Research Article - (2025) Volume 4, Issue 3
Cardiovascular Sequelae of COVID-19: A Narrative Review on Myocarditis, Microthrombosis, and Beyond
Received Date: Jun 16, 2025 / Accepted Date: Jul 11, 2025 / Published Date: Jul 18, 2025
Copyright: ©©2025 Brendan Jones. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Jones, B. (2025). Cardiovascular Sequelae of COVID-19: A Narrative Review on Myocarditis, Microthrombosis, and Beyond. Biomed Sci Clin Res, 4(3), 01-04.
Abstract
Background SARS-CoV-2 infection has been linked to both acute and long-term cardiovascular (CV) complications.
Objective Provide a narrative synthesis of evidence on cardiac remodeling, myocarditis, arrhythmia, microthrombosis, and heart failure following COVID-19.
Methods We reviewed PubMed-indexed clinical and epidemiologic studies (2020–2025) addressing post-acute CV complications.
Results COVID-19 survivors face elevated risks of myocarditis (~6×), arrhythmias (~1.6×), and heart failure (1.7–2×) even after mild disease [1-3]. Endothelial dysfunction, microthrombi, direct myocardial injury, and inflammation underpin these sequelae [3-5]. CMR studies in athletes show low prevalence of clinically relevant myocarditis (~1–3%), with subclinical fibrosis in a minority [6-8].
Conclusions Persistent CV sequelae after COVID-19 are prevalent and clinically relevant; surveillance with imaging, biomarkers, and guideline-based therapy is imperative.
Keywords
COVID-19, Myocarditis, Microthrombosis, Cardiac Remodeling, Arrhythmia
Introduction
SARS-CoV-2 targets the CV system via ACE2 receptors, provoking systemic inflammation, endotheliitis, and thrombotic microangiopathy [1, 2]. Although acute cardiac injury during hospitalization is well-characterized, long-COVID cardiovascular sequelae—including myocarditis, arrhythmias, and heart failure— persist in survivors [1, 3-9].
Pathophysiological Mechanisms
• Endothelial dysfunction & microthrombosis: Microthrombi are frequently observed in cardiac microvasculature, distinct from typical coronary thrombi, contributing to ischemia and remodeling [3, 5, 10].
• Direct myocardial injury: Viral infiltration and cytokine-mediated damage trigger myocarditis, fibrosis, and dysautonomia [2, 7, 11].
• Chronic inflammation: Persistent immune activation may potentiate arrhythmia and autonomic dysfunction [1, 4, 7].
Clinical Sequelae
Myocarditis & Remodeling
Post-COVID myocarditis risk increases six-fold relative to controls [1]. CMR studies in athletes found ~1–3% with myocarditis; a small subset showed subclinical fibrosis up to 6 months post-infection [6-8, 12]
Arrhythmias
Arrhythmia incidence is ~1.6 times higher [1, 3]. Potential mechanisms include inflammation, fibrotic remodeling, and autonomic dysregulation [4, 7].
Heart Failure
Risk of new-onset heart failure increases by ~1.7–2 times [1, 3]. Studies using large health databases report sustained elevated risk for up to 12 months [1, 9].
Epidemiology & Risk Stratification

Microthrombosis & Ischemic Injury
Autopsy and imaging studies confirm microthrombi as a major driver of myocardial necrosis [3, 10]. These vascular insults aggravate long-term cardiac dysfunction.
Diagnostic & Monitoring Recommendations
• CMR: Gold standard; essential for diagnosing myocarditis and fibrosis, particularly in athlete [6-8].
• Biomarkers/ECG/Echo: Troponin, NT-proBNP, D-dimer, ECG, echo to monitor those with symptoms or high risk [3, 9].
• Longitudinal Surveillance: Healthcare systems should incorporate CV follow-up into post-COVID care pathways [1].
Management Strategies
• Medical Therapy: ACE-I/ARB, beta-blockers, diuretics per myocarditis/heart failure guidelines. [1, 4]
• Anticoagulation: Consider in high-risk microthrombotic cases (persistent D-dimer elevation). [3, 11]
• Return-to-Play (RTP): For athletes with myocarditis, restrict activity 3–6 months; RTP only after negative CMR and normalized biomarkers.[12, 13]
Future Research Directions
• Longitudinal registries to track CV outcomes and arrhythmic events. [6, 12]
• Clinical trials targeting endothelial repair and antithrombotic therapy. [3, 10]
• Research into dysautonomia and microvascular dysfunction in persistent symptoms. [4, 7]

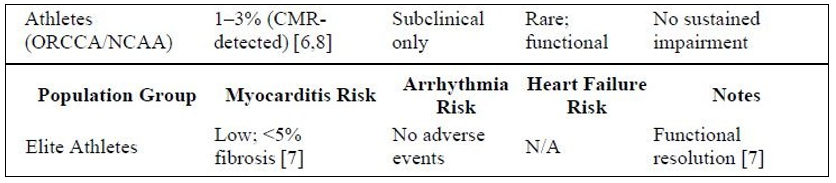
Table 1: Summary of Post-COVID Cardiovascular Risk by Population
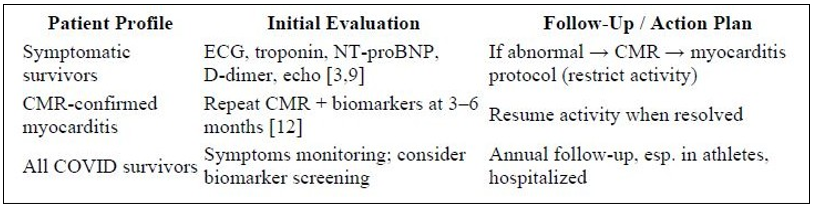

Table 2: Diagnostic & Management Algorithm for Post-COVID Cardiovascular Sequelae
Conclusion
COVID-19 poses a lasting threat to cardiovascular health, manifested in myocarditis, arrhythmias, heart failure, and microvascular damage. Evidence supports structured surveillance, targeted imaging, and adherence to management protocols. Integration of cardiopulmonary care into long-COVID pathways is critical to mitigating morbidity in survivors, particularly among high-risk groups [14].
Author Disclosures
Author Contributions
I, Brendan Jones, conceptualized the review, conducted the literature search, synthesized the findings, and wrote the manuscript.
Conflict of Interest
The author declares no conflicts of interest. Funding: No external funding was received for this work.
Use of AI Tools
This manuscript was prepared with the assistance of AI language models to enhance clarity, grammar, and structure. All intellectual content, critical analysis, and interpretation of data remain the sole responsibility of the author.
References
- Xie, Y., Xu, E., Bowe, B., & Al-Aly, Z. (2022). Long-term cardiovascular outcomes of COVID-19. Naturemedicine, 28(3), 583-590.Crook, H., Raza, S., Nowell, J., Young, M., & Edison,P. (2021). Long covid—mechanisms, risk factors, andmanagement. bmj, 374.
- Kawai, K., Gianatti, A., ... & Finn, A. V. (2021). Microthrombi as a major cause of cardiac injury in COVID-19: a pathologic study. Circulation, 143(10), 1031-1042.
- Pellegrini, D., Kawakami, R., Guagliumi, G., Sakamoto, A.,Kawai, K., Gianatti, A., ... & Finn, A. V. (2021). Microthrombi as a major cause of cardiac injury in COVID-19: a pathologic study. Circulation, 143(10), 1031-1042.
- Nalbandian, A., Sehgal, K., Gupta, A., Madhavan, M. V., McGroder, C., Stevens, J. S., ... & Wan, E. Y. (2021). Post-acute COVID-19 syndrome. Nature medicine, 27(4), 601-615.
- Aono, J., Kikuchi, K., Higashi, H., Saito, M., & Sumimoto, T. (2016). Epigastric and chest pain in celiac artery dissection: spontaneous isolated dissection of the celiac trunk. European Heart Journal-Cardiovascular Imaging, 17(3), 315-315.
- Petek, B. J., Moulson, N., Drezner, J. A., Harmon, K. G.,Kliethermes, S. A., Churchill, T. W., ... & Baggish, A. L. (2022). Cardiovascular outcomes in collegiate athletes after SARS-CoV-2 infection: 1-year follow-up from the outcomes registry for cardiac conditions in athletes. Circulation, 145(22), 1690-1692.
- Lim, K., Yang, J. H., Miranda, W. R., Chang, S. A., Jeong,D. S., Nishimura, R. A., ... & Oh, J. K. (2021). Clinical significance of pulmonary hypertension in patients with constrictive pericarditis. Heart, 107(20), 1651-1656.
- Daniels, C. J., Rajpal, S., Greenshields, J. T., Rosenthal, G. L., Chung, E. H., Terrin, M., ... & Big Ten COVID-19 Cardiac Registry Investigators. (2021). Prevalence of clinical and subclinical myocarditis in competitive athletes with recent SARS-CoV-2 infection: results from the big ten COVID-19 cardiac registry. JAMA cardiology, 6(9), 1078-1087.
- Jones, B. (2025). Cardiovascular Sequelae of COVID 19: A Narrative Review on Myocarditis, Microthrombosis, and Beyond.
- Jones, B. Cardiovascular Sequelae of COVID-19: A Narrative Review on Myocarditis, Microthrombosis, and Beyond Author.
- Turner, S., Naidoo, C. A., Usher, T. J., Kruger, A., Venter, C., Laubscher, G. J., ... & Pretorius, E. (2024, March). Increased levels of inflammatory and endothelial biomarkers in blood of long COVID patients point to thrombotic endothelialitis. In Seminars in thrombosis and hemostasis (Vol. 50, No. 02, pp. 288-294). Thieme Medical Publishers, Inc.
- Kim, J. Y., Han, K., & Suh, Y. J. (2021). Prevalence of abnormal cardiovascular magnetic resonance findings in recovered patients from COVID-19: a systematic review and meta-analysis. Journal of Cardiovascular Magnetic Resonance, 23(1), 100.
- Mack, M. J., & Adams, D. H. (2023). Avoidance of patient prosthesis mismatch after aortic valve replacement: have we been too aggressive?. Journal of the American College of Cardiology, 81(10), 976-978.
- Sperhake, J. P. (2020). Autopsies of COVID-19 deceased?Absolutely!. Legal Medicine, 47, 101769.



