Research Article - (2026) Volume 11, Issue 2
Preconception Care Utilization and Associated Factors among Pregnant Mothers Attending Antenatal Care Follow-Up of Federal Police Hospital, Ethiopia 2023
2Menlik II Medical and Health Science College Department of Public Health, Ethiopia
Received Date: Nov 28, 2025 / Accepted Date: Apr 01, 2026 / Published Date: Apr 08, 2026
Copyright: ©2026 Chala Getaneh, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Gudeta, M., Woldeselassie, F., Getaneh, C. (2026). Preconception Care Utilization and Associated Factors among Pregnant Mothers Attending Antenatal Care Follow-Up of Federal Police Hospital, Ethiopia 2023. Int J Women
Abstract
Background: Preconception care is taking care to women and couples before conception occurs. It has a positive impact on reduction in maternal mortality and decreases the risk of adverse pregnancy outcome and aimed at improving women’s health status, reducing behaviors, individual environmental factors. The existing interventions strategies are too late to prevent Adverse Pregnancy Outcome. Those services are given after the conception happened and the women aware that she is pregnant.
Objective: Study was aimed to assess preconception care Utilization and associated factors among pregnant women attending Antenatal care at Ethiopian Federal Police Hospital from August20-september15/2023.
Methods: A cross-sectional study design was used among 398 pregnant women systematically selected at Ethiopian Federal Police Hospital. Data entry was done into Epi-data version 3.1and exported to SPSS version 25.0 for analysis using p–value <0.05 at 95% CI was statistically significant. Bivariable analysis was performed using binary logistic regression; at (P< 0.25) was a criterion to select candidate variables for multivariable analysis. Multivariable logistic regression analysis was performed to adjust for possible confounding variables at P-value <0.05, at 95% CI was used in judging the Statistical significance of the association.
Result: This study found that 19.1% of the study participants had utilized preconception care. Factors found to be show association with women’s preconception care utilization were partner support (AOR=2.004,at 95% CI 1.104-3.638) previous history of obstetric problem(AOR=2.290 at 95% CI, 1.219-4.303),diagnosed for Anemia(AOR=0.187, at 95% CI, 0.046-0.770), knowledge on preconception care utilization (AOR=2.753,at 95% CI, 1.522-4.98),Women who were advised on preconception care utilization(AOR=6.123, at 95% CI, 2.709-13.843) and unwillingness of health care providers to give services (AOR=0.436,at 95% CI, 0.218-0.871) were factors significantly associated with preconception care utilization.
Conclusion: preconception care utilization was low and partner support, previous history of obstetric problem, knowledge, getting an advice, unwillingness of service provider and being diagnosed for anemia were significantly associated with preconception care utilization.
Recommendation: Integrating preconception care utilization with other maternal health services, improving women’s/ partiers’ knowledge and strengthening pre-pregnancy counseling services is crucial.
Keywords
Preconception Care Utilization, Pregnant Women, Federal Police Hospital
Abbreviations
ANC: Antenatal Care
APO: Adverse Pregnancy Outcome
BMI: Body Mass Index
CVD: Cardiovascular Disease
EDHS: Ethiopian Demographic Health Survey
GDM: Gestational Diabetic Mellitus
HIV: Human Immune Virus
IMR: Infant Mortality Rate
LTR: Life Time Risk
MNCH: Maternal, Newborn and Child Health
NMR: Neonatal Mortality Rate
NTD: Neural Tube Defect
PCC: Preconception Care
PNC: Postnatal Care
PRAMS: Pregnancy Risk Assessment Monitoring System
RH: Reproductive Health
SDG: Sustainable Development Goal
UN: United Nation
WHO: World Health Organization
Introduction
Background
Pre-conception care is the provision of the biomedical, behavioral and social health interventions to women and couples before conception occurs [1]. Preconception care (PCC) is particularly important as fetal development commences in thefirst trimester of pregnancy, before many women are aware of their pregnancy [2]. This care recognizes that many adolescent girls and young women will be thrust into motherhood without the knowledge, skills or support they need; and that by promoting health and providing preventive care, for better outcomes for them and their children [3]. Evidence strongly suggests that earlier care before pregnancy leads to improved women's health and improved pregnancy outcome for both the mother and the newborn [4]. The WHO passed its recommendations so that PCC can be implemented in all countries of the world including the middle and low-income countries, along with the other health service packages PCC can reduce death among mothers and children, prevent unplanned and unwanted pregnancies, prevent delivery complications, prevent stillbirth, prevent Low birth weight and preterm labor, prevent congenital anomalies and neonatal infections, prevent stunting, and prevent mother to child transmission of HIV/STIs [5].
Every year, in the past 25 years, about half a million women die due to maternal causes and the sum of the consecutive maternal death reported from the year 1990-2015 results in 10.9 million estimated maternal deaths [6]. The risk of maternal and infant mortality and pregnancy-related complications can be reduced by increasing access to quality preconception (before pregnancy) and inter-conception (between pregnancies) care [7]. About 830 women die from pregnancy and childbirth related complications around the world every day and in 2015 around 303, 000 women died from pregnancy and childbirth related problem [6]. Most of these complications develops during pregnancy, exist before and worsened during pregnancy especially if not managed as part of the preconception care [8]. The lately identified but effective evidence-based intervention among the continuum of the spectrum of the maternal and child health services is preconception care which targeting the critical periods of the infant’s organ formation [9]. Since a majority of women are unaware of the effects of their own health conditions and health-related behaviors may have effects on the fetus, they entering in a pregnancy with various preconception risk factors to APO [10]. Different articles show that the women’s preconception care knowledge and practice in developing countries including Africa is low [11-13]. In Ethiopia there are no formal preconception clinics established in health care settings. Yet, preconception care is introduced during maternal and child health services like, consultations for contraception, follow¬up for chronic diseases, follow up for immunizations services and during post-natal care services.
Methodology
Study Area and Period
The Ethiopian Federal police hospital is found in Addis Ababa Lideta sub-city. It provides health care services for all Police members and their families in the country as a referral Hospital. A study will be conducted from August 20-september15/2023 among 398 pregnant women who are attending antenatal care at Ethiopian Federal Police Hospital. According to the hospital report 2021 more than 93,000 Outpatient attendant services, more than 10,000 maternal health care services (1588 was delivery service). The expected monthly all ANC visit (new +repeat) was 843. According to report, in the last fiscal year the percentage of at least one ANC visit was 100% and at least ANC four visits were 95%. The pregnant women tested for syphilis and HIV/AIDS were 100%, CAR was 85% and proportion of infant who received all vaccines was 91%, proportion of infant whose mothers had protective doses of TT against NNT was 83% and number of still birth in last fiscal year was eight.
Study Design
A Hospital based cross sectional study design was carried out to conduct the study.
Population
• Source Population: The source populations were all pregnant women who are attending ANC at Federal Police Hospital, Ethiopia 2023.
• Study Unit: All list of pregnant mothers attending ANC during study period at Federal Police Hospital, Ethiopia 2023.
• Sample Population: All randomly selected pregnant mothers who are attending ANC during study period.
• Inclusion Criteria: All pregnant women who are attending ANC during study federal police hospital, Ethiopia 2023.
• Exclusion Criteria: Pregnant mothers who come for revisit during data collection period were excluded and the study was excluded women who severely ill at the time of data collection period since they could not able to give oral consent and relevant data.
• Samplesize Determination: The designed Sample size was calculated by single population proportion formula. The sample size calculated with following assumption: 95% confidence interval and anticipated prevalence of women’s experience on preconception care is 38.2% based on study done in west shewa oromia region, 5% margin of error [14].
Accordingly, the required sample size will be calculated as the following
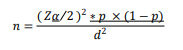
Where; n = Sample size Z = the standard normal deviation at 95% confidence interval; =1.96, P = anticipated proportion of preconception care experience among ANC attendants 38.2 % (0.382) d = margin of error that can be tolerated, 5% (0.05) Then the sample size could be calculated as:
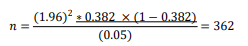
So, the required sample size was, 362; when P= 38.2 % (0.382); and adjusted non-respondent’s rate of 10%, the final sample size was: 362*10%=36 and then, 362+36= 398.Therefore 398 pregnant mothers on antenatal care visit were participants of the study. The sample size for the second objective was calculated by using Epi info version7 software by taking 80% power and 95% confidence interval. Therefore, the calculated sample size for the second objective was lower than the first objective sample; then the final sample size for the study will be the first objective sample which will be 398.
|
Second objectives |
Factor |
% of outcome in exposed |
% of outcome in non-exposed |
Power |
CI |
OR |
Total sample size |
Reference |
|
1. history FP |
63.3 |
85.3 |
80% |
95% |
0.296 |
143 |
[15] |
|
|
History of pregnancy induced HTN |
2.2 |
77.9 |
80% |
95% |
0.0063 |
83 |
[16] |
|
|
|
Knowledge |
5.5 |
94.5 |
80% |
95% |
2.5 |
34 |
[17] |
Table 1: Second Objective Sample Size Calculation
Sampling Technique and Procedure
Federal police hospital is purposely selected. A samplesize of 398 were selected based on the expected number of monthly ANC attedant of pregnant women at Federal police hospitaleach (based on the last month ANC attendant report). Each pregnant mother was selected by systematic random sampling technique. The total monthly expected number of ANC attendants’Federal police hospitalis 630). The sampling interval was determined to select study participant. The monthly expected number of ANC attendant Federal police hospital was 843 and, the sampling interval value 2 will be used.
Figure 1: Schematic Presentation of Sampling Technique on Preconception Care Utilization Among ANC Attendants at Federal Police Hospital, 2023
Data Collection Tool
The tool was adopted from previous literature in different parts of the world and will be modified according to local context based on objectives of the study [14,15,17-19]. Interviewer administered questionnaire was used to collect quantitative data from the respondents. The questionnaire first prepared in English language then translated to local languages Amharic before data collection. The questionnaires were primarily containing socio-demographic data, knowledge statement on PCC, overall PCC utilization, obstetric factors data and history of chronic disease in each subsection.
Data Collection Method
The study was utilized an interviewer administered structured questionnaire Three data collectors (3 BSC degree in midwifery), and one public health officer as supervisor were involved on data collection and trained on how to access records and how to approach each item in the instrument, wisely using of time, data handling and submission of the collected data. The questionnaire was prepared in English language, translated in to a common spoken Language, Amharic and then transcribed back to English properly by expert to check its consistency.
Study Variables
• Dependent Variables: Preconception care utilization
• Independent Variables
![]() Socio-demographic factors which includes Age, Educational status and husband’s educational status Occupation and Marital status
Socio-demographic factors which includes Age, Educational status and husband’s educational status Occupation and Marital status
![]() Obstetric factors which includes gravidity, parity, family planning use and bad obstetric history
Obstetric factors which includes gravidity, parity, family planning use and bad obstetric history
![]() Knowledge on preconception care which includes knowledge on benefits of PCC, knowledge on PCC components.
Knowledge on preconception care which includes knowledge on benefits of PCC, knowledge on PCC components.
![]() History of maternal chronic disease which includes diabetic mellitus hypertension, asthma, Epilepsy, syphilis, anemia and HIV/AIDS.
History of maternal chronic disease which includes diabetic mellitus hypertension, asthma, Epilepsy, syphilis, anemia and HIV/AIDS.
Operational Definition
• Preconception Care Utilization: If women received at least one types of interventions either advice or treatment and life style modification, care women received regarding components of preconception care (screened for any disease and get treatment, take folic acid, take vaccine, get counseling, cessation of alcohol and cigarette smoking, planned pregnancy) before being pregnant [20].
• Knowledge on PCC: Women’s level of knowledge on PCC was measured based on correct response using seven PCC knowledge-based questions. Each correct and incorrect response was scored one and zero point respectively.
• Having Knowledge: Respondent scored greater than or equal to the mean was considered as “have knowledge” and respondents scored less than the mean was considered as “not have knowledge on preconception care utilization” [15].
• Preconception care components: In this study preconception care components are HIV testing and counseling, STI screening and treatment, chronic medical condition screening and treatment nutrition and weight monitoring counseling and ferrous supplementation, immunization (TT), Advice on cessation of alcohol and advice on cessation of cigarette smoking, family planning [18,20].
Data Quality Control
The Questionnaire was pre-tested on 5% of study participants in Zewditu memorial hospital two weeks before the actual data collection period to check the consistency of instruments, adequacy of variable and orders of the question. After pretest, amendment was made accordingly. The interview guide questionnaire was prepared in English and translated in to Amharic by an expert for ease of interview study participants were informed, voluntary and they could withdraw at any time with no consequence. Training will be given for data collectors and for supervisor by principal investigator on how to fill the Questionnaire and method of approaching study participants. The filled questionnaires will be Checked for completeness by the supervisors at the site of data collection and finally by Principal investigator. The data will be coded, cleaned before entered into Epi-data.
Data Processing and Analysis Method
The data will be coded and entered into Epi-data version 4.2.0 and exported to SPSS version 20.0 for analysis. Descriptive statistics like mean, frequency and proportion will be used and findings will be presented in texts, tables and charts. Based on the 10 knowledge items and 11 PCC utilization data will be computed an overall knowledge and utilization score for each study participant. Logistic regression including vicariate and multivariate analysis will be used to examine association between dependent and independent variables. Statistical significance considered at p-value less than 0.05. AOR at 95% CI used to show the strength and significance of that association.
Results
Socio-Demographic Characteristics of the Study Participants
A total of 398 pregnant women attending ANC were involved in the study with the response rate of 100%. The mean age of the study participants was 27.87(±SD 5.26). As Table1 shows the majority of the study participants were married 378(95 %), 8(2. %) were divorced, 6(1.5%) were single and 3(0.8%) were widowed concerning to marital status. Most of the respondents were college and above 174(43.4%), 154(38.7%) completed secondary school, 42(10.6%) of them were completed primary school and 27(6.8%) were not have formal education. Concerning husband’s educational status 300(75.4%) of them were graduated from a college and above, 68(17.1) of them completed secondary school and only 11(2.8%) of them had no formal education. The majority of the study participants were orthodox religion followers 185 (46.5%) followed by protestant religion followers 122 (30.1%) and Muslim religion followers 71(17.8%), followers. Among the total study participants 215(54.0%) were government employers, 94(23.6%) were house wives, about 54(13.6%) private business owners in their occupation (Table 2).
|
Variables |
|
Frequency |
Percent (%) |
|
Women’s Age (years) |
15-24 |
119 |
29.9 |
|
25-34 |
229 |
57.5 |
|
|
35 and older |
47 |
11.8 |
|
|
Marital status |
Married |
378 |
95.0 |
|
Single |
6 |
1.5 |
|
|
Divorced |
8 |
2.0 |
|
|
Widow |
3 |
0.8 |
|
|
Other |
2 |
0.5 |
|
|
Women’s educational Status |
No formal education |
27 |
6.8 |
|
Primary school |
42 |
10.6 |
|
|
Secondary school |
154 |
38.7 |
|
|
College and above |
174 |
43.7 |
|
|
Husband Educational Status |
No formal education |
11 |
2.8 |
|
Primary school |
18 |
4.5 |
|
|
Secondary school |
68 |
17.1 |
|
College and above |
300 |
75.4 |
|
|
Women’s Occupation |
House wife |
94 |
23.6 |
|
Private business |
54 |
13.6 |
|
|
Government employee |
215 |
54.0 |
|
|
Others |
34 |
8.5 |
|
|
Family size |
Less than 4 |
308 |
77.4 |
|
4 and above |
89 |
22.4 |
|
|
Religion |
Orthodox |
185 |
46.5 |
|
Muslim |
71 |
17.8 |
|
|
Protestant |
122 |
30.7 |
|
|
Others |
20 |
5.0 |
Table 2: Socio Demographic Characteristics of Pregnant Women in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Knowledge of Pregnant Women on Preconception Care Utilization
The study found that only 167(42%) of pregnant women had knowledge on PCC utilization while remaining 231(58%) pregnant women had no knowledge on PCC utilization (Figure 2).
Figure 2: Pregnant Women’s Knowledge Level on Preconception Care Utilization in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Almost more than half of the study participants 208(52.3%) had an information about preconception care utilization and agreed that using family planning before pregnancy is very important, about 124(31%) of the study participants knew the importance of TT vaccination before conception. One hundred seventy-seven (44.5%) agreed about chronic medical condition screening is important before pregnancy. One hundred sixty (40.2%) of the pregnant women knew the effects of alcohol and cigarettes smoking on pregnancy before conception. One hundred fourteen (28.5%) of the study participants knew weight monitoring is important before conception. Only 72(18.1%) of the women agreed that taking folic acid to avoid neutral tube defects is important before pregnancy. A 128(32.2%) of the respondents knew about STI and HIV/AIDS screening is important before conception F (Table 3).
|
Knowledge Variables |
Response |
Frequency |
Percent (%) |
|
Ever heard about PCC utilization |
Yes |
208 |
52.3 |
|
No |
190 |
47.7 |
|
Using FP before pregnancy is important |
Yes |
208 |
52.3 |
|
No |
190 |
47.7 |
|
|
Vaccinated of TT before pregnancy is important |
Yes |
124 |
31.2 |
|
No |
274 |
68.8 |
|
|
Screened for chronic medical illness when planned to pregnancy is important |
Yes |
177 |
44.5 |
|
No |
221 |
55.5 |
|
|
Avoiding taking alcohol and cigarette when planned to pregnancy is important |
Yes |
160 |
40.2 |
|
No |
238 |
59.8 |
|
|
Keeping body weight when intended to pregnant is important |
Yes |
114 |
28.6 |
|
No |
284 |
71.4 |
|
|
Taking folic acid to avoid neutral tube defects is important |
Yes |
72 |
18.1 |
|
No |
326 |
81.9 |
|
|
Testing for STI/HIV when intended to pregnant is important |
Yes |
128 |
32.2 |
|
No |
270 |
67.8 |
Table 3: Pregnant Women’s Knowledge Level on Preconception Care Utilization in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Source of Information on Preconception Care Utilization
More than half of the study participants 216(54.3%) heard about preconception care utilization. The study participants were asked to indicate the source of information on preconception care utilization and only 181(45.47%) indicated source of information. One hundred thirty-three (33.4%) of the women reported they were heard from health care facilities which was the most reported source of information. Thirty-two (8%) of study participants were heard from mass media about preconception care utilization, twenty-nine (7.3%) heard from community and Only 19(4.8%) of them heard from religious institution which is the least source of information (Table 4).
|
Source of information |
Response |
Frequency |
Percent (%) |
|
Community |
Yes |
29 |
7.3 |
|
No |
190 |
47.7 |
|
|
Religious organization |
Yes |
19 |
4.8 |
|
No |
190 |
47.7 |
|
|
Health Care facilities |
Yes |
133 |
33.4 |
|
No |
274 |
68.8 |
|
|
Mass media |
Yes |
32 |
8.0 |
|
No |
221 |
55.5 |
|
|
Others |
Yes |
4 |
1.0 |
Table 4: Pregnant Women’s Source of Information on Preconception Care Utilization in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Obstetric Characteristics of Study Participants
More than half (66.8%), (66.3%) of the pregnant women were multigravida and nullipara respectively. One third (31.7%) and 33.2% of the women were multipara and primigravida respectively. Majority of the respondents 318 (79.9%) of the current pregnancy were planned pregnancy the rest 20.1% were unplanned. Majority, 299 (75.1%) of respondents had no previous obstetric problem outcome and the rest 99(24 %) of respondents had reported previous obstetric problem in which the most reported adverse obstetric outcome was abortion 46(11.6%) and congenital malformation 37(9.3%) respectively. Among the study participants who were married more than half 53.5% of respondents had support from their husbands for preconception care utilization. One hundred thirty-eight 34.7% of women reported unavailability of preconception care utilization unit in health facility is a problem. Majority 96.5% of the respondents reported that no traditional and cultural obstacles to utilize preconception care (Table 5).
|
Obstetric Characteristics |
|
Frequency |
Percent (%) |
|
Parity |
Nulipara |
272 |
68.3 |
|
Multipara |
126 |
31.7 |
|
|
Gravidity |
Primigravida |
132 |
33.2 |
|
Multigravida |
266 |
66.8 |
|
|
Obstetric Problem |
Yes |
99 |
24.9 |
|
No |
299 |
75.1 |
|
|
Previous Obstetric Problem |
Abortion |
46 |
11.6 |
|
Congenital malformation |
37 |
9.3 |
|
|
Still birth |
10 |
2.5 |
|
|
Neonatal death |
6 |
1.5 |
|
|
Planned Pregnancy |
Yes |
318 |
79.9 |
|
No |
80 |
20.1 |
|
|
Partners support for PCC |
Yes |
213 |
53.5 |
|
No |
185 |
46.5 |
|
|
Unavailability of PCC Utilization Unit |
Yes |
138 |
34.7 |
|
No |
260 |
65.3 |
|
|
Traditional and Cultural Obstacles |
Yes |
14 |
3.5 |
|
No |
384 |
96.5 |
Table 5: Pregnant Women’s Obstetric Characteristics in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Pregnant Women Preconception Care Utilization
Seventy-six (19.1%) of pregnant women utilized preconception care. As Table 6 shows the most utilized component of preconception care was family planning 18(4.5%) while the least utilized component of preconception care was folic acid utilization 4 (1%). Among the study participants 9(2.26%) utilized TT vaccination before pregnancy, 12(3%) screened for chronic medical condition, 7(1.76%) got advice on the effects of alcohol drinking and cigarette smoking on their health and pregnancy outcome. Only 8(2%) women were monitored their weight before pregnancy and 11(2.76%) of them were utilized HIV/AIDS screening before conception (Table 6).
|
Variables |
Response |
Frequency |
Percent (%) |
|
Utilized FP |
Yes |
18 |
4.5 |
|
No |
380 |
95.5 |
|
|
Immunized Against Tetanus |
Yes |
9 |
2.26 |
|
No |
389 |
97.74 |
|
|
Screened for any Medical Condition During Preconception |
Yes |
12 |
3.0 |
|
No |
386 |
97 |
|
|
Advised on the Effects of Alcohol and Cigarette Smoking |
Yes |
7 |
1.76 |
|
No |
391 |
98.24 |
|
|
Weight monitored before conception |
Yes |
8 |
2.01 |
|
No |
390 |
97.99 |
|
|
Screened for HIV/AIDS before Current Pregnancy |
Yes |
11 |
2.76 |
|
No |
387 |
97.23 |
|
|
Screened for Another STIs |
Yes |
7 |
1.76 |
|
No |
391 |
98.24 |
|
|
Consumed Folic Acid Supplementation Three Months before Conception |
Yes |
4 |
1.00 |
Table 6: Preconception Care Utilization Service Characteristics in Ethiopia Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Maternal Chronic Disease
Pregnant women were asked for chronic medical condition they were diagnosed before current pregnancy. Thirty-one (7.8%) of the women were diagnosed for Anemia, 27(6.8%) of them diagnosed for Hypertension, fourteen (3.5%) of the women were diagnosed for Diabetes mellitus and only three (0.8%0 of the pregnant women were reported that they were diagnosed for HIV/AIDS before current pregnancy (Table 7).
|
Maternal Chronic Disease |
Response |
Frequency |
Percent (%) |
|
Hypertension |
Yes |
27 |
6.8 |
|
No |
371 |
93.2 |
|
|
Diabetes mellitus |
Yes |
14 |
3.5 |
|
No |
384 |
96.5 |
|
|
HIV/AIDS |
Yes |
3 |
0.8 |
|
No |
395 |
99.2 |
|
|
Epilepsy |
Yes |
5 |
1.3 |
|
No |
393 |
98.7 |
|
|
Asthma |
Yes |
8 |
2.0 |
|
No |
390 |
98.0 |
|
|
Anemia |
Yes |
31 |
7.8 |
|
No |
367 |
92.2 |
|
|
Syphilis |
Yes |
3 |
0.8 |
Table 7: Maternal Chronic Disease Characteristics among Pregnant Women in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Health Care Provider Factors
Majority, 269 (67.6%) of the participants reported that health care provider’s sex was female and 120 (30.2%) of the health care providers were unwilling to provide counseling and services related to preconception care utilization, whereas only 146(36.7%) of the participants reported that the health care providers were knowledgeable on preconception care utilization. Eighty-four (21.1%) of the study participants confirmed that they were disrespected during services and only 81(20.4%) study participants were counseled on preconception care utilization services at study area and only 116(29.1%) of them were reported that health care providers listened them carefully and answered the question they raised (Table 8).
|
Maternal chronic disease |
Response |
Frequency |
Percent (%) |
|
Counseled on Preconception utilization |
Yes |
81 |
20.4 |
|
No |
317 |
79.6 |
|
|
Disrespected during services |
Yes |
84 |
21.1 |
|
No |
314 |
78.9 |
|
|
Service provider knowledgeable |
Yes |
146 |
36.7 |
|
No |
252 |
63.3 |
|
|
Unwillingness |
Yes |
120 |
30.2 |
|
No |
278 |
69.8 |
|
|
Health care provider listen carefully |
Yes |
116 |
29.1 |
|
No |
282 |
70.9 |
|
|
Sex of the service provider |
Male |
129 |
32.4 |
Table 8: Health Care Provider’s Factors on Preconception Care Utilization among Pregnant Women in Ethiopian Federal Hospital, Addis Ababa, Ethiopia, 2023(n=398)
Associated Factors with Preconception Care Utilization
In binary logistic regression twenty-nine variables were entered in to analysis with dependent variable to determine the significance of each variable. The significance level of each variable was checked (p<0.25) and ten variables were significantly associated in binary logistic regression with dependent variable. Bivariate logistic regression analysis was used to identify set of predictor variables for preconception care utilization among different variables. The significant variables were Women’s knowledge on preconception care utilization, occupational status, previous history of obstetric problem, being diagnosed for anemia, being diagnosed for Asthma, having information about preconception care utilization, getting advice on the service, unavailability of preconception care utilization unit in hospital, partner support on preconception care utilization, unwillingness of service provider on preconception care were identified as variables associated with preconception care utilization. After controlling for the effect of potential confounding variables using multivariable logistic regression, partner support on preconception care services, previous history of obstetric problem, Women’s knowledge, getting an advice on the service, unwillingness of service provider on preconception care utilization and being diagnosed for anemia were remained significantly associated with preconception care utilization services with 95% CI (p. value<0.05).
Variables significantly associated in binary logistic regression but insignificant in multivariable logistic regression were being diagnosed for Asthma and hypertension, Women’s occupation and unavailability of preconception care unit in health facilities with 95% CI(p<0.25) were significant in binary analysis but insignificantly associated in multivariable analysis with preconception care utilization. As well as ever heard about preconception care, educational status of the respondent and husbands were also significant in binary analysis and not significant in multivariable logistic regression analysis. The study showed that six factors found to be significantly associated with women’s preconception care utilization.
Pregnant women who had a partner support on preconception care service with 95% CI (AOR=1.104-3.638) (p=0.022) were 2.004 times more likely to utilize preconception care services than their counter parts. This implies partner involvement in PCC service could improve women’s service utilization. Women who have previous history of obstetric problem with 95% CI, (AOR=1.219-4.303) (P=0.010) were 2.290 times more likely to utilized preconception care services than their counter parts. Pregnant women, who were diagnosed for Anemia with 95% CI, (AOR=0.046-0.770) (P= 0.020) were 81.3% less likely to utilize preconception care services than women who were not diagnosed for Anemia. Pregnant women who had a good knowledge on preconception care utilization with 95% CI, (AOR=1.522-4.98) (P=0.001) were 2.753 times more likely to utilize preconception care services than their counter parts. Women who were advised on preconception care utilization with 95% CI, (AOR=2.709-13.843) (P=0.000) were 6.123 times more likely to utilize preconception care services than their counter parts and women who reported that the unwillingness of health care providers to give services with 95% CI, (AOR=0.218-0.871) (P=0.019) were 56.4% times less likely to utilize preconception care services than their counter parts (Table 9).
|
Variables |
|
PCC utilization |
COR (95%) CI Sig. |
AOR (95%) CI Sig. |
|
|
|
|
Yes |
No |
|
|
|
Partner support |
Yes |
24 |
161 |
1.499(0.804,2.796) 0.203* |
2.004 (1.104-3.638) 0.022** |
|
|
No |
52 |
161 |
1 |
|
|
Obstetric problem |
Yes |
26 |
73 |
2.441(1.267,4.703), 0.008* |
2.290(1.219-4.303) 0.010** |
|
Diagnosed for Anemia |
Yes |
3 |
28 |
0.346(0.90-1.314) 0.119* |
0.187 (.046-.770) 0.020 |
|
|
No |
294 |
73 |
1 |
|
|
Diagnosed for Asthma |
Yes |
3 |
5 |
0.004* |
1.208(0.422-3.456) 0.725 |
|
|
No |
317 |
73 |
1 |
|
|
Knowledge on PCC |
Good |
50 |
117 |
3.323(1.796-6.676) 0.000* |
2.753(1.522-4.981) 0.001** |
|
|
Poor |
26 |
205 |
1 |
|
|
Advised on utilization |
Yes |
22 |
59 |
1.236(0.0477-1.387) 0.093 |
6.123 (2.709-13.843) 0.000** |
|
|
No |
54 |
263 |
1 |
|
|
Diagnosed for HTN |
Yes |
3 |
24 |
0.398(0.085-1.866) 0.243* |
0.399 (0.096-1.652) 0.205 |
|
|
No |
73 |
298 |
1 |
|
|
Unavailability of unit |
Yes |
113 |
209 |
0.246(0.0 51-1.183) 0.080* |
0.310(0.065-1.472) 0.141 |
|
|
No |
25 |
51 |
1 |
|
|
Unwillingness of HCP |
Yes |
17 |
103 |
1.851(0.306-1.851) 0.000* |
0.436(0.218-.871) 0.019** |
|
|
No |
59 |
219 |
1 |
|
|
Occupation of Women |
Gov’t employed |
53 |
188 |
0.716(0.352-2.462) 0.000* |
2.952(0.782-11.141) 0.110 |
|
|
Unemployed |
12 |
145 |
|
|
|
*significant at p-value<0.25, ** significant at p-value <0.05, COR crude odd ratio, Adjusted odd ratio, p-value for COR p-value for AOR., 1- logical reference. |
|||||
Table 9: Binary and Multivariable Logistic Regression Analysis on Preconception Care Utilization among ANC Attendant in Ethiopian Federal Police Hospital, Addis Ababa, Ethiopia (n=398)
Discussion
Understanding of Preconception care utilization is essential for many developing countries especially Sub-Saharan African countries, such as Ethiopia, where adverse pregnancy outcome remains alarmingly high [17]. This hospital based cross-sectional study was carried out to assess the utilization of preconception care and its associated factors among pregnant women in Ethiopian Federal Police Hospital. This study found that 19.1% of the study participants had utilized preconception care. Partner support on preconception care utilization, previous history of obstetric problem, Women’s knowledge on preconception care utilization, getting an advice on the service, unwillingness of service provider on preconception care utilization and being diagnosed for anemia were found to be independent factors affecting the utilization of PCC utilization among pregnant women in Ethiopian Federal Police Hospital Ethiopia. The preconception care utilization prevalence 19.1% obtained by this study is similar with different studies done in Kenya, SNN Hossana and Hawassa [19,21,22]. This similarity might be due to the study setting, design and socioeconomic similarity among participants.
This finding is higher than the report from the study done in Sudan Abakalik, Southern Nigeria, Debre Berhan and is higher than study conducted in Debre Marikos town and mekele town in Ethiopia where only 8.4% of pregnant women were utilized Preconception care services [13,17,18,23,24]. This variability may be related to difference in study population, level of education, culture and study setting. However, this study is far lower than the conducted in Iran (68.8%), France (85%) Jordan (85%) and in USA (76%) and study in west shoa which showed that 38.2% of the women who attended ANC were experienced preconception care [13,25,26]. This might be due to difference in study setting since the previous study was facility based and difference in study population and the other study conducted in sendafa town health facilities which showed 58.2% [14,27]. This discrepancy might be due to the difference in access to information and low relative media coverage, socio economic status and quality of health care system. This study also identifies factors associated with preconception care utilization. The current study indicated that women who had previous obstetric problem were two times more likely utilized preconception care than those who had no previous obstetric problem ever. This finding was similar with previous study conducted in mizan Aman Mekelle, London, and Iran [17,25,28,29].
This showed that women who had previous obstetric problem were more likely to utilized preconception care. This might be due to increased self-responsibility and those women were more conscious on their next pregnancy. In addition, this study indicated that women who had good knowledge on preconception care utilization were almost three times more likely to utilized preconception care than women who had poor knowledge on preconception care. This finding was similar with previous study conducted in Mekelle, Debre Birhan, Nepal and Nigeria which showed that knowledgeable women were more likely utilized preconception care [17,18,30,31]. This might be due to increase health seeking behavior of the women and highly motivated to get services. In addition, this might be due to increase positive behavior towards the action. This implies that improving the women’s knowledge could improve the utilization of preconception care. This clearly showed that a lot need to be done to improve knowledge of the women towards preconception care in the study area and in the country for the improvement of preconception care utilization. This study revealed that women who had a partner support on Preconception care utilization were two times more likely to utilized PCC than their counter parts. Study from Egypt and Ethiopia, Mekele town, Debre Berhan town also in line with this study and this may be due to having reproductive health policies including male involvement strategies promoting maternal and child health care services. In addition, women who have partner support can discuss more about the importance and benefit of PCC services [11,17,18]. The study also found that being diagnosed for Anemia was negatively associated with women’s preconception care utilization. In this study Women who were being diagnosed for Anemia were 81.3% less likely to utilized PCC than their counter parts. But the study from Jordan and china are contrast with this study showing that no association between being diagnosed for anemia and PCC utilization [32,33]. This might be the difference between socio-demographic differences between study participants.
The other factor which showed statistically significant association with preconception care utilization was advice received on preconception care previously. Women who were advised on preconception care utilization were 6.123 times more likely to utilized preconception care than their counter parts. This could explain as follows; women who received advice regarding preconception care are more likely to get preconception care and tend to undergo lifestyle modifications related with preconception care. Those women who advised to control preexisting medical conditions or take folic acid supplementation or undergo weight management or diet modification are more likely to undertake these interventions than other women who didn’t get this advice. This finding is supported by study carried out at teaching hospital in Southeast Nigeria which revealed that there was statistically significant correlation between utilization of preconception care and information from doctors. This implies that strengthening counseling services provided for women can increase women utilization of preconception services and help them to start their pregnancy at best possible health. The other associated factor revealed in this study was unwillingness of health care provider to provide PCC. Women who reported that the unwillingness of health care providers to give PCC were 56.4% less likely to utilize preconception care services than their counter parts.
Strength and Limitation
Limitation of the Study
A limitation of this study is that it is purely quantitative and does not have capacity to explore contextual and social factors that may be limiting women in preconception care services. It is also prone to recall bias as women were asked about pre-pregnancy care for the current pregnancy.
Strength of the Study
In this study Participants were recruited using probability sampling technique and larger sample size.
Conclusion
The finding of this study showed that preconception care utilization was low and partner support on preconception care utilization, previous history of obstetric problem, Women’s knowledge on preconception care utilization, getting an advice on preconception care utilization, unwillingness of service provider on preconception care utilization and being diagnosed for anemia were significantly associated with preconception care utilization services [34-68].
Recommendation
For Ethiopian Federal Police Hospital: Integrating preconception care services with other maternal neonatal child health, improving women’s/couple’s knowledge & strengthening counseling services is vital. Mobilizing and motivating health care providers’ through on job training in collaboration with governmental and non-governmental stake holders work in area of maternal and child health to increase women preconception care utilization and CRC. Information, education, and communication (IEC) activities should be strengthened at all level of Federal police commission health facilities that increase the awareness of mothers about preconception care.
For Health Care Providers: Providing Health education for women in reproductive age groups on preconception care services, its components and importance at all level of health care setting to increase the uptake of preconception care services by integrating with other maternal health services. Recognize the role of male partner in preconception care services; through education, men will likely increase the awareness of these issues among married couples and male involvement should be encouraged for provision of partner support. Encourage male involvement by health extension workers, applying CRC at all health service settings.
For Researchers in Academic Area: Further qualitative research should be done on the relationship factors associated and the preconception care utilization services. It would be better to design culturally appropriate, evidence-based policy, strategically interventions and programs which encompass the all components of preconception care which will be changing into the action.
Declarations
Ethical Approval and Consent to Participate: Ethical clearance and support letter were obtained from Addis Ababa medical and Business college Ethical review Committee. Permission to letter to gather data was obtained from Federal Police Hospital administrative office. An information sheet was provided for study participants on the introductory part of the questionnaires and interview topic guide that further explains the study purpose and confidentiality of the research information. In addition, oral consent was sought from the study participants prior to data collection. Respondents have the right not to participate or withdraw from the study at any stage, and all study methods were performed in accordance with the Declaration of Helsinki.
Availability of Data and Materials: The data used to support the findings of this study are available from the corresponding author upon request.
Author Contributions
Meskerem Gudeta, Conceptualization, Formal analysis, Methodology, Resources, Software, Visualization, Writing and original draft. Fikirte Woldeselassie, Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Project administration, Resources, Software, Visualization, Writing –original draft. Chala Getaneh Conceptualization, Formal analysis, Methodology, Software, Supervision, Writing, review & editing.
Acknowledgments
The authors would like to express their gratitude to respective health facility, data collectors, supervisors and study participants for their diligence and dedication in the collecting and inputting high quality data used in the study.
References
- Mason, E., Chandra-Mouli, V., Baltag, V., Christiansen, C., Lassi, Z. S., & Bhutta, Z. A. (2014). Preconception care: advancing from ‘important to do and can be done’to ‘is being done and is making a difference’. Reproductive health, 11(Suppl 3), S8.
- Guideline N. Diabetes in pregnancy: management from preconception to the postnatal period NICE guideline Published: 25 February 2015. 2019;(February 2015):55.
- Kerber, K. J., de Graft-Johnson, J. E., Bhutta, Z. A., Okong, P., Starrs, A., & Lawn, J. E. (2007). Continuum of care for maternal, newborn, and child health: from slogan to service delivery. The Lancet, 370(9595), 1358-1369.
- Dean, S., Rudan, I., Althabe, F., Webb Girard, A., Howson, C., Langer, A., ... & Bhutta, Z. A. (2013). Setting research priorities for preconception care in low-and middle-income countries: aiming to reduce maternal and child mortality and morbidity. PLoS medicine, 10(9), e1001508.
- Braspenningx, S., Haagdorens, M., Blaumeiser, B., Jacquemyn, Y., & Mortier, G. (2013). Preconceptional care: a systematic review of the current situation and recommendations for the future. Facts, views & vision in ObGyn, 5(1), 13.
- Alkema, L., Chou, D., Hogan, D., Zhang, S., Moller, A. B., Gemmill, A., ... & Say, L. (2016). Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. The lancet, 387(10017), 462-474.
- Kay, J., Posner Samuel, F., Janis, B., Cordero José, F., Atrash Hani, K., Parker Christopher, S., ... & Curtis Michele, G. (2006). Recommendations to improve preconception health and healthcare—United States. A report of the CDC/ATSDR Preconception Care Work Group and the Select Panel on Preconception Care. Atlanta, 55, 1-23.
- Say, L., Chou, D., Gemmill, A., Tunçalp, Ö., Moller, A. B., Daniels, J., ... & Alkema, L. (2014). Global causes of maternal death: a WHO systematic analysis. The Lancet global health, 2(6), e323-e333.
- Dean, S. V., Lassi, Z. S., Imam, A. M., & Bhutta, Z.(2014). Preconception care: promoting reproductive planning. Reproductive health, 11(Suppl 3), S2.
- Mastroiacovo, P., Nilsen, R. M., Leoncini, E., Gastaldi, P., Allegri, V., Boiani, A., ... & Scarano, G. (2014). Prevalence of maternal preconception risk factors: an Italian multicenter survey. Italian journal of pediatrics, 40(1), 91.
- Al Darzi, W., Al Mudares, F., Farah, A., Ali, A., & Marzouk, D. (2014). Knowledge of periconceptional folic acid use among pregnant women at Ain Shams University Hospital, Cairo, Egypt. EMHJ-Eastern Mediterranean Health Journal, 20(9), 561-568.
- Lim E, Lee S, Arzuar N, Rahim A, Azdiana S, Din T. www. eduimed.com â?» Penerbit Universiti Sains Malaysia. Educ Med J [Internet]. 2016;8(4):47–56. http://dx.doi.org/10.5959/ eimj.v8i4.473
- Lawal, T. A., & Adeleye, A. O. (2014). Determinants of folic acid intake during preconception and in early pregnancyby mothers in Ibadan, Nigeria. The Pan African Medical Journal, 19, 113.
- Gezahegn, A. (2016). Assessment knowledge and experience of preconception care among pregnant mothers attending antenatal care in West Shoa Zone Public Health Centers, 2016 (Doctoral dissertation, Addis Ababa University).
- Ayalew, Y., Mulat, A., Dile, M., & Simegn, A. (2017). Women’s knowledge and associated factors in preconception care in adet, west gojjam, northwest Ethiopia: a community based cross sectional study. Reproductive health, 14(1), 15.
- Ayalew, A. F., Bantie, G. M., Kassa, T. B., & Woya, A. A. (2019). Prevalence of pre-eclampsia and associated factors among women attending antenatal care services in Felege-Hiwot referral hospital, Bahir Dar city, Northwest Ethiopia.
- Asresu, T. T., Hailu, D., Girmay, B., Abrha, M. W., & Weldearegay, H. G. (2019). Mothers’ utilization and associated factors in preconception care in northern Ethiopia: a community based cross sectional study. BMC pregnancy and childbirth, 19(1), 347.
- Demisse, T. L., Aliyu, S. A., Kitila, S. B., Tafesse, T. T., Gelaw, K. A., & Zerihun, M. S. (2019). Utilization of preconception care and associated factors among reproductive age group women in Debre Birhan town, North Shewa, Ethiopia. Reproductive health, 16(1), 96.
- Joyce, C., Keraka, M., & Njagi, J. (2018). Assessment of the knowledge on pre conception care among women of reproductive age in Ruiru sub-county, Kiambu county, Kenya. Glob J Health Sci, 3(1), 82-100.
- Goshu, Y. A., Liyeh, T. M., & Ayele, A. S. (2018). Preconception care utilization and its associated factors among pregnant women in Adet, North-Western Ethiopia (Implication of Reproductive Health). Journal of Women's Health Care, 7(05).
- Wegene, M. A., Gejo, N. G., Bedecha, D. Y., Kerbo, A. A., Hagisso, S. N., & Damtew, S. A. (2022). Utilization of preconception care and associated factors in Hosanna Town, Southern Ethiopia. PloS one, 17(1), e0261895.
- Kassa, A., & Yohannes, Z. (2018). Women’s knowledge and associated factors on preconception care at Public Health Institution in Hawassa City, South Ethiopia. BMC research notes, 11(1), 841.
- Ahmed, K., Saeed, A., & Alawad, A. (2015). Knowledge, attitude and practice of preconception care among Sudanese women in reproductive age about rheumatic heart disease. Int J Public Health, 3(5), 223-7.
- Experience THE, Tertiary OFA, Facility H, Pregestational OOF, Mellitus D, Pregnant A, et al. January, 2019 Volume 11, No. 1. 2019;11(1).
- Jafari, F., & Rashidi, S. (2017). Iranian women's knowledge and attitude regarding preconception health: 12 years after integration into the primary health care network. Journal of Nursing and Midwifery Sciences, 4(4), 104-109
- Diabetes and Pregnancy Group F. Knowledge about preconception care in French women with type 1 diabetes.2005. 2005;Vol 31, N°.
- Gurmu, K., Negash, W., Kaba, Z., & Wondimu, R. (2021).Experience of pregnant mothers on preconception care among antenatal care attendants in Sendafa town public health facilities, Ethiopia, 2020. World, 6(3), 99-109.
- Setegn, M. (2021). What women do before pregnancy? A preconception care of women in Mizan-Aman town Southwest, Ethiopia, a mixed study. Prim Health Care, 11(1), 361.
- Dean, S. V., Imam, A. M., Lassi, Z. S., & Bhutta, Z. A. (2013). Systematic review of preconception risks and interventions. Pakistan: Division of Women and Child Health, Aga Khan University.
- Idris, S. H., Sambo, M. N., & Ibrahim, M. S. (2013). Barriers to utilisation of maternal health services in a semiurban community in Northern Nigeria: The clients’ perspective. Nigerian Medical Journal, 54(1) .
- Gautam P, Dhakal R. Knowledge on Preconception Care among Reproductive age Women. Saudi J Med Pharm Sci [Internet]. 2016;2(1):1–6.
- Ding Yan, D. Y., Li XiaoTian, L. X., Xie Fei, X. F., & Yang YuLin, Y. Y. (2015). Survey on the implementation of preconception care in Shanghai, China.
- Al-Akour, N. A., Sou’Ub, R., Mohammad, K., & Zayed, F. (2015). Awareness of preconception care among women and men: a study from Jordan. Journal of Obstetrics and Gynaecology, 35(3), 246-250
- Health Council of the Netherlands: Preconception care: A good beginning. Health Council of the Netherlands. 2007.
- United Nations. Millenium develoment goals. 2015;1–75.
- World health organization. maternal-mortality-infographic2015_part4 who.pdf. geneve,swizerland; 2015
- Mgawadere, F., Kana, T., & Van Den Broek, N. (2017). Measuring maternal mortality: a systematic review of methods used to obtain estimates of the maternal mortality ratio (MMR) in low-and middle-income countries. British medical bulletin, 121(1), 121-134.
- Csace, I. (2016). Ethiopia demographic and health survey 2016. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF, 1-551.
- Atrash, H. K., Johnson, K., Adams, M., Cordero, J. F., & Howse, J. (2006). Preconception care for improving perinatal outcomes: the time to act. Maternal and child health journal, 10(Suppl 1), 3-11.
- World Health Organization. (2015). Trends in maternal mortality: 1990 to 2015. 2015. World Health Organization. Geneva.
- HSTP F. Health Sector Transformation Plan. 2015.
- World Health Organization. (2013). Meeting to develop a global consensus on preconception care to reduce maternal and childhood mortality and morbidity: World Health Organization Headquarters, Geneva, 6–7 February 2012: meeting report.
- Patabendige, M., & Goonewardene, I. M. R. (2013). Preconception care received by women attending antenatal clinics at a Teaching Hospital in Southern Sri Lanka. Sri Lanka Journal of Obstetrics and Gynaecology, 35(1).
- Akinajo OR, Osanyin GE, Okojie OE. DOI: 10.4103/jcls. jcls_3_17. 2019;(4):4–11.
- Mutale, P., Kwangu, M., Muchemwa, C. M. K., Silitongo, M., & Chileshe, M. (2017). Knowledge and preconception care seeking practices among reproductive-age diabetic women in Zambia. International Journal of Translational Medical Research and Public Health, 1(2), 36-43
- Conlin, M. L., MacLENNAN, A. H., & Broadbent, J. L. (2006). Inadequate compliance with periconceptional folic acid supplementation in South Australia. Australian and New Zealand journal of obstetrics and gynaecology, 46(6), 528-533.
- Sh S, Aghodak P IM. Effect of preconception care protocol implementation on women’s awareness. Iranian Journal of Education in Medical science. 2007:525-32. 2007.
- A. T. Knowledge, practice and associated factors of preconception care service among pregnant women attending antenatal care in governmental health facilities, Debremarkos town, Northwest Ethiopia: unpublished thesis. 2015. 2015.
- Goodfellow, A., Frank, J., McAteer, J., & Rankin, J. (2017). Improving preconception health and care: a situation analysis. BMC health services research, 17(1), 595.
- Dean, S. V., Lassi, Z. S., Imam, A. M., & Bhutta, Z.(2014). Preconception care: nutritional risks and interventions. Reproductive health, 11(Suppl 3), S3.
- Gluckman, P. D., Hanson, M. A., & Buklijas, T. (2010). A conceptual framework for the developmental origins of health and disease. Journal of developmental origins of health and disease, 1(1), 6-18.
- M. Maternal Care Package A Guide to field Healthcareworkers. Sri Lanka: WHO. Retrieved 0ctober22, 2019.
- Dean, S. V., Lassi, Z. S., Imam, A. M., & Bhutta, Z. A. (2014). Preconception care: closing the gap in the continuum of care to accelerate improvements in maternal, newborn and child health. Reproductive health, 11(Suppl 3), S1.
- Nepali, G., & Sapkota, S. D. (2017). Knowledge and practice regarding preconception care among antenatal mothers. International Journal of Perceptions in Public Health, 1(4), 224-227.
- Muraizeq Y, Alshammari M, Almutairi A. RESEARCH ARTICLE PRE CONCEPTION CARE : ITS RECOGNITION AND ACCEPTANCE IN HAIL , KSA . A CROSSSECTIONAL STUDY College of Medicine / University of Hail , KSA of Medicine / University of Hail , KSA. 2018.
- Ahmed, M. H., & Piro, J. (2017). T., 2017. Knowledge, Practice, and Attitude of Married Women About Preconception Care. Journal of Client-Centered Nursing Care, 3(1), 37-44.
- Mazza, D., & Chapman, A. (2010). Improving the uptake of preconception care and periconceptional folate supplementation: what do women think?. BMC Public Health, 10(1), 786.
- Joyce, C. H. E. P. N. G. E. T. I. C. H. (2018). Utilization of Preconception Care Services among Women of Reproductive Age in Kiambu County, Kenya (Doctoral dissertation, Kenyatta University).
- Shadab, P., Nekuei, N., & Yadegarfar, G. (2017). The prevalence of preconception care, its relation with recipients’ individuality, fertility, and the causes of lack of checkup in women who gave birth in Isfahan hospitals in 2016. Journal of education and health promotion, 6(1), 88.
- Hakari, D., Mohammadzadeh, R. A. H. M. A. T., Velayati, A., & Bolourian, M. (2011). Barriers of prenatal care and its relationship with pregnancy outcome among women visited to Tabriz hospitals in 2009.
- Shen, H., Edwards, H., Courtney, M., McDowell, J., & Wei, J. (2013). Barriers and facilitators to diabetes selfâ?management: Perspectives of older community dwellers and health professionals in C hina. International journal of nursing practice, 19(6), 627-635.
- Kim, S. Y., Deputy, N. P., & Robbins, C. L. (2018). Diabetes during pregnancy: surveillance, preconception care, and postpartum care. Journal of Women's Health, 27(5), 536-541.
- Chuang, C. H., Velott, D. L., & Weisman, C. S. (2010). Exploring knowledge and attitudes related to pregnancy and preconception health in women with chronic medical conditions. Maternal and child health journal, 14(5), 713-719.
- Mahmud, M., & Mazza, D. (2010). Preconception care of women with diabetes: a review of current guideline recommendations. BMC women's health, 10(1), 5.
- Bhutta, Z. A., Dean, S. V., Imam, A. M., & Lassi, Z. S. (2011). A systematic review of preconception risks and interventions. Karachi: The Aga Khan University..
- Elsinga, J., de Jong-Potjer, L. C., van der Pal-de, K. M., le Cessie, S., Assendelft, W. J., & Buitendijk, S. E. (2008). The effect of preconception counselling on lifestyle and other behaviour before and during pregnancy. Women's Health Issues, 18(6), S117-S125.
- Akinajo, O. R., Osanyin, G. E., & Okojie, O. E. (2019). Preconception care: Assessing the level of awareness, knowledge and practice amongst pregnant women in a tertiary facility. Journal of Clinical Sciences, 16(3), 87-92.
- Boka, A., & Nigatu, D. (2019). Assessment of adverse birth outcomes and associated factors among diabetic pregnant mothers who delivered at Mettu Karl Hospital, Illubabor Zone, South West Ethiopia-2018. Intern Med, 9(302), 2.


