Case Report - (2025) Volume 3, Issue 1
Lipoplastic Lymphadenopathy: A Rare Cause for Generalized Lymphadenopathy
2Professor of Pathology, Tanta University, Egypt, Consultant Pathology, Pure Health, United Arab Emirates
Received Date: Dec 26, 2024 / Accepted Date: Jan 24, 2025 / Published Date: Feb 21, 2025
Copyright: ©Â©2025 Ramadan Fouad Arafa, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Arafa, R. F., Elbarkouky, A. (2025), Lipoplastic Lymphadenopathy: A Rare Cause for Generalized Lymphadenopathy, Trans Med OA, 3(1), 01-03.
Abstract
Lipoplastic lymphadenopathy (also called lipolymph) is a histopathological benign condition in which there is excess ectopic adipose tissue in the lymph node causing its enlargement. We present a 30-year-old man with no past medical history of note, admitted with pallor, easy bruises, and fatigue. He has iron deficiency anemia. He has also generalized lymphadenopathy. Computed Tomography (CT) of the chest, abdomen, and pelvis with IV contrast showed generalized low attenuation lymph nodes. Excisional biopsy was done to exclude hematological malignancy which was diagnosed as lipoplastic lymphadenopathy. He was managed with intravenous iron and packed red blood cell (PRBCs) transfusion and discharged in a stable condition.
Keywords
Generalized Lymphadenopathy, Lipoplastic Lymphadenopathy, Low Attenuation Lymphadenopathy
Introduction
Lipoplastic lymphadenopathy is a rare benign pathological condition characterized by abnormal accumulation of fat in the lymph node causing its enlargement [1]. This condition had been reported as a pulmonary nodule , in cervical lymph nodes, disseminated generalized lymph nodes, ovaries, and retroperitoneal lymph nodes [2-4]. Lipoplastic lymphadenopathy is of unclear etiology, but obesity, gender, age, and previous inflammation are considered to be related to their occurrence [1,5]. It appears in computerized tomography as low attenuated enlarged lymph nodes and should be differentiated from other causes of lymphadenopathy like cavitating tuberculous lymphadenopathy, celiac disease, lymphoma or metastatic malignancies [6].
Case Report
A 29-year-old male was admitted with severe anemia and ecchymosis in both legs for evaluation. He has easy bilateral leg bruising for the last 2 months. No history of trauma, or bleeding from anywhere. He denies any alcohol, smoking or drug abuse. No comorbid conditions.
Systemic examination was unremarkable except for marked pallor, bilateral leg ecchymotic patches, and enlarged axillary lymph nodes more in right side.
Laboratory Investigations
White blood cell count 4.22 x 103/µL, Hemoglobin 6.7 gm/dL, Platelet 342 x 103/µL. Blood film showed marked hypochromic anemia with anisocytosis suggestive of iron deficiency anemia. Renal function and liver function tests were normal except for hypoalbuminemia 19 gm/L. C-reactive protein 65 mg/dL, ESR 92 mm/hr.
Anemia profile showed very low iron, and normal ferritin, vitamin B12 and folate levels. LDH is normal. HIV is negative. Faecal immunochemical test and stool occult blood are negative. Ultrasound abdomen multiple paraaortic and porta hepatis malignant – looking enlarged lymph nodes suggestive of malignant lymphadenopathy.
CT neck, chest, abdomen, and pelvis with IV contrast (Figure 1) showed multiple variable sized peripherally enhanced with hypodense centre enlarged (low attenuated) lymph nodes seen involving superior mediastinum (A), porta hepatis (B), superior mesenteric (C), and para-aortic lymph nodes. Figure 2 showed enlarged retroperitoneal lymph nodes suggestive of tuberculosis or leukemia.
Right axillary lymph node excisional biopsy was done. The excised lymph node is about 1.3 x 1 x 1 cm with surrounded fatty tissue. The cut section shows central yellowish area. Histopathological examination revealed histomorphology of benign reactive lymph nodes with diffuse ectopic fatty infiltration of lymph nodes consistent with lipoplastic lymphadenopathy (Figure 3).
He was given 2 units packed red blood cells (PRBCs), post transfusion Hb 9.1 gm/dL. He was discharged home with advice regarding oral iron and follow up.
Discussion
Lipoplastic lymphadenopathy is a rare benign pathologic disease characterized by enlarged lymph nodes with lower attenuation due to abnormal accumulation of benign mature fat [1]. It may be radiologically misdiagnosed as malignant either primary like lymphoma or metastatic, tuberculous, fungal, or cavitating disease [6]. Excisional biopsy and histopathologic examination are essential to confirm the diagnosis. There is no known etiology for lipoplastic lymphadenopathy, but it may be linked to obesity, gender, age, and previous inflammation may be linked to its occurrence [1]. it may also be linked to thyroid diseases and diabetes [7].
Iron deficiency anemia and hypoalbuminemia were attributed to nutritional deficiency.
In several case reports and case series, lipoplastic lymphadenopathy causes single group of lymph node enlargement or a single nodule in the pelvis or lung [1-6]. To our knowledge, our patient is the first reported case of lipolymph-induced generalized lymphadenopathy.
Our reported case has severe iron deficiency anemia and hypoalbuminemia. He has negative stool occult blood and fecal immunochemical tests which exclude gastrointestinal bleeding. The link between lipoplastic lymphadenopathy and iron deficiency anemia is not clear. It may be accidental association, but it needs further work up.
Summary and Recommendations
Lipoplastic lymphadenopathy is a rare disease caused by abnormal accumulation of fat in the lymph nodes. It should be differentiated from other causes of lymphadenopathy especially malignancy, infections, and glycogen storage disease.
We reported a 29-year-old gentleman presented with generalized lymphadenopathy and severe iron deficiency anemia. Lymph node excisional biopsy was done to detect the diagnosis especially lymphoma. The Histopathologic examination was consistent with lipoplastic lymphadenopathy. We attributed iron deficiency to dietary causes.
Up to our knowledge, it is the first reported case of generalized lymphadenopathy due to lipoplastic lymphadenopathy.
Although lipoplastic lymphadenopathy is a rare disease but it should be considered in the differential diagnosis of lymphadenopathy. We recommend further work up to detect any possible link between iron deficiency and lipoplastic lymphadenopath
Figure 1: Computed Tomography of the Chest and Abdomen with IV Contrast Showing Enlarged Mediastinal Lymph Node (A), Porta Hepatis Lymph Node (B), Superior Mesenteric Lymph Nodes (C) and para-aortic Lymph Nodes (D).
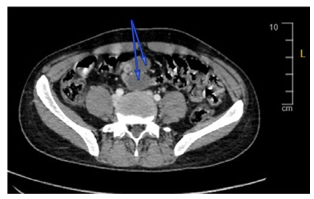
Figure 2: Computed Tomography (CT) of the Abdomen Showing Enlarged Retroperitoneal Lymph Nodes (arrows).
Figure 3: Histopathology of Lymph node Showing diffuse fatty Infiltration Occupies Most of Lymph Node (hematoxylin and eosin stain,x 100)
Acknowledgement
We acknowledge and appreciate the generous support and great help from Dr. Talaat Algammal, MD consultant radiology for preparing radiology Figures.
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose
References
- Huang, Y., Huang, K., Fan, M., Jiang, L., Zhu, D., & Zhou, Q. (2021). Lipolymph node presenting as a pulmonary nodule: A case report. Thoracic Cancer, 12(6), 993-994.
- Parsons, C. A., & King, D. M. (1982). Disseminated lipoplastic lymphadenopathy. The British Journal of Radiology, 55(655), 535-536.
- Fairey, R., Worth, A., & Gustafson, R. C. (1987). Lipoplasticlymphadenopathy presenting as an ovarian mass: a case report. Gynecologic oncology, 28(3), 345-351.
- Manning, L. G., Pischinger, R. J., & Bobroff, L. M. (1975). Lipoplastic lymphadenopathy simulating malignant lympho- ma and pelvic lipomatosis: Report of a case and review of the literature. The Journal of Urology, 114(5), 788-790.
- Balakrishna J. Adipose tissue. PathologyOutlines.com web- site. https://www.pathologyoutlines.com/topic/lymphnode- sadiposetissuemetaplasia.html. Accessed February 14th, 2024.
- Bashir U, Hajihashemi A, Yap J, et al. Low attenuation lymph- adenopathy. Reference article, Radiopaedia.org (Accessed on 09 Mar 2024)
- Giovagnorio, F., Drudi, F. M., Fanelli, G., Flecca, D., & Francioso, A. (2005). Fatty changes as a misleading factor in the evaluation with ultrasound of superficial lymph nodes. Ultrasound in medicine & biology, 31(8), 1017-1022.



