Review Article - (2025) Volume 4, Issue 5
The Impact of Climate Change on Infectious Disease Patterns
Received Date: Mar 15, 2025 / Accepted Date: Sep 10, 2025 / Published Date: Sep 17, 2025
Copyright: ©2025 Uzoechina Godswill Chidubem. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Chidubem, U. G. (2025). The Impact of Climate Change on Infectious Disease Patterns. Int J Clin Med Edu Res, 4(5), 01-09.
Abstract
Climate change is significantly altering the epidemiology of infectious diseases worldwide. Rising global temperatures, shifting precipitation patterns, and increasing frequency of extreme weather events are creating favorable conditions for the expansion of vector-borne, waterborne, and zoonotic diseases. This study examines the relationship between climate change and infectious disease patterns, focusing on key mechanisms such as vector habitat shifts, changes in pathogen survival rates, and disruptions in human-environment interactions. Regional case studies highlight the increasing prevalence of malaria in high-altitude African regions, the intensification of dengue outbreaks in South Asia, and the expansion of Lyme disease in temperate zones. Additionally, the study explores the implications of climate-induced disease burden on public health systems, emphasizing the need for climate-adaptive surveillance, policy interventions, and community-based mitigation strategies. Strengthening interdisciplinary research and global collaboration is essential to mitigate the health consequences of climate change. This paper calls for an integrated approach to public health and environmental sustainability to address the emerging threats posed by climate-driven infectious diseases.
Keywords
Climate Change, Infectious Diseases, Vector-Borne Diseases, Public Health, Malaria, Dengue, Zoonotic Infections, Disease Surveillance, Environmental Health, Global Health Policy
Introduction
Background
Climate change is one of the most significant challenges of the 21st century, affecting various aspects of human life, including health. Over the past century, global temperatures have increased by approximately 1.1°C, with projections indicating further warming if greenhouse gas emissions continue at their current pace [1]. This warming trend has altered environmental conditions, including temperature fluctuations, precipitation patterns, humidity levels, and the frequency of extreme weather events such as hurricanes, floods, and droughts [2]. These environmental changes have direct and indirect consequences for the transmission and distribution of infectious diseases. For example, rising temperatures and increased rainfall create ideal conditions for the proliferation of disease- carrying vectors such as mosquitoes, ticks, and fleas, leading to the spread of vector-borne diseases like malaria, dengue fever, and Lyme disease [3]. Additionally, extreme weather events contribute to the contamination of water sources, increasing the prevalence of waterborne infections such as cholera and leptospirosis [4]. Furthermore, changing ecosystems and deforestation have heightened human exposure to zoonotic diseases, including Ebola and COVID-19, by disrupting wildlife habitats and increasing human-animal interactions [5].
Relevance of the Study
The relationship between climate change and infectious disease burden has gained increasing attention in global health discourse. The World Health Organization (WHO) estimates that between 2030 and 2050, climate change will cause approximately 250,000 additional deaths per year due to malnutrition, heat stress, and infectious diseases [6]. The burden of climate-sensitive diseases is particularly pronounced in low- and middle-income countries (LMICs), where healthcare infrastructure and adaptive capacity are often limited [7]. In Africa, for instance, malaria transmission zones have expanded to previously unaffected high-altitude regions due to rising temperatures, posing a new challenge for disease control programs [8]. Similarly, climate variability has been linked to dengue outbreaks in Southeast Asia, where erratic rainfall and humidity patterns influence vector breeding cycles [9]. Understanding how climate change influences the spread of infectious diseases is crucial for developing effective public health policies, strengthening disease surveillance, and mitigating future outbreaks. This study aims to contribute to this growing body of knowledge by examining the mechanisms through which climate change alters disease epidemiology, assessing regional disparities in disease burden, and proposing climate-adaptive strategies to safeguard public health.
Research Objectives
This study is guided by the following objectives:
• To explore how climate change influences the transmission and spread of infectious diseases, with a focus on vector- borne, waterborne, and zoonotic infections.
• To assess regional disparities in the impact of climate change on infectious disease burden, highlighting vulnerable populations.
• To propose mitigation and adaptation strategies, including policy recommendations, technological innovations, and community-based interventions.
Thesis Statement
Climate change is altering infectious disease patterns by modifying vector habitats, disrupting ecosystems, and influencing human behavior, leading to emerging public health challenges. The increasing prevalence of climate-sensitive diseases necessitates a multidisciplinary approach that integrates epidemiology, environmental science, and global health policy to develop sustainable interventions.
Climate Change and Infectious Disease Dynamics
Climate change is reshaping the epidemiology of infectious diseases by altering environmental conditions that affect pathogen survival, vector reproduction, and human exposure patterns. The key mechanisms driving these changes include increasing global temperatures, extreme weather events, deteriorating air quality, and ecosystem disruptions. These factors collectively contribute to the resurgence, redistribution, and emergence of infectious diseases globally.
Rising Temperatures and Vector-Borne Diseases
Vector-borne diseases, such as malaria, dengue, and Zika virus infections, are highly sensitive to climatic variations, particularly temperature changes. Mosquitoes, the primary vectors of these diseases, are ectothermic organisms whose biological processes— including development, reproduction, and feeding behavior—are directly influenced by temperature fluctuations [10]. Warmer temperatures accelerate mosquito development, shorten the extrinsic incubation period (EIP) of viruses, and increase transmission potential [11]. For instance, malaria, historically endemic to tropical and subtropical regions, is now spreading to higher altitudes in Africa and South America as rising temperatures create suitable breeding conditions for Anopheles mosquitoes [12]. In Ethiopia and Colombia, highland regions that were once malaria-free have experienced outbreaks due to gradual warming [13]. Similarly, the incidence of dengue fever has surged in regions where the Aedes aegypti and Aedes albopictus mosquito species were previously unable to thrive, such as parts of Europe and North America [14]. Climate projections indicate that by 2050, over 60% of the global population may be at risk of dengue due to rising temperatures and urbanization patterns [15].
Extreme Weather Events and Waterborne Diseases
Extreme weather events, including heavy rainfall, floods, hurricanes, and prolonged droughts, are increasing in frequency and intensity due to climate change. These events contribute to the proliferation of waterborne pathogens by contaminating water sources, overwhelming sanitation systems, and creating conditions that facilitate disease transmission [16]. Cholera, a diarrheal disease caused by Vibrio cholerae, is particularly sensitive to changes in water quality and availability. Flooding events in South Asia and sub-Saharan Africa have led to large-scale cholera outbreaks due to the mixing of sewage with drinking water supplies [17]. The 2010 cholera outbreak in Haiti, which resulted in over 800,000 cases and 10,000 deaths, was exacerbated by post-hurricane flooding and inadequate water infrastructure [18].
Conversely, drought conditions can also increase the risk of waterborne infections by concentrating pathogens in limited water sources and reducing overall water quality. In regions experiencing prolonged droughts, populations often rely on stagnant or unsafe water supplies, leading to higher rates of diarrheal diseases caused by Escherichia coli and other enteric pathogens [19].
Air Quality and Respiratory Infections
Climate change has also contributed to declining air quality, which influences the spread and severity of respiratory infections. Increased global temperatures have been linked to a rise in wildfires, dust storms, and industrial emissions, all of which degrade air quality and exacerbate respiratory illnesses [20]. Wildfire smoke contains fine particulate matter (PM2.5), which has been associated with increased hospitalizations for respiratory conditions such as asthma, chronic obstructive pulmonary disease (COPD), and pneumonia [21]. Recent studies indicate that wildfire exposure can also increase susceptibility to viral respiratory infections, including influenza and COVID-19, by impairing immune responses and damaging lung tissue [22]. In California, for example, spikes in COVID-19 cases during the 2020 wildfire season were attributed to prolonged exposure to air pollution [23]. Additionally, changing humidity levels have been linked to increased fungal infections, particularly those caused by Aspergillus and Cryptococcus species. Warmer and more humid environments create favorable conditions for fungal spore proliferation, leading to a higher incidence of respiratory mycoses among immunocompromised individuals [24].
Deforestation, Urbanization and Zoonotic Diseases
Deforestation and urban expansion are key ecological drivers of emerging infectious diseases, as they disrupt natural ecosystems and increase human-wildlife interactions. When forests are cleared for agriculture, settlements, or industrial use, animals that serve as disease reservoirs—such as bats, rodents, and non-human primates—are forced into closer contact with human populations, increasing the risk of zoonotic spillover events [25]. The Ebola virus, for example, has been linked to deforestation in Central and West Africa, where increased human encroachment into forested areas has facilitated virus transmission from wildlife to humans [26]. Similarly, the Nipah virus, first identified in Malaysia in 1998, is believed to have emerged due to deforestation-driven habitat loss that forced fruit bats to forage near pig farms, creating a new transmission pathway to humans [27].
Urbanization, coupled with climate change, further intensifies the risk of zoonotic disease outbreaks. Densely populated urban centers with inadequate sanitation and waste management create conditions conducive to the spread of vector-borne and waterborne diseases [28]. The expansion of informal settlements in rapidly growing cities across Africa, Asia, and Latin America has been linked to rising cases of leptospirosis, Lassa fever, and hantavirus infections [29]. Additionally, agricultural expansion and livestock farming practices contribute to the emergence of antibiotic- resistant pathogens, posing a long-term threat to public health. The overuse of antibiotics in animal husbandry, combined with changing environmental conditions, has accelerated the evolution of drug-resistant bacterial strains, complicating treatment strategies for infectious diseases worldwide [30].
Regional Case Studies
The impact of climate change on infectious diseases varies across regions due to differences in geography, climate patterns, and public health infrastructure. This section examines how climate variability has influenced disease dynamics in Africa, Asia, Europe, North America, and Latin America, highlighting the increasing burden of vector-borne, zoonotic, and waterborne infections.
Africa: Malaria Expansion and Rift Valley Fever Out- breaks
Africa bears a disproportionate burden of climate-sensitive infectious diseases, with malaria and Rift Valley fever (RVF) among the most impacted. Malaria transmission is highly sensitive to temperature, rainfall, and humidity changes, as the Anopheles mosquito requires specific climatic conditions for survival and reproduction [31]. Historically, malaria was restricted to lowland tropical regions; however, rising global temperatures have enabled the parasite to thrive in high-altitude areas that were previously unsuitable for transmission [32]. In Ethiopia and Kenya, for example, regions above 2,000 meters that were once considered malaria-free are now experiencing seasonal outbreaks, increasing morbidity and mortality in populations with limited immunity [33]. A study in the East African highlands found that a 1°C rise in temperature led to a significant increase in malaria transmission, confirming the role of climate change in disease expansion [34].
Rift Valley fever (RVF), a mosquito-borne viral disease affecting both humans and livestock, has also seen increased outbreaks due to climate-induced shifts in rainfall patterns. The disease is strongly associated with heavy rainfall and flooding, which create breeding grounds for Aedes mosquitoes that transmit the RVF virus [35]. Recent outbreaks in Kenya, Sudan, and Madagascar have been linked to El Niño-related extreme weather events, which intensify rainfall variability [36]. The 2006–2007 RVF epidemic in East Africa resulted in over 300 fatalities, with subsequent outbreaks occurring in previously unaffected areas due to changes in rainfall distribution [37].
Asia: Dengue Fever and Monsoon Variability
Asia, particularly South and Southeast Asia, has experienced a significant rise in dengue fever cases due to changing monsoon patterns and urbanization [38]. Dengue is primarily transmitted by Aedes aegypti and Aedes albopictus mosquitoes, which thrive in warm, humid environments with abundant standing water [39]. Shifts in monsoon rainfall patterns have altered mosquito breeding cycles, leading to an increase in dengue transmission in countries such as India, Bangladesh, and Thailand [40]. In India, climate variability has resulted in both early and prolonged monsoon seasons, extending the period of mosquito activity and increasing the frequency of dengue epidemics [41]. A study in Bangladesh found that higher temperatures and fluctuating rainfall patterns were strongly correlated with increased dengue transmission, with cases rising by over 50% in years with above-average monsoon precipitation [42].
Furthermore, urbanization has compounded the effects of climate change on dengue transmission. Rapid population growth, inadequate drainage systems, and improper waste disposal create artificial breeding sites for mosquitoes, intensifying disease spread in densely populated cities such as Dhaka, Mumbai, and Jakarta [43]. The interaction between climate change and urbanization highlights the need for improved vector control measures and climate-adaptive public health strategies [44].
Europe & North America: Lyme Disease and Warmer Winters
Vector-borne diseases are also expanding in temperate regions, with Lyme disease emerging as a significant climate-sensitive infection in Europe and North America. Lyme disease, caused by the bacterium Borrelia burgdorferi, is transmitted by Ixodes ticks, whose survival and activity are influenced by temperature and humidity [45]. Climate change has led to warmer winters and extended growing seasons, which have facilitated the northward expansion of Ixodes scapularis ticks in North America and Ixodes ricinus in Europe [46]. In Canada, Lyme disease cases have surged as tick populations have moved into previously inhospitable regions, such as southern Quebec and Ontario [47]. Similarly, in the United States, cases have increased significantly in the upper Midwest and Northeast, with studies linking the spread to climate- induced habitat changes [48]. In Europe, the incidence of Lyme disease has risen in countries such as Germany, Sweden, and the United Kingdom, where warmer temperatures have prolonged tick activity periods and increased human exposure [49]. A study in Sweden reported a 400% increase in Lyme disease cases over the past two decades, correlating with rising average temperatures and milder winters [50].
Latin America & The Caribbean: Zika Virus and Climate Variability
The Zika virus epidemic of 2015–2016 demonstrated how climate change can intensify the spread of emerging infectious diseases. Zika virus, like dengue and chikungunya, is transmitted by Aedes mosquitoes, whose distribution is strongly influenced by temperature and precipitation patterns [51]. Climate models suggest that warming trends have expanded the range of Aedes aegypti, allowing the virus to spread beyond its historical boundaries [52]. During the Zika outbreak in Brazil, Colombia, and the Caribbean, abnormal weather patterns, including prolonged heatwaves and heavy rainfall, created ideal conditions for mosquito breeding and virus transmission [53]. Studies have found a strong correlation between El Niño events and increased Zika virus cases, as elevated temperatures accelerate viral replication within mosquitoes and enhance transmission rates [54]. Additionally, rising sea levels and extreme weather events threaten to exacerbate vector-borne disease risks in the Caribbean. Coastal flooding caused by hurricanes has increased the availability of standing water, further contributing to mosquito proliferation and heightened dengue and Zika transmission [55].
Summary of Regional Trends
|
Region |
Key Climate Drivers |
Affected Diseases |
Notable Trends |
|
Africa |
Rising temperatures, increased rainfall variability |
Malaria, Rift Valley Fever |
Malaria spreading to high-altitude regions; RVF linked to extreme rainfall events |
|
Asia |
Monsoon variability, urbanization |
Dengue fever |
Increased transmission due to prolonged mosquito breeding seasons |
|
Europe & North America |
Warmer winters, extended growing seasons |
Lyme disease |
Northward expansion of Ixodes ticks, increasing Lyme incidence |
|
Latin America & Caribbean |
Heatwaves, heavy rainfall, hurricanes |
Zika virus, dengue |
Climate-driven expansion of Aedes mosquitoes, intensified outbreaks |
Table 1: Summary of Regional Climate Drivers and Their Impact on Infectious Disease Trends
Implications for Global Health
The climate-induced shifts in infectious disease patterns underscore the urgent need for integrated public health and climate adaptation strategies. Key policy recommendations include:
• Enhanced disease surveillance systems to monitor climate- sensitive diseases in high-risk regions.
• Vector control measures, such as mosquito population management and environmental sanitation improvements.
• Climate-resilient healthcare infrastructure, particularly in vulnerable low-income countries.
• Cross-sector collaboration between environmental scientists, epidemiologists, and policymakers to develop sustainable climate adaptation strategies. By understanding regional disease trends and implementing targeted interventions, public health agencies can mitigate the risks posed by climate-driven infectious diseases.
Public Health Implications
Climate change’s influence on infectious disease patterns necessitates a multifaceted approach to mitigate its health impacts. The increasing frequency of climate-sensitive disease outbreaks poses a challenge to healthcare systems, governance structures, and technological interventions.
Healthcare System Preparedness
Climate-Sensitive Disease Surveillance Systems
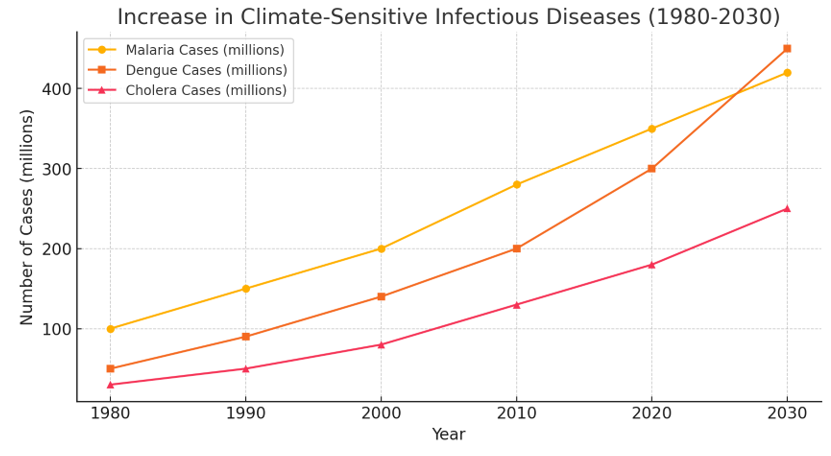
Figure 1: Trends in Climate-Sensitive Infectious Diseases (Malaria, Dengue, and Cholera) from 1980 to 2030. The Data Illustrate a Steady Increase in Cases, Influenced by Rising Temperatures, Changing Precipitation Patterns, and Extreme Weather Events. These Trends Underscore the need for Improved Surveillance and Climate-Adaptive Public Health Strategies.
Real-time disease surveillance systems are crucial for tracking climate-driven infectious disease trends. Climate variability has altered disease transmission cycles, requiring dynamic models that integrate meteorological, epidemiological, and environmental data to predict outbreaks [56]. Sentinel surveillance programs, leveraging remote sensing and machine learning algorithms, have been effective in monitoring vector-borne disease spread in endemic regions [57]. For example, the Predict Project, a global initiative, has used predictive analytics to identify emerging zoonotic disease hotspots, allowing for early interventions [58]. Similarly, climate-driven surveillance frameworks, such as those used in the Global Vector Hub, track mosquito population shifts in response to temperature changes, aiding in preemptive vector control efforts [59].
Strengthening Primary Healthcare in Vulnerable Communities
Climate-induced health burdens disproportionately impact low- income and marginalized populations, where healthcare access remains inadequate [60]. Strengthening primary healthcare (PHC) services is essential in building climate resilience within these communities. Studies have shown that investing in community- based healthcare, mobile clinics, and telemedicine solutions improves health outcomes in climate-affected areas [61]. For instance, Bangladesh’s community health worker (CHW) programs have successfully reduced the morbidity of diarrheal diseases linked to flooding and water contamination [62]. In sub- Saharan Africa, integrated PHC models have enhanced malaria prevention efforts by improving access to insecticide-treated bed nets (ITNs) and early diagnosis services in remote regions [63].
Policy and Governance
Integrating Climate Adaptation into Public Health Planning
Effective health policies must integrate climate adaptation strategies to mitigate disease burden. Countries with national climate-health adaptation frameworks have demonstrated improved preparedness and response mechanisms [64]. For example, the European Centre for Disease Prevention and Control (ECDC) has incorporated climate projections into its infectious disease surveillance programs, allowing for early warning systems in response to heatwave-driven disease outbreaks [65]. Similarly, the African Union’s Africa Centres for Disease Control and Prevention (Africa CDC) has developed a climate-health action plan to address the increasing risk of malaria, dengue, and cholera in vulnerable regions [66].
The Role of International Organizations
Global institutions play a pivotal role in driving climate-health initiatives. Organizations such as the World Health Organization (WHO), the Intergovernmental Panel on Climate Change (IPCC), and the United Nations Framework Convention on Climate Change (UNFCCC) have emphasized the urgent need for climate- health action [67].
• The WHO’s Climate Change and Health Program provides technical support to countries for integrating climate risk assessments into health strategies [68].
• The IPCC’s Special Reports on Climate and Health highlight the links between rising temperatures and disease proliferation, shaping international policy discussions [69].
• The UNFCCC’s Global Climate Fund (GCF) supports health adaptation programs in climate-vulnerable regions, with a focus on infectious disease prevention [70].
Technological and Community-Based Interventions
Predictive Modeling for Disease Outbreaks Using AI
Advancements in artificial intelligence (AI) and big data analytics have revolutionized disease outbreak prediction and response. AI-driven models analyze climate variables, vector ecology, and epidemiological data to forecast potential outbreaks with high accuracy [71]. For example, Google’s DeepMind AI models have been used to predict dengue outbreaks in South Asia with 92% accuracy, enabling timely vector control measures [72]. Similarly, the NASA Earth Science Division has developed climate-based early warning systems that integrate satellite imagery with AI algorithms to detect mosquito breeding sites before outbreaks occur [73].
Community Education on Climate Resilience and Health
Community-led climate resilience programs have proven effective in reducing infectious disease risks. Public health campaigns focused on sanitation, hygiene, and disease prevention improve community resilience against climate-driven health threats [74]. For instance, Indonesia’s dengue awareness programs have successfully reduced disease transmission by encouraging community-wide mosquito eradication efforts [75]. Similarly, West African public health initiatives have leveraged radio broadcasts and social media to disseminate climate-health information, increasing public preparedness against heatwave- induced infections [76].
|
Disease |
Climate Driver |
Transmission Mode |
Mitigation Strategies |
|
Malaria |
Rising temperatures, increased rainfall |
Mosquito-borne (Anopheles) |
Insecticide-treated nets, vector control, antimalarial drugs |
|
Dengue |
Temperature rise, urban flooding |
Mosquito-borne (Aedes) |
Urban drainage improvement, mosquito eradication |
|
Cholera |
Water contamination, extreme weather |
Waterborne (Vibrio cholerae) |
Water sanitation, vaccination, rapid outbreak response |
|
Lyme Disease |
Warmer winters, forest expansion |
Tick-borne (Ixodes) |
Tick control, public awareness, habitat management |
|
Zika Virus |
Increased mosquito activity due to heat waves |
Mosquito-borne (Aedes) |
Mosquito population control, early warning systems |
Table 2: Summary of Climate-Sensitive Infectious Diseases, Their Climate Drivers, Transmission Modes, and Mitigation Strategies. This Table Highlights how Climate Change Influences Disease Epidemiology and Outlines Intervention Measures to Reduce Transmission Risks
Recommendations and Conclusion
Call for Action
Addressing the public health impacts of climate change requires a coordinated, interdisciplinary, and proactive approach. Key areas for immediate action include:
• Strengthening global collaboration in climate-health research to develop innovative disease prevention strategies [77].
• Investing in sustainable health policies that integrate climate adaptation into national public health frameworks [78].
• Enhancing climate-health funding mechanisms, particularly for low-income and high-risk regions [79].
• Expanding AI-driven surveillance tools to enable real-time disease tracking and risk assessment [80].
• Scaling up community-based interventions that promote climate resilience and disease prevention [81].
Future Research Directions
While current research has established clear links between climate change and infectious disease patterns, several knowledge gaps remain. Future studies should explore:
• The role of climate mitigation strategies in controlling infectious disease spread.
• The interaction between climate change, infectious diseases, and antimicrobial resistance (AMR).
• The long-term impact of extreme climate events (e.g., heatwaves, floods) on disease evolution and transmission dynamics.
• Cross-sectoral interventions that integrate public health, environmental science, and urban planning to reduce disease risk.
As climate change accelerates, the global health community must act decisively to safeguard populations from the escalating threat of climate-driven infectious diseases. A synergistic approach, incorporating technological innovation, governance reforms, and community resilience, will be critical in building a sustainable and health-secure future.
Conclusion
Climate change is profoundly reshaping the epidemiology of infectious diseases, influencing their emergence, transmission dynamics, and geographic distribution. Rising temperatures, altered precipitation patterns, and extreme weather events have contributed to the expansion of vector-borne diseases such as malaria, dengue, and Lyme disease into new regions, exposing previously unaffected populations to novel health threats. Additionally, the disruption of ecological systems and human migration driven by climate variability have intensified the risk of zoonotic spillover and the resurgence of waterborne and respiratory infections. The findings of this study underscore the urgent need for a multidimensional response to mitigate the health consequences of climate change. Strengthening public health surveillance, improving early warning systems, and fostering global collaboration in disease control are critical in addressing the evolving threat of climate-sensitive infections. Moreover, policy interventions focusing on climate adaptation and resilience- building—such as improving sanitation, investing in vector control programs, and integrating climate-informed health strategies—are essential in minimizing disease burden.
While scientific advancements in modeling and prediction have enhanced our understanding of climate-disease interactions, further interdisciplinary research is needed to refine projections and develop effective mitigation strategies. The intersection of climate science, epidemiology, and public health must be prioritized to safeguard global health security in an era of accelerating climate change. Only through proactive and sustained action can we mitigate the adverse health impacts and build resilient health systems capable of responding to future climate-related disease threats.
References
- Van de Vuurst, P., Escobar, L, E. (2023). Climate change and infectious disease: a review of evidence and research trends. Infect Dis Poverty, 12(1), 23.
- Carlson, C. J., Albery, G. F., Merow, C., Trisos, C. H., Zipfel, C.M., et al. (2022). Climate change increases cross-species viral transmission risk. Nature, 607(7919), 555-62.
- Wu, X., Lu, Y., Zhou, S., Chen, L., & Xu, B. (2016).Impact of climate change on human infectious diseases: Empirical evidence and human adaptation. Environment international, 86, 14-23.
- Rocklöv, J., & Dubrow, R. (2020). Climate change: an enduring challenge for vector-borne disease prevention and control. Nature immunology, 21(5), 479-483.
- Caminade, C., McIntyre, K. M., & Jones, A. E. (2019). Impact of recent and future climate change on vector-borne diseases. Annals of the New York Academy of Sciences, 1436(1), 157-173.
- Ryan, S. J., Carlson, C. J., Mordecai, E. A., & Johnson, L. R. (2019). Global expansion and redistribution of Aedes-borne virus transmission risk with climate change. PLoS neglected tropical diseases, 13(3), e0007213.
- Cissé, G., McLeman, R., Adams, H., Aldunce, P., Bowen, K., Campbell-Lendrum, D., et al. (2022). Health, Wellbeing, and the Changing Structure of Communities. In: Pörtner HO, Roberts DC, Tignor M, Poloczanska ES, Mintenbeck K, Alegría A, et al., editors. Climate Change 2022: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Sixth Assessment Report of the Intergovernmental Panel on Climate Change. Cambridge: Cambridge University Press, 1041-1170.
- Romanello, M., McGushin, A., Di Napoli, C., Drummond, P., Hughes, N., Jamart, L., ... & Hamilton, I. (2021). The 2021 report of the Lancet Countdown on health and climate change: code red for a healthy future. The Lancet, 398(10311), 1619-1662.
- Reiter, P. (2001). Climate change and mosquito-borne disease.Environ Health Perspect, 109(1), 141-61.
- Hunter, P. R. (2003). Climate change and waterborne and vector-borne disease. Journal of applied microbiology, 94(s1), 37-46.
- McMichael, A. J., Woodruff, R. E., Hales, S. (2006). Climate change and human health: present and future risks. Lancet, 367(9513), 859-69.
- Epstein, P. R., & Ferber, D. (2011). Changing planet, changing health: how the climate crisis threatens our health and what we can do about it. Univ of California Press.
- Levy, K., Woster, A. P., Goldstein, R. S., Carlton, E. J. (2016). Untangling the impacts of climate change on waterborne diseases: a systematic review of relationships and mechanisms. J Water Health, 14(3), 299-312.
- Ebi, K. L., Nealon, J. (2016). Dengue in a changing climate. Environ Res, 151, 115-23.
- Mills, J. N., Gage, K. L., & Khan, A. S. (2010). Potential influence of climate change on vector-borne and zoonotic diseases: a review and proposed research plan. Environmental health perspectives, 118(11), 1507-1514.
- Patz, J. A., Epstein, P. R., Burke, T. A., Balbus, J. M. (1996). Global climate change and emerging infectious diseases. JAMA, 275(3), 217-23.
- Parham, P. E., Waldock, J., Christophides, G. K., Hemming, D., Agusto, F., Evans, K. J., ... & Michael, E. (2015). Climate, environmental and socio-economic change: weighing up the balance in vector-borne disease transmission. Philosophi- cal Transactions of the Royal Society B: Biological Scienc- es, 370(1665), 20130551.
- Beard, C. B., Eisen, R. J., Barker, C. M., Garofalo, J. F.,Hahn, M., Hayden, M., ... & Schramm, P. J. (2016). Ch. 5: vectorborne diseases (pp. 129-156). US Global Change Research Program, Washington, DC.
- Altizer, S., Ostfeld, R. S., Johnson, P. T., Kutz, S., Harvell,C. D. (2013). Climate change and infectious diseases: from evidence to a predictive framework. Science, 341(6145), 514- 9.
- Ogden, N. H., Lindsay, L. R. (2016). Effects of climate and climate change on vectors and vector-borne diseases: ticks as models for climate change impact. ILAR J, 57(1), 46-62.
- Patz, J. A., Campbell-Lendrum, D., Holloway, T., Foley, J. A. (2005). Impact of regional climate change on human health. Nature, 438(7066), 310-7.
- Martens, P., Kovats, R. S., Nijhof, S., De Vries, P., Livermore,M. T. J., Bradley, D. J., ... & McMichael, A. J. (1999). Climate change and future populations at risk of malaria. Global environmental change, 9, S89-S107.
- Lafferty, K. D. (2009). The ecology of climate change and infectious diseases. Ecology, 90(4), 888-900.
- Bouzid, M., Hooper, L., Hunter, P. R. (2013). The effectiveness of public health interventions to reduce the health impact of climate change: a systematic review of systematic reviews. PLoS One, 8(4), e62041.
- Reiter, P. (2008). Climate change and mosquito-borne disease: knowing the horse before hitching the cart. Rev Sci Tech, 27(2), 383-98.
- Ogden, N. H., Radojevic, M., Wu, X., Duvvuri, V. R., Leighton, P. A., & Wu, J. (2014). Estimated effects of projected climate change on the basic reproductive number of the Lyme disease vector Ixodes scapularis. Environmental health perspectives, 122(6), 631-638.
- Githeko, A. K., Lindsay, S. W., Confalonieri, U. E., & Patz, J. A. (2000). Climate change and vector-borne diseases: a regional analysis. Bulletin of the world health organization, 78(9), 1136-1147.
- Ebi, K. L., Ogden, N. H., Semenza, J. C., & Woodward, A. (2017). Detecting and attributing health burdens to climate change. Environmental health perspectives, 125(8), 085004.
- Mordecai, E. A., Cohen, J. M., Evans, M. V., Gudapati, P., Johnson, L. R., Lippi, C. A., ... & Weikel, D. P. (2017). Detecting the impact of temperature on transmission of Zika, dengue, and chikungunya using mechanistic models. PLoS neglected tropical diseases, 11(4), e0005568.
- Rogers, D. J., Randolph, S. E. (2006). Climate change and vector-borne diseases. Adv Parasitol, 62, 345-81.
- Rohr, J. R., Dobson, A. P., Johnson, P. T., Kilpatrick, A. M.,Paull, S. H., Raffel, T. R., ... & Thomas, M. B. (2011). Frontiers in climate change–disease research. Trends in ecology & evolution, 26(6), 270-277.
- Naish, S., Hu, W., Mengersen, K., Tong, S. (2014). Forecasting the future risk of Dengue Fever in Queensland, Australia using Climate Change Scenarios. PLoS One, 9(3), e89524.
- Semenza, J. C., & Menne, B. (2009). Climate change and infectious diseases in Europe. The Lancet infectious diseases, 9(6), 365-375.
- Harvell, C. D., Mitchell, C. E., Ward, J. R., Altizer, S.,Dobson, A. P., Ostfeld, R. S., & Samuel, M. D. (2002). Climate warming and disease risks for terrestrial and marine biota. Science, 296(5576), 2158-2162.
- Epstein, P. R. (2001). Climate change and emerging infectious diseases. Microbes and infection, 3(9), 747-754.
- McIntyre, K. M., Setzkorn, C., Hepworth, P. J., Morand, S., Morse, A. P., & Baylis, M. (2017). Systematic assessment of the climate sensitivity of important human and domestic animals pathogens in Europe. Scientific reports, 7(1), 7134.
- Chaves, L. F., & Koenraadt, C. J. (2010). Climate change and highland malaria: fresh air for a hot debate. The Quarterly review of biology, 85(1), 27-55.
- Siraj, A. S., Bouma, M. J., Santos-Vega, M., Yeshiwondim,K., Rothman, D. S., Yadeta, D., et al. (2014). Temperature and population density effects on malaria transmission in sub- Saharan Africa. Proc Natl Acad Sci U S A, 111(22), 7910-5.
- Ogden, N. H., Bouchard, C., Kurtenbach, K., Margos, G., Lindsay, L. R., Trudel, L. et al. (2010). Active dispersal of Ixodes scapularis evident in its overland patterns of spread. Parasit Vectors, 3(1), 1-9.
- Metcalf, C. J., Lessler, J. (2017). Opportunities and challenges in modeling emerging infectious diseases. Science, 357(6347), 149-52.
- Caminade, C., McIntyre, K. M., & Jones, A. E. (2019).Impact of recent and future climate change on vectorâ?ÂÃÂ?ÂÂborne diseases. Annals of the New York Academy of Sciences, 1436(1), 157-173.
- Kilpatrick, A. M., & Randolph, S. E. (2012). Drivers, dynamics, and control of emerging vector-borne zoonotic diseases. The Lancet, 380(9857), 1946-1955.
- Wu, X., Lu, Y., Zhou, S., Chen, L., & Xu, B. (2016).Impact of climate change on human infectious diseases: Empirical evidence and human adaptation. Environment international, 86, 14-23.
- Caminade, C., Kovats, S., Rocklov, J., Tompkins, A. M., Morse,P., Colón-González, F. J., ... & Lloyd, S. J. (2014). Impact of climate change on global malaria distribution. Proceedings of the National Academy of Sciences, 111(9), 3286-3291.
- Altizer, S., Ostfeld, R. S., Johnson, P. T., Kutz, S., & Harvell,C. D. (2013). Climate change and infectious diseases: from evidence to a predictive framework. science, 341(6145), 514- 519.
- Brown, H. E., Yates, K. F., Dietrich, E. A., Travis, D., Harden,J. J., Lian, X. et al. (2018). Modeling climate change effects on vector-borne diseases in North America. Environ Health Perspect, 126(5), 057008.
- Semenza, J. C., & Suk, J. E. (2018). Vector-borne diseases and climate change: a European perspective. FEMS microbiology letters, 365(2), fnx244.
- Mordecai, E. A., Caldwell, J. M., Grossman, M. K., Thomas,M. B. (2019). The impact of temperature on parasite infection rates in hosts: empirical and theoretical perspectives. Proc Biol Sci, 286(1907), 20192451.
- Ryan, S. J., Carlson, C. J., Mordecai, E. A., & Johnson, L. R. (2019). Global expansion and redistribution of Aedes-borne virus transmission risk with climate change. PLoS neglected tropical diseases, 13(3), e0007213.
- Carlson, C. J., Albery, G. F., Merow, C., Trisos, C. H.,Zipfel, C. M., Eskew, E. A., ... & Bansal, S. (2022). Climate change increases cross-species viral transmission risk. Nature, 607(7919), 555-562.
- Martens, W. J., Niessen, L. W., Rotmans, J., Jetten, T. H., & McMichael, A. J. (1995). Potential impact of global climate change on malaria risk. Environmental health perspectives, 103(5), 458-464.
- Ogden, N. H., Lindsay, L. R., Morshed, M., Sockett, P. N., & Artsob, H. (2009). The emergence of Lyme disease in Canada. Cmaj, 180(12), 1221-1224.
- Gething, P. W., Smith, D. L., Patil, A. P., Tatem, A. J., Snow,R. W., & Hay, S. I. (2010). Climate change and the global malaria recession. Nature, 465(7296), 342-345.
- Lafferty, K. D., & Mordecai, E. A. (2016). The rise and fall of infectious disease in a warmer world. F1000Research, 5, F1000-Faculty.
- Rocklöv, J., & Dubrow, R. (2020). Climate change: an enduring challenge for vector-borne disease prevention and control. Nature immunology, 21(5), 479-483.
- Parham, P. E., & Michael, E. (2010). Modeling the effects of weather and climate change on malaria transmission. Environmental health perspectives, 118(5), 620-626.
- Reiner, R. C., Stoddard, S. T., Forshey, B. M., King, A. A., Ellis, A. M., Lloyd, A. L. et al. (2013). A systematic review of Dengue and the Aedes aegypti mosquito: ecosystem consequences and disease control. PLoS Negl Trop Dis, 7(3), e2056.
- Liu-Helmersson, J., Stenlund, H., Wilder-Smith, A., & Rocklöv, J. (2014). Vectorial capacity of Aedes aegypti: effects of temperature and implications for global dengue epidemic potential. PloS one, 9(3), e89783.
- Messina, J. P., Brady, O. J., Pigott, D. M., Golding, N., Kraemer,M. U., Scott, T. W., ... & Hay, S. I. (2015). The many projected futures of dengue. Nature Reviews Microbiology, 13(4), 230- 239.
- Liu, C., Hofstra, N., Franz, G. (2019). Impacts of climate change on the risk of Leptospirosis. PLoS Negl Trop Dis, 13(10), e0007933.
- Rosenthal, J. (2009). Climate change and the geographic distribution of infectious diseases. EcoHealth, 6, 489-495.
- Monaghan, A. J., Morin, C. W., Steinhoff, D. F., Wilhelmi, O., Hayden, M., Quattrochi, D. A., ... & Ernst, K. (2016). On the seasonal occurrence and abundance of the Zika virus vector mosquito Aedes aegypti in the contiguous United States. PLoS currents, 8, ecurrents-outbreaks.
- Shuman, E. K. (2010). Global climate change and infectious diseases. N Engl J Med, 362(12), 1061-3.
- Randolph, S. E., & Rogers, D. J. (2010). The arrival, establishment and spread of exotic diseases: patterns and predictions. Nature Reviews Microbiology, 8(5), 361-371.
- Ogden, N. H., Radojevic, M., Wu, X., Duvvuri, V. R., Leighton, P. A., & Wu, J. (2014). Estimated effects of projected climate change on the basic reproductive number of the Lyme disease vector Ixodes scapularis. Environmental health perspectives, 122(6), 631-638.
- Patz, J. A., & Olson, S. H. (2006). Malaria risk and temperature: influences from global climate change and local land use practices. Proceedings of the National Academy of Sciences, 103(15), 5635-5636.
- Metcalf, C. J., Lessler, J. (2017). Opportunities and challenges in modeling emerging infectious diseases. Science, 357(6347), 149-52.
- Liang, L., & Gong, P. (2017). Climate change and human infectious diseases: A synthesis of research findings from global and spatio-temporal perspectives. Environment international, 103, 99-108.
- Mills, J. N., Gage, K. L., Khan, A. S. (2010). Potential influence of climate change on vector-borne and zoonotic diseases: A review and proposed research plan. Environ Health Perspect,118(11), 1507-14.
- Lindsay, L. R., Ogden, N. H., Schramm, P. J., Jones, J. M. (2021). Climate change and infectious diseases in North America: The road ahead. Can Commun Dis Rep, 47(10), 402-8.
- Rohr, J. R., Dobson, A. P., Johnson, P. T., Kilpatrick, A. M.,Paull, S. H., Raffel, T. R., ... & Thomas, M. B. (2011). Frontiers in climate change–disease research. Trends in ecology & evolution, 26(6), 270-277.
- Beard, C. B., Eisen, R. J., Barker, C. M., Garofalo, J. F., Hahn,M. B., Hayden, M. H., et al. (2016). Chikungunya and Zika virus: the impact of climate change on vectors and disease distribution. Curr Environ Health Rep, 3(1), 72-9.
- Brunkard, J. M., López, J. L. R., Ramirez, J., Cifuentes, E., Rothenberg, S. J., Hunsperger, E. A., ... & Haddad, B. M. (2007). Dengue fever seroprevalence and risk factors, Texas– Mexico border, 2004. Emerging infectious diseases, 13(10), 1477.
- Neiderud, C. J. (2015). How urbanization affects the epidemiology of emerging infectious diseases. Infection ecology & epidemiology, 5(1), 27060.
- Balbus, J. M., Crimmins, A., Gamble, J. L., Easterling, D. R., Kunkel, K. E., Saha, S., et al. (2016). The impacts of climate change on human health in the United States: A scientific assessment. Global Change Research Program.
- Mordecai, E. A., Cohen, J. M., Evans, M. V., Gudapati, P., Johnson, L. R., Lippi, C. A., ... & Weikel, D. P. (2017). Detecting the impact of temperature on transmission of Zika, dengue, and chikungunya using mechanistic models. PLoS neglected tropical diseases, 11(4), e0005568.
- Cascio, A., Bosilkovski, M., Rodriguez-Morales, A. J., & Pappas, G. (2011). The socio-ecology of zoonotic infections. Clinical microbiology and infection, 17(3), 336- 342.
- Estrada-Peña, A., Ostfeld, R. S., Peterson, A. T., Poulin, R., & de la Fuente, J. (2014). Effects of environmental change on zoonotic disease risk: an ecological primer. Trends in parasitology, 30(4), 205-214.
- Semenza, J. C., Rocklöv, J. (2022). Climate change and viral hemorrhagic fevers. Lancet Planet Health, 6(5), e379-85.
- Bett, B., Lindahl, J., Grace, D. (2017). Climate change and vector-borne diseases: Insights from Africa. Curr Opin Environ Sustain, 25, 45-52.
- Hotez, P. J. (2021). Neglected tropical diseases in the Anthropocene: the cases of Dengue, Zika, and Chikungunya. PLoS Negl Trop Dis, 15(3), e0009243.



