Research Article - (2025) Volume 1, Issue 1
Isolation and Identification of Bacteria from Suya Meat Sold at Gwagwalada Market
Received Date: Mar 07, 2025 / Accepted Date: Apr 18, 2025 / Published Date: Apr 23, 2025
Copyright: ©�2025 J. C. Ogbu, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Olarinoye Blessed Mubarak, B. O. Akanbi, J. C. Ogbu and Jimba R. A. (2025). Isolation and identification of bacteria from Suya meat sold in Gwagwalada Market. Arch Cienc Investig, 1(1), 01-05.
Abstract
Suya, a popular Nigerian street food and accessible protein source is a significant public health risk due to potential bacterial contamination. The aim of this study was to investigate the microbial contamination of suya meat sold at Gwagwalada Market, focusing on the isolation and identification of bacterial species. Twenty (20) Samples were collected from multiple vendors and analyzed for total bacterial counts (TBC) and total coliform counts (TCC). Samples were plated using spread plate method on media agar and incubate at 37o C for 24 hours. The TBC ranged from 2.2 x108 to 3.2 x 108 CFU/g while the total coliform count ranged 1.8x106 to 2.9x106 , exceeding acceptable limits for ready-to-eat foods. Three bacterial species were identified: Staphylococcus aureus (30.0%), Bacillus subtilis (22.5%), Pseudomonas aeruginosa (20.0%), Klebsiella pneumoniae (15.0%), and Escherichia coli (12.5%). The findings highlight significant hygiene and safety concerns due to poor handling practices, environmental contamination, and inadequate storage conditions and thus recommends the need for stricter hygiene regulations, vendor training, and consumer awareness to ensure the safety of suya meat and reduce potential public health risks.
Introduction
Suya is a popular grilled meat snack that originated from northern Nigeria and has become a widely cherished delicacy across the country and beyond [1]. Traditionally made from thin slices of beef, goat, or chicken, Suya is seasoned with a blend of spices, which often includes groundnut powder, ginger, pepper, and various seasonings, imparting a distinctive flavor and aroma to the meat [2]. The meat is usually marinated, skewered on sticks, and then grilled over an open flame, resulting in a unique smoky flavor and tender texture [3]. Suya is commonly prepared and sold by street vendors in various cities and towns, making it a major component of Nigerian street food culture [4]. However, due to its method of preparation and the conditions in which it is sold, Suya is often exposed to environmental contaminants, which can compromise its safety and quality. Studies indicate that contamination can arise from various sources, including handling by vendors, poor hygiene practices, and exposure to dust and flies during display and sale [5]. One significant health concern related to Suya consumption is bacterial contamination, especially from pathogens such as Escherichia coli and Staphylococcus spp. [3]. These bacteria can be introduced through improper handling, unsanitary preparation surfaces, and inadequate cooking temperatures (Ifeanyi et al., 2020). According to Musa and Awogbemi, the consumption of contaminated Suya poses serious health risks, including foodborne illnesses, particularly in individuals with compromised immune systems. Moreover, several studies have highlighted the importance of regulatory oversight in ensuring the safety of Suya meat [1]. Health authorities advocate for periodic training and sensitization of street food vendors to improve hygiene practices and food safety standards [1]. The implementation of these practices could significantly reduce contamination risks and enhance consumer health. Suya meat provides nutritional value as it is a rich source of protein and essential nutrients, although its fat content can vary based on the type of meat used [4]. Despite the risks associated with its preparation and sale, Suya remains a culturally significant food with high demand, particularly for its convenience, affordability, and unique flavor profile [5].
Materials & Methods
Study Area
The study was conducted at the University of Abuja, located in Gwagwalada, Federal Capital Territory (FCT): Nigeria. Geographically, the University of Abuja is located between latitude 9.0765o N and longitude 7.3986oE. In terms of its physical space, the University covers an area of approximately 11,824 hectares (29,181 acres) and it is situated on the plains of the Guinean savannah in central Nigeria [6].
Sample Size
The number of samples collected for this research work was twenty (20), this was collected randomly from Suya vendors around different vending locations at Gwagwalada local market with no emphasis on any special recommendation to be eligible as a sample donor.
Sample Collection
A total of twenty (20) Suya samples were collected from different vendors at Gwagwalada local market. These samples were transported in sterile polyethylene bags to the Microbiological Laboratory at the University of Abuja and processed within 3 – 5 hours for microbial analysis.
Sample Preparation
Upon arrival at the laboratory, the samples were prepared following standard microbiological procedures for bacterial isolation. A 10-gram portion of each sample was weighed and mixed with 90 mL of buffered peptone water, then serially diluted to obtain various concentrations for analysis, followed by serial dilution for subsequent microbiological analyses [7]. These prepared samples were then plated on selective media appropriate for isolating common bacteria in meat products, such as E. coli, Staphylococcus aureus, and Salmonella spp., and incubated under suitable conditions to encourage bacterial growth.
Materials and Reagents
Sterile containers, sampling bags, Nutrient agar, MacConkey Agar and Salmonella Shigella agar, Petri dishes, microscopic slides, cover slips, test tubes, buffered peptone water, distilled water, hydrogen peroxide (H2O2) and sterile pipettes.
Preparation of Media
All media were prepared following the manufacturer’s protocol. Media used included Nutrient agar, MacConkey Agar and Salmonella Shigella agar. They were autoclaved at 121oC for 15 minutes. The cooled media was poured into Petri dishes and then allowed to cool and solidify. These was used for the isolation, identification, growth and maintenance of microorganisms.
Serial Dilution
Six (6) test tubes were used, 9ml of distilled water was poured into each test tube using a syringe that was sterilized in between by putting the needle over a Bunsen burner and waving it gently to reduce the heat. One gram (1g) of each of the already finely crushed Suya samples were poured into the first test tube (10-1): the test tube is swirled gently to enable the distilled water and the sample mix properly. One ml (1 ML) of the mixture was taken from the test tube and added to the next test tube (10-2) another one ml (1 ML) was taken from the second test tube and subsequently added to the last test tube (10-6) [8].
Spread Plate Method
The sterilized Nutrient agar was poured into three Petri dishes and left to solidify. Using a syringe, 0.1 ML of the sample in the test tubes were dispensed onto the agar plates which was labelled 10-1, 10-2 and 10-3 respectively. A glass rod was sterilized by passing it through a flame and moving it back and forth. The glass rod was left to cool down for a few seconds, then it was used to gently spread the sample on the top of the agar plate evenly which helps to improve the growth of individual colonies. The agar plates were kept in the incubator at 37 Degree Celsius and was observed after 24 hours [8].
Microbial Load Count
After 24 hours, the media plates were removed from the incubator and observed for bacteria and coliforms. Colonies (between 30 and 100) were counted and noted. Colonies observed in the both NA plates and MacConkey plates were noted.
Gram Staining Test
A loopful of sterile distilled water was be dropped on a clean grease free slide by using a sterile inoculating loop after which an inoculum from the culture was mixed with the water on the slide. The smear was allowed to air dried and then heat fixed gently by passing it quickly over a Bunsen flame. The smear was flooded with crystal violet solution for 60 seconds (one minutes) and rinsed with water. The smear was flooded with Lugol’s iodine for 30 seconds and rinsed with water, 70% alcohol was poured on the slides for 15 seconds until the crystal violet had been completely will washed off. It was then counterstained with Safranin for 60 seconds and allowed to dry. The slides were then observed under oil immersion objective. Gram-positive cells remained purple while Gram negative appeared red or pink.
Biochemical Tests
Catalase Test
A drop of hydrogen per oxide was put on a glass slide. Colonies were picked with a sterile loop and added to the drop. Observation was made for bubble production. Colonies that have catalase can break down hydrogen peroxide into water and oxygen, which can be seen in the form of air bubbles leaving the solution.
Citrate Test
Citrate test was done was unique colonies where picked with a sterilized loop and streaked across the plates containing citrate media without breaking the agar and then incubated for 24 hours. Data was collected based on color change.
Methyl Red Test
Five millimeters of glucose phosphate broth (1g glucose, 0.5% KH2PO4, 0.5% peptone and 100 mL distilled water) was dispensed into clean test tube and sterilized. The tube was then inoculated with the isolates and incubated at 37°C for 48 hours. At the end of incubation, few drops of methyl red solution was added. This were repeated for each isolate and color change was observed. A red color indicates a positive reaction.
Oxidase Test
This test was done by dropping 2–5 drops of a freshly prepared oxidase (paminodimethylanine) reagent on a filter paper, the suspected organism is picked using a sterile wire loop and mix with the oxidase reagent. This were repeated for each isolates. A change from the normal color to deep purple means a positive result, while no change means negative.
Coagulate Test
About 2 drops of normal saline was added on a grease free slide then using sterile inoculating loop an isolate was taken and emulsified on it. And a drop of plasma was then adding and rocked. This were repeated for each isolates. Presence of agglutination means a positive result while no agglutination means a negative results.
Indole Test
The isolate was inoculated in a test tube containing 3mL of sterile tryptone water. It was then incubated at 37oC for 24 hours. The test for indole was done by adding 0.5mL of kovac’s reagent and shaken gently. Then it was examined for a color change. Examination for a red color in the surface of the layer within 10 minutes means positive, while no color change means negative.
Results
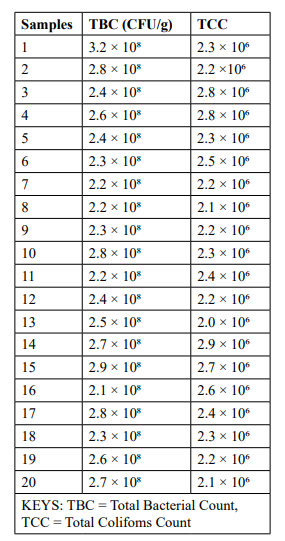

Table 1: Colony Forming Units of Bacterial Isolates (CFU/g)
|
Isolate |
GR |
Shape |
Color |
Edge |
Elevation |
Surface Optical |
Suspected Organism |
|
A |
+ |
Rod |
White |
Flat |
Rough |
Translucent |
Bacillus subtilis |
|
B |
- |
Rod |
Colorless |
Flat |
Rough |
Translucent |
Escherichia coli |
|
C |
- |
Rod |
Blue |
Flat |
Smooth |
Opaque |
Pseudomonas aeruginosa |
|
D |
- |
Rod |
Pink |
Convex |
Smooth |
Opaque |
Klebsiella pneumoniae |
|
E |
- |
Cocci |
Cream |
Raised |
Smooth |
Opaque |
Staphylococcus aureus |
|
KEYS: GR= Gram Reaction, A= Isolate one, B= Isolate two, C= Isolate three |
|||||||
Table 2: Morphological and Cultural Characteristics of Bacterial Isolates
|
Isolate |
IN |
CA |
MR |
CI |
OX |
CO |
Probable Organism |
|
A |
- |
+ |
- |
+ |
+ |
- |
Bacillus subtilis |
|
B |
+ |
+ |
+ |
- |
- |
- |
Escherichia coli |
|
C |
- |
+ |
- |
- |
+ |
- |
Pseudomonas aeruginosa |
|
D |
- |
+ |
- |
+ |
- |
- |
Klebsiella pneumoniae |
|
E |
- |
+ |
+ |
+ |
- |
+ |
Staphylococcus aureus |
|
KEYS: IN: Indole test, CA: Catalase test, MR: Methyl Red test, CI: Citrate utilization test, OX: Oxidase test, CO: Coagulase test |
|||||||
Table 3: Biochemical Tests of Probable Organisms
|
Vendor |
Number of Samples |
Isolate |
Frequency |
|
1 |
2 |
Bacillus subtilis |
1 |
|
Escherichia coli |
1 |
||
|
Staphylococcus aureus |
2 |
||
|
2 |
2 |
Bacillus subtilis |
1 |
|
Escherichia coli |
1 |
||
|
Klebsiella pneumoniae |
2 |
||
|
3 |
2 |
Bacillus subtilis |
1 |
|
Pseudomonas aeruginosa |
1 |
||
|
Staphylococcus aureus |
2 |
||
|
4 |
2 |
Bacillus subtilis |
1 |
|
Escherichia coli |
1 |
||
|
Staphylococcus aureus |
2 |
||
|
5 |
2 |
Bacillus subtilis |
1 |
|
Klebsiella you |
1 |
||
|
Pseudomonas aeruginosa |
2 |
||
|
6 |
2 |
Bacillus subtilis |
1 |
|
Escherichia coli |
1 |
||
|
Staphylococcus aureus |
2 |
||
|
7 |
2 |
Klebsiella pneumoniae |
1 |
|
Pseudomonas aeruginosa |
1 |
||
|
Staphylococcus aureus |
2 |
Table 4: Distribution of Microbial Isolates
|
Bacterial Isolates |
Frequency of occurrence |
Percentage (%) |
|
Bacillus subtilis |
9 |
22.5 |
|
Escherichia coli |
5 |
12.5 |
|
Klebsiella pneumoniae |
6 |
15.0 |
|
Pseudomonas aeruginosa |
8 |
20.0 |
|
Staphylococcus aureus |
12 |
30.0 |
|
Overall Total |
40 |
100 |
Table 5: Frequency of Occurrence of Microbial Isolates from Suya
Discussion
Suya is a traditional Nigerian street meal that is consumed by many people, particularly in cities, where it is an easily accessible protein source. This study was aimed at investigating the presence of bacteria in Suya meat sold at the Gwagwalada Market. The bacterial isolates identified in this study, including Staphylococcus aureus (30.0%), Bacillus subtilis (22.5%), Pseudomonas aeruginosa (20.0%), Klebsiella pneumoniae (15.0%), and Escherichia coli (12.5%). The study also revealed a significant microbial load in suya meat sold at Gwagwalada Market, with total bacterial counts (TBC) ranging 2.2 x108 to 3.2 x 108 CFU/g while the total coliform count ranged 1.8x106 to 2.9x106. This aligns with findings from similar studies on street-vended meat products, which often highlight the potential public health risks posed by high bacterial counts [9]. The presence of Bacillus subtilis, Pseudomonas aeruginosa, and Staphylococcus aureus as the predominant bacterial isolates further supports the assertion that poor hygiene practices during processing and handling contribute significantly to contamination [10]. Staphylococcus aureus, which accounted for 30.0% of the isolates, is often associated with foodborne illnesses and is a common contaminant in ready-to-eat foods due to human contact [11]. The detection of Escherichia coli and Klebsiella pneumoniae emphasizes the risk of fecal contamination and potential pathogenicity. Emmanuel et al. highlighted similar findings, identifying E. coli as a major contaminant in street- vended suya and attributing its presence to the use of contaminated water for washing utensils and hands during preparation. These bacteria are indicators of fecal contamination and pose a risk for diarrheal diseases and urinary tract infections. The presence of pathogenic bacteria like Staphylococcus aureus, Escherichia coli, and Klebsiella pneumoniae highlights the potential health risks associated with consuming contaminated suya. According to WHO (2023), RTE foods contaminated with pathogens can lead to outbreaks of foodborne diseases, particularly in developing countries where monitoring and enforcement of food safety standards are inadequate. Interestingly, Bacillus subtilis had the frequency of occurrence (22.5%). While it is generally considered non-pathogenic, its presence in such high quantities may indicate environmental contamination or improper storage conditions, as Bacillus subtilis thrives in poorly sanitized environments. Additionally, Pseudomonas aeruginosa, with a frequency of 20.0%, is a known spoilage organism and opportunistic pathogen, suggesting that the suya might have been exposed to water or equipment that was not properly sanitized [12]. The microbial counts observed in this study exceed acceptable limits for ready- toeat foods, as prescribed by international standards such as the Food and Agriculture Organization (FAO). This raises serious concerns about the safety of suya sold at Gwagwalada Market. Similar studies on suya and other street-vended foods have reported comparable levels of contamination, often attributing them to inadequate vendor education, unhygienic practices, and environmental factors such as exposure to dust and flies [13]. It is worth noting that the high total coliform counts observed in this study suggest fecal contamination, which may arise from the use of contaminated water or improper waste disposal near the vending sites. Previous research has shown a strong correlation between coliform counts and the presence of enteric pathogens in street vended foods, which poses a significant risk to public health [14]. This study highlights the urgent need for improved hygiene standards and monitoring mechanisms for street-vended foods in Gwagwalada.
Conclusion
The study reveals a significant level of microbial contamination, with total bacterial counts exceeding acceptable limits for ready- to-eat foods. The identification of Bacillus subtilis, Staphylococcus aureus, and Pseudomonas aeruginosa emphasizes the potential health risks posed by the consumption of improperly handled or stored suya. The high frequency of these bacterial isolates highlights the role of poor hygiene, inadequate vendor practices, and environmental contamination in compromising food safety. Addressing these challenges requires stringent regulatory enforcement, improved vendor hygiene training, and consumer education on food safety practices. Implementing these measures will ensure the production of safer street-vended foods, thereby protecting public health and enhancing food security [15].
References
- Yakubu, B., & Emeka, P. E. (2022). Campylobacter and Listeria contamination in meat: A public health perspective.Nigerian Journal of Food Microbiology, 13(1), 92–105.
- Musa, O., & Awogbemi, A. (2020). Microbiological analysis of Suya meat in Nigeria. African Journal of Microbiology Research, 8(4), 90–96.
- Adeyemi, O., & Adesiyan, A. (2019). Hygiene practices and food safety measures of street vendors in Nigeria. Journal of Food Safety, 5(2), 123–130.
- Akinola, S. A., Bello, J. R., & Olatunji, T. M. (2021). Nutritional and microbiological assessment of street-vended Suya in Nigeria. Nigerian Journal of Nutritional Science, 19(1), 75–83.
- Chukwuma, J., Okechukwu, N., & Oluwole, I. (2017). Food safety challenges in Nigerian street food sector. African Journal of Public Health, 12(3), 89–97.
- University of Abuja. (2015). Postgraduate handbook.
- Salter, R. S., Durbin, G. W., Martinez, D., Bird, P., Bastin, B., & Crowley, E. (2020). AOAC-OMA/MicroVal harmonized validation of Peel Plate™ EB (Enterobacteriaceae bacteria): First Action 2018.05. Journal of AOAC International, 103(6), 1588–1603.
- Cheesbrough, M. (2020). District laboratory practice in tropical countries: Part 2. Cambridge University Press.
- Ologhobo, A. D., Olayemi, A. B., & Ogunseye, T. J. (2020). Assessing microbial hazards in ready-to-eat meat products: A Nigerian perspective. Food Control, 23(3), 429–435.
- Emmanuel, O. M., Adewale, O. B., & Funke, R. A. (2020). Isolation and identification of bacteria in street-vended suya in Abuja, Nigeria. African Journal of Microbiology Research, 14(3), 85–91.
- Adebayo, A., & Oladipo, S. (2018). Bacterial contamination in ready-to-eat street-vended foods: Implications for food safety. Journal of Public Health Research, 7(3), 45–52.
- Obi, C. N., & Eke, O. S. (2021). Environmental and hygienic factors influencing microbial contamination in street-vended foods. International Journal of Hygiene and Food Safety, 19(1), 1–8.
- Eze, C. U., Adekunle, A. O., & Adesanya, T. A. (2020). Microbial quality of suya meat sold in street markets: A case study. African Journal of Food Science, 14(5), 178–186.
- Okeke, A. C., Nwankwo, I. O., & Ugwuanyi, J. K. (2017). Total coliform counts as an indicator of fecal contamination in street foods. Nigerian Journal of Microbiology, 35(2), 65–72.
- Ifeanyi, C. I., Obi, C. N., & Akindele, M. O. (2020). Bacterial contamination and food safety in Nigerian delicacies. Food Microbiology, 45(3), 210–218.