Research Article - (2024) Volume 2, Issue 10
Study of Iron Deficiency Anemia in First Three Trimesters of Pregnant Women During in RAMADAN: A Prospective Study
2Department of Pharmacology and Toxicology, Zubaeda Alsayeh, University of Zawia, Faculty of Pharmacy, Az Zawiyah, Libya
Received Date: Oct 21, 2024 / Accepted Date: Nov 19, 2024 / Published Date: Nov 21, 2024
Copyright: ©Ã?©2024 Ahmed Ali Ebshena, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Ebshena, A. A., Alsayeh, Z. M. (2024). Study of Iron Deficiency Anemia in First Three Trimesters of Pregnant Women During in RAMADAN: A Prospective Study. Int Internal Med J, 2(10), 01-06.
Abstract
Background: Iron deficiency is defined as a condition in which Hemoglobin (Hb) level in the body is lower than normal, which results in decreased oxygen-carrying capacity of red blood cells to tissues, Pregnant women with Iron Deficiency Anemia are at a higher risk of postpartum hemorrhage.
Methods: This study was a prospective analytical study conducted at the Sabratha Laboratory from RAMADAN 2021 to 2023. This study was conducted on all pregnant women with hemoglobin level less than 11 gm/dl in the first trimester and less than 10 gm/dl in the second and third trimesters. Data were 30 cases collected by studying from the Sabratha Laboratory in Libya. A self-designed questionnaire was used. The questionnaire was translated into the Arabic language for ease of understanding and administration to study the population.
Conclusion: To improve maternal and fetal outcomes, it is recommended that primary health care has to be strengthened and high priority has to be given to aspects such as prevention, early diagnosis, and treatment of anemia in pregnancy before Fasting Ramadan.
Keywords
Iron Deficiency, Anemia, Pregnancy
Introduction
Background
Iron deficiency is defined as a condition in which Hemoglobin (Hb) level in the body is lower than normal, which results in decreased oxygen-carrying capacity of red blood cells to tissues [1]. It affects all age groups, but pregnant women and children are more vulnerable. Stevens et al., reported that the global prevalence of anemia in non-pregnant women, pregnant women and children is 29, 38 and 43%, correspondingly [2].
According to the WHO guidelines, anemia in pregnancy is defined as a hemoglobin level < 11 g/dL in the first trimester and less than 10g/dl in the second and third trimesters [3]. The prevalence of anemia is an important health indicator.
Iron deficiency (ID) and iron deficiency anemia (IDA) are a global health problem affecting developing and developed countries. Pregnant women were identified as a risk group due to adverse outcome on pregnancy, maternal and fetal outcome Pregnant women with IDA are at a higher risk of postpartum hemorrhage (PPH), receiving blood transfusion, and heart failure. In addition, Iron deficiency (ID) and iron deficiency anemia IDA during pregnancy can be considered as a risk factor for preterm delivery, low birth weight, perinatal, and neonatal mortality Maternal iron deficiency, with or without associated anemia, has an adverse effect on fetal iron status because decreased maternal hemoglobin concentration is associated with decreased fetal iron stores.
Physiologically, plasma volume expands by 25–80% of prepregnancy volumes between the second trimester and the middle of the third trimester of pregnancy [4]. This induces a modest decrease in Hb levels during Pregnancy which is called physiological hemodilution. Previous studies show that the best time to investigate any risk factors associated with anemia maybe up 20 weeks of gestation [5].
Anything deed is performed by any Muslim is classified according to Islamic law as either essential (Wajib), recommended (Sunnah), permissible (Harus), offensive (Makruh) or unlawful (Haram). He/she gets reward accordingly [6]. Fasting in the month of Ramadan, the ninth month of the Islamic calendar is one of the five fundamental pillars of Islam and is an essential (Wajib) act whose performance is rewarded by Allah and nonperformance punished [7]. However, there are a few categories of people who are exempted from this religious obligation which include children under the age of puberty, mentally incapacitated, old frail elderly, acutely unwell, travelers, menstruating women and pregnant.
Goal of the Study
- The present study was carried out to examine the knowledge, beliefs, attitude, and practices of pregnant Muslims regarding fasting during the month of Ramadan and to determine the association of demographic variables (Age, Parity, Educational Status, Duration of Pregnancy, Co-morbidities) with the frequency of fasting.
- The prospective observational study is undertaken to estimate the prevalence and to study maternal and early neonatal morbidity and mortality associated with anemia in a pregnant woman.
Material and Method
Study Design
This study was a prospective analytical study conducted at the Sabratha Laboratory from RAMADAN 2021 to 2023.
This study was conducted on all pregnant women with hemoglobin level less than 11 gm/dl in the first trimester and less than 10 gm/dl in the second and third trimesters. Data were 190 cases collected by studying from the Sabratha Laboratory in Libya.
A self-designed questionnaire was used. The questionnaire was translated into the Arabic Language for ease of understanding and administration to study the population.
The questionnaire comprised two parts, first part contained the demographic variables (age, parity, educational status, duration of current pregnancy, co-diabetes). ,asthma, hypertension) morbidities The second part contained the research variables (knowledge regarding fasting during pregnancy, observation of fasting during Ramadan, knowledge about “fasting compensation” after delivery , consultation with the doctor before deciding to fast during pregnancy in Ramadan, the reason for not fasting during pregnancy, possible harms of fasting in pregnancy, and adversities encountered during fasting, is fasting in pregnancy more difficult than without pregnancy).
Exclusion criteria were patients information was gathered about the patient’s medical history such as pulmonary, cardiac or cerebrovascular disease, diabetes, hypertension, any malignancy, medication intoxications, Pulmonary disease.
Statistical Analysis
The data was entered and analyzed in SPSS version 22. Frequencies and percentages were tabulated for demographic characteristics and their relation to fasting and their beliefs. Chi- square test was used to analyze this association with p-value <0.05 considering statistically significant.
The Results
Table I: Demographic Characteristics of the Study.(n=190)
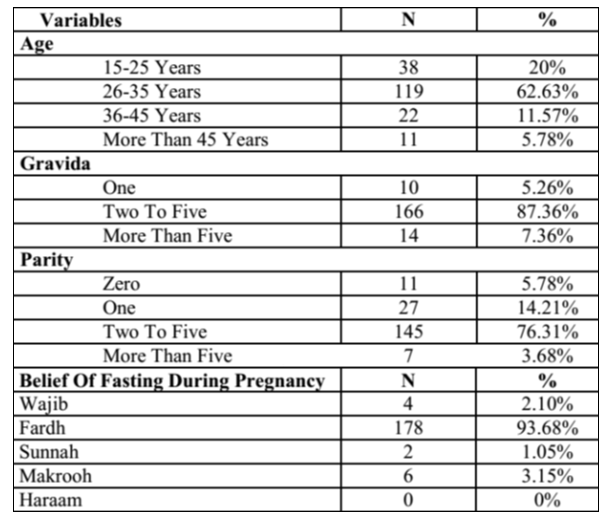
The in general response rate was 94% (190/250). The responses given to the questionnaire are given in the tables.77% fasted during Ramadan, out of which 50% fasted for a duration of 11 to 20 days and 95% considered fasting in pregnancy difficult than otherwise.71% consulted a doctor for decision regarding fasting. 94% considered it “Wajib” with 91% being aware of fasting compensation after delivery. 47% perceived, feeling of weakness due to lack of nutritionâ?? as the main risk of fasting. Educational status, presence of co-morbidity and duration of pregnancy were positively associated with fasting (p-value <0.05).
Figure 2: Fasting Rates by Trimester
Overall fasting rate in the sample and fasting rates by pregnancy trimester overlap with Ramadan
All interviewees, 35% reported having fasted during pregnancy. 47% of the fasting women reported fasting at least 20 days, while the fasting rate is highest in the first pregnancy trimester (Fig 2). Women who fast during pregnancy are likely to be more religious.
Figure 2: Belief of Fasting RAMADAN During Pregnancy
Figure 2. shows a lot of women believed in fasting Ramadan during while pregnant was Fardh (93.68%), The prevalence of anemia is an important health indicator, otherwise, Iron deficiency (ID) and iron deficiency anemia (IDA) are global health problems affecting developing and developed countries. Pregnant women were identified as a risk group due to adverse outcomes in pregnancy, maternal and fetal outcomes Pregnant women with IDA are at a higher risk of postpartum hemorrhage (PPH), receiving a blood transfusion, and heart failure.
Discussion
before making the decision of whether to fast during Ramadan or not. 89% of the husbands forbade their wives to observe fasting during Ramadan out of which 12% still opted to fast despite husband’s restriction. According to previous studies, there are many predictors which influence the fasting behaviors of the pregnant women, doctors and hundreds decision being the top of the list [5,6]. 7% of the spouses restricted their wives from fasting during Ramadan according to Singaporean research [8]
In contrary to our results, 72.4% never consulted their doctors for pre-Ramadan Advice in a research [4]. study, 94% were aware of the religions obligation regarding Ramadan fasting as an essential act and a similar percentage were aware about the fasting compensation (“Qada”) with a percentage of 90%.
According to a study carried out in Thailand to assess the basic knowledge of pregnant women regarding Islamic law, attitude and practices of Ramadan fasting during pregnancy, most of the participants (85.5%) .
60% of the non-fasting women were worried about the weakness they may face during the fasting hours. 95% said that fasting during pregnancy is more difficult than in non-pregnancy state and 48% of the respondents faced hunger/thirst as the most common adverse effect of fasting. 47% considered feeling weak due to lack of nutrition as a risk due to fasting while 25% considered fasting during the state of pregnancy as risk-free. Lou A et al reported that 62% of the pregnant women believed that fasting was harmful to themselves, their foetus, on both [9]. In contrary to this, a Thailand based research concluded that majority of the pregnant women believed that fasting during pregnancy did no harm to maternal health [10].
There was positive correlation of fasting with duration of pregnancy, educational status and co-morbidities while no relationship with age and parity was seen. Many previously conducted researches show similar trends with positive correlation of fasting gestational age and educational status presence of co-morbidities in form of either debates mellitus, hypertension, asthma or ischemic heart disease also showed significant correlation with the frequency of fasting a limitations of our study was that it did not check the association of socioeconomic status with the fasting frequency as was seen by studies carried out previously in this domain [5,6,11,12].
Conclusions and Recommendations
The high prevalence of anemia in pregnant women indicates that Iron deficiency continues to be a major public health problem. Iron deficiency Anemia in pregnancy increases maternal and fetal risks, female literacy, and bad obstetric history were important risk factors contributing to anemia in pregnant women. To improve maternal and fetal outcomes, it is recommended that primary health care has to be strengthened and high priority has to be given to aspects such as prevention, early diagnosis, and treatment of anemia in pregnancy before Fasting Ramadan.
Acknowledgements
The authors would like to thank the staff and anesthesiology team at Libyan Teaching Hospital for their help and support during the research study. They appreciate their cooperation which was invaluable in enabling the author to conduct the research, and also, they are grateful to who participated in the study.
Disclosure Statement
No potential conflict of interest was reported by the authors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors Contribution
Ahmed EBshena and ZUBAEDA ALSAYEH conducting studies, interpreting data, and drafting the manuscript. Both authors approved the paper for publication
Authors Contribution
AAE and ZMA conducting study, interpreted data and draft the manuscript. All authors approved the paper for publication
References
- Hassan, M. M. (2017). ĪmÄn, IslÄm, taqwÄ, kufr, shirk, and nifÄq: Definitions, examples and impacts on human life.
- Ghouri, N., Hussain, S., Mohammed, R., Beshyah, S. A., Chowdhury, T. A., Sattar, N., & Sheikh, A. (2018). Diabetes, driving and fasting during Ramadan: the interplay between secular and religious law. BMJ Open Diabetes Research and Care, 6(1), e000520.
- Abolaban, H., & Al Moujahed, A. (2017). Muslim patients in Ramadan: a review for primary care physicians. Avicenna journal of medicine, 7(03), 81-87.
- Masood, S. N., Saeed, S., Lakho, N., Masood, Y., Ahmedani,M. Y., & Shera, A. S. (2018). Pre-Ramadan health seeking behavior, fasting trends, eating pattern and sleep cycle in pregnant women at a tertiary care institution of Pakistan. Pakistan Journal of Medical Sciences, 34(6), 1326.
- van Bilsen, L. A., Savitri, A. I., Amelia, D., Baharuddin, M., Grobbee, D. E., & Uiterwaal, C. S. (2016). Predictors of Ramadan fasting during pregnancy. Journal of epidemiology and global health, 6(4), 267-275.
- Glazier, J. D., Hayes, D. J., Hussain, S., D’Souza, S. W., Whitcombe, J., Heazell, A. E., & Ashton, N. (2018). The effect of Ramadan fasting during pregnancy on perinatal outcomes: a systematic review and meta-analysis. BMCpregnancy and childbirth, 18, 1-11.
- Savitri, A. I. (2016). Maternal nutrition and newborn health outcome (Doctoral dissertation, Utrecht University).
- Adler-Lazarovits, C., & Weintraub, A. Y. (2019). Physicians’ attitudes and views regarding religious fasting during pregnancy and review of the literature. European Journal of Obstetrics & Gynecology and Reproductive Biology, 233, 76-80.
- Lou, A., & Hammoud, M. (2016). Muslim patients’ expectations and attitudes about Ramadan fasting during pregnancy. International Journal of Gynecology & Obstetrics, 132(3), 321-324.
- Hassanein, M., Al-Arouj, M., Hamdy, O., Bebakar, W. M. W., Jabbar, A., Al-Madani, A., ... & Ben-Nakhi, A. (2017). Diabetes and Ramadan: practical guidelines. Diabetes research and clinical practice, 126, 303-316.
- Mubeen, S. M., Mansoor, S., Hussain, A., & Qadir, S. (2012). Perceptions and practices of fasting in Ramadan during pregnancy in Pakistan. Iranian Journal of Nursing and Midwifery Research, 17(7), 467-471.
- Saro, S., & Tanawattanacharoen, S. (2018). Knowledge, attitudes and practices of Ramadan fasting in pregnant Thai-Muslim women. Thai Journal of Obstetrics and Gynaecology, 83-95.




