Review Article - (2025) Volume 10, Issue 2
Transformation of Victorian Community Forensic Mental Health Services: Past, Present & Future
2Centre for Forensic Behavioural Science, Swinburne University of Technology, Australia
Received Date: May 29, 2025 / Accepted Date: Jun 20, 2025 / Published Date: Jan 27, 2025
Copyright: ©Â©2025 Sobia Khan, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Khan, S., Young, M., Furness, T. (2025). Transformation of Victorian Community Forensic Mental Health Services: Past, Present & Future. Int J Psychiatry, 10(2), 01-09.
Abstract
The Victorian Institute of Forensic Mental Health (Forensicare) community forensic mental health service (CFMHS) provides forensic mental health services to consumers with severe mental illness who are involved, or at risk of being involved, with the justice system. This narrative review aimed to provide an overview of the Forensicare CFMHS evolution since 2007 and describes the current provisions and future pathways of the service. The review identified several programs currently offered by the CFMHS, highlighting a significant expansion in service provision over the past 17 years and considers these changes in line with the Royal Commission into Victoria’s Mental Health System, the Mental Health Act (2014), and the Mental Health and Wellbeing Act (2022). The review provides an overview of the changes to the delivery of forensic mental health services in the State of Victoria and presents a revised service model and model of care, the Community Forensic Integrative Service (CFIS) Model. A significant gap exists in the available academic literature, evidenced through the absence of published program evaluations. The review concludes that empirical research evaluating the CFMHS in Victoria should be a priority.
Keywords
Forensic, Mental Health, Community, Programs, Intervention, Victoria
Abbreviations
Crimes Act 1997 (Mental Impairment and Unfitness to be Tried) (CMIA)
Community Forensic Mental Health Service (CFMHS)
Community Forensic Integrative Service (CFIS)
Mental Health Program (MHP)
Problem Behaviour Program (PBP)
Non-Custodial Supervision Order (NCSO)
Area Mental Health Services (AMHS)
Area Mental Health and Wellbeing Services (AMHWS)
Forensic Clinical Specialist Program (FCSP)
Coping with Child Exploitation Material Use (CEM-COPE)
Forensicare Serious Offender Consultation Service (F-SOCS)
Community Treatment and Transition (CTT)
Victorian Fixated Threat Assessment Centre (VFTAC)
Forensic Mental Health Implementation Plan (FMHIP)
Mental Health Advice and Response Service (MHARS)
Regional Community Forensic Mental Health Services (RFMHS)
Introduction
Forensic mental health services represent the intersection between mental health services and the criminal justice system [1]. These services assess and treat individuals with mental illness who are involved with, or at risk of being involved with the criminal justice system [2, 3]. Since 1998, the Victorian Institute of Forensic Mental Health, operating as Forensicare, is the publicly funded state-wide responsible authority for the provision of forensic mental health services in prison, inpatient, and community settings [4, 5]. In the Australian state of Victoria, under the Crimes Act 1997 (Mental Impairment and Unfitness to be Tried - CMIA), upon a finding of not guilty by reason of mental impairment an individual is considered a ‘forensic patient’ and will be received by Forensicare [3, 6]. The court can impose either a custodial or non-custodial supervision order. Forensic patients, referred to henceforth as consumers, on custodial supervision orders are held within the Forensicare inpatient mental health facility. Consumers on non-custodial supervision orders or consumers who have been granted extended leave from their custodial supervision orders are involved with the Forensicare Community Forensic Mental Health Services (CFMHS).
A 2007 review described CFMHS in Australia, of which a description of Victoria’s CFMHS was outlined [7]. Until 2007, clinical services at the Forensicare CFMHS were provided through two programs: The Mental Health Program (MHP) and the Problem Behaviour Program (PBP). Subsequent research identified development of forensic mental health services in Victoria comprising two additional programs within the Forensicare CFMHS; Court Services Program; Community Integration Program [8]. Since then, Victoria’s publicly funded mental health system has undergone expansion and restructure and the CFMHS is now embarking on a revision of service provision including the current service model and model of care. Therefore, the objective of the current review was to build on previous work by describing the transformation of the CFMHS through description of past, present, and future innovations. The aims of this review were to:
(1) provide an overview of Victoria’s CFMHS transformation since 2007;
(2) describe current provisions of the CFMHS; and
(3) outline the road ahead of the CFMHS.
Evolution of Community Forensic Mental Health in Victoria
The current review identified diversity in models of care, clinical services, and interventions currently provided by the Forensicare CFMHS since 2007 (see Figures 1, 2). To demonstrate the evolution of the Forensicare CFMHS and how this was influenced by legislation and evaluation, we present a chronological timeline of events; Court Services Program; Non-Custodial Supervision Order Program; Forensic Clinical Specialist Program; Mental Health Act 2014; Problem Behaviour Program; Coping with Child Exploitation Material Use; Forensicare Serious Offender Consultation Service; Community Treatment & Transition; Victorian Fixated Threat Assessment Centre; Court based Mental Health Advice & Response Service; Royal Commission into Victoria’s Mental Health System; Mental Health Act and Wellbeing 2022; Forensicare Strategic Plan and Model of Care 2021-26; Regional Community Forensic Mental Health Services; Community Forensic Disability Mental Health Service (Glaser Clinic).


Court Services Program (2007)
The Court Services Program was developed to assist all levels of courts in Victoria with the sentencing of people with diverse mental health, intellectual disability and other issues through pre-sentence assessment and report preparation by psychologists and psychiatrists [8]. However, there are no current reports or evaluations to determine efficacy of the program to meet its stated objectives.
Non-Custodial Supervision Order Program (2007) Consumers on a non-custodial supervision order (NCSO) have this order supervised by Forensicare, with treatment undertaken by local area mental health services (AMHS) or in extremely rare cases, a private practitioner [3]. The NCSO Program was developed at the Forensicare CFMHS in 2007 in response to the increasing number of consumers with serious mental illness being subject to NCSOs under the CMIA. The primary aim of the program is to supervise consumers compliance with their NCSO and provide reports to the courts on treatment progress and risk assessments. The program supports and consults Victorian Area Mental Health and Wellbeing Services (AMHWS) and other treating services in the treatment and management of consumers on NCSOs, provides specialist
expertise in identifying and managing risk, ensures AMHWS and other treating services are aware of their roles and responsibilities under the CMIA, provides education and training to AMHS in relation to issues affecting NCSO clients and provides reports to the court on the progress of clients on NCSOs. This forms a variant of an integrated model of forensic service, with readmissions to the local mental health facility if required and apprehension to the forensic inpatient facility reserved for consumers presenting with risk of serious endangerment to members of the public [6].
Forensic Clinical Specialist Program (2010)
The Forensic Clinical Specialist Program (FCSP) was established in 2010 in recognition of the over-representation of people with severe mental illness involved in the justice system, as offenders, victims, and people in need of comprehensive care and support [9]. The Harper Review’s (a 2015 review to provide advice on the legislative and governance models under the Victorian Serious Sex Offenders Act) recommendation for the need of improved decision making and coordination between the criminal justice and mental health systems to ensure community safety and appropriate care of clients, alongside the 2016-17 Victorian State Budget were key drivers in the expansion of the FCSP. The role of the program is to build forensic mental health expertise and capacity within AMHWS and to optimally assess and manage offending and problem behaviours [9, 10]. The FCSP supports AMHS in the recruitment of forensic clinical specialists and provides ongoing support, education and training [9].
Mental Health Act 2014
Since the inception of the CMIA (1997), several changes have occurred within the broad public mental health sector in Victoria. In 2014, a framework for recovery-oriented practice and recognised recovery was developed in the new Mental Health Act 2014 [11]. The Mental Health Act was a law that outlined the rights of people with mental illness or psychological distress, and how they can be assessed, treated, and supported. The Act introduced principles to support shared decision making and a greater emphasis on consumer recovery.
Problem Behaviour Program (2004, 2016)
In 2004, the Problem Behaviour Clinic and the Psychosexual Treatment Program combined and became the PBP, a program catered to those who engage in problem behaviours with or without the presence of mental illness [12-14]. Then in 2016, following recommendations of the Harper Review, the Victorian government substantially increased funding to the PBP, allowing a significant expansion of the service. The PBP is a unique feature of the Forensicare CFMHS, the service expands the scope of traditional CFMHSs beyond a narrow focus on mental illness to broader aspects of psychopathology and criminogenic needs [15]. It was established to provide psychiatric and psychological evidence- based assessment and treatment to people with a range of problem behaviours, including interpersonal violence, threats, stalking, fire setting, and sexual offending [7, 8, 12-14].
An assessment at the PBP is undertaken by a psychologist or psychiatrist and can include a semi-structured interview, collection of collateral information from family, friends and actors of the justice system and structured risk assessments (e.g., HCR-20). Treatment is offered to consumers according to the level of risk assessed and the availability of other treatment options. Individuals referred for treatment are typically those for whom correctional group treatments are not available or feasible. Treatment modality is based on cognitive behaviour therapy and relapse prevention approaches, and the goal of treatment is the cessation of the problem behaviour [15]. The PBP provides a referral point for individuals based on the nature of their criminogenic behaviour rather than the presence of mental disorder and offers services to individuals who are at risk of engaging in criminal behaviour but have not yet done so [12, 13-15].
The PBP is recognised both nationally and internationally as a centre of excellence for work with a wide range of offender groups, conducting thousands of assessments [12]. In 2012, Forensicare committed to a comprehensive evaluation of the program resulting in a grey-literature report. The PBP was shown to be effective in reducing reoffending, regardless of whether the individual is taken on for treatment or only provided with an assessment. During the five-year evaluation period, 824 individuals were assessed (74%) and/or treated (26%) through the PBP. The majority (73%) of consumers involved in the PBP indicated they found the service to be ‘very good’ and most (80%) indicated they felt ‘very supported’ by the PBP. Further, a large majority (80-93%) felt that treatment helped them to understand and manage their problem behaviour and to understand and reduce their offending behaviour.
In terms of reoffending data, 64% of all individuals referred to the program did not reoffend after contact. Of those who were taken on for treatment through the PBP, 72% had not reoffended by the end of the evaluation period. The period of lowest risk of reoffending was during treatment and although reoffending rates increased after treatment completion, these rates remained lower than pre-treatment offending. Consumers who were recommended for treatment but failed to attend, reoffended more often than those not recommended for treatment. These findings indicated clinicians were making appropriate recommendations regarding treatment, targeting those consumers who were high risk. Contact with the PBP also coincided with a reduction in contact with AMHWS. In addition, there was a reduction in crisis team and outpatient contacts for those who completed treatment through the PBP. Although the evaluation showed positive results for consumers who completed treatment through the PBP, only 40% of those recommended to attend treatment did so until completion.
CEM-COPE (2019)
The Coping with Child Exploitation Material Use (CEM-COPE) Program is an empirically informed group treatment program for child sexual abuse material only offenders with no known history of contact sexual offences [16]. The CEM-COPE program has been recently developed and builds on existing treatment research for child sexual abuse material only offenders, programs and evaluation outcomes. The program is evidence-based and was developed through an extensive literature review and expert consultation. In keeping with Risk, Needs and Responsivity principles, the CEM-COPE program aims to assist individuals to understand and manage their risk through low-intensity psychoeducation and skills-based intervention. The program is currently being piloted through the PBP to obtain feedback from group members and facilitators regarding clinical utility, efficacy and feasibility. Whilst no formal evaluation data has been published, the program has been incorporated into a high degree research candidature. To date, one round of the CEM-COPE program has been delivered. Participant engagement has been reported as good and feedback on the program has been positive to date with some considerations provided about program pace, length and format.
The Forensicare Serious Offender Consultation Service (F-SOCS) was developed in Victoria in 2016, for high-risk offenders with enduring mental illness supervised by community correctional services, who are poorly engaged or disengaged from mental health services and are considered high risk for serious offending [17,18]. The aims of F-SOCS are to improve mental health outcomes for high-risk serious offenders with severe mental illness, support community correctional services and AMHS and reduce the risk of serious offending among consumers [17]. The service is led by a consultant forensic psychiatrist and provides forensic mental health assessment, consultation and coordination of services. Referrals to F-SOCS are screened by the senior clinician to ensure they meet criteria. If an individual is accepted for assessment, a comprehensive psychiatric assessment will occur including structured risk assessment and current service provision evaluation. A comprehensive psychiatric report is provided to the community correctional service and AMHWS, including recommendations and referrals. The F-SOCS provide a three- and six-month review to evaluate the individual’s engagement with services and provide further consultation if required. A unique aspect of F-SOCS is the capacity to provide services prior to release from prison, enabling a better understanding of the individual’s needs prior to release and allowing service provision to begin without delay. An initial evaluation of the pilot program allowed the program to be adapted and developed in line with feedback and a full rollout across Victoriae was launched in 2017. No further descriptions or evaluations were found in the academic or grey literature searches.
Community Treatment & Transition (2016)
The Community Treatment and Transition (CTT) Program operates as a parallel forensic service, overseeing the treatment, care and supervision of consumers transitioning from the Thomas Embling Hospital (i.e., inpatient) to community settings [19, 20]. Clinicians working within the CTT Program provide community based clinical and case management to consumers on extended leave under the CMIA, assess and manage consumer related risk, support recovery, provide legal supervision, monitor and foster compliance of consumers with conditions on their orders and provide reports and evidence to the courts regarding consumer progress. Readmission, if required, is to the forensic inpatient facility at Thomas Embling Hospital.
Victorian Fixated Threat Assessment Centre (2018)
The Victorian Fixated Threat Assessment Centre (VFTAC) provides identification, assessment, and intervention coordination for individuals who pose a significant threat of lone actor grievance fuelled violence and who have a suspected or known mental disorder or disability [21]. Threat assessments are made using an evidence-based tool jointly administered by Victoria Police and forensic mental health staff. The Risk Aide-Memoire and the Grievance fuelled violence Risk Aide-Memoire are the threat guidance tools used exclusively by FTACs in all Australian states and territories, including Victoria. These tools are a prompt for key factors that should be considered in determining the current level of concern (low, moderate or high). The outcome of the assessment forms the basis for the development of a management plan, which includes referrals to appropriate services such as drug and alcohol agencies and specialist mental health services [22].
Court based Mental Health Advice & Response Service (2018)
The Forensic Mental Health Implementation Plan (FMHIP) is a cross-portfolio framework to reform the forensic mental health system over a ten-year period [23, 24]. The Mental Health Advice and Response Service (MHARS) was introduced in 2017-18 under the FMHIP, it incorporates and expands on two previously existing services providing clinical mental health advice to Magistrates and community correctional services on the mental health of accused persons. The purpose of MHARS is to provide clinical mental health advice within the court to improve the appropriateness of interventions and referrals for people appearing before the court. Twenty-five clinicians across 13 Magistrates Courts of Victoria facilitate screening and assessment to determine if mental illness is present and if it has a bearing on the case and screening of mental health needs to inform recommendations.
Royal Commission into Victoria’s Mental Health System (2021)
In February 2019, the Governor of the State of Victoria upon advice from the Victorian Government, formally established the Royal Commission into Victoria’s Mental Health System [25]. The interim and final reports from this Royal Commission concluded that the mental health system had catastrophically failed and was underprepared for future challenges. The final report set out 65 recommendations to transform the system into one that is contemporary and adaptable. The Royal Commission made several recommendations to strengthen treatment, care and support for people experiencing mental illness who are involved, or at risk of being involved, with the justice system, including recommendation 37.2; to expand the existing forensic community model [25]. A core tenet from the Royal Commission was that “the future mental health and wellbeing system will be fundamentally restructured around a community-based model of care, where people access treatment, care and support close to their homes and their communities” [25, p20]. As a result, there has been an increasing shift towards community-based services in place of inpatient services to provide care in the least restrictive environment possible due to the move toward deinstitutionalisation [26].
Mental Health Act and Wellbeing 2022
The Mental Health and Wellbeing Act 2022 (Vic) was developed to set the foundations for the reformed mental health and wellbeing system envisioned by the Royal Commission [27]. The Act superseded the Mental Health Act (2014) and includes 13 mental health and wellbeing principles that health professionals must consider when making decisions about people’s care. These principles are dignity and autonomy; diversity of care; least restrictive; supported decision making; family and carers; lived experience; health needs; dignity of risk; wellbeing of young people; diversity; gender safety; cultural safety and; wellbeing of dependents.
The Forensicare Strategic Plan and Model of Care 2021-26
Following the findings and recommendations of the Royal Commission into Victoria’s Mental Health System, Forensicare released a 2021-2026 Strategic Plan and Model of Care [28, 29]. Both documents highlighted the Forensicare purpose to “empower recovery for all Victorians living with mental illness who are at risk of entering, or have entered the justice system, to lead safe and meaningful lives free from offending”. The Strategic plan outlines four strategic directions: 1) consumer recovery pathway; 2) connections and partnerships that support the recovery of consumers, their carers, families and supporters; 3) workplace of choice for people with lived experience, mental health clinicians and corporate service leaders; and 4) research, education and innovation. Forensicare acknowledges four dimensions of recovery in this model of care (personal, wellbeing, clinical and offence specific) and the journey of recovery is characterised by three key phases (understanding strengths and needs, rehabilitation and community reintegration and continuity of care).
Regional Community Forensic Mental Health Services (2023)
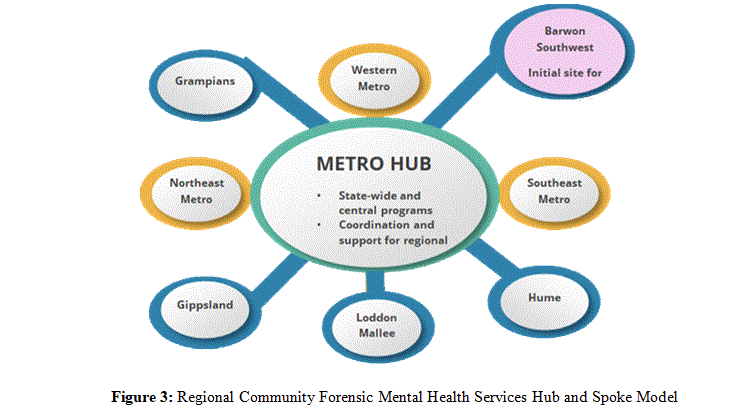
The first of the regional services have been established in the Barwon Southwest and Hume regions of regional Victoria. In line with recommendations from the Royal Commission into Victoria’s Mental Health System, Forensicare plans to implement community-based forensic mental health services in each of the eight mental health and wellbeing regions in Victoria [25, 30]. The Regional Community Forensic Mental Health Services (RFMHS) are multidisciplinary teams providing specialist services in collaboration with AMHWS, existing Forensicare programs and other key services [30]. The aim of the expansion is to improve outcomes for regional consumers who have offending risks and mental illness and/or problem behaviour. The design of the RCHMS is based on a hub and spoke model (see Figure 3). The regional teams will form the ‘spokes’ to the Forensicare CFMHS metropolitan ‘hub’. The regional teams will progressively develop ability to deliver most functions of CFMHS. Once implemented, the teams will provide consultation, reports, case management, shared care, coordination, supervision, forensic therapeutic interventions and assist prisoners transitioning from metropolitan prisons to the regions. The RFMHS will provide consultancy to and shared care with AMHS, a new service model that Forensicare has developed in the context of establishing the RFMHS. At the time of this review, two of the eight RFMHS have been established in the Barwon and Hume regions, however, no evaluations of the service have been conducted and no academic literature published.
Community Forensic Disability MH Service (Glaser Clinic) (2024)
The Glaser Clinic, also known as the Community Forensic Disability Mental Health Service, was established in 1993, and was governed by the Department of Families and Fair Housing [31]. In 2024, Forensicare overtook the governance of the clinic. It is a unique, state-wide outpatient service for individuals with cognitive disability and mental illness who are involved in the justice system. The Glaser Clinic provides community-based triage and assessment, coordination, service development and capacity building for people with co-occurring disability and mental illness who present with offending or problem behaviour. The service was established due to the lack of appropriate and dedicated dual disability services in Victoria. The aims of the service are to improve the wellbeing of consumers by reducing offending behaviour and improving connections to the community, ensuring consumers have timely access to treatment, ensuring consumers are involved in treatment planning and providing stakeholders with appropriate knowledge and skills to meet the needs of consumers. While there is no academic or grey literature evidence found evaluating the Glaser Clinic in this review, the clinic is currently undergoing evaluation from the Department of Health, Victoria.
The Road Ahead - Community Forensic Integrative Service Model
The forensic community mental health provision in Victoria has grown significantly over the last decade. The expansion is in response to increasing demand, provision of funding and a desire to fill service provision gaps. This organic growth model has followed a diverse development of a service model primarily based in liaison and consultation ways of working.
The Forensicare Model of Care 2021-26 resulted in significant expansion of forensic mental health services provision including a forensic bed expansion at Thomas Embling Hospital and the RFMHS teams in response to the recommendations of the Royal Commission. This provided an opportunity to restructure the CFMHS provision under a unifying service model that supports consumers throughout their recovery journeys. The CFIS model of service provides a clear operating service model to achieve this.
Several of the Royal Commission recommendation are relevant the new service model developed for CFMHS relating to expansion of the forensic community model. The Department of Health has determined that meeting this recommendation will be achieved through establishing specialist mental health teams in each of the eight mental health and wellbeing regions in Victoria and redeveloping the FCSP guidelines to support the planned expansion. Forensicare is leading both initiatives through the design of the aforementioned regional teams and implementation of the CFIS model.
The CFIS Service Model: A Hybrid Integrated Approach to Forensic Mental Health Care
The CFIS operates within a hybrid integrated service model that incorporates key elements of shared care, while also integrating components of parallel forensic services to support consumers transitioning from the Thomas Embling Hospital setting. This model maintains the liaison-based approach to service delivery and prioritizes capacity building and skill enhancement within general adult mental health services through integrated collaboration [20]. The primary recovery objective of this model is to facilitate reintegration into mainstream mental health services.
This model represents a paradigm shift from the traditional Con- sultation & Liaison model toward an integrated framework that aligns with consumer recovery pathways. It emphasizes partner- ships, collaboration, and stakeholder engagement, particularly with custodial services, Thomas Embling Hospital, and AMHWS. The model supports forensic consumers on extended leave and mental health supervision orders by ensuring coordinated care, shared responsibility, and structured transitional support for indi- viduals at high risk of service disengagement and recidivism. Key elements of this transformation include: Transition from cross-sec- tional assessments to longitudinal care; decentralisation of clinical operations; evolution from single-function teams to multifunction- al teams; continuity of care and responsibility; in reach function to units and custody settings; joint responses based on level of risk; and shared care
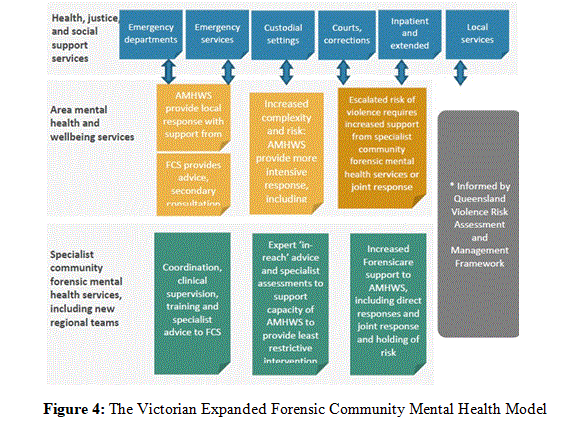
This integrated approach represents a progressive evolution in forensic mental health service delivery, promoting continuity of care, collaborative risk management, and recovery-oriented practice within both forensic and general mental health settings. The model will adapt the Queensland Government’s violence risk assessment and management framework for mental health services. The framework describes a pathway for mental health services to access forensic expertise and advice through a tiered approach (see Figure 4). The forensic service delivery based on forensic need and structured forensic risk assessment and not just the presence of absence of a court order.
Conclusion
The Forensicare CFMHS provides direct clinical care and a range of services to support the care and management of people at the intersection of the criminal justice and mental health systems, within a community setting. Since initial review of CFMHSs there has been a substantial expansion of the programs and services offered by the Forensicare CFMHS. Several programs, an intervention model, service model and models of care were identified in the academic and grey literature searches. The programs identified ranged from providing primary clinical assessment and intervention to consumers, support to AMHS, assessment and recommendations to courts and support during transition from prison or hospital. Describing the Forensicare CFMHS has demonstrated how the publicly funded forensic mental health service is striving to meet recommendations of the Royal Commission and continued clinical innovation mandated in the Mental Health and Wellbeing Act (2022). There is tremendous opportunity to evaluate and report on the current and future programs of the Forensicare CFMHS to inform the impact on clinical outcomes for the consumers and their families and carers.
Funding
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Author Contribution
SK was responsible conceptualisation, writing, reviewing and editing. MY and TF were responsible for the literature search, writing, reviewing and editing.
Conflict of Interest
SK and TF are employed at the Victorian Institute of Forensic Mental Health (Forensicare). MY holds a joint appointment at the Victorian Institute of Forensic Mental Health (Forensicare).
Data Availability
The lead author can be contacted to obtain relevant documents cited in the body of the manuscript that are not publicly available and relevant CFIS design and practice principles, service offerings, and clinical and legal governance documents.
References
1. Robertson, P., Barnao, M., Ward, T. (2011). Rehabilitation frameworks in forensic mental health. Aggression and Violent Behavior 16, 472-84.
2. O'Donahoo, J., & Simmonds, J. G. (2016). Forensic patients and forensic mental health in Victoria: Legal context, clinical pathways, and practice challenges. Australian Social Work, 69(2), 169-180.
3. Victorian Institute of Forensic Mental Health. (2020). Non- Custodial Supervision Order Consultation & Liaison Program (NCSO Program) Program Guidelines. Victorian Institute of Forensic Mental Health.
4. Jager, A. D. (2001). Forensic psychiatry services in Australia. International Journal of Law and Psychiatry, 24(4-5), 387-98.
5. Furness, T., Bardoel, A., Djurkovic, N., Fullam, R., & Ogloff, J. R. (2024). Workplace culture for forensic mental health services: a mixed methods descriptive study. BMC Health Services Research, 24(1), 1498.
6. Crimes (Mental Impairment and Unfitness to be Tried) Act 1997 (Vic).
7. Brett, A., Carroll, A., Green, B., Mals, P., Beswick, S., Rodriguez, M., ... & Gagliardi, C. (2007). Treatment and security outside the wall: diverse approaches to common challenges in community forensic mental health. International Journal of Forensic Mental Health, 6(1), 87-99.
8. Ogloff, J. R. (2010). The evolution of forensic mental health services in Victoria, Australia: Contributions of Professor Paul Mullen. Criminal Behaviour and Mental Health, 20(3), 232-241.
9. Forensicare. (2022). Forensic Clinical Specialist Program Operational Guidelines. Forensicare.
10. Forensicare. (2021). Forensic Clinical Specialist Program Risk Framework. Forensicare.
11. Mental Health Act 2014 (Vic).
12. MacKenzie, R. D., & James, D. V. (2011). Management and treatment of stalkers: Problems, options, and solutions. Behavioral Sciences & the Law, 29(2), 220-239.
13. McEwan, T. E., MacKenzie, R. D., & McCarthy, J. (2014). The Problem Behaviour Program: Threat assessment and management in community forensic mental health. International handbook of threat assessment, 360-374.
14. Victorian Institute of Forensic Mental Health. (2021). Problem Behaviour Program Program Guidelines. Victorian Institute of Forensic Mental Health.
15. McCarthy, J., McGrail, J., Mcewan, T., Ducat, L., Norton, J., et al. (2015). Evaluation of the Problem Behaviour Program: A Community Based Program for the Assessment and Treatment of Problem Behaviours. Forensicare and Centre for Forensic Behavioural Science, Swinburne University of Technology.
16. Henshaw, M., Arnold, C., Darjee, R., Ogloff, J. R., & Clough, J. A. (2020). Enhancing evidence-based treatment of child sexual abuse material offenders: The development of the CEM-COPE Program. Trends and Issues in Crime and Criminal Justice, (607), 1-14.
17. Forensicare. (2018). Forensicare Serious Offender Consultation Service (F-SOCS) Operations Manual. Forensicare.
18. Carroll, A., & Brett, A. (2024). Jailing is failing: psychiatry can help. BJPsych Bulletin, 48(5), 280-284.
19. Forensicare. Community Treatment & Transition Program Operations Manual. Forensicare; 2021.
20. Natarajan, M., Srinivas, J., Briscoe, G., & Forsyth, S. (2012). Community forensic psychiatry and the forensic mental health liaison model. Advances in psychiatric treatment, 18(6), 408- 415.
21. Gray, M., McCarthy, J., Mawren, D., Cooper, S., Simms, C., & Pathé, M. (2024). A descriptive study of young people with Autism Spectrum Disorder referred to a Fixated Threat Assessment Centre. Psychiatry, Psychology and Law, 1-13.
22. Victoria State Government Health and Human Services. (2020). Service System Enhancements for the Fixated Threat Assessment Centre Service Model Guidelines. Victoria State Government Health and Human Services.
23. Forensicare. (2018). Mental Health Advice and Response Service Operating Framework. Forensicare.
24. Forensicare. (2019). Clinical Guidelines Mental Health Advice and Response Service. Forensicare.
25. State of Victoria. (2021). Royal Commission into Victoria's Mental Health System Final Report 2021. State of Victoria.
26. McKenna, B., & Sweetman, L. E. (2020). Models of care in forensic mental health services: A review of the international and national literature. Wellington: Ministry of Health.
27. Mental Health and Wellbeing Act 2022 (Vic).
28. Forensicare. 2021-26 Strategic Plan. Forensicare; 2021.
29. Forensicare. Model of Care 2021-26. Forensicare; 2021.
30. Forensicare. (2023). Regional Forensic Mental Health Services Barwon South West Team Operations Manual. Forensicare.
31. Forensicare. (2024). Community Forensic Disability Mental Health Service (Glaser Clinic) Service Model. Forensicare.


