Case Report - (2022) Volume 7, Issue 3
Tacrolimus-induced Reversible Cerebral Vasoconstriction Syndrome after Heart Transplant: Case Report
Received Date: Jul 11, 2022 / Accepted Date: Jul 18, 2022 / Published Date: Jul 25, 2022
Copyright: ©Koichi Inoue, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Citation: Koichi Inoue, Satoshi Kainuma, Daisuke Yoshioka, Koichi Toda, Shigeru Miyagawa (2022) Tacrolimus-induced Reversible Cerebral Vasoconstriction Syndrome after Heart Transplant: Case Report. Cardio Open, 7(3): 269-270.
Abstract
We describe the case of a patient with a recurrent severe headache that occurred after heart transplant surgery. She was diagnosed with reversible cerebral vasoconstriction syndrome (RCVS) since typical imaging was seen through brain contrast computed tomography. Tacrolimus, an immunosuppressant, was suspected as the cause of the RCVS. The treatment was switched to cyclosporine, after which there was rapid improvement of her symptoms. This case highlights the importance of an immediate diagnosis to switch immunosuppressants to relieve symptoms and prevent progression to severe neurological dysfunction.
Keywords
Heart Transplant, Cerebral vasoconstriction, Immunosuppressant
Introduction
Reversible cerebral vasoconstriction syndrome (RCVS) is a rare condition characterized by an acute, recurrent and severe head- ache called “thunderclap headache”. This condition is seen in imaging as multifocal segmental vasoconstriction of cerebral arteries. Although the pathogenesis of the RCVS remains un- clear, it has been reported that the disease can occur in certain situations such as exposure to vasoactive or immunosuppres- sive drugs, and prevail throughout the postpartum period [1,2]. The diagnosis of RCVS needs a high level of clinical suspicion. Herein, we describe a successfully treated case of tacrolimus-in- duced RCVS after heart transplant.
Case Presentation
A 44-year-old woman with a history of dilated cardiomyopathy, who had been supported with a left ventricular assist device for four years, underwent heart transplant. A triple-drug regimen consisting of prednisolone, mycophenolate mofetil, and tacroli- mus was initiated. Since she had mild renal dysfunction, basilix- imab was injected in advance. Tacrolimus was initiated on the fifth day after surgery.
She suddenly presented with a thunderclap headache and vomit- ing six days after the operation. Although brain computed tomog- raphy (CT) demonstrated, no signs of haemorrhage or infarc- tion were detected. She also had hypertension; thus, a calcium channel blocker was promptly administered, which achieved well-controlled blood pressure. However, recurring symptoms required her to take analgesics in Figure 1. Therefore, brain CT angiography was performed, which revealed the typical “strings and beads” appearance due to segmental vasoconstriction of bi- lateral posterior cerebral arteries (Figure 2A, white arrowheads). Based on these findings, she was diagnosed with RCVS.
Figure 1: Clinical timeline after heart transplant. Black arrows mean using of analgesics for headache. Headache did not improve despite decreased blood pressure, but it promptly improved after cyclosporine replaced tacrolimus.
Figure 2A: Computed tomography angiographic imaging at the time of onset of thunderclap headache. Multifocal segmental vasoconstriction of bilateral posterior cerebral arteries was ob- served (white arrowheads).
Tacrolimus, a drug suspected to cause the RCVS, was discontin- ued although its blood concentration was within the target range, and cyclosporine was given instead. The symptoms immediately improved and never recurred. Signs of allograft rejection were not observed and she was discharged without any neurological complications. Release of cerebrovascular constrictions was observed on subsequent brain magnetic resonance angiography (MRA) three months after discharge (Figure 2B, white arrow- heads).
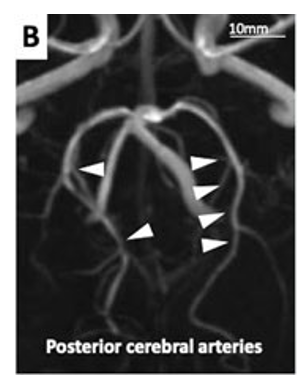
Figure 2B: Magnetic resonance angiography done three months after discharge. Vasoconstriction of cerebral arteries improved (white arrowheads).
Discussion and Conclusion
RCVS is characterized by acute and repetitive thunderclap headache and the multi-segmental vasoconstriction of cerebral arteries on imaging. Prompt diagnosis and treatment are vitally important because RCVS may progress to encephalopathy, cere- bral infarction and haemorrhage [1,2]. Although brain MRA is a useful diagnostic modality, CT angiography was initially per- formed in this case since temporary epicardial pacing leads were placed after surgery, which led to the diagnosis of the RCVS [3]. Moreover, a high level of clinical suspicion is necessary for the diagnosis since it is an underappreciated disease among clini- cians.
Management of the RCVS usually consists of resting, treating symptoms (e.g. analgesics), and controlling the blood pressure. Calcium channel blockers have been reported to be effective in relieving the symptoms, but their impact on cerebral vasocon- striction or stroke severity remains unclear [1,2]. In addition, like our case, some patients have refractory symptoms despite achieving a well-controlled blood pressure. This case emphasiz- es withdrawal of the causative drug as the most effective treat- ment for improving the symptoms, and for relieving cerebrovas- cular constrictions seen on subsequent imaging [4,5].
RCVS should be considered as a possible cause of headache in heart transplant recipients because an immunosuppressive agent may be the trigger. Immediately changing immunosuppressants is effective for cases with these conditions.
Ethics Approval and Consent to Participate and for Publication
The Institutional Review Board of Osaka University Hospital approved this paper, and the patient for the use of records and publication gave written informed consent. The procedures fol- lowed were in accordance with the Declaration of Helsinki.
Author’s contributions: Conception and design of study by Koichi Inoue, Satoshi Kainuma and Daisuke Yoshioka. Draft- ing the manuscript by Koichi Inoue. Revising the manuscript critically for important intellectual content by Koichi Toda and Shigeru Miyagawa. All authors read and approved the final man- uscript.
References
- Ducros, A. (2012). Reversible cerebral vasoconstriction syndrome. The Lancet Neurology, 11(10), 906-917.
- Cappelen-Smith, C., Calic, Z., & Cordato, D. (2017). Re- versible cerebral vasoconstriction syndrome: recognition and treatment. Current treatment options in neurology, 19(6), 1-15.
- Chen, S. P., Fuh, J. L., Wang, S. J., Chang, F. C., Lirng, J.F., Fang, Y. C., ... & Wu, J. C. (2010). Magnetic resonance angiography in reversible cerebral vasoconstriction syn- dromes. Annals of neurology, 67(5), 648-656.
- Ueki, H., Sanayama, Y., Miyajima, A., Tsuchimochi, T., Ig- arashi, S., & Sunami, S. (2016). Reversible cerebral vaso- constriction syndrome promptly diagnosed with magnetic resonance imaging including magnetic resonance angiog- raphy during immunosuppressive therapy in a 16-year-old girl with refractory cytopenia of childhood. Hematology Reports, 8(4), 6673.
- Gonzalezâ?Martinez, A., Romeroâ?Palacián, D., Dotor Garcíaâ?Soto, J., Sánchez, P., Reig Roselló, G., & Zapata Wainberg, G. (2019). Tocilizumabâ?Associated Reversible Cerebral Vasoconstriction: A Case Report. Headache: The Journal of Head and Face Pain, 59(2), 259-263.




