Research Article - (2023) Volume 2, Issue 1
Impact of Direct or Indirect Transfer on Acute Type A Aortic Dissection in The Tokai Region of Japan
2Department of Emergency and Critical Care Medicine, Aichi, Medical University Hospital, 1-1 Yazako Karimata, Nagakute, Aichi, Japan
Received Date: Oct 11, 2023 / Accepted Date: Nov 29, 2023 / Published Date: Dec 14, 2023
Copyright: ©Â©2023 Kayo Sugiyama, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Sugiyama, K., Watanuki, H., Tochii, M., Kuge, Y., Koiwa, D., et al. (2023). Impact of Direct or Indirect Transfer on Acute Type A Aortic Dissection in The Tokai Region of Japan. J Surg Care, 2(1), 71-78.
Abstract
Objectives: To evaluate the outcomes of direct versus indirect transfer in treating acute type A aortic dissection (ATAAD) and assess the outcomes of patients transferred from tertiary versus non-tertiary hospitals.
Materials and MethodsThis study included 98 patients with ATAAD who underwent emergency surgery at our hospital from August 2015 to July 2023. We compared patients transferred directly to our hospital for emergency surgery with those transferred to other hospitals before ours.
Results Patients transferred from other hospitals had a significantly longer time from disease onset to arrival at the hospital and arrival in the operating room. However, they had a good preoperative condition, shorter postoperative hospital stay, lower major adverse cardiac or cerebrovascular events, and lower late mortality. Preoperative patient pathology or postoperative course among them showed no significant differences, regardless of whether the patient was transferred from a non-tertiary hospital.
Conclusions Patients transferred from other hospitals had better outcomes, most likely because they were relatively low-risk; high-risk cases might not have been efficiently transferred. The size of the referring hospital was not associated with the prognosis. Developing a network system in the Tokai region to efficiently transfer high-risk patients with acute aortic syndrome is warranted.
Keywords
Acute Type A Aortic Dissection, Acute Aortic Syndrome, Time from Onset to Arrival at The Hospital, Time from Onset to Arrival at The Operating Room, Tertiary Hospital
Introduction
The interval between symptom onset, diagnosis, and surgery has a significant impact on mortality in patients with acute type A aortic dissection (ATAAD) [1]. There have been reports of higher life-saving rates associated with early transfer, diagnosis, and treatment of patients [2,3]. Therefore, promising approaches to reduce treatment delays have been reported [3,4]. Matthew et al. demonstrated that surgical intervention within 4 h of diagnosis leads to significantly better outcomes; ATAAD must continue to be considered a time-sensitive emergency, and steps must be taken to expedite the surgery [1]. Transfers from other hospitals are expected to take longer than directly transferred cases. However, few reports have described the relationship between prognosis and transfer strategies in acute aortic syndrome.
However, reports have shown that improved diagnostic techniques and urgent care have only a marginal impact on early mortality, that is, patients with more severe conditions, such as typical symptoms, pulse loss, cardiac tamponade, and shock, undergo surgery earlier than other patients, whereas treatment of minor cases tends to be delayed [5,6]. Patients without typical symptoms or a sense of severity tend to experience delayed transfer; however, such patients survive. As a result, it has been reported that patients who are transferred earlier have poorer postoperative outcomes [7]. Furthermore, patients who died at a transfer facility or en route were not recorded. Therefore, patients who reached the facility alive had already undergone an element of selection [8].
It is also important to consider whether the referral source is a non-tertiary hospital [3]. In this study, we compared the outcomes of patients referred from other hospitals with those who visited our hospital directly. In addition, we compared the outcomes of patients referred from tertiary hospitals with the outcomes of those referred from non-tertiary hospitals.
Materials and Methods
A total of 118 patients who presented with ATAAD at our institution between August 2015 and August 2022 were included in this single-center retrospective study. Twenty patients were excluded from the analysis if the presenting/diagnostic or surgical times were not available. Patients who died before arriving at our hospital or the operating room were excluded from the present study. Ninety-eight patients with ATAAD who underwent emergency surgery were included in this study. We compared patients who were transferred directly to our hospital for emergency surgery (41 patients, 42%) with those who were transferred from other hospitals after diagnosis (57 patients, 58%).
The diagnosis of ATAAD was confirmed using contrast-enhanced computed tomography (CT) at our hospital or previous hospitals. On confirmation of an AAD, the recommended medications (labetalol or esmolol) are administered to achieve the desired parameters (systolic blood pressure 100–120 mmHg) according to the protocol recommended by Harris et al [9]. Preoperative CT imaging was used to determine the extent of dissection, location of the entry tear, and potential organ malperfusion. Other data on patient demographics and comorbidities (hypertension, smoking history, chronic respiratory disease, chronic renal disease requiring hemodialysis, history of coronary artery disease, history of cerebrovascular disease, family background, and family history of aortic dissection) were recorded. Coronary artery disease was defined as a history of coronary revascularization. Cerebrovascular disease was defined as permanent neurological dysfunction. The German Registry for Acute Aortic Dissection Type A (GERAADA) score is a simple and effective tool for predicting the 30-day mortality rate of patients undergoing surgery for ATAAD [10-13].
The time from onset to arrival at the hospital and the time from onset to arrival at the operating room were calculated. The symptom onset time was defined by each patient’s subjective reports as recorded in their medical records. The time of arrival at the hospital was defined as the timestamp of entry into the emergency department. Perioperative parameters, including operation time, cardiopulmonary bypass time, aortic cross-clamp time, cerebral perfusion time, circulatory arrest time, and minimal body temperature, were assessed. Early outcomes included early mortality, cause of death, and other complications during hospitalization.
Aichi Medical University Hospital is a tertiary hospital with existing relationships with a large number of rural and community hospitals in the Tokai region of Japan. The Tokai region is located almost in the middle of the Japanese Archipelago, covering Shizuoka, Aichi, and Mie prefectures, and the southern part of Gifu Prefecture. Nagoya City, the capital of Aichi Prefecture, is the most important city in the region, with a population of approximately 2.1 million. This is smaller than Tokyo, Yokohama, or Osaka but remains Japan’s fourth largest city. Our institution is often not geographically the closest cardiac surgery center to the referring facility. We investigated the address at which the patient was admitted to the ambulance using the Japanese postal code and found no significant difference in the distance from the source of transport to our hospital (P = 0.82). A cardiologist, available in-house for 24 h, directs initial patient management in the emergency department, with the cardiac surgeon assuming the leadership of the ATAAD team once the diagnosis is confirmed. Once the patient is anesthetized, intraoperative transesophageal echocardiography (TEE) is performed. TEE confirms the diagnosis, delineates aortic valve involvement, and provides a means for intraoperative monitoring and planning.
Central aortic repair was performed to exclude the entry and reinstall the true lumen. The extent of graft replacement was based on the position of the primary entry. When the entry was in the ascending aorta, hemiarch replacement was performed; when the entry was in the aortic arch, total or partial arch replacement was performed. An intra-bladder or pharyngeal temperature of 25 °C was used as the target. Cardiopulmonary bypass was instituted via bicaval drainage and cannulation of the femoral and right axillary arteries. Conventional selective cerebral perfusion was initiated for brain perfusion. Four experienced cardiac surgeons performed open surgical repair.
The primary endpoint was defined as major adverse cardiac or cerebrovascular events (MACCE), and the secondary endpoint was major adverse aortic events (MAAE). MACCE were defined as the composite of total death, cardiac events, cerebrovascular events, and revascularization, including percutaneous coronary intervention, cerebrovascular intervention, and coronary artery bypass grafting. The MAAE were a composite of major aortic events and aortic reintervention. Major aortic events included aortic rupture and redissection. Major aortic reinterventions included additional thoracic endovascular aortic repair and aortic surgery.
Statistical Procedures
Continuous variables were expressed as medians (range), and categorical variables were expressed as numbers (percentages). Categorical variables were analyzed using Fisher’s exact test. Continuous variables were compared using Student’s t-test, whereas nonparametric variables were analyzed using the Mann–Whitney U-test. All data analyses were performed using the JMP 14.1 software (SAS Institute, Cary, NC, USA). Statistical significance was defined as P < 0.05.
Results
This study included 98 patients with acute type A aortic dissection who underwent emergency surgery at our hospital between August 2015 and July 2023. Forty-one patients were transported directly to our hospital for emergency surgery (direct transfer cases) and 57 patients were transferred to other hospitals and to our hospital after diagnosis (cases transferred from other hospitals). The median age was 68 years (range, 34–88 years) and 66 patients were male (67%). The time from onset to arrival at the hospital and the time from onset to arrival at the operating room were 180 (20-741) and 285 (61-962) minutes, respectively. Early mortality occurred in six patients (6%): three patients died of extensive cerebral infarction, one of descending aortic rupture, one of multiorgan failure, and one of coma. Late mortality occurred in four (4%) cases: two patients died of heart failure 3 months and 2 years after surgery and two patients died of an unknown causes 3 months and 6 months after surgery.
The follow-up period was 295 (0-2022) days. During follow-up, including duplicates, MACCE occurred in 23 (23%) cases, of which 10 patients died in the early and late periods, including one case of stroke, four patients who required redo open-heart surgery, two patients who needed percutaneous coronary intervention, one patient who developed heart failure requiring hospitalization, and eight patients who developed major cerebrovascular events. In redo open-heart surgery, two patients underwent re-anastomosis of the artificial graft because of severe bending, one patient underwent aortic valve replacement, and one patient underwent aortic root repair. MAAE occurred in 19 (19%) cases, of which one patient died due to aortic rupture, four patients required redo open-heart surgery or open surgery for new aortic lesions, and 15 patients underwent endovascular aortic repair or intervention for aortic disease, including one case of redo open surgery.
The patient characteristics and preoperative data are summarized in Table 1.
|
|
Direct admission n =41 |
Transfer from other hospitals n =57 |
P value |
|
Age |
68 (45-86) |
68 (34-88) |
0.47 |
|
Sex (male, %) |
27 (66) |
39 (68) |
0.79 |
|
Previous cardiac surgery (%) |
1 (2) |
3 (5) |
0.93 |
|
Resuscitation before surgery (%) |
4 (10) |
2 (4) |
0.21 |
|
Intubation at referral (%) |
5 (12) |
2 (4) |
0.10 |
|
Catecholamines at referral (%) |
4 (10) |
1 (2) |
0.16 |
|
Aortic valve regurgitation (moderate to severe) (%) |
7 (17) |
13 (23) |
0.48 |
|
Preoperative organ malperfusion (%) |
22 (54) |
22 (39) |
0.14 |
|
Preoperative hemiparesis (%) |
9 (22) |
14 (25) |
0.76 |
|
Extension of dissection, Asc: Arch: Des (%) |
6; 1; 34 |
4; 4; 50 |
0.30 |
|
Location of the primary entry tear, Asc: Arch: Des (%) |
22(54); 18(44); 1(2) |
19(33); 37(65); 1(2) |
0.12 |
|
Hypertension (%) |
31 (76) |
42 (74) |
0.42 |
|
Smoking (%) |
21 (51) |
28 (49) |
0.84 |
|
Chronic respiratory disease (%) |
2 (5) |
3 (5) |
0.93 |
|
Hemodialysis (%) |
0 |
1 (2) |
0.30 |
|
Coronary artery disease (%) |
0 |
3 (5) |
0.069 |
|
Cerebrovascular disease (%) |
1 (2) |
3 (5) |
0.17 |
|
Family history (%) |
2 (5) |
2 (4) |
0.74 |
|
Spouse or partner (%) |
27 (66) |
40 (70) |
0.79 |
|
Cohabitant (%) |
31 (76) |
44 (77) |
0.98 |
|
Time from onset to arrival at the hospital (minutes) |
58 (20-741) |
245 (42-619) |
<0.0001 |
|
Time from onset to arrival at the operating room (minutes) |
187 (61-962) |
319 (102-654) |
0.011 |
|
GERAADA score |
17 (9.2-77.6) |
13.5 (8.1-58.8) |
0.032 |
|
Tamponade |
13 (32) |
9 (16) |
0.15 |
Table 1: Characteristics of Patients
Statistical significance was defined as P < 0.05.
GERAADA score: The German Registry for Acute Aortic Dissection Type A score
There were no significant differences in sex, previous cardiac surgery, resuscitation before surgery, intubation at referral, catecholamines at referral, aortic valve regurgitation (moderate to severe), preoperative organ malperfusion, preoperative hemiparesis, extension of dissection, location of the primary entry tear within the aortic arch, tamponade, history of hypertension, smoking, chronic respiratory disease, hemodialysis, coronary artery disease, cerebrovascular disease, or family history between the two groups.
Patients transferred from other hospitals had a significantly longer time from onset to arrival at the hospital (P < 0.0001), a longer time from onset to arrival at the operating room (P = 0.011), and lower GERAADA scores (P = 0.032). The time from onset to arrival at the hospital and the time from onset to arrival at the operation room were 58 (20-741) and 187 (61-962) minutes, respectively, in direct transfer cases. The time from onset to arrival at the hospital and the time from onset to arrival at the operation room were 245 (42-619) and 319 (102-654) minutes, respectively, in cases transferred from other hospitals.
The operative procedures and postoperative outcomes are summarized in Table 2.
|
|
Direct admission n =41 |
Transfer from other hospitals n =57 |
P value |
|
Central aortic repair (HAR, PAR, TAR) |
20, 4, 16 |
21, 6, 30 |
0.33 |
|
Concomitant procedure |
CABG 6, AVR 1, PVI 2, VSSR 1 |
CABG 4, AVR 4, PVI 3, VSSR 1 |
|
|
Operation time (minutes) |
438 (274-865) |
440 (241-684) |
0.19 |
|
CPB (minutes) |
232 (145-552) |
238 (125-378) |
0.25 |
|
ACC (minutes) |
128 (85-362) |
130 (82-236) |
0.17 |
|
SCP (minutes) |
94 (30-342) |
127 (30-255) |
0.73 |
|
CA (minutes) |
50 (33-129) |
52 (28-95) |
0.27 |
|
ICU stay (days) |
3 (0-45) |
3 (1-21) |
0.067 |
|
Hospitalization (days) |
22 (0-98) |
19 (9-40) |
0.024 |
|
Cardiac event (%) |
3 (7) |
1 (2) |
0.17 |
|
Neurological outcomes (%) |
3 (7) |
5 (9) |
0.79 |
|
Tracheostomy (%) |
4 (10) |
2 (4) |
0.21 |
|
Renal complication (%) |
0 |
1 (2) |
0.30 |
|
Transfer to other hospital |
7 (17) |
10 (18) |
0.26 |
|
30-day mortality (%) |
5 (12) |
2 (4) |
0.10 |
|
Late mortality (%) |
3 (8) |
0 |
0.0092 |
|
MACCE (%) |
17 (41) |
13 (23) |
0.049 |
|
MAAE (%) |
5 (12) |
18 (32) |
0.021 |
Table 2: Operative Procedures and Outcomes
Statistical significance was defined as P < 0.05. ACC: aortic cross clamp; AVR: aortic valve replacement; CA: circulatory arrest; CABG: coronary artery bypass grafting; CPB: cardiopulmonary bypass time; HAR: hemiarch replacement; ICU: intensive care unit; MAAE: major adverse aortic events; MACCE: major adverse cardiac or cerebrovascular events; PAR: partial arch replacement; PVI: pulmonary venous isolation; SCP: selective cerebral perfusion; TAR: total arch replacement; VSSR: valve-sparing aortic root replacement
There were no significant differences in the operation time, cardiopulmonary bypass time, aortic cross-clamp time, cerebral perfusion time, circulatory arrest time, minimal body temperature, intensive care unit stay, cardiac events, neurological outcomes, tracheostomy, renal complications, transfer to other hospitals, or early mortality between the two groups. Patients transferred from other hospitals had a significantly shorter postoperative hospital stay (P = 0.024), lower incidence of MACCE (P = 0.0488), and lower late mortality (P = 0.0092). However, they had significantly higher incidence of MAAE (P = 0.021).
While early mortality occurred in five patients (12%) and late mortality in three (8%) patients in direct transfer cases, early mortality occurred in two patients (4%) and no late mortality was seen in cases transferred from other hospitals. Freedom from mortality was significantly different (Fig. 1), whereas freedom from MACCE (Fig. 2) and MAAE (Fig. 3) were not significantly different between patients transferred from other hospitals and those transferred directly. Figure 3: Freedom from MAAE In Patients Transferred from Other Hospitals and Transferred Directly.
Figure 1: Freedom from Mortality.
Statistical significance was defined as P < 0.05.
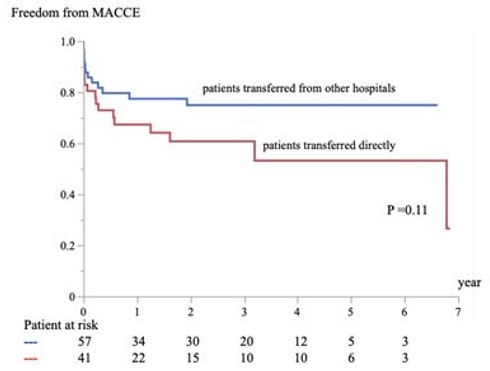
Figure 2: Freedom from MACCE In Patients Transferred from Other Hospitals and Transferred Directly.
Statistical significance was defined as P < 0.05. MACCE: major adverse cardiac or cerebrovascular events
Figure 3: Freedom from MAAE In Patients Transferred from Other Hospitals and Transferred Directly.
Statistical significance was defined as P < 0.05. MAAE: major adverse aortic events
A comparison of preoperative and postoperative outcomes of transferred cases between tertiary and non-tertiary hospitals is shown in Table 3. Of the 57 cases transferred from other hospitals, 44 (77%) cases were referred from a tertiary hospital. There were no significant differences in GERAADA scores, time from onset to arrival at the hospital, time from onset to arrival at the operating room, operation time, postoperative hospital stay, early mortality, late mortality, MACCE, or MAAE between the two groups.
|
|
Tertiary institution n =44 (%) |
Non-tertiary institutionn =13 (%) |
P value |
|
Age |
68 (34-88) |
67 (40-73) |
0.77 |
|
Sex (male, %) |
31 (70) |
8 (62) |
0.55 |
|
Previous cardiac surgery (%) |
3 (7) |
0 |
0.21 |
|
GERAADA score |
13.6 (8.1-55.2) |
14 (8.5-58.8) |
0.49 |
|
Tamponade |
8 (18) |
3 (23) |
0.7 |
|
Time from onset to arrival at the hospital (minutes) |
244 (74-619) |
247 (42-552) |
0.79 |
|
Time from onset to arrival at the operating room (minutes) |
305 (121-654) |
369 (102-604) |
0.24 |
|
Operation time (minutes) |
436 (241-684) |
440 (252-643) |
0.94 |
|
Hospitalization (days) |
19 (9-39) |
22 (11-40) |
0.49 |
|
Early mortality (%) |
1 (2) |
1 (8) |
0.39 |
|
Late mortality (%) |
0 |
0 |
0.39 |
|
MACCE (%) |
8 (18) |
5 (38) |
0.14 |
|
MAAE (%) |
16 (36) |
2 (15) |
0.13 |
Table 3: Outcomes Between Tertiary and Non-Tertiary Institute
Statistical significance was defined as P < 0.05. GERAADA score, German Registry for Acute Aortic Dissection Type A score; MAAE, major adverse aortic events; MACCE, major adverse cardiac or cerebrovascular events
Discussion
In the present study, patients transferred from other hospitals had a significantly lower GERAADA score, shorter postoperative hospital stay, lower incidence of MACCE, and lower late mortality despite a significantly longer time from onset to arrival at the hospital and operating room. In contrast, patients transferred directly to our hospital had significantly higher GERAADA scores, resulting in poor outcomes. Based on these results, we speculate that transfer time is not directly associated with an improved prognosis.
Preoperative clinical status, rather than operative complexity, is the primary factor affecting postoperative mortality and outcomes in ATAAD [1,10-13]. Patients presenting with emergent conditions such as cardiac tamponade, hypotension, or shock tend to undergo more rapid treatment [3,4]. According to the Japanese Registry of Aortic Dissection data (JRAD), severe preoperative conditions, including shock, need for preoperative cardiopulmonary resuscitation, disturbance of consciousness, and advanced age, were risk factors for in-hospital mortality, even though the referral interval was short. Furthermore, the relationship between in-hospital mortality and the interval from symptom onset to arrival at JRAD centers revealed that in-hospital mortality was higher in patients who were transferred within 150 min than in those who arrived at JRAD centers later than 150 min after symptom onset [7].
Evangelista et al. described that it is not surprising that the period was shorter in unstable patients than in stable patients. They suggested that the major predictors of death, such as tamponade and shock, also forced the surgeon to operate sooner on the most critical patients. Furthermore, they reported that patients who died at the transfer facility or en route were not captured in the International Registry of Acute Aortic Dissection (IRAD), and patients who reached an IRAD facility alive had already undergone selection [8]. Based on these considerations, discussing a patient’s prognosis is difficult without considering the patient’s preoperative condition.
Matthew et al. reported that inter-hospital transfer did not correlate with time to treatment or outcomes [1]. Tseng et al. also reported that inter-hospital transfer did not influence the surgical outcomes in patients with ATAAD. They concluded that transferring patients with ATAAD to tertiary hospitals with experienced cardiac surgical teams may not increase surgical risk [14]. In the present study, there might have been bias in that critical cases were considered unsuitable for transfer at the previous hospital, and relatively mild cases were considered suitable for transfer. Thus, there is an urgent need to create a highly efficient transport network to eliminate selection bias before transfer. Centers with delays in diagnosis and surgery are likely non-tertiary hospitals that are less familiar with dissection. Patients who initially present to non-tertiary hospitals experience delays in recognition and treatment [3].
Although there are many other tertiary medical institutions in the Tokai region, emergency services during the night or weekends are limited to university hospitals, including our institution and some tertiary institutions. In the present study, most medical institutions that referred patients to our facility were tertiary hospitals (77%) and should have been familiar with acute aortic syndrome. However, the results from non-tertiary hospitals were not different from those from tertiary hospitals; therefore, the present study suggests that the size of the referring hospital does not affect the outcome of ATAAD. Matthew et al. created a method whereby referring hospitals can directly upload any radiological images to an online server so that the receiving physician can view them even before speaking with the referring physician through the Transfer Center [1].
Inoue et al. reported that the short interval from the onset of symptoms to arrival at JRAD centers (median, 199 min) was one of the remarkable features of JRAD. They suggested that this short time could reflect geographic and socioeconomic factors, such as the size of the land, quality of the emergency medical system, and high availability of CT per inhabitant [7]. Even in tertiary institutions, physicians may be unfamiliar with the imaging evaluations of acute aortic syndrome. To provide accurate diagnostic imaging and efficient patient transfer, it is critical to establish an acute aortic syndrome network in the Tokai region, which consists of experienced aortic centers, as well as prompt diagnosis with advanced image-sharing technology.
This study has some limitations. First, relatively few patients were included due to the rarity of this condition. Second, this was a retrospective single-center study lacking any form of randomization. To overcome these limitations, a multi-institutional study is required. Third, patients with ATAAD who died before arriving at our hospital were excluded. Furthermore, a key source of delay not addressed in this study was the time that symptomatic patients with ATAAD spent at home before hospital presentation. Fourth, patients with ATAAD are not equivalent when the initial treatment is given at the previous medical facility. Little is known from this data set about the type or experience of physicians who encounter patients first. Physicians’ practical experiences, particularly related to aortic emergencies, may be particularly relevant. Fifth, our study utilizes a subjective reporting of symptom onset and relies on the accuracy of emergency department medical record documentation. Further investigation into these limitations is required.
Conclusion
Patients transferred from other hospitals had better clinical conditions upon arrival and outcomes than those transferred directly. The referral hospital grade did not affect ATAAD outcomes. To eliminate selection bias before transfer, we need to establish a network in the Tokai region equipped with more efficient means of patient transfer, such as image-sharing technology and patient education.
Acknowledgments
The authors thank Honyaku Center for reviewing and editing this manuscript. The authors would like to thank their colleagues for their helpful comments. We also thank Honyaku Center Inc. for English language editing.
Conflicts of Interest
The authors declare that they have no competing interests.
Author Contributions
Study conception: KS, Data collection: KS, YK, Analysis: KS, Investigation: KS, HW, Manuscript preparation: KS, Funding acquisition: KS, Critical review and revision: all authors, Final approval of the article: all authors, Accountability for all aspects of the work: all authors
Funding
No financial support was received for the study.
Availability of Data and Materials
Not applicable.
Ethics Approval and Consent to Participate
All procedures were performed according to the tenets of the Helsinki Declaration, and the Ethics Committee of Aichi Medical University Hospital approved the study on October 19, 2022 (approval number, 2022-126). All patients provided written consent for their clinical data to be used for scientific presentation or publication.
Consent for Publication
The patient provided permission to publish the study. Patient identity has been protected.
References
- Matthews, C. R., Madison, M., Timsina, L. R., Namburi, N., Faiza, Z., & Lee, L. S. (2021). Impact of time between diagnosis to treatment in Acute Type A Aortic Dissection. Scientific Reports, 11(1), 3519.
- Nakai, C., Izumi, S., Haraguchi, T., Henmi, S., Nakayama, S., Mikami, T., & Tsukube, T. (2021). Impact of time from symptom onset to operation on outcome of repair of acute type A aortic dissection with malperfusion. The Journal of Thoracic and Cardiovascular Surgery.
- Harris, K. M., Strauss, C. E., Eagle, K. A., Hirsch, A. T., Isselbacher, E. M., Tsai, T. T., ... & International Registry of Acute Aortic Dissection (IRAD) Investigators. (2011). Correlates of delayed recognition and treatment of acute type A aortic dissection: the International Registry of Acute Aortic Dissection (IRAD). Circulation, 124(18), 1911-1918.
- Froehlich, W., Tolenaar, J. L., Harris, K. M., Strauss, C., Sundt, T. M., Tsai, T. T., ... & Trimarchi, S. (2018). Delay from diagnosis to surgery in transferred type A aortic dissection. The American journal of medicine, 131(3), 300-306.
- Anagnostopoulos, C. E., Prabhakar, M. J., & Kittle, C. F. (1972). Aortic dissections and dissecting aneurysms. The American journal of cardiology, 30(3), 263-273.
- Kocher, K. E., Meurer, W. J., Fazel, R., Scott, P. A.,Krumholz, H. M., & Nallamothu, B. K. (2011). National trends in use of computed tomography in the emergency department. Annals of emergency medicine, 58(5), 452-462.
- Inoue, Y., Matsuda, H., Uchida, K., Komiya, T., Koyama, T., Yoshino, H., ... & Ogino, H. (2020). Analysis of acute type A aortic dissection in Japan Registry of Aortic Dissection (JRAD). The Annals of Thoracic Surgery, 110(3), 790-798.
- Evangelista, A., Isselbacher, E. M., Bossone, E., Gleason, T. G., Eusanio, M. D., Sechtem, U., ... & Eagle, K. A. (2018). Insights from the international registry of acute aortic dissection: a 20-year experience of collaborative clinical research. Circulation, 137(17), 1846-1860.
- Harris, K. M., Strauss, C. E., Duval, S., Unger, B. T.,Kroshus, T. J., Inampudi, S., ... & Henry, T. D. (2010). Multidisciplinary standardized care for acute aortic dissection: design and initial outcomes of a regional care model. Circulation: Cardiovascular Quality and Outcomes, 3(4), 424-430.
- Czerny, M., Schoenhoff, F., Etz, C., Englberger, L., Khaladj, N., Zierer, A., ... & Carrel, T. P. (2015). The impact of preoperative malperfusion on outcome in acute type A aortic dissection: results from the GERAADA registry. Journal of the American College of Cardiology, 65(24), 2628-2635.
- Czerny, M., Siepe, M., Beyersdorf, F., Feisst, M., Gabel, M., Pilz, M., ... & Rylski, B. (2020). Prediction of mortality rate in acute type A dissection: the German Registry for Acute Type A Aortic Dissection score. European Journal of Cardio-Thoracic Surgery, 58(4), 700-706.
- Luehr, M., Merkle-Storms, J., Gerfer, S., Li, Y., Krasivskyi, I., Vehrenberg, J., ... & Wahlers, T. (2021). Evaluation of the GERAADA score for prediction of 30-day mortality in patients with acute type A aortic dissection. European Journal of Cardio-Thoracic Surgery, 59(5), 1109-1114.
- Sugiyama, K., Watanuki, H., Tochii, M., Futamura, Y., Kitagawa, Y., Makino, S., ... & Matsuyama, K. (2022). Impact of GERAADA score in patients with acute type A aortic dissection. Journal of Cardiothoracic Surgery, 17(1), 127.
- Tseng, Y. H., Kao, C. C., Lin, C. C., Chen, C. W., Lu, M.S., Lu, C. H., & Huang, Y. K. (2019). Does interhospital transfer influence the outcomes of patients receiving surgery for acute type A aortic dissection? Type A aortic dissection: is transfer hazardous or beneficial?. Emergency Medicine International, 2019.





