Research Article - (2025) Volume 4, Issue 2
Primordial Silence and Therapeutic Presence: Theodicy and the Paradox of Divine Concealment in Clinical Practice
Received Date: May 12, 2025 / Accepted Date: Jun 05, 2025 / Published Date: Jun 20, 2025
Copyright: ©©2025 Julian Ungar-Sargon. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Ungar-Sargon, J. (2025). Primordial Silence and Therapeutic Presence: Theodicy and the Paradox of Divine Concealment in Clinical Practice. Biomed Sci Clin Res, 4(2), 01-10.
Abstract
This essay examines the theological concept of divine presence manifesting through absence as articulated in the Talmudic passage Menachot 29b, where Moses witnesses Rabbi Akiva's martyrdom and receives God's enigmatic response: "Be silent, for such is My decree." Drawing on contemporary therapeutic frameworks developed by Dr. Julian Ungar-Sargon, this analysis explores how the paradox of divine concealment (hester panim) informs clinical practice, particularly in contexts of inexplicable suffering and existential crisis. The essay argues that the therapeutic encounter mirrors the theological tension between divine accessibility in interpretive partnership and divine mystery in the face of suffering, offering a framework for understanding healing that transcends purely biomedical paradigms [1,2].
Keywords
Theodicy, Divine Concealment, Hester Panim, Tzimtzum, Talmud Menachot 29b, Rabbi Akiva, Therapeutic Presence, Narrative Medicine, Spirituality in Healthcare, Clinical Practice, Doctor-Patient Relationship, Sacred Silence, Meaning-Making, Moral Injury, Healthcare Worker Burnout, Palliative Care, Embodied Experience, Hermeneutical Medicine, Integrative Healthcare
Introduction
The Babylonian Talmud's account in Menachot 29b presents one of the most theologically challenging narratives in rabbinic literature. After witnessing Rabbi Akiva's interpretive brilliance—his ability to derive "heaps and heaps of halakhot" from the crowns on Torah letters—Moses asks to see Akiva's reward, only to witness his brutal martyrdom at Roman hands. Moses's anguished question, "Such Torah, and such a reward?" receives the divine response: 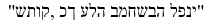 ("Be silent, for such is My decree").
("Be silent, for such is My decree").
This theological encounter between human demand for justice and divine inscrutability has profound implications for contemporary therapeutic practice. The intersection of spirituality and medicine has become increasingly recognized as essential to comprehensive healthcare [3,4]. Our work on the theological dimensions of healing, particularly his exploration of divine presence and concealment in therapeutic spaces, provides a crucial framework for understanding how this ancient theodicy informs modern clinical encounters [5]. His essays at jyungar.com systematically develop what might be called a "theology of therapeutic presence" that recognizes the sacred-profane dialectic inherent in healing relationships, addressing a growing need in healthcare for approaches that integrate meaning-making with clinical intervention [6].
The Structure of Divine Silence
The Menachot 29b narrative establishes a fundamental tension between two modes of divine engagement. In the first section, God engages Moses in detailed dialogue about the crowns on letters, explaining Akiva's future interpretive genius and even allowing Moses to observe Akiva's teaching. This represents what we might call the dialogical mode of divine presence—accessible, explanatory, and collaborative.
However, when Moses witnesses Akiva's martyrdom and questions divine justice, God's response shifts dramatically to the apophatic mode—the theology of divine concealment [7]. The command to "be silent" does not represent theological evasion but rather the recognition that some experiences transcend rational discourse and require what we describe as "revelation in concealment" [8].
This structural shift parallels what we identify in therapeutic encounters as the movement between explicable medical discourse and the irreducible mystery of suffering [9]. In our clinical work, we has "repeatedly encountered the limitations of conventional clinical discourse when working with patients with chronic neurological disease whose experiences resist categorization or exceed the boundaries of diagnostic language" [10]. This limitation is particularly acute in addressing what narrative medicine scholars have termed the "suffering that cannot be spoken" [11,12].
Divine Concealment and Clinical Practice
Our theological framework explicitly engages with the concept of hester panim (divine concealment), a theme that resonates deeply with the Menachot passage. His essay "Mariupol and Warsaw Ghetto: Theodicy Then and Now" raises the fundamental question: "Are there times when the suffering of exile is so profound that this covenant is called into question (hester panim) [13].?"
This question becomes clinically relevant when practitioners encounter patients whose suffering appears to exceed any meaningful therapeutic intervention. The physician who treats terminally ill children, the therapist working with trauma survivors, or the neurologist confronting degenerative disease often finds themselves in Moses's position—witnessing suffering that challenges fundamental assumptions about justice, meaning, and divine presence. Contemporary research on moral injury among healthcare workers demonstrates how these encounters lead to profound spiritual and existential crisis [14,15].
Our response to this clinical-theological crisis does not involve abandoning the sacred dimensions of healing but rather developing what he calls a "tzimtzum model" of therapeutic presence [16]. Drawing on the kabbalistic concept of divine contraction, this approach recognizes that therapeutic effectiveness sometimes requires the practitioner to create space for mystery rather than rushing to explanatory frameworks. This parallels developments in narrative medicine that emphasize the importance of bearing witness to patient suffering without immediate intervention [17,18].
The Paradox of Presence Through Absence
The divine command to Moses—"Be silent"—establishes a theological principle that we have systematically developed. Our "Divine presence and concealment in the therapeutic space" explores how healing relationships embody the paradox articulated in Menachot 29b: divine presence is sometimes most authentically encountered through the absence of explanation [19].
This paradox operates on multiple levels:
Epistemological: Just as Moses cannot understand Akiva's advanced interpretations despite being the source of the original revelation, practitioners often cannot fully comprehend their patients' experiences despite their medical training. This mirrors what narrative medicine theorists describe as the "hermeneutic gap" between clinical knowledge and lived experience [20,21].
Ontological: The being of both God and the therapeutic relationship transcends the categories available for description or manipulation. Research in medical humanities emphasizes how healing involves dimensions that exceed biomedical categorization [22,23].
Ethical: The demand for explanation in the face of suffering can itself become a form of violence, requiring instead what Emmanuel Levinas calls "ethical proximity" to the face of the other (24). Studies in palliative care demonstrate how premature explanatory frameworks can undermine patient dignity and meaning-making [25,26].
Clinical Applications
Our therapeutic framework translates these theological insights into practical clinical approaches. His work emphasizes "the essential unity of mind, body, and spirit while creating spaces for therapeutic encounters that honor the full personhood of patients" precisely by refusing to reduce patient experience to explanatory categories [27]. This approach aligns with evidence-based research demonstrating the efficacy of spiritually-integrated healthcare interventions [28,29].
This approach manifests in several key practices:
Sacred Silence: Rather than filling therapeutic silence with interpretation or advice, practitioners learn to inhabit silence as a space of potential revelation. Like God's command to Moses, therapeutic silence becomes not an absence of engagement but a different mode of presence. Research in narrative medicine demonstrates the healing potential of witnessed silence in clinical encounters [30,31].
Hermeneutic Listening: our work on "Hermeneutic Approaches to Medicine: From Objective Evidence to Patient as Sacred Text" parallels Akiva's interpretive method, treating patient narratives as containing layers of meaning that exceed immediate comprehension [32]. This approach is supported by studies showing improved patient outcomes when clinicians attend to narrative dimensions of illness [33,34].
Tolerating Mystery: The practitioner learns to remain present with patients whose suffering resists explanation, mirroring Moses's ultimate acceptance of divine inscrutability while maintaining covenantal relationship. Clinical research on chronic illness demonstrates the importance of providers' capacity to remain present with unexplainable suffering [35,36].
The Physicians Existential Crisis
In "Beyond Theodicy: The Physician's Existential Crisis" we engage with the theological challenges raised by the Menachot passage [37]. Healthcare providers, like Moses witnessing Akiva's martyrdom, regularly encounter situations where their commitment to healing confronts the reality of inexplicable suffering and death. This phenomenon has been extensively documented in studies of physician burnout and moral injury [38,39].
The traditional biomedical model offers no adequate response to these encounters because it operates within what we identifiy as a "Cartesian dualism" that separates physical intervention from existential meaning [40]. The result is what he calls the "compromised healer"—the practitioner who maintains technical competence while experiencing spiritual crisis. Contemporary research demonstrates that over 40% of healthcare workers experience symptoms consistent with moral injury, which significantly exceeds traditional burnout measures [41,42].
Grief Work and Sacred Relationship
We framework for "caregiver's grief work" recognizes that practitioners experience cumulative trauma analogous to Moses's witnessing of Akiva's fate [43]. The medical profession's "culture of emotional stoicism" parallels the theological tendency to avoid difficult questions about divine justice. Research demonstrates that healthcare workers experience rates of depression and anxiety significantly exceeding the general population, with inadequate attention to the spiritual dimensions of this suffering [44,45].
However, we have argued that authentic healing requires practitioners to inhabit their own grief and uncertainty rather than defending against it. This involves developing what he calls "grief integration" practices that allow providers to remain present with suffering without either emotional numbing or overwhelm [46]. Studies in narrative medicine demonstrate the efficacy of reflective writing and storytelling in processing healthcare workers' cumulative trauma [47,48].
The theological parallel is significant: Moses does not abandon his relationship with God after witnessing Akiva's martyrdom, but he also does not receive easy answers. Instead, he learns to inhabit the tension between covenant and crisis, presence and absence, meaning and mystery. This reflects what researchers describe as "post-traumatic growth" in healthcare providers—the development of enhanced meaning-making capacity through encounters with suffering [49,50].
Primordial Divine Intention
In "Tzimtzum Model and Doctor-Patient Relationships" we provided an application of the Menachot 29b theological framework to clinical practice [51]. The kabbalistic concept of tzimtzum—divine self-contraction to create space for creation— offers a model for therapeutic presence that paradoxically manifests through strategic absence.
The theological depth of this connection becomes apparent when we examine the precise language used in both contexts. God's response to Moses—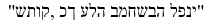 ("Be silent, for such is My decree/intention")—employs the same formulation found in the Alter Rebbe's description of the primordial divine intention preceding tzimtzum:
("Be silent, for such is My decree/intention")—employs the same formulation found in the Alter Rebbe's description of the primordial divine intention preceding tzimtzum: ![]() ("When it arose in [divine] thought 'I will reign'") [85]. This linguistic parallel suggests that the command for silence in the face of Akiva's suffering and the cosmic tzimtzum that enables creation both stem from the same primordial divine intention. In the Menachot passage, God's refusal to explain Akiva's suffering can be understood as a form of tzimtzum—not divine abandonment but rather divine contraction that creates space for human agency, meaning-making, and relationship. The command to "be silent" becomes not a shutting down of dialogue but an invitation to a different kind of encounter, rooted in the same divine "machshava" (thought/intention) that governs creation itself. This parallels therapeutic approaches that emphasize creating space for patient meaning- -making rather than imposing clinical interpretations [52,53].
("When it arose in [divine] thought 'I will reign'") [85]. This linguistic parallel suggests that the command for silence in the face of Akiva's suffering and the cosmic tzimtzum that enables creation both stem from the same primordial divine intention. In the Menachot passage, God's refusal to explain Akiva's suffering can be understood as a form of tzimtzum—not divine abandonment but rather divine contraction that creates space for human agency, meaning-making, and relationship. The command to "be silent" becomes not a shutting down of dialogue but an invitation to a different kind of encounter, rooted in the same divine "machshava" (thought/intention) that governs creation itself. This parallels therapeutic approaches that emphasize creating space for patient meaning- -making rather than imposing clinical interpretations [52,53].
The Hermeneutic Revolution as Therapeutic Model
Drawing on the scholarly analysis of Daniel Boyarin, Yair Furstenberg, and Azzan Yadin-Israel, we can understand the Menachot passage as representing a fundamental epistemological shift from prophetic authority to interpretive creativity [86,87]. This shift, which Yadin-Israel identifies as "the return of a model of interpretive authority that enjoyed great prominence in Second Temple literature," provides a theological foundation for what Susan Handelman calls the "hermeneutic revolution" that challenges Hellenic modes of abstract thought [88,89].
The therapeutic implications are profound: just as the passage legitimizes Rabbi Akiva's creative interpretation while maintaining Moses's foundational authority, the therapeutic encounter can honor both clinical expertise and patient meaning-making. The "crowns" (tagin) that enable Akiva's interpretive work become symbols of what we might call "interpretive infinity"—the principle that human experience contains more meaning than immediate clinical categories can encompass [90].
This theological framework, enriched by understanding the shared divine "machshava" underlying both tzimtzum and theodicy, translates into specific therapeutic practices that honor what contemporary scholars identify as the "hermeneutic paradox" of the Menachot passage—where traditional authority and interpretive innovation are simultaneously preserved and transformed [91]:
Diagnostic Humility: Recognizing that patient experience exceeds clinical categories, practitioners learn to hold diagnostic frameworks lightly while remaining open to dimensions of experience that resist medical explanation. Like Moses's bewilderment at Akiva's teaching, clinical humility acknowledges that patients may possess insights into their condition that exceed medical understanding. This approach is supported by research demonstrating improved patient satisfaction and clinical outcomes when providers acknowledge the limits of medical knowledge [54,55].
Presence Over Intervention: Like God's presence with Moses despite refusing explanation, therapeutic effectiveness sometimes requires being present with patients in their suffering without rushing to fix or explain. The Alter Rebbe's insight that divine intention ![]() precedes both creation and specific responses to suffering suggests that therapeutic presence itself participates in this primordial divine intention. Studies in palliative care demonstrate that patients value presence and witness as much as technical intervention [56,57].
precedes both creation and specific responses to suffering suggests that therapeutic presence itself participates in this primordial divine intention. Studies in palliative care demonstrate that patients value presence and witness as much as technical intervention [56,57].
Sacred Holding as Interpretive Space: The therapeutic relationship becomes a container for mystery and meaning-making rather than simply a vehicle for symptom reduction. Just as the "crowns" (tagin) on letters become sites of creative exegesis where human interpretive genius collaborates with divine intention, the therapeutic space becomes a realm where patient narratives can unfold their full interpretive potential. Research in chronic illness management shows that patients who experience their healthcare relationships as "sacred holding" demonstrate better coping and quality of life outcomes [58,59].
The Meta Interpretive Dimension
The passage's enduring power lies in what contemporary scholars identify as its meta-interpretive dimension—its function as a text about the nature of textual interpretation itself [90,91]. This aspect becomes therapeutically significant when we recognize that patients, like Rabbi Akiva, are engaged in creative interpretation of their illness experience, deriving meaning from the seemingly insignificant "crowns" of their symptoms, relationships, and life circumstances.
As Handelman's analysis demonstrates, the rabbinic rejection of Platonic idealism in favor of textual materialism—where meaning emerges through interpretive engagement rather than abstract contemplation—provides a model for therapeutic relationships that honor patient agency in meaning-making [88,89]. The therapeutic encounter becomes a space where, as one scholar notes, "humans are co-creators of the Torah, not merely interpreters in the usual sense of those subject to the dictates of the text explicated" [92].
This hermeneutic paradox identified in contemporary scholarship— where traditional authority and interpretive innovation are simultaneously preserved and transformed—offers a framework for understanding how clinical expertise and patient wisdom can coexist without hierarchy. The practitioner, like Moses in Akiva's study hall, may find themselves initially bewildered by patient interpretations of illness experience, yet ultimately comforted by recognizing that innovation and tradition can coexist within a single healing framework [91].
The Limits of Technological Medicine
Our critique of "scientific reductionism that can inadvertently reduce patients to collections of symptoms and laboratory values" parallels the theological critique implicit in the Menachot passage [60]. Just as Moses's prophetic authority cannot comprehend Akiva's interpretive innovation, technological medicine often cannot encompass the full reality of patient experience. This limitation becomes particularly acute in contexts of chronic illness, terminal disease, and trauma—precisely the situations where the theodicy question becomes most pressing [61,62].
The practitioner trained to intervene and cure confronts the reality of conditions that exceed technological manipulation, requiring instead what we call "therapeutic vision" that transcends conventional biomedical paradigms [63]. Contemporary research demonstrates that purely technological approaches to healthcare contribute to provider burnout and moral injury while failing to address patient spiritual needs [64,65].
Pluralistic Therapeutic Approaches
The comparative religious analysis by Holger Zellentin reveals how the Menachot passage functions as a Jewish response to Christian claims about supersession, presenting Akiva as fulfilling Moses rather than replacing him [93]. This insight has important implications for therapeutic practice in pluralistic healthcare settings, where practitioners must navigate diverse religious and spiritual frameworks for understanding suffering.
Where Christian transfiguration narratives typically present Jesus as superior to Moses, sometimes with anti-Jewish undertones, the rabbinic counter-narrative "sets up Akiva as a messianic figure, but not the Messiah; and he is martyred and his body consumed, but he is not yet resurrected" [94]. This theological stance—affirming interpretive creativity while maintaining covenantal continuity— provides a model for therapeutic relationships that honor diverse spiritual perspectives without hierarchical ranking.
The therapeutic practitioner, informed by this hermeneutic approach, can recognize that patients from different faith traditions may bring distinct frameworks for understanding suffering, healing, and meaning-making. Rather than privileging one interpretive system over another, the "tzimtzum model" suggests creating space where multiple meaning-making frameworks can coexist and inform the healing process [95,96].
Integration
The Menachot passage suggests that the tension between understanding and mystery, presence and absence, is not a problem to be solved but a fundamental structure of authentic relationship—whether with the divine or in therapeutic encounter. We propose "an integrative framework for understanding the sacred dimensions of medical practice" that honors this tension rather than resolving it [66].
This integration involves: Narrative Medicine:
Treating patient stories as sacred texts requiring interpretive sophistication analogous to Akiva's hermeneutical approach. Extensive research demonstrates the eficacy of narrative medicine in improving empathy, communication skills, and professional development among healthcare providers [67,68].
Spiritual Assessment: Recognizing that healing involves dimensions of meaning that exceed physical intervention. Studies show that patients whose spiritual needs are addressed demonstrate improved health outcomes across multiple domains [69,70].
Community Care: Understanding that like the martyrdom of Rabbi Akiva, individual suffering has communal and historical dimensions that require collective response. Research on social determinants of health emphasizes the importance of community- based approaches to healing [71,72].
Conclusion
The Talmudic passage in Menachot 29b offers more than historical insight into ancient theodicy debates; it provides a foundational framework for understanding the sacred dimensions of therapeutic relationship. We have attempted to demonstrate how this ancient theological wisdom can inform contemporary clinical practice, particularly in contexts where conventional biomedical approaches encounter their limits [73,74].
The paradox of divine presence manifesting through absence— God's command to Moses to "be silent"—becomes a model for therapeutic presence that neither abandons patients to meaningless suffering nor reduces their experience to explanatory categories. Instead, it calls practitioners to inhabit the tension between covenant and crisis, knowledge and mystery, intervention and witness. This approach is supported by growing evidence that spiritually-integrated healthcare improves both patient outcomes and provider well-being [75,76].
This approach does not abandon scientific rigor but rather situates it within a larger framework that recognizes healing as involving dimensions of meaning, relationship, and transcendence that exceed purely technological intervention [77,78]. Like Moses accepting both the interpretive partnership offered in the first part of the narrative and the divine mystery revealed in the second, practitioners learn to hold together the explicable and inexplicable dimensions of therapeutic encounter.
Ultimately, our work suggests that the most authentic response to the theodicy crisis—whether ancient or contemporary—involves neither cynical abandonment of meaning nor naive affirmation of easy answers. Instead, it requires developing capacities for what might be called "sacred silence"—the ability to remain present with mystery while maintaining commitment to healing relationship [79,80].
The theological insight of Menachot 29b, filtered through contemporary therapeutic wisdom, offers a framework for clinical practice that honors both the scientific and sacred dimensions of healing. In a healthcare environment increasingly dominated by technological reductionism and economic efficiency, this perspective provides both critique and alternative—a vision of medicine that serves not only biological function but human flourishing in its fullest sense [81,82].
The theological insight that emerges from connecting the Alter Rebbe's formulation with the Menachot passage is profound: the same divine "machshava" (intention) that governs cosmic creation through tzimtzum also governs the response to individual suffering through commanded silence. This suggests that therapeutic presence, particularly in encounters with inexplicable suffering, participates in the fundamental structure of divine creativity itself [97,98].
As Moses learned to inhabit the tension between prophetic authority and divine mystery, contemporary practitioners can learn to hold together clinical competence and sacred presence, diagnostic precision and therapeutic humility, intervention and witness. The shared language of ![]()
" reveals that this integration is not merely analogical but participates in the primordial divine intention that enables both creation and healing response to proceed through strategic absence and presence [99,100].
This integration offers hope not only for more effective healthcare but for a recovery of medicine's calling to serve the whole person in the context of ultimate meaning and relationship [83,84].
My poem "Before He Thought Silence" (August 15, 2024)[] serves as a lyrical meditation on the theological themes explored in the main essay, transforming the academic analysis of Menachot 29b into a personal contemplation of divine creativity, human suffering, and the paradoxical nature of sacred presence. The poem's structure mirrors the movement from cosmic creation through historical martyrdom to individual spiritual response, embodying the very hermeneutic process that the essay identifies in Rabbi Akiva's interpretive method.
Structural Analysis
Opening Movement: Primordial Divine Intention The poem's opening lines—"Before He thought, about this world / An idea arose in His mind, Israel"—directly invoke the theological framework established in the essay's analysis of the Alter Rebbe's formulation ![]()
("when it arose in [divine] thought"). The poem places Israel as the primordial divine intention that precedes even creation itself, establishing a theological priority that parallels the essay's argument about the shared "machshava" underlying both tzimtzum and theodicy.
The immediate transition to "In the silence of shtok kach ala bemachshava" performs a remarkable poetic compression, collapsing the temporal distance between primordial divine intention and the specific response to Rabbi Akiva's martyrdom. This compression suggests that the command to silence in the face of suffering was not a reactive divine response but part of the original creative intention—a insight that deepens the essay's theological analysis.
The Tzimtzum Metaphor: Divine Self-Limitation as Death
The poem's central metaphor—"In that first breath of life He too had to die a bit / In His plenitude, in His pleroma He too had to make room"—provides a lyrical rendering of the tzimtzum concept that the essay explores academically. The choice of "die a bit" rather than technical kabbalistic terminology makes viscerally present the cost of creation, transforming theological abstraction into embodied experience.
The breathing metaphor that dominates the poem serves multiple functions:
Physiological Immediacy: The description of "that unconscious deep inhalatory gasp recognized only when I surface after being too long submerged" grounds the cosmic drama in immediate bodily experience, paralleling the essay's emphasis on therapeutic presence that honors embodied patient experience.
Therapeutic Resonance: The reference to waterboarding—"(And they say water boarding is not torture!)"—introduces contemporary political trauma into the theological meditation, suggesting that the poem itself performs the kind of interpretive work the essay identifies in therapeutic encounters where personal, historical, and cosmic suffering intersect.
Reciprocal Relationship: The movement from divine exhalation to human inspiration to final expiration creates a cyclical structure that mirrors the essay's analysis of therapeutic relationship as mutual encounter rather than one-way intervention.
Historical Martyrdom: The Telescoping of Suffering
The poem's catalog of martyrdom—"Rabbi Akiva, and the mothers who would sacrifice their children in the churches of Mainz, Speyer and Worms, and the babies who would go up in the flames of Hitler's inferno"—performs what might be called a "telescoping of suffering" that collapses historical distance to suggest the unity of Jewish martyrological experience.
This technique parallels the essay's analysis of how therapeutic encounters involve recognizing that "individual suffering has communal and historical dimensions that require collective response." The poem suggests that contemporary therapeutic work occurs within this larger matrix of historical trauma, making every clinical encounter potentially a site of historical witnessing.
The Akeda Reinterpretation: Sarahs Prophetic Protest
The poem's treatment of Sarah's death—"As one of possible suicide in order to confront her Maker With the real question behind the Akeda, the binding of Isaac"—introduces a radical reinterpretation that transforms the traditional narrative of faithful acceptance into one of prophetic protest. Drawing on the Piacezna's wartime teachings, the poem suggests that Sarah "foresaw in her prophetic mind / Generation after generation of blood, and man's inhumanity to man."
This reinterpretation has profound implications for the essay's therapeutic framework:
Prophetic Vision as Clinical Insight: Sarah's ability to see future suffering parallels the clinical practitioner's recognition of patterns of trauma that exceed individual cases.
Protest as Sacred Act: Sarah's potential suicide becomes not despair but theological argument, suggesting that challenging divine justice can itself be a form of religious devotion—a principle crucial for therapeutic work with patients whose suffering challenges conventional meaning-making frameworks.
Maternal Perspective: The emphasis on Sarah's maternal vision introduces gender-specific dimensions of suffering that the essay's focus on Moses and Akiva does not fully develop.
Theological Innovation: Mesiras Nefesh as Imitatio Dei
The poem's most significant theological contribution lies in its formulation of mesiras nefesh (self-sacrifice) as "imitatio dei"— the imitation of God's creative act:
"By dying and giving Him our last breath We, too, act in creation in the very surrender to creation. We, too, breathe back into God what He had given so painfully By limiting Himself in this world."
This insight extends the essay's tzimtzum model in crucial ways: Therapeutic Implications: If human self-sacrifice mirrors divine self-limitation, then therapeutic encounters that require practitioners to "die a bit" to their ego-driven desires for cure or explanation become participations in cosmic creativity rather than professional failures.
Reciprocal Cosmology: The poem suggests that human response to suffering is not merely reactive but genuinely creative, contributing to ongoing divine self-revelation through history.
Death as Creative Act: The reframing of dying as creative participation rather than mere biological termination provides a framework for palliative care that honors dying as spiritually significant rather than medical defeat.
The Return to Silence: Theodicy as Creative Command
The poem concludes by returning to the Menachot passage: "When the angels then protest citing 'zu Torah vezu schora!' / Is this Torah and is this its reward' / God's response remains 'shtok! Kach ala bemachshava. / 'Be silent! For thus it arose in My mind'."
This return performs several crucial functions:
Circular Structure: The poem's return to its opening theme creates a circular structure that mirrors the cyclical breathing metaphor and suggests that theodicy questions are not solved but continually revisited.
Angels vs. Humans: The attribution of protest to angels rather than Moses (as in the Talmudic text) suggests that the question of suffering's meaning is not merely human but challenges even celestial understanding.
Divine Consistency: The repetition of "kach ala bemachshava" emphasizes that the response to suffering stems from the same primordial intention that governs creation, not from divine arbitrariness or indifference.
Poetic Technique and Theological Method
The poem's stream-of-consciousness style, with its parenthetical interruptions and fragmented syntax, mirrors the interpretive process that the essay identifies in Rabbi Akiva's method. Just as Akiva derives "heaps and heaps of halakhot" from seemingly insignificant textual elements, the poem finds theological significance in breathing patterns, historical memories, and bodily sensations.
Embodied Theology
The poem's consistent attention to bodily experience—breathing, gasping, drowning, surfacing—provides a counterpoint to the essay's more abstract theological analysis. This embodiment parallels the essay's emphasis on therapeutic approaches that honor patients' lived experience rather than reducing them to diagnostic categories.
Temporal Compression
The poem's movement between primordial creation, historical martyrdom, and personal spiritual experience performs a temporal compression that mirrors the therapeutic encounter's ability to make past trauma present and healing possible.
For Therapeutic Spaces
The poem's theological insights translate into several clinical implications that extend the essay's therapeutic framework:
Breathing as Therapeutic Metaphor: The poem's emphasis on breath offers a concrete technique for therapeutic presence— attention to breathing as a way of honoring both the cost of life and the necessity of surrender.
Historical Consciousness in Clinical Work: The poem's telescoping of historical trauma suggests that effective therapeutic work must acknowledge how individual suffering participates in larger patterns of historical trauma and resistance.
Death as Creative Process: The poem's reframing of dying as creative participation provides a framework for end-of-life care that honors dying as spiritually significant rather than medical failure.
For Spiritual Development
Prayer as Theological Argument: The poem's presentation of Sarah's protest as potentially sacred suggests that spiritual maturity involves the capacity to argue with divine justice rather than simply accepting it.
Embodied Spirituality: The poem's attention to breathing, drowning, and surfacing provides a model for spiritual practice that engages the body rather than transcending it.
Historical Consciousness: The poem suggests that authentic spiritual development requires engaging with the historical trauma that shapes contemporary experience rather than pursuing individual enlightenment in isolation
For Spiritual Development
Prayer as Theological Argument: The poem's presentation of Sarah's protest as potentially sacred suggests that spiritual maturity involves the capacity to argue with divine justice rather than simply accepting it.
Embodied Spirituality: The poem's attention to breathing, drowning, and surfacing provides a model for spiritual practice that engages the body rather than transcending it.
Historical Consciousness: The poem suggests that authentic spiritual development requires engaging with the historical trauma that shapes contemporary experience rather than pursuing individual enlightenment in isolation
Conclusion
"Before He Thought Silence" serves as more than poetic accompaniment to the essay's theological analysis; it performs the very hermeneutic work that the essay identifies as central to both Rabbi Akiva's interpretive method and contemporary therapeutic practice. The poem demonstrates how personal spiritual reflection can contribute to theological understanding, while theological insight can inform both clinical practice and spiritual development.
The poem's integration of cosmic creation, historical trauma, and personal spiritual experience provides a model for the kind of "sacred holding" that the essay identifies as crucial for therapeutic relationships that honor both scientific rigor and spiritual depth. In its attention to breathing as the fundamental rhythm that connects divine creativity with human mortality, the poem offers a concrete technique for developing the kind of "therapeutic presence" that can remain with patients in their suffering without either abandoning them to meaninglessness or reducing their experience to explanatory categories.
Most significantly, the poem's theological innovation—under- standing human self-sacrifice as participation in divine creativity rather than mere response to divine demand—provides a frame- work for clinical work that honors healthcare providers' own spir- itual development as integral to their professional effectiveness. The practitioner who learns to "breathe back into God" what has been received through therapeutic encounter participates in the ongoing divine creativity that the poem identifies as the ultimate meaning of both creation and healing response.
References
- Puchalski, C. M. (2001, October). The role of spirituality in health care. In Baylor University Medical Center Proceedings (Vol. 14, No. 4, pp. 352-357). Taylor & Francis.
- Balboni, M. J., & Balboni, T. A. (2018). Hostility to hospitality: spirituality and professional socialization within medicine. Oxford University Press.
- Best, M., Butow, P., & Olver, I. (2016). Doctors discussing religion and spirituality: A systematic literature review. Palliative medicine, 30(4), 327-337.
- Koenig, H. G., Hooten, E. G., Lindsay-Calkins, E., & Meador,K. G. (2010). Spirituality in medical school curricula: findings from a national survey. The International Journal of Psychiatry in Medicine, 40(4), 391-398.
- Ungar-Sargon, J. (2025). Divine presence and concealment in the therapeutic space. EC Neurology, 17(5), 01-13.
- Ungar-Sargon, J. (2025). Revelation in concealment:Theological reflections on the therapeutic encounterIII. American Journal of Medical and Clinical Research & Reviews, 4(4), 1-12.
- LaRocca-Pitts M. Theodicy and end-of-life care. Soc Work Health Care. 2014;53(8):749-65.
- Ungar-Sargon, J. (2025). Revisioning Healthcare Spaces: Lessons from Spiritual Community in Contemporary Medical Practice. American Journal of Medical and Clinical Research & Reviews, 4(6), 1-17.
- Julian, U. S. (2025). Beyond Theodicy: The Physician's Existential Crisis.
- Ungar-Sargon, J. (2025). The compromised healer: Moral ambiguity in the physician's role through literary and historical lenses. J Clin Rev Case Rep.
- Charon, R. (2001). Narrative medicine: a model for empathy,reflection, profession, and trust. jama, 286(15), 1897-1902.
- Kalitzkus, V., & Matthiessen, P. F. (2009). Narrative-based medicine: potential, pitfalls, and practice. The Permanente Journal, 13(1), 80.
- Ungar-Sargon J. Mariupol and Warsaw Ghetto: Theodicy then and now. Available from: https://www.jyungar.com/ theological-essays/2022/6/20/mariupol-and-warsaw-ghetto- theodicy-then-and-now
- Dean, W., Talbot, S., & Dean, A. (2019). Reframing clinician distress: moral injury not burnout. Federal Practitioner, 36(9), 400.
- Sherman, M., & Klinenberg, E. (2024). Beyond burnout: Moral suffering among healthcare workers in the first COVID-19 surge. Social Science & Medicine, 340, 116471.
- Ungar-Sargon J. The Tzimtzum model and doctor-patient relationships. Adv Med Clin Res. 2025;6(1):94-101.
- Greenhalgh, T. (1999). Narrative based medicine in an evidence based world. Bmj, 318(7179), 323-325.
- Egnew, T. R. (2018). A narrative approach to healing chronic illness. The Annals of Family Medicine, 16(2), 160-165.
- Ungar-Sargon, J. (2025). Divine presence and concealment in the therapeutic space. EC Neurology, 17(5), 01-13.
- Charon, R. (2001). Narrative medicine: a model for empathy,reflection, profession, and trust. jama, 286(15), 1897-1902.
- Zaharias, G. (2018). What is narrative-based medicine?: Narrative-based medicine 1. Canadian Family Physician, 64(3), 176-180.
- Rosti, G. (2017). Role of narrative-based medicine in proper patient assessment. Supportive Care in Cancer, 25, 3-6.
- Lederman, M. (2016). Social and gendered readings of illness narratives. Journal of Medical Humanities, 37, 275-288.
- Levinas, E. (1979). Totality and infinity: An essay onexteriority (Vol. 1). Springer Science & Business Media.
- Balboni, T. A., Paulk, M. E., Balboni, M. J., Phelps, A. C.,Loggers, E. T., Wright, A. A., ... & Prigerson, H. G. (2010). Provision of spiritual care to patients with advanced cancer: associations with medical care and quality of life near death. Journal of Clinical Oncology, 28(3), 445-452.
- Brady, M. J., Peterman, A. H., Fitchett, G., Mo, M., & Cella,D. (1999). A case for including spirituality in quality of life measurement in oncology. Psychoâ?Oncology: Journal of the Psychological, Social and Behavioral Dimensions of Cancer, 8(5), 417-428.
- Ungar-Sargon, J. A New Model for Healing Part II. Addict Res. 2024; 8 (2): 1-10. Correspondence: Julian Ungar- Sargon, Franciscan Hospital System, IN, 47978.
- Puchalski, C., Ferrell, B., Virani, R., Otis-Green, S., Baird, P., Bull, J., ... & Sulmasy, D. (2009). Improving the quality of spiritual care as a dimension of palliative care: the report of the Consensus Conference. Journal of palliative medicine, 12(10), 885-904.
- Koenig, H. G. (2012). Religion, spirituality, and health: The research and clinical implications. International Scholarly Research Notices, 2012(1), 278730.
- Mehl-Madrona, L., McFarlane, P., & Mainguy, B. (2021). Effects of a life story interview on the physician–patient relationship with chronic pain patients in a primary care setting. The Journal of Alternative and Complementary Medicine, 27(8), 688-696.
- Kaye, E. C., Rockwell, S. L., Lemmon, M. E., Baker, J. N., & Mack, J. W. (2022). The art of saying nothing. Pediatrics, 149(6).
- Ungar-Sargon, J. (2025). The Patient as Parable: Highlighting the Interpretive Framework: Applying Mystic.
- Lanphier, E. (2021). Narrative and medicine: Premises, practices, pragmatism. Perspectives in Biology and Medicine, 64(2), 211-234.
- Haidet, P., Kroll, T. L., & Sharf, B. F. (2006). The complexity of patient participation: lessons learned from patients’ illness narratives. Patient education and counseling, 62(3), 323-329.
- Egnew, T. R. (2018). A narrative approach to healing chronic illness. The Annals of Family Medicine, 16(2), 160-165.
- Scott, J. G., Cohen, D., DiCicco-Bloom, B., Miller, W. L., Stange, K. C., & Crabtree, B. F. (2008). Understanding healing relationships in primary care. The Annals of Family Medicine, 6(4), 315-322.
- Julian, U. S. (2025). Beyond Theodicy: The Physician's Existential Crisis.
- Chirico, F. (2016). Job stress models for predicting burnout syndrome: a review. Annali dell'Istituto superiore di sanita, 52(3), 443-456.
- Shanafelt, T. D., Hasan, O., Dyrbye, L. N., Sinsky, C., Satele, D., Sloan, J., & West, C. P. (2015, December). Changes in burnout and satisfaction with work-life balance in physicians and the general US working population between 2011 and 2014. In Mayo clinic proceedings (Vol. 90, No. 12, pp. 1600-1613). Elsevier.
- Descartes, R. (1996). Discourse on the method: And,meditations on first philosophy. Yale University Press.
- Prasad, K., McLoughlin, C., Stillman, M., Poplau, S., Goelz, E., Taylor, S., ... & Sinsky, C. A. (2021). Prevalence and correlates of stress and burnout among US healthcare workers during the COVID-19 pandemic: a national cross-sectional survey study. EClinicalMedicine, 35.
- Lennon, R. P., Parascando, J., Talbot, S. G., Zhou, S., Wasserman, E., Mantri, S., ... & Dean, W. (2023). Prevalence of moral injury, burnout, anxiety, and depression in healthcare workers 2 years in to the COVID-19 pandemic. The Journal of nervous and mental disease, 211(12), 981-984.
- Ungar-Sargon, J. (2025). Navigating the Depths: A Framework for Caregiver’s Grief Work. J Behav Health, 14(2), 1-9.
- Bryant-Genevier, J. (2021). Symptoms of depression, anxiety, post-traumatic stress disorder, and suicidal ideation among state, tribal, local, and territorial public health workers during the COVID-19 pandemic—United States, March–April 2021. MMWR. Morbidity and mortality weekly report, 70.
- Sexton, J. B., Adair, K. C., Leonard, M. W., Frankel, T. C., Proulx, J., Watson, S. R., ... & Frankel, A. S. (2018). Providing feedback following Leadership WalkRounds is associated with better patient safety culture, higher employee engagement and lower burnout. BMJ quality & safety, 27(4), 261-270.
- Ungar-Sargon, J. (2025). Prolonged Grief Disorder: Treatment Approaches and the Spiritual Dimensions of Healing. Addict Res, 9(1), 1-7.
- DasGupta S, Charon R. Personal illness narratives: using reflective writing to teach empathy. Acad Med. 2004;79(4):351-6.
- Wald, H. S., & Reis, S. P. (2010). Beyond the margins: reflective writing and development of reflective capacity in medical education. Journal of general internal medicine, 25, 746-749.
- Tedeschi, R. G., & Calhoun, L. G. (2004). " Posttraumatic growth: conceptual foundations and empirical evidence". Psychological inquiry, 15(1), 1-18.
- Prati, G., & Pietrantoni, L. (2009). Optimism, social support, and coping strategies as factors contributing to posttraumatic growth: A meta-analysis. Journal of loss and trauma, 14(5),364-388.
- Ungar-Sargon, J. (2025). Revisioning Healthcare Spaces: Lessons from Spiritual Community in Contemporary Medical Practice. American Journal of Medical and Clinical Research & Reviews, 4(6), 1-17.
- Frank, A. W. (2013). The wounded storyteller: Body, illness & ethics. University of Chicago Press.
- Kleinman, A. (2020). The illness narratives: Suffering,healing, and the human condition. Hachette UK.
- Silverman, J., Kurtz, S., & Draper, J. (2016). Skills for communicating with patients. crc press.
- Brown, J. B. (1998). Patient-centred medicine: transforming the clinical method. Patient Education and Counseling, 34, S44.
- Cassell, E. J. (1998). The nature of suffering and the goals ofmedicine. Loss, Grief & Care, 8(1-2), 129-142.
- Chochinov, H. M. (2007). Dignity and the essence of medicine: the A, B, C, and D of dignity conserving care. Bmj, 335(7612), 184-187.
- Hsu, C., Phillips, W. R., Sherman, K. J., Hawkes, R., & Cherkin, D. C. (2008). Healing in primary care: a vision shared by patients, physicians, nurses, and clinical staff. The Annals of Family Medicine, 6(4), 307-314.
- Post, S. G., Puchalski, C. M., & Larson, D. B. (2000). Physicians and patient spirituality: professional boundaries, competency, and ethics. Annals of internal medicine, 132(7), 578-583.
- Ungar-Sargon J. Capitalism and health care: A critique. Jpn J Med Sci. 2024;5(1):174-84.
- Arthur, H. M. (2006). Depression, isolation, social support, and cardiovascular disease in older adults. Journal of Cardiovascular Nursing, 21(5), S2-S7.
- Committee on Quality of Health Care in America. (2001). Crossing the quality chasm: a new health system for the 21st century. National Academies Press.
- Ungar-Sargon, J. (2024). The therapeutic vision: Non- conventional healing—a new paradigm. J Neurol Neurosci Res, 5, 54-59.
- Shanafelt, T. D., Boone, S., Tan, L., Dyrbye, L. N., Sotile, W., Satele, D., ... & Oreskovich, M. R. (2012). Burnout and satisfaction with work-life balance among US physicians relative to the general US population. Archives of internal medicine, 172(18), 1377-1385.
- Dyrbye, L. N., Thomas, M. R., & Shanafelt, T. D. (2006). Systematic review of depression, anxiety, and other indicators of psychological distress among US and Canadian medical students. Academic medicine, 81(4), 354-373.
- Ungar-Sargon, J. (2024). A New Model for Integrative Diagnosis and Management of PTSD in a Large Population. Addict Res, 8(1), 1-13.
- Arntfield, S. L., Slesar, K., Dickson, J., & Charon, R. (2013). Narrative medicine as a means of training medical students toward residency competencies. Patient education and counseling, 91(3), 280-286.
- Costa-Drolon, E., Verneuil, L., Manolios, E., Revah-Levy,, & Sibeoni, J. (2021). Medical students’ perspectives on empathy: a systematic review and metasynthesis. Academic medicine, 96(1), 142-154.
- Sulmasy, D. P. (2002). A biopsychosocial-spiritual model for the care of patients at the end of life. The gerontologist, 42(suppl_3), 24-33.
- Peterman, A. H., Fitchett, G., Brady, M. J., Hernandez, L., & Cella, D. (2002). Measuring spiritual well-being in people with cancer: the functional assessment of chronic illness therapy—Spiritual Well-being Scale (FACIT-Sp). Annals of behavioral medicine, 24(1), 49-58.
- Marmot, M., Friel, S., Bell, R., Houweling, T. A., & Taylor,S. (2008). Closing the gap in a generation: health equity through action on the social determinants of health. The lancet, 372(9650), 1661-1669.
- Wilkinson, R., & Pickett, K. (2011). The spirit level: Why greater equality makes societies stronger. Bloomsbury Publishing USA.
- Ungar-Sargon, J. (2025). Divine presence in healing: A Kabbalistic approach to compassionate care. J Behav Health, 14(2), 1-4.
- Ungar-Sargon, J. (2025). The Nature of the Animal Soul and Possibility of Transformation: An Integrated Approach to Addiction-Related Illness. American Journal of Medical and Clinical Research & Reviews, 4(4), 1-26.
- Gijsberts, M. J. H., Liefbroer, A. I., Otten, R., & Olsman, E. (2019). Spiritual care in palliative care: a systematic review of the recent European literature. Medical Sciences, 7(2), 25.
- Delgado-Guay, M. O., Hui, D., Parsons, H. A., Govan, K., De la Cruz, M., Thorney, S., & Bruera, E. (2011). Spirituality, religiosity, and spiritual pain in advanced cancer patients. Journal of pain and symptom management, 41(6), 986-994.
- Engel, G. L. (1977). The need for a new medical model: a challenge for biomedicine. Science, 196(4286), 129-136.
- Sulmasy, D. P. (2006). The rebirth of the clinic: An introduction to spirituality in health care. Georgetown University Press.
- Ungar-Sargon, J. (2025). The spiritual space between nurse and patient. Global Journal of Critical Care and Emergency Medicine.
- Ungar-Sargon, J. (2025). Questioning Divine Absence: Interpretations of Exodus 17: 7 through Contemporary Theological Discourse Implications for Therapeutic Language. Int J Psychiatr Res, 8(1), 1-7.
- Kleinman, A., Eisenberg, L., & Good, B. (1978). Culture, illness, and care: clinical lessons from anthropologic and cross-cultural research. Annals of internal medicine, 88(2),251-258.
- Good, B. J. (1994). Medicine, rationality and experience: an anthropological perspective (No. 1990). Cambridge University Press.
- Pellegrino, E. D., & Thomasma, D. C. (1993). The virtues in medical practice. Oxford University Press.
- Lutz, C. S. (2012). Reading Alasdair MacIntyre's after virtue. A&C Black.
- Holubová, M. (2006). Likutej amarim a chasidská spiritualita.
- Furstenberg, Y. (2012). The agon with moses and homer: Rabbinic Midrash and the second sophistic. In Homer and the Bible in the Eyes of Ancient Interpreters (pp. 299-328). Brill.
- Yadin-Israel, A. (2014). Bavli Menaḥot 29b and the Diminutionof the Prophets. Journal of Ancient Judaism, 5(1), 88-105.
- Handelman, S. A. (2012). The slayers of Moses: The emergence of rabbinic interpretation in modern literary theory. State University of New York Press.
- Handelman, S. A. (1991). Fragments of redemption: Jewish thought and literary theory in Benjamin, Scholem, and Levinas.
- Yadin-Israel, A. (2015). Scripture and Tradition: Rabbi Akiva and the Triumph of Midrash. University of Pennsylvania Press.
- Stern, D. (1996). Midrash and theory: Ancient Jewish exegesis and contemporary literary studies. Northwestern University Press.
- Rubenstein, J. L. (2010). Stories of the Babylonian Talmud. JHU Press.
- Zellentin, H. M. (2023). Rabbinic parodies of Jewish and Christian literature.
- Boyarin, D. (2004). Border lines: the partition of Judaeo- Christianity. University of Pennsylvania Press.
- Puchalski, C. M. (2012). Spirituality in the cancer trajectory. Annals of oncology, 23, iii49-iii55.
- Koenig, H. G., King, D., & Carson, V. B. (2012). Handbook of religion and health. Oup Usa.
- Scholem, G. (1995). Major trends in Jewish mysticism. Schocken.
- Wolfson, E. R. (2009). Open secret: Postmessianic messianism and the mystical revision of Menahem Mendel Schneerson. Columbia University Press.
- Magid, S. (2014). Hasidism incarnate: Hasidism, Christianity, and the construction of modern Judaism. Stanford University Press.
- Fishbane, E. P. (2018). The Art of Mystical Narrative: A Poetics of the Zohar. Oxford University Press.



