Case Report - (2018) Volume 3, Issue 1
Multiple Intraoral Venous Malformations In A Geriatric Patient: A Rare Case Report
Received Date: Apr 11, 2018 / Accepted Date: Apr 16, 2018 / Published Date: Apr 24, 2018
Copyright: ©S Dangore Khasbage. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Venous malformation (VM) is defined as a simple malformation with slow flow and an abnormal venous network. This is caused by a disturbance in the late stages of angiogenesis (trunal stage) resulting in the persistence of arteriovenous anastomosis present during embryonic life. This case report describes an unusual case of multiple intraoral venous malformations with questionable augmentation. A 65 year-old female had reported with a complaint of discomfort in mouth since 8 years. Intraoral examination revealed presence of six spherical swellings (three on dorsal surface of tongue, one on ventral surface of tongue and two on left buccal mucosa) with bluish-violet hue, approximately 2 to 3 cm in diameter each. On the basis of history and clinical findings, vascular malformation was provisionally suspected. Adequate imaging established the diagnosis. A review of clinical aspects, diagnostic procedures as well as therapeutic options currently available for venous malformations are discussed in this article.
Keywords
Vascular Malformation, Venous Malformation, Hemangioma
Introduction
Vascular lesions are among the most common congenital and neonatal abnormalities. On the basis of histological and embryological aspects, these are divided into two categories – haemangiomas and vascular malformations [1].
Vascular malformations may be single vessel forms or a combination and are designated according to the predominant channel type as capillary malformations, lymphatic malformations, venous malformations (VM), arteriovenous malformations, and complex forms [2, 3]. Capillary, lymphatic and VM are classified as “low-flow” lesions. Arterial and arteriovenous malformations are often referred as “high-flow” vascular malformations and are often the cause of massive, sometimes fatal haemorrhages [3, 4]. Amongst all VM are the most common with overall incidence about 1 in 10 000 [5, 6].
In this article, an unusual case of multiple intraoral VMs and review about diagnostic procedures as well as therapeutic options for these lesions are described.
Case Report
A 65 year old female reported to Department of Oral Diagnosis and Medicine with a chief complaint of multiple intraoral growths since 10 years. History revealed that the patient had noticed four small nodular painless peanut sized swellings on oral mucosa (two on left buccal mucosa and two on dorsum surface of tongue). Within the subsequent two years two additional swellings appeared. All these swellings increased gradually in size to the present status in last 8-10 years. Due to swellings, the patient had difficulty in chewing, swallowing and speaking. Patient also gives history of repeated trauma but no history of bleeding. Her medical history revealed that she was suffering from diabetes mellitus, ischemic heart disease and schizophrenia and was taking regular oral medications for the same since 6-7 years.
Intraoral examination revealed presence of six swellings, three diffuse swellings situated on dorsum surface of the tongue (Figure 1), two nodular well defined swellings on left buccal mucosa (Figure 2) and one on ventral surface of tongue.
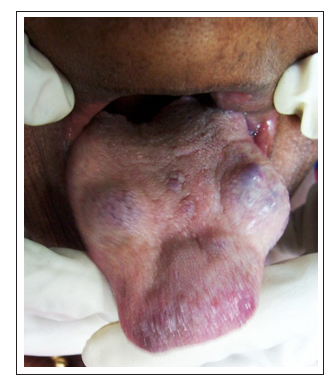
Figure 1: Three diffuse swellings on dorsal surface of tongue
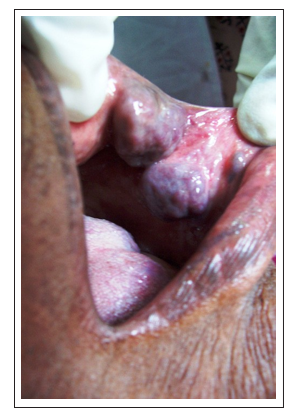
Figure 2: Two well defined swellings on left buccal mucosa
Approximate size of each swelling was 2 to 3 cm in diameter, irregularly spherical in shape, had bluish-violet hue. On the basis of history and clinical features a provisional diagnosis of vascular malformations was made while hemangioma was considered in differential diagnosis. As a tradition, color Doppler ultrasonography was performed as first imaging modality which showed the presence of low venous flow within the malformation suggesting VM. Considering patient’s age and her systemic status, serial laser treatment by using YAG laser (1064 nm wavelength) was planned. The lesions on left buccal mucosa were treated by laser in non contact mode for 3 minutes on the first visit of the patient with an expectation to cause shrinkage of the lesions. However, she was not willing for further diagnostic procedures as well as treatment and lost subsequent follow-up
Discussion
Most VM are solitary, but multiple cutaneous or visceral lesions can occur [6]. But, multiple intraoral VM is an unusual presentation. In the present case, history and clinical features correspond to vascular low flow malformation. However, it is impossible to predict the exact cause for sudden appearance of lesions before 10 years as no such presentation about VM is reported in literature. However, rapid increase in size of arteriovenous malformation is reported secondary to infection, trauma, ligation, attempted excision or via hormonal influences such as during pregnancy and puberty [7]. Similarly, in this case, two etiological factors, either trauma during mastication or hormonal imbalance during menopause can be predicted.
Regarding diagnostic approach, conventional radiography usually demonstrates a soft-tissue mass with occasional phleboliths and, occasionally, adjacent skeletal anomalies. Doppler ultrasonography demonstrates absence of flow or low-velocity venous flow. Computed tomography and magnetic resonance (MR) imaging are used primarily for pretreatment evaluation of lesion extension. These lesions are usually hypo intense on T1-weighted MR images and markedly hyper intense on T2-weighted images with variable gadolinium enhancement [5, 8].
Direct phlebography helps to confirm the diagnosis and exclude other soft-tissue tumors. Three distinct phlebographic patterns are cavitary, spongy, dysmorphic [5, 8]. Angiography demonstrates the flow characteristics, feeding vessels, and dangerous anastomoses [9, 10].
Seldom, immunohistochemistry may be necessary to distinguish between vascular malformations and vascular tumors by evaluation of proliferation markers [2].
Concerning the treatment, only symptomatic VM causing important functional and aesthetic prejudice require treatment. Treatment goals and modalities change with the size, depth, location and nature of lesion. Management includes conservative and surgical modalities. Surface non-contact Nd: YAG laser can be used to treat any intraoral involvement of the venous malformation. Serial laser treatments as often as every 3 months can be used to control the growth and diminish the size of the malformation in the tongue, buccal, palatal, and gingival areas [11].
Sclerotherapy can be used with or without surgery. The purpose of using sclerothearpy before surgery is to shrink a VM by sclerotherapy before scheduling surgical resection [3]. Direct phlebography is performed when a more detailed assessment of the vascular pattern is needed or as part of sclerotherapy [5].
Surgical excision continues to be a good treatment option but excision of extensive lesions remains a challenge as VMs are rarely well-defined lesions and intraoperative bleeding can make identification and preservation of important structures difficult [11]. The patient with a large VM can be managed non- operatively by giving daily aspirin to prevent thrombosis and associated pain [10].
To summarize, VMs, although benign lesions, can present a diagnostic and management challenge. A multidisciplinary approach to treat these lesions is strongly recommended as there is no single superior treatment modality.
1. Competing Interests: None
2. Funding Information: Not Applicable
3. Authors’ Contributions-sole author Dr Suwarna Dangore- Khasbage contributed at all steps of this work
References
- Mulliken JB, Glowacki J. Hemangiomas (1982) and vascular malformations in infants and children: a classification based on endothelial characteristics. Plast Reconstr Surg 69: 412-422.
- Lanza A, Gombos F (2008) A case of multiple oral vascular tumors: the diagnostic challenge on haemangioma still remains open. The J Stomatol Invest 2: 67-71.
- Jennifer J. Marler, John B. Mulliken (2005) Current management of hemangiomas and vascular malformations. Clin Plastic Surg 32: 99 -116.
- Fishman SJ, Mulliken JB. Hemangiomas (1996) and vascular malformations of infancy and childhood. Pediatr Clin North Am 40: 1177-1200.
- Dubois J, Soulez G, Oliva VL, Marie-Jose´e Berthiaume, Chantale Lapierr et al. (2001) Soft-Tissue Venous Malformations in Adult Patients: Imaging and Therapeutic Issues. Radio Graphics 21: 1519-1531.
- Boon LM, Mulliken JB, Enjolras O, Vikkula M (2004) Glom venous malformation (glomangioma) and venous malformation: distinct clinicopathologic and genetic entities. Arch Dermatol 140: 971-976.
- Martines F, Immordino V (2009) Arteriovenous malformation of the base of tongue in pregnancy: case report. Acta Otorhinolaryngol Ital 29: 274-278.
- Cappabianca S, Vecchio WD, Giudice A, Colella G (2006) Vascular malformations of the tongue: MRI findings on three cases. Dento Maxillofac Rad 35: 205-208.
- Kakimoto N, Tanimoto K, Nishiyama H, Murakami S, Furukawa S et al. (2005) CT and MR imaging features of oral and maxillofacial hemangioma and vascular malformation. Eur J Radiol 55: 108-112.
- Hein KD, Muliken JB, Kozakewich HP, Upton J, Burrows PE(2002) Venous malformations of skeletal muscle. Plast ReconstrSurg 110: 1625-1635.
- Buckmiller LM, Richter GT, Suen JY (2010) Diagnosis and management of hemangiomas and vascular malformations of the head and neck. Oral Dis 16: 405-418.


