Case Report - (2024) Volume 3, Issue 1
Management of Complex Calculi: Is Surgery Still Useful? Case report
Received Date: Feb 28, 2024 / Accepted Date: Mar 28, 2024 / Published Date: Apr 04, 2024
Copyright: ©© 2024 Anass Rhayour, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Anass, R., Jaafar, F., Ilyass, Z., Amine, S., Tarik, K., et al. (2024). Management of Complex Calculi: Is Surgery Still Useful? Case report. World J Clin Med Img, 3(1), 01-02.
Abstract
In recent decades, there has been a significant shift in the surgical management of renal lithiasis. Urologists face a therapeutic hurdle when treating coralliform calculi. The use of open or laparoscopic surgery has drastically decreased as a result of advancements in extracorporeal lithotripsy (ESWL), ureterorenoscopy (URS), and percutaneous nephrolithotomy (PCNL) in terms of minimally invasive access (flexible URS, combined techniques), energy (sonotrodes, and various types of laser), and technique. [1,2,3]. We report the case of a 70 years old female patient, who consulted for a simple right renal colic, the patient underwent an KUB radiography which found a calcium-toned opacity (Figure 1). We completed with and CT scan showing a dilatation du to complex lithiasis (89x23x33mm 1141 HU) (Figure 2).
Keywords
Urolithiasis, Laparoscopic Nephrolithotomy, Complex Calculi
Introduction
In recent decades, there has been a significant shift in the surgical management of renal lithiasis. Urologists face a therapeutic hurdle when treating coralliform calculi. The use of open or laparoscopic surgery has drastically decreased as a result of advancements in extracorporeal lithotripsy (ESWL), ureterorenoscopy (URS), and percutaneous nephrolithotomy (PCNL) in terms of minimally invasive access (flexible URS, combined techniques), energy (sonotrodes, and various types of laser), and technique. [1,2,3]. We report the case of a 70 years old female patient, who consulted for a simple right renal colic, the patient underwent an KUB radiography which found a calcium-toned opacity (Figure 1). We completed with and CT scan showing a dilatation du to complex lithiasis (89x23x33mm 1141 HU) (Figure 2).
Abbreviations
PCNL: Percutaneous nephrolithotomy ESWL: Extrocorporeal Shock Wave Lithotripsy URS: Ureterorenoscopy HU: Hounsfield Unit The decision was a laparoscopic pyelolithotomy. Post-operative recovery was straightforward, with the removal of the JJ stent after 2 weeks (Figure 3). We therefore highlight that open or laparoscopic surgery is still a valuable tool in the surgeon's toolbox, even though its use has decreased. Laparoscopic or even open removal of stones represents less than 5% of the management techniques still used for urolithiasis [4]. Despite advances in minimally invasive endo-urological techniques, surgical management, whether open or laparoscopic, still has its place in the management of complex calculi [5].
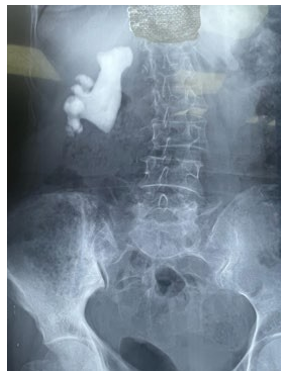
Figure 1: KUB radiography showing and calcium toned stones
Figure 2: CT showing a complexe calculi 89x23x33 1141 HU
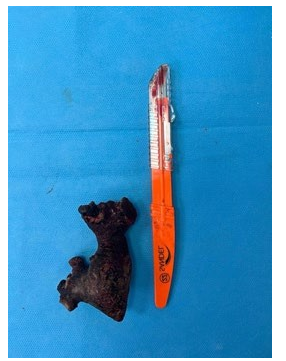
Figure 3: Postoperative picture of the calculi
References
- Saussine, C., Lechevallier, E., & Traxer, O. (2008). Coral stones or complex stones: surgical treatment. Advances in Urology , 18 (12), 966-971.
- Carpentier, X., Meria, P., Bensalah, K., Chabannes, E., Estrade, V., Denis, E., ... & Traxer, O. (2014). Update on the management of kidney stones in 2013. Lithiasis Committee of the French Urology Association. Advances in Urology , 24 (5), 319-326.
- Lunardi, P., Timsit, M. O., Roumiguie, M., Dariane, C., N’Guyen, K., Beauval, J. B., & Leroux, S. (2015). Traitement en un temps de la lithiase rénale complexe : à propos d’une série moderne de néphrotomies bivalves. Progrès En Urologie, 25(2), 90–95.
- Holmes, S. A. V., & Whitfield, H. N. (1991). The current status of lithotripsy. British journal of urology, 68(4), 337-344.
- Sohrabi, C., Mathew, G., Maria, N., Kerwan, A., Franchi, T., & Agha, R. A. (2023). The SCARE 2023 guideline: updating consensus Surgical CAse REport (SCARE) guidelines. International Journal of Surgery, 109(5), 1136-1140.



