion
Diaphragmatic injury should be suspected following penetrating thoracoabdominal injury, life threatening conditions such as hemothorax and hypotension/hemorrhagic shock are frequently common, hence imaging investigations should not delay immediate surgical intervention such as emergency thoracotomy and exploratory laparotomy in patient with acute respiratory distress and hypotension following penetrating thoracoabdominal injury with hemothorax, diaphragmatic and gastric laceration [11- 13].
Consent
Written informed consent was obtained from the patient for publication of this case report and the accompany images.
Competing Interests
The authors declare that they have no competing interests.
Authors Contributions
Quincy-jones TCHUMUKONG SHUMBANG contributed to case conceptualization, data collection, formal analysis and writing of manuscript. Martin MOKAKE conducted extensive literature reviews, data collection and editing of manuscript. Christian Damien TCHUISSEU NGAPJANG reviewed the paper. Philippe Albert LINGO reviewed the paper. Marc EFFILA AMBASSA reviewed the paper. Bertolt Brecht NTEUNGUE KOUAM reviewed the paper. BRINYUY NYUYDZEFON collected data. Ronald GOBINA reviewed literature review. VERLA Vincent SIYSI editing of manuscript.
Acknowledgements
The contribution of the emergency, theatre and surgical unit team of Buea Regional Hospital.
References
- Gooseman, M. R., Rawashdeh, M., Mattam, K., Rao, J. N., Vaughan, P. R., & Edwards, J. G. (2019). Unifying classification for transdiaphragmatic intercostal hernia and other costal margin injuries. European Journal of Cardio- Thoracic Surgery, 56(1), 150-158.
- Abdellatif, W., Chow, B., Hamid, S., Khorshed, D., Khosa, F., Nicolaou, S., & Murray, N. (2020). Unravelling the mysteries of traumatic diaphragmatic injury: an up-to-date review. Canadian Association of Radiologists Journal, 71(3), 313- 321.
- Kokatnur L, Rudrappa M. Diaphragmatic Palsy. Diseases. 2018 Mar;6(1):16.
- Martin, M. J., Brown, C. V., Shatz, D. V., Alam, H. B., Brasel,K. J., Hauser, C. J., ... & Inaba, K. (2018). Evaluation and management of abdominal stab wounds: a Western Trauma Association critical decisions algorithm. Journal of Trauma and Acute Care Surgery, 85(5), 1007-1015.
- Williams, M., Carlin, A. M., Tyburski, J. G., Blocksom, J. M., Harvey, E. H., Steffes, C. P., & Wilson, R. F. (2004). Predictors of mortality in patients with traumatic diaphragmatic rupture and associated thoracic and/or abdominal injuries. The American surgeon, 70(2), 157-163.
- Bang, G. A., Motto, G. B., Yamben, M. A. N., Chappi, C.T., Chopkeng, J. C., Biwole, D. B., & Nonga, B. N. (2022). Traumatic Rupture of the Diaphragm: Retrospective Study of 27 Cases Operated in Three Hospitals in Yaoundé (Cameroon). Surgical Science, 13(4), 207-215.
- Moore, E. E., Malangoni, M. A., Cogbill, T. H., Shackford,S. R., Champion, H. R., Jurkovich, G. J., ... & Trafton, P.G. (1994). Organ injury scaling iv: thoracic vascular, lung, cardiac, and diaphrag. Journal of Trauma and Acute Care Surgery, 36(3), 299-300.
- Radswiki, T. (2024). Diaphragmatic rupture | Radiology Reference Article.
- Keyes, S., Spouge, R. J., Kennedy, P., Rai, S., Abdellatif, W., Sugrue, G., ... & Murray, N. (2024). Approach to acute traumatic and nontraumatic diaphragmatic abnormalities. Radiographics, 44(6), e230110.
- Yahyoev, S. O., & Khodzhimatov, G. M. (2022). Diagnostic methods and surgical treatment of patients with thoracoabdominal traumas (review of the literature). Kardiochirurgia i Torakochirurgia Polska/Polish Journal ofThoracic and Cardiovascular Surgery, 19(4), 226-231.
- Pumarejo Gomez L, Tran VH. Hemothorax. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 [cited 2024 Aug 5].
- Goligher, E. C., Brochard, L. J., Reid, W. D., Fan, E., Saarela, O., Slutsky, A. S., ... & Ferguson, N. D. (2019). Diaphragmatic myotrauma: a mediator of prolonged ventilation and poor patient outcomes in acute respiratory failure. The Lancet Respiratory Medicine, 7(1), 90-98.
- Uhlich, R., Kerby, J. D., Bosarge, P., & Hu, P. (2018). Diagnosis of diaphragm injuries using modern 256-slice CT scanners: too early to abandon operative exploration. Trauma Surgery & Acute Care Open, 3(1).