Research Article - (2025) Volume 4, Issue 3
Minimally Invasive Percutaneous Mechanical Discectomy for Lumbar Disc Herniation: A Case Report and Technical Insight
2Azienda Ospedaliera Universitaria Università degli Studi della Campania Luigi, Vanvitelli, Naples Dipartimento di medicina di precisione, Italy
3Saint Camillus International University of Health and Medical Sciences, Rome, Italy
4University of Salerno, Italy
Received Date: Jun 26, 2025 / Accepted Date: Jul 28, 2025 / Published Date: Sep 23, 2025
Copyright: ©Â©2025 Francesco Saturno, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Saturno, F., Monaco, G., Salerno, A., Cianciola, A., Secondulfo, C., et al. (2025). Minimally Invasive Percutaneous Mechanical Discectomy for Lumbar Disc Herniation: A Case Report and Technical Insight. J Surg Care, 4(3), 01-04.
Abstract
Background: Low back pain is one of the leading causes of disability worldwide and contributes significantly to healthcare costs. Among its most common etiologies is lumbar disc herniation, often associated with radicular symptoms and reduced quality of life.
Objective: This article presents a case of symptomatic L3-L4 lumbar disc herniation treated with a minimally invasive percutaneous discectomy technique. We describe the procedural steps and assess the patient's clinical outcomes over a one-year follow-up.
Methods: A 38-year-old patient with persistent radicular pain and dysesthesia underwent percutaneous discectomy using a bipolar radiofrequency system, enabling decompression, ablation, and annular modulation in a single procedure. The technique was performed under fluoroscopic guidance.
Results: Postoperative evaluation at 7 days, 3 months, 6 months, and 1 year showed complete resolution of symptoms and progressive clinical improvement, with no complications.
Conclusion: The described percutaneous discectomy technique appears safe and effective for selected patients with contained lumbar disc herniation. Further studies are needed to validate long-term outcomes and define standardized indications.
Keywords
Health, Apps, Google Play Store, Machine Learning
Introduction
Low back pain remains one of the most prevalent and disabling conditions globally, representing a significant burden on healthcare systems and society. Approximately 80% of the adult population in industrialized countries experiences at least one episode during their lifetime. Over the past decade, the number of spinal surgical procedures has markedly increased, partly due to population aging and advancements in diagnostic imaging. One of the primary causes of low back pain and radiculopathy is lumbar disc degeneration, which can lead to nucleus pulposus herniation, local inflammation, or nerve root compression. While conservative therapy remains effective in about 60% of cases, a subset of patients requires surgical intervention to achieve symptomatic relief.
The traditional surgical approach—open discectomy—aims to decompress the nerve root and alleviate pain. However, in recent years, numerous minimally invasive techniques have emerged, including percutaneous mechanical and laser discectomy, as shown in figure 1. These procedures aim to reduce tissue damage and recovery time, while maintaining efficacy. Despite encouraging results and good patient acceptance, these techniques have encountered skepticism in parts of the surgical community. Among them, endoscopic foraminal discectomy has gained widespread recognition. In this article, we present a case of lumbar herniation treated with a percutaneous mechanical discectomy system, describing the technique in detail and reporting clinical follow-up.
Figure 1: Spinal Needle Positioning under Fluoroscopic Guidance during the Percutaneous Discectomy Procedure
Case Description
A 38-year-old male patient presented with persistent right-sided radicular pain and dysesthesia in the lower limb. MRI (T1, T2, STIR sequences) revealed a right foraminal L3-L4 lumbar disc herniation, with preservation of the nucleus pulposus.
The patient initially underwent a cycle of image-guided epidural steroid injections, which provided only partial and temporary relief. Given the persistence of symptoms and radiological findings, surgical intervention was indicated. The selected procedure was a percutaneous mechanical discectomy using an integrated, minimally invasive radiofrequency-based system capable of core decompression, nuclear ablation, and annular modulation.
Surgical Technique
Step 1: Needle Insertion and Discography: A 16G spinal needle was inserted through Kambin’s triangle into the proximal third of the L3-L4 disc space. A discogram was performed using a mixture of contrast agent, saline, and indigo carmine dye in a 6:3:1 ratio.
Step 2: Guidewire Placement: A guidewire was advanced through the needle into the disc nucleus, and correct placement was verified fluoroscopically.
Step 3: Skin Incision and Cannula Introduction: After a small incision with a No. 11 scalpel, the needle was removed, and a dilator-cannula assembly was introduced over the guidewire. As shown in Figure 2, a lumbar foramen dilator was inserted through the lateral access under fluoroscopic control.
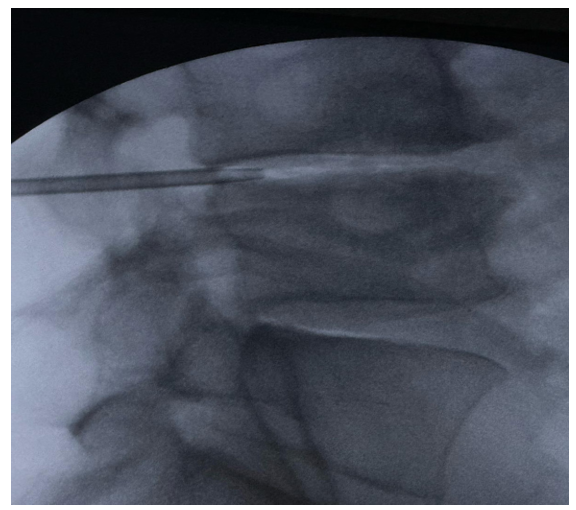
Figure 3: Lateral fluoroscopic view showing the insertion of a dilator into the intervertebral foramen during a minimally invasive percutaneous procedure. The instrument is precisely positioned under imaging guidance to allow access to neural or discal structures, facilitating the subsequent therapeutic phase. The correct trajectory and depth of the dilator are confirmed by the visualization of adjacent bony landmarks
Figure 2: The operator is inserting a lumbar foramen dilator through a lateral percutaneous access under fluoroscopic guidance. The real-time fluoroscopic image on the monitor shows a lateral projection, allowing verification of the correct trajectory and depth of the instrument within the intervertebral foramen
Step 4: Anulotomy and Cannula Advancement: An anulotomy was performed using a drill advanced through the annulus. Once the working portal was established, the guidewire and dilator were removed.
Step 5: Manual Discectomy: A 2.7 mm grasping forceps was inserted through the cannula to manually remove approximately 1–2 grams of nuclear material. The excised tissue was collected for pathological examination.
Step 6: Nucleus Ablation: Radiofrequency ablation was performed using a bipolar probe with settings at 25W (Bipolar Turbo mode). Energy was delivered in six 6-second pulses at clock positions.
Step 7: Annular Modulation: Using the bipolar coagulation mode (25W), the same probe was applied along the annular wall in a sawing motion. This step aimed to contract collagen fibers and treat nociceptors.
The system operated at low temperatures (up to 41°C in the nucleus, 32.5°C in the annulus), ensuring thermal safety and preserving adjacent structures. No intraoperative complications were observed. Funding
Postoperative Follow-Up and Outcome
The patient was evaluated at 7 days, 3 months, 6 months, and 1 year postoperatively. He reported complete resolution of radicular pain and dysesthesia, with progressive and stable clinical improvement over time. No recurrence or complications were noted.
Conclusion
Minimally invasive percutaneous mechanical discectomy rep- resents a promising alternative to conventional surgery for select- ed patients with contained lumbar disc herniation. The described technique combines core decompression, ablation, and annular modulation in a single, fluoroscopically guided session, ensuring precision and safety. Although open microdiscectomy remains the gold standard due to its reproducibility and outcomes, percutane- ous approaches are gaining attention for their reduced invasive- ness, shorter recovery, and low complication rates. However, the evidence base remains limited, and further randomized controlled studies are warranted to define their role in modern spine surgery. Minimally invasive percutaneous discectomy techniques have shown promising long-term outcomes in selected patients, as sup- ported by recent studies [1-12].
Funding
This research received no external funding.
References
- Manchikanti L, Kaye AD, Knezevic NN, et al. (2020). Efficacy of Percutaneous Disc Decompression in the Management of Lumbar Disc Herniation. A Systematic Review. Pain Physician. 23(2):137-154.
- Mobbs, R. J., Rao, P. J. (2019). Minimally invasive lumbar discectomy: current practice and future developments. J Spine Surg. 5(1): S42–S50.
- Kim, H. S., Chung, C. K., Jahng, T.A., Kim, H. J. (2018).Percutaneous lumbar discectomy: review of current concepts and indications. World Neurosurg. 112:374-384.
- Zeng, C., Li, H., Yang, T., et al. (2018). Comparison of minimally invasive and open discectomy for lumbar disc herniation: a meta-analysis of randomized controlled trials. Int J Surg. 56:320-329.
- Gibson, J. N. A., & Waddell, G. (2007). Surgical interventions for lumbar disc prolapse: updated Cochrane Review. Spine, 32(16), 1735-1747.
- Choy, D. S. (1995). Percutaneous lumbar discectomy. Neuro surg Clin N Am. 6(3):423-428.
- Casper, G. D. (2010). Indications and contraindications for minimally invasive spine surgery. Spine. 35(26 Suppl): S254– S261.
- Muto, M., Zanirato, A., Migliorini, F. (2022). Minimally invasive percutaneous lumbar discectomy: indications and long-term outcomes. Eur Spine J. 31(9):2225-2235.
- Ryang, Y. M., Narvid, J., Albers, G. W., et al. (2021). Endoscopic transforaminal lumbar discectomy: A systematic review and meta-analysis of clinical outcomes. Neurosurg Focus. 50(1):E5.
- Choi, K. C., Shim, H. K., Ryu, K. S., et al. (2020). Long- term clinical outcomes of percutaneous endoscopic lumbar discectomy in patients with lumbar disc herniation: a minimum 5-year follow-up study. Pain Physician. 23(5): E487-E495.
- Lee, C. H., Kim, Y. S., Kwon, B. K., et al. (2021).Radiofrequency nucleoplasty for lumbar disc herniation: clinical outcomes and safety profile. J Pain Res. 14:1073- 1081.
- Laxmaiah Manchikanti, M. D., Boswell, M. V., & MA, S.A. (2009). Comprehensive evidence-based guidelines for interventional techniques in the management of chronic spinal pain. Pain physician, 12, 699-802.





