Review Article - (2025) Volume 4, Issue 3
Mapping the Gaps: A Meta-Review of Systematic Reviews on Global Depression Prevalence and its Policy Implications
2Texas A&M University, USA
3Western Illinois University, USA
4University of Gloucestershire, USA
5University of Louisiana, USA
6University of Wisconsin-Milwaukee, USA
7University of Abuja, Nigeria
Received Date: Jul 17, 2025 / Accepted Date: Aug 22, 2025 / Published Date: Aug 27, 2025
Copyright: ©Â©2025 Godwin Aipoh, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Aipoh, G., Hanson, U., Ubani, C., Oye, V., Jegede, O., et, al. (2025). Mapping the Gaps: A Meta-Review of Systematic Reviews on Global Depression Prevalence and its Policy Implications. Int J Health Policy Plann, 4(3), 01-10.
Abstract
Introduction and Background: Depression is a leading cause of disability globally, yet understanding its prevalence remains fragmented. Despite increasing systematic reviews, synthesis across populations and regions is still limited. Background: Systematic Reviews and Meta-Analyses (SRMAs) on depression prevalence have proliferated in the last decade. However, methodological inconsistencies, limited geographic coverage, and a lack of policy focus restrict their utility for global strategy.
Purpose and Objectives: This first comprehensive meta-review of existing literature aims to identify gaps and to evaluate global/ continental reach; assess methodological quality and policy alignment; highlight under represented regions and populations to inform future research and policy.
Methodology: Following PRISMA 2020, we systematically searched four databases (2014-2024). Included re- views met quality, scope, and reporting criteria; excluded single country, clinical only, non-English publications. A total of 36 SR-MAs was included.
Results: The findings show a strong continental skew: 55% of studies focus on Asia. Africa and Australia are grossly underrepresented. Most reviews focus on clinical populations, adolescents, or the elderly, neglecting vulnerable groups like informal workers, displaced people, and those facing economic shocks.
Recommendations and Conclusion: We recommend that future research should: Prioritize geographic inclusivity for underrepresented regions. Include broader populations, especially socially vulnerable groups. Align closely with public health goals. While the current evidence base offers insights, there is a need to bridge the gaps. Bridging these gaps is essential for equitable, data-driven policies meeting the depression needs of all communities, especially those often excluded.
Keywords
Continent, Depression, Global Health, Meta-Analyses, Policy Implications, Prevalence, Systematic Review
Introduction
“Depression is not a sign of weakness—it is a signal that something deep within needs attention, healing, and care.”
– Godwin Aipoh
Depression ranks among the leading causes of disability globally and significantly contributes to the overall burden of disease. According to the World Health Organization, approximately 280 million people experience depression globally, with wide disparities in prevalence across countries and demographic groups [1]. Although progress has been made in estimating the burden of depression, much of the evidence still comes from individual studies or first-level meta-analyses, which differ widely in methods, populations, and diagnostic tools. See references [2-5]. At least 21 million Americans experience a major depressive episode annually [6]. This figure emerges from a society that actively promotes open dialogue and help-seeking behavior regarding mental health. It is therefore plausible that the prevalence may be higher in contexts where depression and mental health concerns are not widely recognized as public or national issues. Depression represents a significant public health issue due to its association with emotional distress, increased healthcare costs, elevated suicide risk, and higher mortality from other health conditions [7,8].
The proliferation of Systematic Reviews and Meta Analyses (SRMAs) on depression prevalence has improved the evidence base for understanding regional and population specific burdens. However, the growing number and inconsistency of these SRMAs make it challenging for policymakers, researchers, and public health agencies to draw clear, actionable insights for global mental health planning. Importantly, no existing study has comprehensively synthesized these SRMAs to assess global coverage, methodological consistency, and policy-relevant gaps in depression prevalence research. A meta review also known as an umbrella review offers a useful way to evaluate the scope, quality, and relevance of existing SRMAs.
This approach allows researchers to detect common methodological trends, expose inconsistencies in findings, and identify under represented populations or regions. For example, while some SRMAs focus on adolescents or older adults in high- income countries, others examine patients with additional chronic or psychiatric conditions. Yet few reviews address vulnerable populations such as displaced persons, informal workers, or those affected by economic instability whose mental health outcomes are essential for shaping equitable health policies. While several studies report a rising trend in depression prevalence, it remains unclear whether this increase is consistent across countries, continents, and sub- groups mainly due to limited and uneven evidence [9,10].
Moreover, global disparities in research representation persist. Regions such as Sub- Saharan Africa, Australia, and Latin America remain underrepresented in both primary and secondary depression research, despite facing high unmet mental health needs [11,12 ]. These imbalances affect the design of effective, context sensitive interventions, especially since global funding and resource allocation often rely on data synthesized from SRMAs.
This study offers three key contributions. First, it highlights major gaps in where and for whom depression prevalence is studied; most reviews focus on Asia and clinical groups, while regions like Sub Saharan Africa and vulnerable populations such as informal workers and displaced people are often overlooked. Second, it exposes wide variation in the tools and methods used across reviews, showing a need for more consistent and transparent re- search practices. Finally, it underscores the real-world consequences of these gaps: without more balanced and representative data, global depression health policies risk misallocating resources and missing those most in need.
Methods
Study Design
This study is a systematic meta-review, also known as an umbrella review, of Systematic Reviews and Meta Analyses (SRMAs) on the global prevalence of depression. We conducted this review in accordance with the PRISMA 2020 guidelines for systematic reviews [13]. We also followed established best practices for conducting and reporting meta reviews in the field of public health.
Search Strategy
A comprehensive literature search was conducted in four major databases: PubMed, Embase, Web of Science, and the Cochrane Library. The search window covered studies published between January 2014 and March 2024. We used Boolean operators to combine search terms such as “Depression”, “Systematic Review”, “Meta-Analysis”, “Global Burden” and “Prevalence”.
Eligibility Criteria
Inclusion criteria were based on the following conditions, with the requirement that at least one criterion be satisfied:
• Study Design: Only systematic reviews or meta-analyses synthesizing data on depression prevalence were included.
• Publication Window: Studies published between January 2014 and March 2024, to ensure up-to-date evidence.
• Scope: Included at least 20 primary studies, or if fewer offered a clear rationale for their inclusion.
• Reporting: Reported the number of included studies, described search strategies, and presented conclusions or policy-relevant insights.
In contrast, articles were excluded based on the following criteria:
• Population: Reviews that focused solely on a single country’s populations were excluded
• Setting: Reviews restricted to clinical settings (e.g., Hospitals, Specialized Clinics).
• Focus: Reviews that did not report prevalence estimates or focused solely on treatment efficacy.
• Publication Date and Access: Studies published before 2014 or not available in full text.
• Language: Non-English publications.
Study Selection
The screening process followed a two-stage protocol. First, two independent reviewers screened titles and abstracts for initial eligibility. In the second stage, full texts were reviewed to confirm inclusion against predefined criteria. Disagreements were resolved through discussion or, if needed, consultation with a third reviewer.
Data Extraction
A standardized data extraction template was developed. The following variables were extracted from each included SRMA:
• First author and year
• Geographic coverage
• Number of included studies,
• Population focus (e.g., General Population, Adolescents, Elderly)
• Depression measurement tools (e.g., PHQ-9, GDS, CES-D)
• Prevalence estimates (If Available)
• Study design of included articles (Cross-Sectional, Longitudinal, Etc.)
• Data extraction was carried out by the lead author and independently verified by two co-authors to ensure consistency and reliability, in line with recommendations by Gunhan et al [14].
Quality Assessment
Methodological quality of each included review was assessed using an adapted version of the AMSTAR-2 tool [15].
A five-point scoring system was used to categorize reviews as:
• High quality (100%): Met all five criteria, including actionable recommendations.
• Good (80%): Met four criteria, including 20 studies analyzed.
• Average (60%): Met three criteria.
• Fair (40%): Met only two, usually limited to SRMA design and publication timeframe.
• This tiered approach allowed us to assess both methodological rigor and policy relevance, in alignment with global health evaluation standards [16,17].
This meta-review addresses a critical gap by synthesizing published SR-MAs on depression prevalence from the past decade.
Our objective is to:
• Evaluate the global and demographic scope of existing SRMAs.
• Assess their methodological quality using an adapted AMSTAR-2 framework.
• Identify populations, regions, and methodological dimensions that remain underrepresented or inconsistently studied.
• These findings aim to guide future research and help shape more equitable, evidence-based mental health policies globally.
Results
Study Selection
The systematic search yielded a total of 1,274 records, of which 981 remained after removing duplicates. Following title and abstract screening, 158 full-text articles were assessed for eligibility. Ultimately, 36 Systematic Reviews and Meta-Analyses (SRMAs) met the inclusion criteria and were included in this meta-review. Flowchart presents a PRISMA diagram summarizing the study selection process. In the summary Table, we provide a concise summary of the articles included in our study. Most of the articles scored above our 40% quality threshold, suggesting generally strong methodological standards based on our evaluation criteria. Only a few articles received average scores. Notably, more than 70% of the articles clearly reported their analytic time- frames, and all followed PRISMA guidelines. We grouped the articles into six thematic categories based on their main research focus.
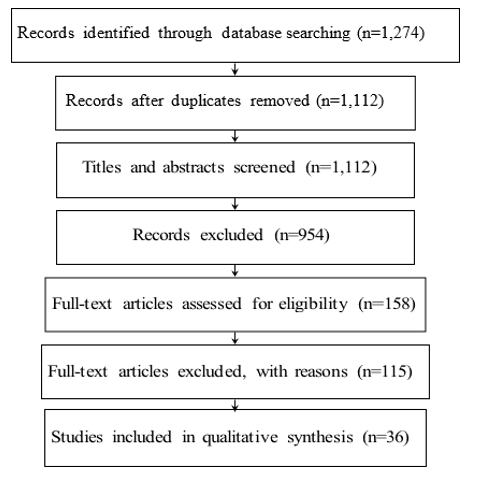
Notes: The study selection process was illustrated using a PRISMA flow diagram, in accordance with the recommendations provided by Page et al [13]. :
Flow Chart: Showing the Selection Process
|
Authors |
Year |
Years Considered |
No of Papers Identified |
No of Papers Used |
Chart Flow Diagram |
Quality |
Concentration |
|
Ting Hu + 6 |
2022 |
2000-2021 |
5791 |
48 |
Yes |
High |
In General, Prevalence is High |
|
Viktoria Vibhakar + 3 |
2019 |
not stated |
3967 |
41 |
Yes |
Good |
Children/ Adolescents |
|
Daan Brandenbarg + 6 |
2019 |
not stated |
643 |
20 |
Yes |
Good |
Cancer Survivors |
|
Trine Ryttersgaard + 4 |
2019 |
1984-2018 |
2028 |
7 |
Yes |
Average |
Young Adult/ Adolescent |
|
Aaisha Farooqi + 7 |
2022 |
1985-2021 |
916 |
44 |
Yes |
High |
Type 1 & 2 Diabetes Patients |
|
Rosa E. Boeschoten + 6 |
2017 |
1965-2014 |
2986 |
58 |
Yes |
High |
Multiple Sclerosis (MS) Patients |
|
Jinghui Wang + 11 |
2017 |
1990-2015 |
3165 |
83 |
Yes |
High |
Outpatients |
|
Motahare Pilevar’ + 5 |
2019 |
2000-2019 |
6140 |
72 |
Yes |
High |
Breast Cancer Patients (BCP) |
|
Hong Cai + 9 |
2023 |
1991-2019 |
5297 |
55 |
Yes |
High |
Older adults |
|
Rohan Puthran + 3 |
2016 |
not stated |
1395 |
77 |
Yes |
Good |
Medical Students |
|
Nasrin Abdoli + 6 |
2022 |
2001-2021 |
2297 |
20 |
Yes |
Good |
Elderly |
|
Bereket Duko + 2 |
2020 |
not stated |
739 |
25 |
Yes |
Good |
Tuberculosis Patients |
|
Lijuan Zhang + 4 |
2017 |
1997-2016 |
3347 |
59 |
Yes |
Good |
Systematic Lupus erthematosus |
|
David Ried + 1 |
2022 |
2005-2019 |
1308 |
210 |
Yes |
Good |
Cancer Patients |
|
Zhanzhan Li + 4 |
2015 |
2005-2014 |
3890 |
41 |
Yes |
Good |
Adults with Hypertension |
|
Sofia Pappa + 5 |
2020 |
2019-2020 |
45 |
45 |
Yes |
Good |
Healthcare Professionals |
|
Darlan Matte + 6 |
2016 |
not stated |
1613 |
8 |
Yes |
Average |
COPD |
|
Parveen Akhtar + 6 |
2020 |
2009-2018 |
2561 |
37 |
Yes |
Good |
Undergraduate in LMIC |
|
Yi-Jung Tung + 3 |
2018 |
2015-2016 |
2872 |
27 |
Yes |
High |
Nursing Students |
|
Wilson Tam + 2 |
2019 |
not stated |
850 |
10 |
Yes |
Average |
Medical Students |
|
Douglas Mata + 6 |
2015 |
1963-2015 |
3343 |
54 |
Yes |
Good |
Resident Physicians |
|
Dara Leung + 3 |
2021 |
not stated |
7370 |
20 |
Yes |
Average |
Dementia Stages |
|
Mohammad Heidari + 6 |
2021 |
1986-2019 |
3527 |
27 |
Yes |
Good |
Post-Hip Fracture |
|
Dario Moreno-A + 5 |
2021 |
1937-2018 |
7397 |
19 |
Yes |
Good |
General Public |
|
Nastaran Karami + 5 |
2023 |
2000-2022 |
9866 |
73 |
Yes |
Good |
Cardiac Patients |
|
Yanli Wu + 3 |
2024 |
2000-2024 |
10032 |
29 |
Yes |
High |
Self-Injured Adolescents |
|
Amir Jalali + 8 |
2024 |
open-2023 |
30283 |
58 |
Yes |
High |
Elderly Population |
|
Bingqing Lu + 2 |
2024 |
open-2023 |
2793 |
96 |
Yes |
High |
Children/ Adolescents |
|
Mohammad Amini + 9 |
2024 |
open-2024 |
680 |
10 |
Yes |
Average |
Orthopedic Residents |
|
Rin Miyaguchi + 6 |
2024 |
not stated |
3919 |
24 |
Yes |
Good |
Restless Legs Syndrome (RLS) |
|
Ting Pan + 5 |
2024 |
open-2023 |
17810 |
86 |
Yes |
Good |
Perinatal Depression |
|
Wenjing Chen + 4 |
2024 |
open-2023 |
859 |
16 |
Yes |
Average |
Melasma Patients |
|
Alexandra Mitchell + 8 |
2023 |
open-2021 |
13902 |
589 |
Yes |
Good |
Perinatal Depression in LMIC |
|
Tai Raina Hunter + 3 |
2024 |
open-2022 |
443 |
21 |
Yes |
Good |
Maternal Post- Childbirth |
|
Alessia Caffieri + 5 |
2023 |
open-2023 |
1268 |
25 |
Yes |
Good |
Perinatal Depression |
|
Zahra Kiani + 5 |
2023 |
open-2022 |
5193 |
22 |
Yes |
Good |
Infertile Men |
Notes: This table offers a snapshot of the key features of the studies included in our review. It outlines the publication year, the study period covered, the number of papers screened and ultimately included, whether a chart flow diagram was provided, the quality assessment, and the specific population focus. Together, these details offer a clear picture of our methodological approach and the strength of our evidence base. The studies span a wide range of populations from those focusing on individuals with chronic illnesses, to others that examine mental health among healthcare professionals [18-25]. Additional studies delve into diverse groups such as adolescents, patients with specific medical conditions, and the general population, offering a rich and varied understanding of depression prevalence across settings [10,26-38].
Table: Overview of Included Studies
Geographic Distribution and Continent Focus
A pronounced geographic and continental imbalance was evident among the included systematic reviews and meta-analyses, as illustrated in Figure 1. We categorized the findings into two groups: continents most frequently represented and those least represented. Asia accounted for the highest proportion, appearing in 55% (n = 20) of the studies, followed by the Americas at approximately 20%. Among the underrepresented continents, Africa appeared in 53% (n = 19) of studies classified as least represented, followed by Australia. In both categories, certain studies lacked sufficient detail to determine the most or least represented continent, and these were classified as “None” in Figure 1.
Figure 1: Most and Least Continents Identified
Target Audience
We further categorized the 36 included studies based on their target audience or scope as shown in Figure 2. This classification yielded six distinct groups: general population, adolescents, individuals with illnesses, professionals, students, and the elderly. About 40% of the studies examined depression in the context of physical illnesses, while 22% focused on the general population. The remaining categories each constituted approximately 11% of thestudies, with the exception of those targeting professionals, which accounted for only about 6%. Notably, we identified a gap in the literature, as certain sub-populations such as security personnel, informal workers, and individuals affected by natural disasters- were largely underrepresented or absent from the reviewed studies. Some of these articles [18,23,26,29,30,33].
Figure 2: Concentration
Forest Plot Synthesis
A forest plot (Figure 3) visualized the variation in pooled prevalence estimates and confidence intervals across SRMAs. Most effect sizes clustered within a central range, though two extreme outliers at +200 and +600 skewed the overall distribution. Confidence intervals varied widely, indicating differences in sample sizes and precision.
Figure 3: Forest Plot
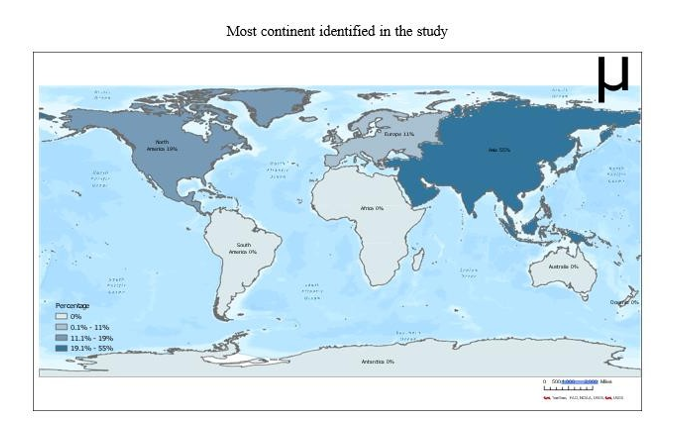
Notes: This figure 4 presents the geographical distribution of studies that examined depression prevalence across continents. It complements the main analysis by highlighting the concentration of research efforts, with Asia and North America being the most represented regions, while Africa, Australia, and South America recorded no included studies
Figure 4: Geographical Distribution of Studies on Depression Prevalence Across Continents
Discussion
This is the first comprehensive meta-review to synthesize global evidence from systematic reviews and meta-analyses on depression prevalence. Our analysis of 36 SRMAs published between 2014 and 2024 reveals major gaps geographic, methodological, and demographic that limit efforts to build globally representative and policy relevant mental health strategies.
Key Findings in Context
The current evidence base is heavily concentrated in Asia, particularly East and South Asia echoing patterns reported by Hu et al [39]. Meanwhile, Africa and Latin America remain significantly underrepresented, despite facing rising mental health burdens and limited access to formal care [11,12]. We also found that existing research takes a fragmented approach to which populations are studied in depression prevalence. Most SRMAs focused on elderly adults, adolescents, or clinical populations, reflecting trends in the existing literature [10,40]. Yet few studies examined high- risk or underserved groups such as postpartum parents, informal workers, refugees, or people affected by economic crises, groups that evidence suggests face disproportionate mental health risks [41,42]. This gap limits how useful current prevalence estimates are for guiding public health planning. The SRMAs we reviewed also varied widely in their methods, especially in the screening tools and analytic techniques they used. For instance, differences in cut off thresholds for GDS-15, PHQ-9, or CES-D complicate cross-study comparisons [43]. These patterns align with Hu et al., who found that differences in screening tools significantly influence prevalence estimates and add to the variability from study to study [39].
Conclusion
This study represents one of the first systematic meta-reviews of systematic reviews and meta-analyses on global depression prevalence. By synthesizing 36 SRMAs conducted over the past decade, we provide a broad, integrative perspective on the global evidence base, highlighting both the most frequently studied regions and those consistently overlooked in depression research. A key contribution of this study is its ability to uncover structural and geographic gaps that are often missed in primary studies or conventional meta-analyses. In particular, we demonstrate that the overwhelming focus on Asia and clinical populations has come at the expense of attention to low-income regions such as Sub- Saharan Africa, and socially vulnerable groups such as informal workers, displaced persons, and those affected by economic shocks. These findings carry important implications for global depression policy. The current imbalance in data may distort global burden estimates and misinform the allocation of re- sources. Additionally, methodological inconsistencies across SRMAs such as differences in screening tools and quality assessments highlight the need for more standardized, trans- parent, and equity-focused research practices in global mental health. Future research should expand on this work by conducting region-specific meta-reviews, examining intersectional vulnerabilities, and connecting prevalence estimates to real world policy and program outcomes. Expanding global surveillance to include the voices and experiences of the underrepresented is not only a methodological necessity but a moral imperative in global mental health.
Policy Implications
The implications for global depression health policy are significant.
• First, the lack of data from low-income regions risks driving systematic underfunding and resource misallocation by global health agencies.
• Second, missing data on key demographic groups limits the ability to design tailored interventions and integrate mental health into universal health coverage systems.
• Third, our results highlight the need for stronger methodological standards in SRMAs especially in tool selection, heterogeneity reporting, and use of quality appraisal tools like AMSTAR-2. Funders and journals should prioritize reviews that explicitly consider policy translation, equity, and inclusion of marginalized populations.
Recommendations for Future Research
Future systematic reviews and meta-analyses should:
• Expand representation from under studied regions such as Sub-Saharan Africa, Latin America, and Australia.
• Include underrepresented populations such as working adults, informal laborers, and displaced individuals
• Use standardized instruments and cut-offs to enable global comparability.
• Include policy-relevant outcomes, such as risk factors, protective determinants, and access barriers
This study has several limitations that warrant consideration.
• First, the exclusion of non-English publications may have introduced a bias in geographic representation.
• Second, our analysis depended on the reporting quality of the included SRMAs. Because this quality varied widely, it limited our ability to ex- tract consistent quantitative effect sizes.
• Third, we did not conduct a pooled quantitative synthesis across SRMAs, as doing so would have required harmonizing outcome measures and screening tools a step that wasn’t feasible given the level of heterogeneity.
Given the well-established link between chronic stress and depression, it is crucial to develop targeted stress reduction strategies particularly for vulnerable groups such as student to help prevent the onset of depression [44,45].
Conflict of Interest and Funding Declaration
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper. This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
- World Health Organization (2022). Mental disorders.
- World Health Organization (2021). World mental health day 2021–key messages. Depression is a leading cause of disability worldwide and a major contributor to the overall global burden of disease.
- Korczak, D. J., Westwell-Roper, C., & Sassi, R. (2023). Diagnosis and management of depression in adolescents. Cmaj, 195(21), E739-E746.
- Wilhelm, M., Bauer, S., Feldhege, J., Wolf, M., & Moessner,M. (2024). Alleviating the burden of depression: a simulation study on the impact of mental health services. Epidemiology and Psychiatric Sciences, 33, e19.
- Aaron, R. V., Ravyts, S. G., Carnahan, N. D., Bhattiprolu, K., Harte, N., McCaulley, C. C., ... & Dudeney, J. (2025). Prevalence of depression and anxiety among adults with chronic pain: A systematic review and Meta-Analysis. JAMA Network Open, 8(3), e250268-e250268.
- Koskie, B. and Raypole, C. (2023). Depression statistics: Types, symptoms, treatments, more.
- Jiang, C. H., Zhu, F., & Qin, T. T. (2020). Relationships between chronic diseases and depression among middle- aged and elderly people in China: a prospective study from CHARLS. Current medical science, 40(5), 858-870.
- Aziz, R., & Steffens, D. C. (2013). What are the causes of late- life depression?. The Psychiatric Clinics of North America, 36(4), 497.
- Compton, W. M., Conway, K. P., Stinson, F. S., & Grant, B.F. (2006). Changes in the prevalence of major depression and comorbid substance use disorders in the United States between 1991–1992 and 2001–2002. American Journal of Psychiatry, 163(12), 2141-2147.
- Moreno-Agostino, D., Wu, Y. T., Daskalopoulou, C., Hasan,M. T., Huisman, M., & Prina, M. (2021). Global trends in the prevalence and incidence of depression: a systematic review and meta-analysis. Journal of affective disorders, 281, 235- 243.
- Bedaso, A., Mekonnen, N., & Duko, B. (2022). Estimate of the prevalence of depression among older people in Africa: a systematic review and meta-analysis. Aging & mental health, 26(6), 1095-1105.
- Patel, V., Saxena, S., Lund, C., Thornicroft, G., Baingana, F., Bolton, P., ... & Unützer, J. (2018). The Lancet Commission on global mental health and sustainable development. The lancet, 392(10157), 1553-1598.
- Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I.,Hoffmann, T. C., Mulrow, C. D., ... & Moher, D. (2021). The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. bmj, 372.
- Günhan, B. K., Friede, T., & Held, L. (2018). A designâ? byâ?treatment interaction model for network metaâ?analysis and metaâ?regression with integrated nested Laplace approximations. Research synthesis methods, 9(2), 179-194.
- Shea, B. J., Reeves, B. C., Wells, G., Thuku, M., Hamel, C., Moran, J., ... & Henry, D. A. (2017). AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. bmj, 358.
- Whiting, P., SavoviÄ?, J., Higgins, J. P., Caldwell, D. M., Reeves, B. C., Shea, B., ... & Churchill, R. (2016). ROBIS: a new tool to assess risk of bias in systematic reviews was developed. Journal of clinical epidemiology, 69, 225-234.
- Whiting, P., SavoviÄ?, J., Higgins, J. P., Caldwell, D. M., Reeves, B. C., Shea, B., ... & Churchill, R. (2018). ROBIS: a new tool to assess risk of bias in systematic reviews was developed. Recenti Progressi in Medicina, 109(9), 421-431.
- Brandenbarg, D., Maass, S. W., Geerse, O. P., Stegmann, M. E., Handberg, C., Schroevers, M. J., & Duijts, S. F. (2019). A systematic review on the prevalence of symptoms of depression, anxiety and distress in longâ?term cancer survivors: implications for primary care. European journal of cancer care, 28(3), e13086.
- Karami, N., Kazeminia, M., Karami, A., Salimi, Y., Ziapour, A., & Janjani, P. (2023). Global prevalence of depression, anxiety, and stress in cardiac patients: a systematic review and meta-analysis. Journal of Affective Disorders, 324, 175-189.
- Leung, D. K., Chan, W. C., Spector, A., & Wong, G. H. (2021). Prevalence of depression, anxiety, and apathy symptoms across dementia stages: a systematic review and metaâ?analysis. International journal of geriatric psychiatry, 36(9), 1330-1344.
- Matte, D. L., Pizzichini, M. M., Hoepers, A. T., Diaz, A. P., Karloh, M., Dias, M., & Pizzichini, E. (2016). Prevalence ofdepression in COPD: a systematic review and meta-analysis of controlled studies. Respiratory medicine, 117, 154-161.
- Riedl, D., & Schuessler, G. (2021). Prevalence of Depression and Cancer–A systematic review. Zeitschrift für Psychosomatische Medizin und Psychotherapie, 68(1), 74-86.
- Mata, D. A., Ramos, M. A., Bansal, N., Khan, R., Guille, C., Di Angelantonio, E., & Sen, S. (2015). Prevalence of depression and depressive symptoms among resident physicians: a systematic review and meta-analysis. Jama, 314(22), 2373- 2383.
- Pappa, S., Ntella, V., Giannakas, T., Giannakoulis, V. G., Papoutsi, E., & Katsaounou, P. (2020). Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Brain, behavior, and immunity, 88, 901-907.
- Pappa, S., Ntella, V., Giannakas, T., Giannakoulis, V. G., Papoutsi, E., & Katsaounou, P. (2021). Prevalence of depression, anxiety, and insomnia among healthcare workers during the covid-19 pandemic: A systematic review and meta- analysis”: Corrigendum,
- Ryttersgaard, T. O., Johnsen, S. P., Riis, J. Ø., Mogensen, P. H., & Bjarkam, C. R. (2020). Prevalence of depression after moderate to severe traumatic brain injury among adolescents and young adults: A systematic review. Scandinavian journal of psychology, 61(2), 297-306.
- Vibhakar, V., Allen, L. R., Gee, B., & Meiser-Stedman,R. (2019). A systematic review and meta-analysis on the prevalence of depression in children and adolescents after exposure to trauma. Journal of affective disorders, 255, 77-89.
- Farooqi, A., Gillies, C., Sathanapally, H., Abner, S., Seidu, S., Davies, M. J., ... & Khunti, K. (2022). A systematic review and meta-analysis to compare the prevalence of depression between people with and without Type 1 and Type 2 diabetes. Primary Care Diabetes, 16(1), 1-10.
- Boeschoten, R. E., Braamse, A. M., Beekman, A. T., Cuijpers, P., Van Oppen, P., Dekker, J., & Uitdehaag, B. M. (2017). Prevalence of depression and anxiety in multiple sclerosis: a systematic review and meta-analysis. Journal of the neurological sciences, 372, 331-341.
- Wang, J., Wu, X., Lai, W., Long, E., Zhang, X., Li, W., ...& Lin, H. (2017). Prevalence of depression and depressive symptoms among outpatients: a systematic review and meta- analysis. BMJ open, 7(8), e017173.
- Pilevarzadeh, M., Amirshahi, M., Afsargharehbagh, R., Rafiemanesh, H., Hashemi, S. M., & Balouchi, A. (2019). Global prevalence of depression among breast cancer patients: a systematic review and meta-analysis. Breast cancer research and treatment, 176(3), 519-533.
- Cai, H., Jin, Y., Liu, R., Zhang, Q., Su, Z., Ungvari, G. S.,... & Xiang, Y. T. (2023). Global prevalence of depression in older adults: a systematic review and meta-analysis of epidemiological surveys. Asian journal of psychiatry, 80, 103417.
- Heidari, M. E., Irvani, S. S. N., Dalvand, P., Khadem, M., Eskandari, F., Torabi, F., & Shahsavari, H. (2021). Prevalence of depression in older people with hipsystematic review and meta-analysis. International Journal of Orthopaedic and Trauma Nursing, 40, 100813.
- Tam, W., Lo, K., & Pacheco, J. (2019). Prevalence of depressive symptoms among medical students: overview of systematic reviews. Medical education, 53(4), 345-354.
- Tung, Y. J., Lo, K. K., Ho, R. C., & Tam, W. S. W. (2018).Prevalence of depression among nursing students: A systematic review and meta-analysis. Nurse education today, 63, 119-129.
- Akhtar, P., Ma, L., Waqas, A., Naveed, S., Li, Y., Rahman, A., & Wang, Y. (2020). Prevalence of depression among university students in low and middle income countries (LMICs): a systematic review and meta-analysis. Journal of Affective Disorders, 274, 911-919.
- Zhang, L., Fu, T., Yin, R., Zhang, Q., & Shen, B. (2017). Prevalence of depression and anxiety in systemic lupus erythematosus: a systematic review and meta-analysis. BMC psychiatry, 17(1), 70.
- Duko, B., Bedaso, A., & Ayano, G. (2020). The prevalence of depression among patients with tuberculosis: a systematic review and meta-analysis. Annals of general psychiatry, 19(1), 30.
- Hu, T., Zhao, X., Wu, M., Li, Z., Luo, L., Yang, C., & Yang, F.(2022). Prevalence of depression in older adults: A systematicreview and meta-analysis. Psychiatry research, 311, 114511.
- Assariparambil, A. R., Noronha, J. A., Kamath, A., Adhikari, P., Nayak, B. S., Shankar, R., & George, A. (2021). Depression among older adults: a systematic review of South Asian countries. Psychogeriatrics, 21(2), 201-219.
- Cutler, D. M., & Sportiche, N. (2022). Economic crises and mental health: Effects of the great recession on older Americans (No. w29817). National Bureau of Economic Research.
- Reeves, A., McKee, M., Gunnell, D., Chang, S. S., Basu, S., Barr, B., & Stuckler, D. (2015). Economic shocks, resilience, and male suicides in the Great Recession: cross-national analysis of 20 EU countries. The European Journal of Public Health, 25(3), 404-409.
- Krishnamoorthy, Y., Rajaa, S., & Rehman, T. (2020). Diagnostic accuracy of various forms of geriatric depression scale for screening of depression among older adults: Systematic review and meta-analysis. Archives of gerontology and geriatrics, 87, 104002.
- Hammen, C. (2005). Stress and depression. Annu. Rev. Clin. Psychol., 1(1), 293-319.
- Aipoh, G. (2016). Factor Analysis of Stress Level and its Impact on Student’s Academic Performance: Evidence from Edo State, Nigeria.




