Research Article - (2025) Volume 10, Issue 2
Bilharzial Appendicitis Caused by Schistosoma Mansoni: A Case Report from the Democratic Republic of Congo
2Department of Pathological Anatomy and Digestive Surgery, University of Kinshasa, CHE IME KIMPESE DR, Congo
3Department of Pathological Anatomy and Digestive Surgery, University of Kinshasa, DRC, Congo
4University of Kinshasa and CHE IME Kimpese, Kongo Central, DRC, Congo
5Service of Pathological Anatomy, CHU Renaissance and University of Kinshasa, Kinshasa, DRC, Congo
6Department of Pathological Anatomy and Digestive Surgery, University of Kinshasa, DRC, Congo
Received Date: Sep 15, 2025 / Accepted Date: Oct 13, 2025 / Published Date: Oct 17, 2025
Copyright: ©2025 Simplice Kanza. is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Kanza, S., Bobanga, T., Veyi, D., Makola, G., Badianjile, M., et al. (2025). Bilharzial Appendicitis Caused by Schistosoma Mansoni: A Case Report from the Democratic Republic of Congo. Int J Cancer Res Ther, 10(2), 01-03.
Abstract
Appendicitis is one of the most frequent inflammations of the digestive tract and is usually treated surgically. Appendectomy is among the most common surgical procedures worldwide, in- cluding in the Democratic Republic of Congo (DRC). However, in most cases, appendectomy specimens are not sent to pathology laboratories but are instead discarded, limiting the confirmation of histopathological causes of appendicitis. Among the rare etiolo- gies, Schistosoma mansoni is known to cause chronic appendicitis in endemic regions.
Key clinical message
Histopathological examination of appendectomy specimens remains crucial in endemic areas, as rare cases of Schistosoma mansoni-re- lated appendicitis may be overlooked. Systematic analysis ensures accurate diagnosis and guides postoperative antiparasitic therapy.
Introduction
Appendicitis is one of the most frequent inflammations of the digestive tract and is usually treated surgically. Appendectomy is among the most common surgical procedures worldwide, in- cluding in the Democratic Republic of Congo (DRC). However, in most cases, appendectomy specimens are not sent to pathology laboratories but are instead discarded, limiting the confirmation of histopathological causes of appendicitis. Among the rare etiolo- gies, Schistosoma mansoni is known to cause chronic appendicitis in endemic regions.
Case History and Examination
We report the case of a 22-year-old female who presented to the Surgery Department of CHE IME Kimpese, Kongo Central Prov- ince, with intermittent pain in the right iliac fossa and periumbil- ical region, fever, nausea, vomiting, diarrhea, and cramps in the right lower limb. Her medical history revealed that symptoms had persisted for 10 days. Initial management at home with vermox and indomethacin suppositories was unsuccessful. On examina- tion, her blood pressure was 110/80 mmHg, temperature 36.3°C respiratory rate 18/min, and heart rate 90 bpm. She appeared ill, with abdominal tenderness in the right iliac fossa and periumbil- ical region, with guarding and a positive Rovsing sign. A diagno- sis of acute appendicitis associated with intestinal parasitosis was suspected.
Differential Diagnosis, Investigations and Treatment
Laboratory results showed leukocytosis with significant eosino- philia. Direct stool examination revealed yeast, but stool concen- tration by the Kato Katz technique was not performed. Abdominal ultrasound was not carried out due to financial constraints. The pa- tient underwent surgery, and the appendectomy specimen was sent to the Pathology Department of CHU Renaissance. Histopatholog- ical analysis demonstrated calcified Schistosoma mansoni eggs in the lamina propria and submucosa of the appendix wall (Figure.1). The patient received praziquantel (Biltricide) 3 tablets as a single dose after surgery. Follow-up was favorable with complete reso- lution of symptoms and no complications at 1 month. Stool exam- ination at 3 months was negative for parasites.
Figure 1: Appendectomy Specimen
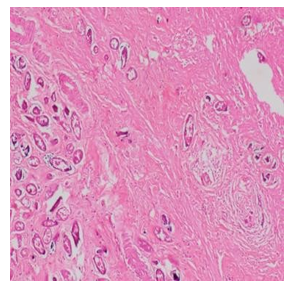
Figure 2: Calcified Schistosoma Mansoni Eggs Stained with Hematoxylin and Eosin (H&E).
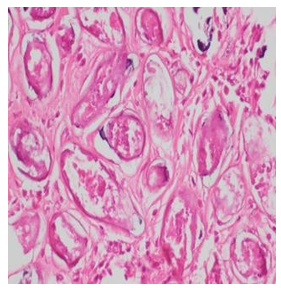
Figure 3: Schistosoma Mansoni Eggs Stained with H&E
Conclusion and Results (Outcome and Follow-Up)
The postoperative course was uneventful, and the patient fully re- covered after treatment with praziquantel. This case highlights the importance of histopathological analysis of appendectomy spec- imens in endemic regions, as it allows the detection of rare but significant etiologies such as Schistosoma mansoni.
Discussion
Bilharzial appendicitis is a rare clinical entity. Few cases have been reported in the literature, including cases in Burkina Faso, Senegal, and Madagascar. The World Health Organization rec- ognizes schistosomiasis as the second most widespread parasitic disease after malaria. Endemic areas include the Nile Valley, West and Southern Africa, parts of Madagascar, and the Democratic Re- public of Congo, particularly Kimpese. Our case emphasizes the need to always consider parasitic etiologies in endemic regions, especially in young adults, and to send all appendectomy speci- mens for histopathological analysis.
Patient Consent
Written informed consent was obtained from the patient for publi- cation of this case report and accompanying images, in accordance with the journal’s patient consent policy.
References
- Tchouanguem, H. N., Fouelifack, F. Y., Keugoung, B., Foueli- fa, L. D., & Moyou, R. S. (2016). Current status of schisto- somiasis in Santchou health area,(Santchou Health District, Cameroon western region). The Pan African Medical Journal, 24, 137-137.
- Dakoni, N., Saotoing, P., Tchawe, R., Koe, V., Ndikwé, J. L., Nlôga, A. N., & Somo, R. M. (2015). Epidemiological survey on schistosomiasis caused by Schistosoma haematobium and Schistosoma mansoni in primary schools in the Sub-Division of Taïbong-Dziguilao, Far-North Region Cameroon. Journal of Applied Biosciences, 90, 8397-8407.
- Njiokou, F., Onguene, A. O., Tchuente, L. T., & Kenmogne,A. (2004). Schistosomose urbaine au Cameroun. Bull. Soc. Pathol. Exot, 97(1), 37-40.
- Wambui, C. W., Madinga, J., Ashepet, M. G., Anyolitho, M. K., Mitashi, P., & Huyse, T. (2024). Knowledge, attitudes and practices toward female genital schistosomiasis among com- munity women and healthcare professionals in Kimpese re- gion, Democratic Republic of Congo. PLOS Neglected Tropi- cal Diseases, 18(7), e0011530.
- Linsuke, S., Nundu, S., Mupoyi, S., Mukele, R., Mukunda, F., Kabongo, M. M., ... & Lutumba, P. (2014). High Prevalence of Schistosoma mansoni in Six Health Areas of–Kasansa Health Zone, Democratic Republic of the Congo. PLoS ne- glected tropical diseases, 8(12), e3387.
- Thiam, I., Doh, K., Seck, M., Kammoun, C., & Woto Gaye,G. (2020, May). Appendicitis schistosomiasis. In Annales de Pathologie (Vol. 40, No. 5, pp. 411-413).
- Petri, D., Baglietto, L., Tavoschi, L., Mazzilli, S., Cocco, N., Ranieri, R., ... & Mavrou, J. (2023). Evaluating vaccine and health literacy in european prisons: A cross-sectional study. In 17th World Congress on Public Health Supplemental material Vol. 5.
- Guiguen, C., Autier, B., Gangneux, J. P., & Chabasse, D.(2021). Coprologie parasitaire: conduite de l’examen et pièges diagnostiques. Revue Francophone des Laboratoires, 2021(529), 32-42.
- Freer, J. B., Bourke, C. D., Durhuus, G. H., Kjetland, E. F., & Prendergast, A. J. (2018). Schistosomiasis in the first 1000 days. The Lancet Infectious diseases, 18(6), e193-e203.
- Ciddio, M., Mari, L., Sokolow, S. H., De Leo, G. A., Casa- grandi, R., & Gatto, M. (2017). The spatial spread of schis- tosomiasis: A multidimensional network model applied to Saint-Louis region, Senegal. Advances in water resources, 108, 406-415.
- Verjee, M. A. (2019). Schistosomiasis: still a cause of signifi- cant morbidity and mortality. Research and reports in tropical medicine, 153-163.
- Perez-Saez, J., Mande, T., & Rinaldo, A. (2019). Space and time predictions of schistosomiasis snail host population dy- namics across hydrologic regimes in Burkina Faso. Geospa- tial health, 14(2).
- Broadway, K. M. (2018). Novel Perspectives on the Utiliza- tion of Chemotactic Salmonella Typhimurium VNP20009 as an Anticancer Agent.
- SIDIBE, M. (2018). Appendicite Aigue Chez L’enfant Dans Le Service De Chirurgie Pediatrique Du Chu Gabriel Toure (Doctoral dissertation, USTTB).
- Diarra, C. B. (2020). Appendicite aiguë au CSRéf de Ouéléssébougou (Doctoral dissertation, Université des Sci- ences, des Techniques et des Technologies de Bamako).
- DILAI, M. O. (2009). Les appendicites aiguës: étude rétro- spective sur 562 cas.
- Helmy, A. H., Magdi, M., Sabri, T., & Abou Shousha, T. (2000). Appendicitis; appendectomy and the value of endemic parasitic infestation. The Egyptian Journal of Surgery, 19(2), 87-91.
- Roth, G. A., Abate, D., Abate, K. H., Abay, S. M., Abbafati, C., Abbasi, N., ... & Borschmann, R. (2018). Global, region- al, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systemat- ic analysis for the Global Burden of Disease Study 2017. The lancet, 392(10159), 1736-1788.