Case Report - (2026) Volume 11, Issue 1
Extensive Necrotic Ulcerations with Leonine Facies Revealing Lucio-Type Lepromatous Leprosy
Received Date: Feb 12, 2026 / Accepted Date: Mar 11, 2026 / Published Date: Mar 23, 2026
Copyright: ©2026 Meryame Hammouch, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Hammouch, M., Hali, F., Chiheb, S. (2026). Extensive Necrotic Ulcerations with Leonine Facies Revealing Lucio-Type Lepromatous Leprosy. Int J Clin Expl Dermatol, 11(1), 01-03.
Abstract
Background: Lucio’s phenomenon is a rare and severe vasculonecrotic complication of diffuse lepromatous leprosy, characterized by extensive necrotic skin lesions due to massive endothelial bacillary proliferation. It typically occurs in untreated or inadequately treated patients.
Case Presentation: We report the case of a 52-year-old male presenting with chronic, diffuse necrotic skin ulcers, a leonine facies, and peripheral neuropathy. History revealed macular hypopigmented lesions dating back 20 years. Skin smears showed a high bacillary index (5+). A diagnosis of Lucio’s phenomenon revealing advanced lepromatous leprosy was established. The patient was treated with WHO-recommended multibacillary multidrug therapy, resulting in significant clinical improvement.
Conclusion: Lucio’s phenomenon represents a diagnostic and therapeutic emergency in multibacillary leprosy. Prompt recognition, rapid bacteriological confirmation, and early initiation of multidrug therapy are crucial to prevent severe functional and systemic complications.
Keywords
Lucio’s Phenomenon, Lepromatous Leprosy, Multibacillary, Necrotic Ulcers, Case Report
Introduction
Lepromatous leprosy represents the multibacillary anergic form of infection caused by Mycobacterium leprae, characterized by massive bacillary dissemination and diffuse cutaneous and neurological involvement [1,2]. Among its reactional complications, Lucio’s phenomenon is a rare and severe entity, initially described in Mexico in the setting of diffuse non-nodular lepromatous leprosy [2,3].
It manifests as extensive necrotic skin lesions secondary to a necrotizing vasculitis associated with marked endothelial bacillary proliferation [3,4]. This complication occurs predominantly in untreated or inadequately treated patients and has become exceptional since the introduction of multidrug therapy recommended by the World Health Organization [5,6].
We report an inaugural case of Lucio’s phenomenon revealing advanced lepromatous leprosy, highlighting the severity of this presentation and the importance of early diagnosis.
Case Presentation
A 52-year-old man was admitted to the emergency department for chronic, diffuse, and progressive cutaneous ulcerations. The medical history revealed the onset, approximately 20 years earlier, of hypopigmented macules localized on the face and extremities, with slow progression over time. These lesions gradually extended and became complicated by deep necrotic ulcerations, predominantly affecting the lower limbs.
On clinical examination, the patient was bedridden, dysphonic, and cachectic. A leonine facies with diffuse facial infiltration was noted. Cutaneous involvement was generalized, consisting of dyschromic lesions, necrotic ulcerations with infiltrated and scarred bases, as well as deformities of the extremities. Neurological examination demonstrated diffuse sensory impairment consistent with peripheral neuropathy. Bilateral inguinal lymphadenopathy was also palpable.
Skin smear examination revealed a high bacillary load, with a bacillary index of 5+. Laboratory investigations showed moderate anemia, with a hemoglobin level of 9 g/dL.
Based on the clinical and paraclinical findings, a diagnosis of Lucio’s phenomenon revealing untreated lepromatous leprosy was established. The patient was started on World Health Organization–recommended multibacillary multidrug therapy (MB-MDT), with subsequent significant clinical improvement.
Discussion
Lucio’s phenomenon is a rare vasculonecrotic complication of diffuse lepromatous leprosy, occurring in the setting of profound cellular anergy and massive bacillary load [1–3]. Unlike erythema nodosum leprosum, which is mediated by immune complex deposition, Lucio’s phenomenon results from direct endothelial invasion by Mycobacterium leprae, leading to vascular thrombosis, ischemia, and extensive necrotic ulcerations [3,4].
Inaugural presentations revealing the disease are now exceptional and reflect prolonged, previously undiagnosed progression [2]. Before the introduction of multidrug therapy, mortality rates reached 20–30%, mainly due to secondary infections and systemic complications [3,4].
In our case, the high bacillary index and infiltrated leonine facies confirm the advanced multibacillary nature of the disease. The differential diagnosis includes systemic vasculitides and infectious necrotizing dermatoses; however, the positive skin smear strongly supports the diagnosis of complicated leprosy.
Prompt initiation of multibacillary multidrug therapy according to World Health Organization recommendations remains crucial for prognosis [6]. This case highlights that, despite the global decline in prevalence, severe presentations still occur and require heightened diagnostic vigilance.
Conclusion
Lucio’s phenomenon represents a diagnostic emergency in multibacillary lepromatous leprosy, reflecting massive bacillary dissemination with necrotizing vascular involvement. In the presence of extensive necrotic skin ulcerations associated with a leonine facies and peripheral neuropathy, leprosy should be promptly considered, even in regions of low endemicity.
Rapid bacteriological confirmation and early initiation of multibacillary multidrug therapy are crucial determinants of prognosis and allow for significant clinical improvement. This case underscores the importance of early recognition of this rare complication in order to prevent severe functional and systemic sequelae.
Figure 1: Necrotic Ulcerations on the Dorsum of the Feet with Toe Necrosis and Bilateral Deformities, Typical Manifestations of Lucio’s Phenomenon
Figure 2: Deep Ulcerations Localized on the Knees, Manifestations of Lucio’s Phenomenon
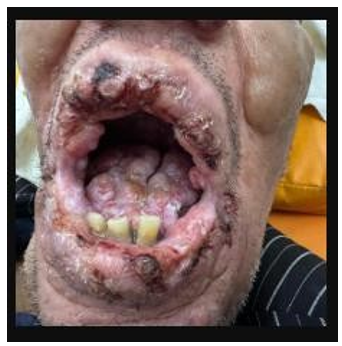
Figure 3: Leonine Facies Associated with Dental and Lingual Malformations in the Patient
References
- Sehgal, V. N., Srivastava, G. (1987). Lucio’s phenomenon: a rare reaction in leprosy. Int J Lepr Other Mycobact Dis, 55(3), 537–543.
- Rea, T. H., Jerskey, R. S. (2005). Lucio’s phenomenon and diffuse nonnodular lepromatous leprosy. Arch Dermatol, 141(9), 1171–1173.
- Azulay, R. D., Azulay, D. R. (1998). The Lucio phenomenon.Int J Dermatol, 37(6), 401–407.
- Santos, M., Talhari, S., & Rabelo, R., et al. (2012). Lucio’s phenomenon: clinical and therapeutic aspects. An Bras Dermatol, 87(3), 453–456.
- Walker, S. L., Lockwood, D. N. J. (2007). Leprosy type1 (reversal) reactions and type 2 reactions (ENL). Clin Dermatol, 25(1), 34–44.
- World Health Organization (2018). Guidelines for the diagnosis, treatment and prevention of leprosy. Geneva: World Health Organization.


