Research Article - (2025) Volume 10, Issue 2
Effectiveness of Ultrasound-Guided Unilateral Subcostal Transverse Abdominal Plane Block Versus Conventional Systemic Analgesics for Postoperative Analgesia among Adult Patients Undergoing Open Cholecystectomy: A Prospective Cohort Study
2School of Medical laboratory, Wolaita Sodo University, Wolaita Sodo, Ethiopia
3Department of Anesthesia, Dilla University College of Health Sciences and Medicine, Dilla, Ethiopia
4School of Medicine, Addis Abeba University, Addis Abeba, Ethiopia
5School of Public health, Wolaita Sodo University, Ethiopia
6School of Anesthesia, Jimma University, Jimma, Ethiopia
Received Date: Jul 09, 2025 / Accepted Date: Aug 11, 2025 / Published Date: Aug 22, 2025
Copyright: ©Â©2025 Mebratu Kebede, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Kebede, M., Tilla, M., Solomon, F., Kasahun, B., Sintayehu, A., et.al. (2025). Effectiveness of Ultrasound-Guided Unilateral Subcostal Transverse Abdominal Plane Block Versus Conventional Systemic Analgesics for Postoperative Analgesia among Adult Patients Undergoing Open Cholecystectomy: A Prospective Cohort Study. J Anesth Pain Med, 10(2), 01-12.
Abstract
Background: Postoperative pain after open cholecystectomy poses a significant challenge, with potential complications and extended hospital stays. Postoperative pain control is traditionally attained by the administration of opioids, which is associated with well-documented side effects. However, limited studies have evaluated the analgesic effect of the subcostal TAP block compared to the conventional systemic analgesics in open cholecystectomy.
Objective: To assess the effectiveness of ultrasound-guided unilateral subcostal transverse abdominal plane block for post- operative analgesia among adult patients undergoing open cholecystectomy.
Method: A prospective cohort study was conducted on 98 patients. Patients in the subcostal transverse abdominals plane block group (n = 49) received block with 20ml of 0.25% bupivacaine, while the non-block group (n = 49) received conventional systemic analgesics. The severity of pain, time to first rescue analgesic administration and total analgesic consumption were assessed 24 hours after surgery. An independent sample t test and a Mann-Whitney U test were used to compare symmetric and asymmetric data, respectively. Time to first rescue analgesic administration was analyzed using Kaplan-Meier survival curve, log rank test and cox-regression for covariates.
Results: In total, 98 patients were analyzed with no dropouts. The severity of postoperative pain was lower in the subcostal transverse abdominals plane block group compared to the non-block group over the whole observation period (P<0.05). Median cumulative opioid consumption in morphine was 0 (0–5) vs. 25 (25–50) mg (P=0.0001) in the subcostal transverse abdominals plane block and non-block groups, respectively. Patients in the subcostal transverse abdominals plane block group had longer time to first rescue analgesia administration, with a median time of 12 hours, 95% CI: [10.997–13.003] compared to the non-block group, whose median time was 0.4hour,95%CI: [0.136- 0.664], with a p=0.001.
Conclusions: Subcostal transverse abdominals plane lowers pain severity, total analgesia consumption, and prolongs time to the first analgesia request. Based on the above findings, we recommend its use for effective postoperative pain management in patients undergoing open cholecystectomy.
Keywords
Analgesia, Cholecystectomy, Postoperative Pain, Subcostal TAP block
Abbreviations
SCTAP-Subcostal Transverse Abdominals Plane Block
MME-Morphine Mill Equivalent
VAS-Visual Analogue Square
BMI-Body Mass Index
HR-Hazard Ratio
WSUCSH-Wolaita Sodo University Comprehensive Specialized Hospital,
SCH-Sodo Christian General Teaching Hospital
Introduction
Cholecystectomy is one of numerous painful upper abdominal surgical procedures. Open cholecystectomy is a frequently performed procedure for symptomatic cholelithiasis, particularly in developing nations where there is scarcity of laparoscopic equipment or expertise. Currently, most cholecystectomies are done by laparoscopic approach; however, open cholecystectomy is common in our setup and involves significant muscle cutting, resulting in moderate to severe postoperative pain [1]. Patients after cholecystectomy often experience persistent moderate to severe pain during coughing and movement within the first 72 hours post-surgery [2,3].
Transverse abdominal plane block (TAP block) has gained popularity as a postoperative analgesic technique after abdominal surgeries. This technique proved to be efficient in reducing perioperative opioid consumption in lower abdominal surgery [4,5]. Hebbard et al. expounded upon the accomplishment of this peripheral block through the application of an ultrasound-guided subcostal oblique approach. This technique facilitated effective postoperative analgesia in upper abdominal procedures such as open cholecystectomy, concurrently yielding a diminished incidence of complications owing to direct ultrasound visualization [6].
Few studies have been published on the ultrasound-guided Subcostal transverse abdominals plane (SCTAP) block technique as post-operative analgesia after cholecystectomy, and those that have been published are varied in terms of the technique or the postoperative analgesic regimen [7,8]. In addition to the differences in the patterns of diseases in our population, it’s strongly suggested that pain severity and perception have significant differences among populations worldwide [9]. Even though epidural anesthesia is one of the alternatives to pain management, the supply of epidural kits is costly and limited in low income countries. However, there is evidence suggesting that ultrasound-guided SCTAP block is comparable to epidural anesthesia in terms of controlling postoperative pain [10].
Furthermore, most studies conducted to assess the analgesic effectiveness of ultrasound-guided SCTAP block are restricted to laparoscopic surgeries; thus, there are limited studies done to evaluate its effectiveness as postoperative analgesia for patients undergoing open cholecystectomy. But in some studies, it was observed that ultrasound-guided SCTAP block, performed after open cholecystectomy under general anesthesia, increased the quality of pain control in the postoperative period and apparently decreased the consumption of opioids [11,12].
Opioid analgesics are the basis of management for moderate to severe postoperative pain and are among the most effective agents for the management of pain. However, opioids are associated with the potential risks of opioid-related side effects (including respiratory and gastrointestinal related events) and abuse or dependence, which can significantly increase the cost of medical care [13].
Ultrasound-guided SCTAP block is technically simple and routinely practiced in our setup. Unfortunately, its effectiveness has not been addressed well before. The aim of this study was to assess the effectiveness of an ultrasound-guided subcostal TAP block versus conventional systemic analgesics as post-operative analgesia among adult patients undergoing open cholecystectomy under general anesthesia.
Methods And Materials
Study Design, Period and Area
This prospective cohort study was conducted at hospitals in sodo town between April 16, 2023, and September 15, 2023. The study was conducted in accordance with the Declaration of Helsinki among patients undergone open cholecystectomy surgery under general anesthesia and taken ultrasound guided SCTAP block as post-operative analgesia (exposed group) vs. non-block group in which post-operative pain was managed with conventional systemic analgesia (un exposed group) The study was registered with the unique protocol registration number of 10650 and the work has been reported in line with the STROCSS criteria [14].
Inclusion Criteria:
ASA I or II adult elective patients who undergo open cholecystectomy under general anesthesia.
Exclusion Criteria:
Refusal of participation in the study, open cholecystectomy under epidural anesthesia, patient remain intubated and admitted to ICU, obese patient (BMI; >30 kg/m2), age <18 and >65, patients with history of chronic pain, psychiatric patient, preexisting neuralgia, opioid tolerance/dependence.
Operational Definition
Visual Analog Score (VAS): Is a validated, subjective measure for acute and chronic pain. Scores are recorded by making a handwritten mark on a 10-cm line that represents a continuum between “no pain” and “worst pain" [15].
Time to First Analgesia Request: A time interval between the block performance and the first post-operative rescue analgesia administration.
Total Post-Operative Analgesia Consumption: Total dose and type of medication given in mg within the first 24 hour starting from admission to recovery room. The total; opioid consumption was measured by converting 24 hours narcotic consumption into standardized morphine mill equivalent (MME) dose.
Post-operative Nausea and Vomiting: When a patient experience at least one episode of either nausea or vomiting within 24 hours.
ASA Status: Is a surgical risk stratification validated by American Society of Anesthesiologist.
Postoperative Analgesic Effectiveness: The capability of analgesia technique to produce a desired result or the ability to produce desired output( lie decreased pain severity in VAS score, prolonged time to first analgesia request and decreased post- operative total analgesia consumption) [16].
Study Outcomes
Severity of postoperative pain by VAS scores
Time to first analgesia request
Total analgesics consumption within 24 hours
Sample Size Determination and Sampling Technique
Sample size was calculated by considering three specific objectives and Sample size estimation based on largest sample size was used and calculated by using a priori power analysis (G Power version 3.1.9.4) [17]. Having no previous study done in the study area, the result adopted from literature of a similar study performed by Milan et al by taking 24 h analgesia consumption (means post-operative analgesia consumption 45.9 and 71.8) and pooled standard deviation was 33.9 and 39.9 between exposed and non- exposed group respectively. With the following assumption: Power as 95%, Level of significance 5% ,1:1 by adding 10% attrition rate and total sample size was 98 (49 in each group) [18].
Study participants were selected by a systematic random sampling technique. After allocating cholecystectomy from two selected hospitals by proportional allocation to size (PAS) [Figure 1] the study unit was determined from 260 patients estimated to undergo cholecystectomy in both hospital during study period, 98 participants were recruited with the probability of about 38%. By considering the consecutive patients scheduled for cholecystectomy data collection was made on 2 patients for every 3 patients who underwent open cholecystectomy. Patients were sorted based on time sequence of PACU admission and one number selected by lottery method was used for exclusion and selection made on the rest of numbers in both groups until the required sample size was reached.
Figure 1: Consort Flow Diagram of the Participants
Data Collection Procedure
After providing training for data collectors, data were collected using pretested questionnaires. Patients scheduled for elective open cholecystectomy were thoroughly assessed before surgery by history taking and chart review was done from patient’s record. On the morning of the surgery, the data collector instructed the patient on how to self-report pain using the VAS score. Socio- demographic and intraoperative variables were filled by the anesthetist in charge, and the remaining postoperative data was collected by three PACU nurses.
On arrival of the patients to the operative theater and after application of the routine hospital monitoring protocol, HR, noninvasive blood pressure, and SPO2 were recorded before induction of general anesthesia. General anesthesia was induced, and during the intraoperative period, HR, NIBP (SBP and DBP), SPO2, and intraoperative analgesic consumption were recorded after induction and at the end of surgery.
At the end of surgery, senior anesthetists give regional anesthesia for postoperative pain management. In study hospitals postoperative pain management for open cholecystectomy mostly done by SCTAP block or other analgesia technique depending on the decision of anesthetist in charge. Therefore, those who take ultrasound guided SCTAP block and non-block group in which post-operative pain was managed with conventional systemic analgesia were included in this study.
Block Technique
The ultrasound-guided unilateral subcostal transverse abdominal plane (TAP) block was performed to provide postoperative analgesia after open cholecystectomy. The procedure was carried out under sterile conditions in the operating room with the patient in the supine position.
Injection Sites
A high-frequency linear ultrasound probe was used to identify the fascial plane between the internal oblique and transverse abdominis muscles. The probe was placed subcostally, starting from the midline and moving laterally until the rectus abdominis muscle was identified. The injection site was selected at the lateral border of the rectus abdominis, at the level of the anterior axillary line.
Local Anesthetic Administration
A 22-gauge, 80-mm echogenic needle was advanced in-plane with the ultrasound probe until the tip was visualized between the lateral border of the rectus abdominis and transverse abdominis muscles. After negative aspiration to confirm the absence of vascular puncture, 20 mL of 0.25% bupivacaine was slowly injected into the facials plane, with intermittent aspiration to avoid intravascular injection. The spread of the local anesthetic was visualized in real- time to ensure proper distribution within the TAP plane.
Total Dose of Local Anesthetic
Each patient received a total dose of 20 mL of 0.25% bupivacaine for the unilateral subcostal TAP block.
Monitoring and Documentation
Patients were monitored for signs of local anesthetic systemic toxicity (LAST) during and after the procedure. The effectiveness of the block was assessed by recording pain scores using visual analogue scale (VAS) at various postoperative intervals (e.g., 30min, 2nd, 4th, 8th, 12th, and 24th hours).
Data Quality Assurance
Data quality was ensured with questionnaires pretested on 5% of the sample size before actual data collection, Training and orientation about the objectives and relevance of the study, each item included in the study tools, and the whole process of data collection were provided for data collectors and supervisors. During data collection, regular supervision and follow-up were undertaken. A supervisor checked each questionnaire daily, with further cross-checking by the principal investigator for completeness and consistency of data. Data clean-up and cross-checking of missing data were done before entering data to Epidata and analyzing it in SPSS.
Data Processing and Analysis
Collected data were entered in Epidata 4.6.0.6 and analyzed using SPSS version 26 software packages. The data was tested for normality by using Shapiro Wilk and homogeneity of variance by Levine’s test for continuous data. Numeric data was described in terms of mean ± SD for symmetric data and median (interquartile range) for asymmetric numeric data. The comparison of numerical variables between study groups was done using the unpaired student t test and the Mann Whitney U test for symmetric and asymmetric data, respectively. Time to first analgesic request was analyzed using log rank test, Kaplan Meier survival curves and cox regression for covariates. Frequency and percentages to describe categorical variables were expressed by using the chi square test. A P value less than 0.05 were considered statistically significant.
Results
Socio Demographic and Preoperative Characteristics
The demographic pre-operative patient characteristics (age, gender, weight, height, BMI, ASA status) were comparable for both groups as shown in Table 1.
|
|
SCTAPB (N=49) |
Conventional systemic analgesia group (n=49) |
P-value |
|
Age(years)* |
40.06±2.996 |
40.41±2.291 |
0.87 |
|
Sex (M/F) |
|
|
0.43 |
|
Male |
7(7.2%) |
1(1.1%) |
|
|
Female |
42(42.8%) |
48(48.9%) |
|
|
Weight(kg)* |
58.88±4.595 |
57.45±4.58 |
0.52 |
|
Height(cm)* |
159±3.2 |
157±4.502 |
0.91 |
|
BMI(kg/m2)* |
22.94±1.506 |
22.76±0.969 |
0.61 |
|
ASA status |
|
|
0.50 |
|
ASA I (n, %) |
44(44.89%) |
46(46.94%) |
|
|
ASA II (n, %) |
5(5.11%) |
7(3.06%) |
|
Hint:*=Mean (standard deviation); Value are presented as: Mean ±SD: Number (%): chi-square test and p<0.05 is statistically significant.
Table 1: Socio Demographic Characteristic of Patients Between Sctap Block and Conventional Systemic Analgesia Group
Intraoperative Patient-Characteristics
The mean total intraoperative analgesic consumption during intraoperative period, duration of surgery and duration of anesthesia were comparable between two groups with P value greater than 0.05 as shown in Table 2.
|
Intraoperative Parameter’s |
SCTAPB n=49 |
conventional systemic analgesics n=49 |
P value |
|
Induction agent |
|
|
0.09 |
|
Propofol |
40(40.8%) |
37(37.7%) |
|
|
Thiopental |
6(6.12%) |
7(7.14%) |
|
|
Ketofol (50%each) |
3(3.08%) |
5(5.16%) |
|
|
Surgeon experience |
|
|
1.00 |
|
Senior (n, %) |
49(50%) |
49(50%) |
|
|
Types of skin incision |
|
|
1.00 |
|
Subcostal (n, %) |
49(50%) |
49(50%) |
|
|
Duration of Surgery * |
91.37±2.86 |
90.81±3.21 |
0.24 |
|
Intraoperative analgesia |
|
|
|
|
Diclofenac IM(mg) |
64.29±12.05 |
67±7.99 |
0.46 |
|
Intraoperative opioid MME(mg) |
9.55±6.31 |
11.84±2.30 |
0.1 |
Hint:*=Mean (standard deviation); Value are presented as: Mean +SD: chi-square test and p<0.05 is statistically significant
Table 2: Intraoperative Characteristic of Patient Between Sctap Block and Conventional Systemic Analgesics
Postoperative Pain Severity
Post-operative Pain Severity Comparison in VAS Score at Rest
There is significant reductions in VAS score at rest in SCTAP block compared to patients taken conventional systemic analgesia (non-block group) during whole observation period with large effect size expressed in terms of Cohan’s d and P<0.05 as shown in Table 3.
|
VAS Score |
SCTAPB group (n=49) |
Conventional systemic analgesic group (n=49) |
P-Value |
|
Immediately at arrival of recovery room VAS score at rest |
0.20±0.407 |
2.65±0.481 |
0.002** |
|
30 min post-operative VAS score |
0.27±0.407 |
2.87±0.542 |
<0.0001*** |
|
2nd hr. post-operative VAS Score at rest |
0.96±0.644 |
3.14±0.644 |
<0.0001*** |
|
4th hr. post-operative VAS score at rest |
1.35±0.481 |
3.27±0.531 |
<0.0001*** |
|
6th hr. post-operative VAS score at rest |
1.53±0.544 |
3.57±0.612 |
<0.0001*** |
|
12th hr. post-operative VAS score at rest |
1.86±0.408 |
3.86±0.36 |
<0.0001*** |
|
24th hr. post-operative VAS score at rest |
2.00±0.289 |
3.86±0.433 |
<0.0001*** |
Hint// **= statistically significant, *** =highly statistically significant.
Table 3: Post-operative Pain Severity Comparison in Vas Score at Rest in Sctap Block and Conventional Systemic Analgesic Group
Post-operative Pain Severity Comparison in Vas Score During Movement
There is significant reductions in VAS score during movement in SCTAP block compared to non-block group during whole observation period with P<0.05 as shown in Table 4.
|
VAS score during movement |
SCTAP group (n=49) |
Conventional systemic analgesia group (n=49 ) |
P-Value |
|
Immediately at arrival of recovery room VAS score |
1.04±0.499 |
3.67±0.591 |
0.002** |
|
30 min post-operative VAS score |
1.042±0.50 |
3.87±0.645 |
0.0001*** |
|
2nd hr. post-operative VAS Score |
1.59±0.497 |
4.04±0.538 |
0.0001*** |
|
4th hr. post-operative VAS score |
1.84±0.426 |
4.22±0.550 |
0.0001*** |
|
6th hr. post-operative VAS score |
2.14±0.456 |
4.39±0.533 |
0.0001*** |
|
12th hr. post-operative VAS score |
2.29±0.50 |
4.39±0.606 |
0.0001*** |
|
24th hr. post-operative VAS score |
2.45±0.542 |
4.39±0.533 |
0.0001*** |
Hint// ** statistically significant, *** =highly statistically significant.
Table 4: Post-operative Pain Severity Comparison in Vas Score During Movement in Sctap Block and Conventional Systemic Analgesia Group
Comparison of time to First Rescue Analgesia Administration
Kaplan-Meier survival curve for first rescue analgesia administration with the patient not receiving any analgesics after 24 hr censored to the right presented in (Figure 2). Log –rank test was obtained between SCTAP block vs. non-block group and (p <0.0001), Patient in the SCTAP block group had significantly longer time to first rescue analgesia administration with median time: 12-hour, 95% CI: [10.997- 13.003] compared to non-block Group, median time 0.4hour,95%CI: [0.136- 0.664]. Cumulative proportion of patient not requesting analgesia at time of 5h after surgery in the non-block group was 1% compared to 90% in SCTAP block group [Figure 2].
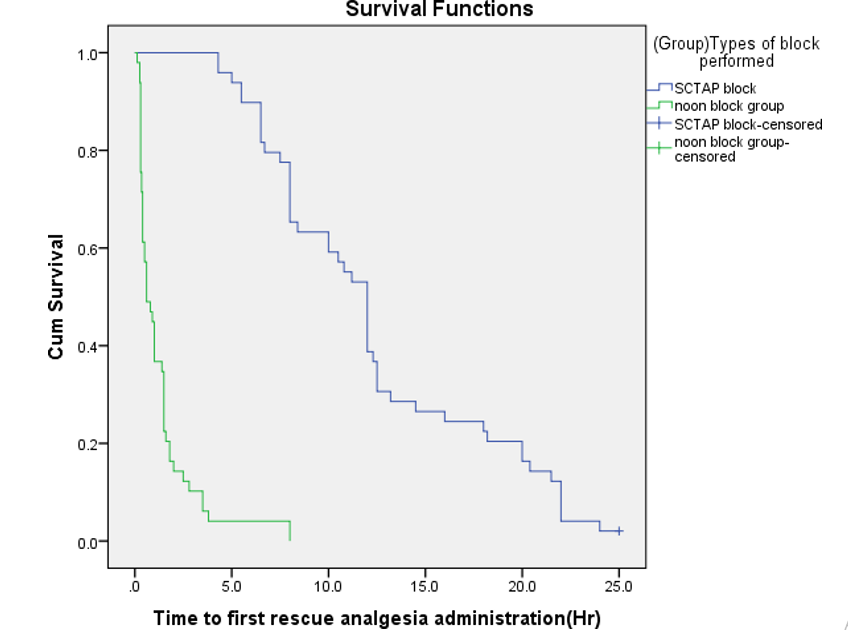
Figure 2: Kaplan Meier Survival Function Curve for Time to First Rescue Analgesic Administration.
Hazard of Receiving the First Rescue Analgesia Administration
A cox proportional hazards model for first rescue analgesia administration adjusted for covariate (study group, sex, age and BMI). In univariate analysis presence of all covariate have no significant association with time first rescue analgesia administration except the exposure status. The hazard of receiving first dose of rescue analgesia in SCTAP block group was reduced by 85% relative to non-block group with 95% of CI (76%-91%) p<0.0001as shown in figure 3.
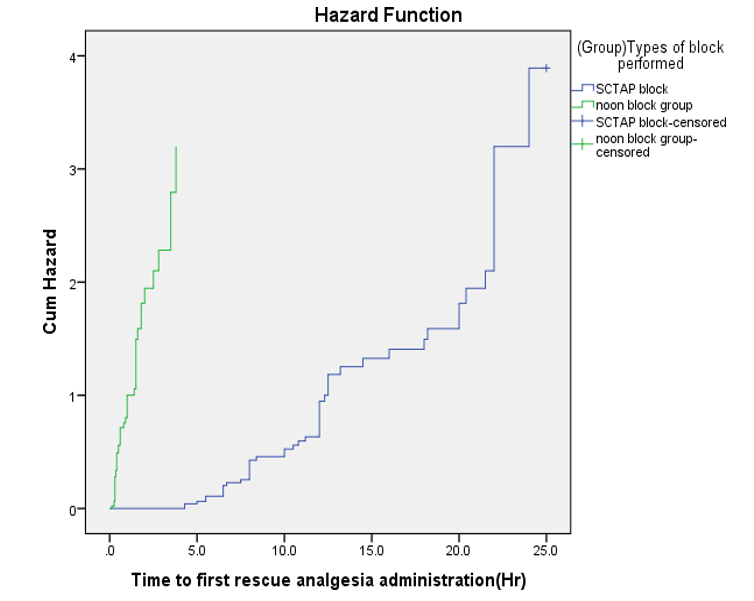
Hint: HR= Hazard ratio, **=highly statistically significant
Figure 3: Kaplan Meier Curve of Hazard Function for Time to First Rescue Analgesia Administration.
Comparison of Total Analgesia Consumption between the Groups
It was discovered that SCTAP block group total diclofenac consumption 75(75-75) was significantly lower than the non- block group 75(75-150).p<0.0001and SCTAP block postoperative opioid consumption in MME 0(0-5) was significantly lower than non-block group 25(25-50), p<0.0001. Table 5
|
Total analgesic consumption with 24 hour in milligram |
SCTAP block group (n=49) |
Conventional systemic analgesia groups (n=49) |
P-value |
|
Diclofenac (IM) |
75(75-75) |
75(75-150) |
0.0001** |
|
Total dose of opioid in MME (IV) |
0(0-5) |
25(25-50) |
<0.0001** |
Hint: the value are presented as median (IQR), **highly statistically significant,, MME(morphine mill equivalent)
Table 5: Comparison of total Analgesia Consumption Between Groups Within 24hrs
Incidence of Nausea and Vomiting Between the Groups
The proportions of patients with nausea and vomiting is lower 3(6.1%) in SCTAP group compared to 33(67.3%) in non- block group with p value of <0.0001. The incidence of post-operative nausea and vomiting is lower in SCTAP block group with RR=0.091 95% CI [0.02-0.276] as shown in figure 4.
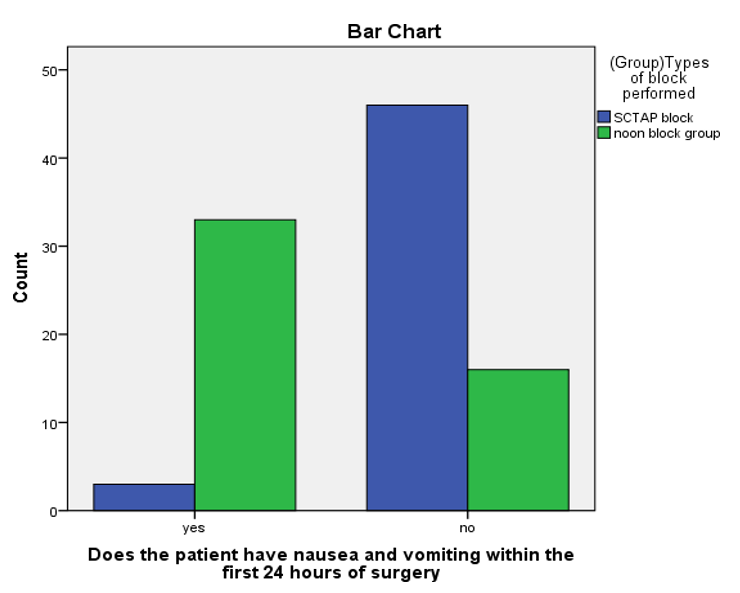
Figure 4: Incidence of Post-Operative Nausea and Vomiting Between Groups.
Discussion
Our study demonstrated that ultrasound guided SCTAP block decreases postoperative pain severity both at rest and movement, reduces post-operative analgesia consumption and prolongs time to first analgesia request in which median time to first analgesia request was significantly prolonged in SCTAP block ,median time:12hour, 95% CI: [10.997- 13.003]versus non-block group, median time 0.4 hour, 95%CI: [0.136- 0.664] and hazard of receiving first dose of rescue analgesia in SCTAP block group was reduced by 85% relative to non-block group with 95% CI of (76%-91%) p<0.0001.
The results of our study shows that postoperative (mean ±SD) pain score were lower in SCTAP block group compared to non- block group immediately at arrival of recovery room, 2nd , 4th, 6th , 12th and 24th post-operative hour both at rest and movement with statistically significant difference of p<0.0001. This finding was comparable with previous study by Arzu et al in which ultrasound guided SCTAP block reduced post- operative pain severity than non- block group immediately at arrival recovery,2nd ,4th,6th,12thand 24thhr with p<0.05 [19]. This could be explained that ultrasound guided SCTAP block resulted in pain reduction after cholecystectomy via subcostal incision that could attribute to blockade of somatic pain fibers originating from T5-T11which reduces the nociceptive input to the central nervous to system that could attenuate central sensitization, thereby leading less postoperative pain [20].
Likewise the result of this study in line with study by Breazu et al 60 patients scheduled for cholecystectomy surgery demonstrated that (mean ±SD) VAS score at 2nd post-operative hour (1.73 ± 1.04) in SCTAP block is lower compared to (3.83 ± 1.76)in non-block group and there is also statistically significant difference in 4th ,6th ,12th and 24thhr at rest and movement with (p- value<0.001. Also the current finding was comparable with previous studies done by Milan et al, Swati et al and Caius et al where ultrasound guided SCTAP block reduced the severity of postoperative pain after open cholecystectomy, liver transplantation and nephrectomy surgery p<0.001.This finding was also supported by other studies [8,11,12,18,21-24].
In this study, the median time to the first analgesic request was significantly prolonged in SCTAP block compared to non-block group and the hazard of receiving first dose of rescue analgesia in SCTAP block group was reduced by 85% relative to non-block group with 95% CI of (76%-91%) p<0.0001. The result of this study corroborated with the study done by Parikh et al in which sixty patients received ultrasound guided SCTAP block were demonstrated and the mean time to first analgesia request in patient undergone SCTAP block group had significantly longer time to first dose of rescue analgesic (547.13±266.96 min vs [22]. 49.17±24.95 in non-block group respectively with p<0.0001. The rationale for long duration of analgesic effect of SCTAP blockade might be linked to the poorly vascularized TAP which allowed time-consuming clearance of bupivacaine local anesthetic. Our findings are also consistent with those of Gurkaran et al in which 70 patients undergone open cholecystectomy the mean time to first rescue analgesia administration in ultrasound guided SCTAP block group was 10.29±4.554hr with p<0.001 [25].
Furthermore, our study also shows comparable result with previous studies by Kamhawy et al, Jinida et al and Seema et al in which patient undergone ultrasound guided subcostal TAP block had prolonged time to first analgesia request than non-block group after cholecystectomy (P<0.0001) [12,21,25]. The similarity might be due to the use of same dose of bupivacaine, 20ml of 0.25%. Although there was prolonged mean time of first analgesic request in the SCTAP block group in both studies, the median analgesic request time was more prolonged in our study, which could be attributed to performance of block at the end of surgery.
Current study revealed that the total amount of opioid consumption over the postoperative 24 hours was lower in the SCTAP block group compared to non-block group, with (P<0.05). which were comparable to the results of Ibrahim and Shamaa et al found that the mean of total consumption of morphine in the initial 24 h postoperative in patients receiving SCTAP block was 16.76 mg compared to 24.76 mg in the control group (p < 0.001).This is due to the fact that local anesthetics injected in facial plane between rectus abdominals and transverse abdominal muscle results in extensive block of nerves innervating subcostal region leading to reduced overall analgesia consumption [26,27].
In contrary to our study a study conducted by Houben et al in Twenty-four hour postoperative opioid consumption were similar in both groups: 21.2mg (95% CI 15.3 to 27.1) vs. 25.2 (95% CI 15.1 to 35.5) oral morphine equivalent in the SCTAP block and non-block group respectively [28]. This might be due to difference in surgical procedure in which laparoscopic surgery were used whereas open cholecystectomy were used in present study, differences in the methodology used in these studies, population difference, medication and the doses of local anesthetics used, comparable finding were depicted with those of Dawlatly et al who showed 55% decrease in opioid requirement after USG-guided subcostal TAP block in patient undergoing cholecystectomy and Niraj et al showed 45% decrease in opioid requirement with USG-guided TAP block in open appendectomy [29]. Also the finding of present study was comparable with previous studies conducted on cholecystectomy, open liver transplantation surgery, nephrectomy and open gastrostomy using the same concentration of bupivacaine [ 8,12,30-32].
As regard to postoperative nausea and vomiting the present study evidenced that ultrasound guided SCTAP block decrease incidence of PONV. In agreement with study by Oksar et al and Zhao et al concluded that SCTAP block decreases incidence of postoperative nausea and vomiting if included as part of multimodal analgesia [33,34]. This could be explained that ultrasound guided SCTAP block resulted in reduced opioid consumption as opioid increases incidence of PONV [35,36].The study's strengths include the fact that it is the first of its kind in the region and the country as a whole, No loss to follow-up of patients, which results in missing data. Variability in the performance of the SCTAP block since different anesthetists were involved, shorter duration of postoperative follow up, lack of standard pain management protocol in the study hospital especially during postoperative period and lack of control over confounding factors like incision size were among limitation we encountered during data Collection [35,36].
The Strength and Limitations of The Study
The study design and homogeneity of the study population are the strength of this study. While being shorter follow-up duration and evaluation of long-term effects are our limitations. We recommend further well-designed multicentre randomized controlled trials.
Conclusion
Ultrasound guided SCTAP block is effective analgesic techniques for treatment of post cholecystectomy pain by reducing post- operative pain score, total analgesic consumption and prolong time to first analgesic request. Therefore, it is safe and effective analgesia for the post-operative pain management in adult patients undergoing open cholecystectomy
References
- Fentie, D. Y., Gebremedhn, E. G., Denu, Z. A., & Gebreegzi,H. (2017). Efficacy of single-injection unilateral thoracic paravertebral block for post open cholecystectomy pain relief: a prospective randomized study at Gondar University Hospital. Local and Regional Anesthesia, 67-74.
- Gan, T. J., Robinson, S. B., Oderda, G. M., Scranton, R., Pepin, J., & Ramamoorthy, S. (2015). Impact of postsurgical opioid use and ileus on economic outcomes in gastrointestinal surgeries. Current medical research and opinion, 31(4), 677- 686.
- MT, F. M., & JJ, P. B. (2015). Ultrasound-guided cutaneous intercostal branches nerves block: A good analgesic alternative for gallbladder open surgery. Revista Espanola de Anestesiologia y Reanimacion, 62(10), 580-584.
- Shibata, Y., Sato, Y., Fujiwara, Y., & Komatsu, T. (2007). Transversus abdominis plane block. Anesthesia & Analgesia, 105(3), 883.
- Hebbard, P. (2008). Subcostal transversus abdominis plane block under ultrasound guidance. Anesthesia & Analgesia, 106(2), 674-675.
- Hebbard, P., Fujiwara, Y., Shibata, Y., & Royse, C. (2007). Ultrasound-guided transversus abdominis plane (TAP) block. Anaesthesia and intensive care, 35(4), 616-618.
- Hebbard, P. D., Barrington, M. J., & Vasey, C. (2010). Ultrasound-guided continuous oblique subcostal transversus abdominis plane blockade: description of anatomy and clinical technique. Regional Anesthesia & Pain Medicine, 35(5), 436-441.
- Swati, S., Shagufta, N., Erum, O., Adil, A., & Urvashi,Y. (2020). Ultrasound-guided intercostal nerve block and subcostal transversus abdominis plane block for postoperative analgesia in patients posted for open cholecystectomy: a randomized controlled trial. Anesthesia Essays and Researches, 14(3), 376-383.
- Ballantyne, J., Cousins, M., Giamberardino, M. A., Jamison,R. N., McGrath, P. A., & Rajagopal, M. T. (2011). Managing acute pain in the developing world. International Association for the study of pain (IASP), Pain Clinical Updates, 19(3).
- Wu, Y., Liu, F., Tang, H., Wang, Q., Chen, L., Wu, H., ... &Xu, X. (2013). The analgesic efficacy of subcostal transversus abdominis plane block compared with thoracic epidural analgesia and intravenous opioid analgesia after radical gastrectomy. Anesthesia & Analgesia, 117(2), 507-513.
- Chen, C. K., & Phui, V. E. (2011). The efficacy of ultrasound- guided oblique subcostal transversus abdominis plane block in patients undergoing open cholecystectomy: case study. Southern African Journal of Anaesthesia and Analgesia, 17(4), 308-310.
- Kamhawy, G., El-Taher, E., & Abdelrahman, M. (2017). A comparison of oblique subcostal transversus abdominis plane block versus thoracic paravertebral block for postoperative analgesia after open cholecystectomy. Egyptian Journal of Anaesthesia, 33(4), 323-329.
- Jahr, J. S., Bergese, S. D., Sheth, K. R., Bernthal, N. M., Ho,H. S., Stoicea, N., & Apfel, C. C. (2018). Current perspective on the use of opioids in perioperative medicine: an evidence- based literature review, national survey of 70,000 physicians, and multidisciplinary clinical appraisal. Pain Medicine, 19(9), 1710-1719.
- Mathew, G., & Agha, R. (2021). STROCSS 2021:strengthening the reporting of cohort, cross-sectional and case-control studies in surgery. IJS Short Reports, 6(4), e35.
- Breivik, H., Borchgrevink, P. C., Allen, S. M., Rosseland, L. A., Romundstad, L., Breivik Hals, E. K., ... & Stubhaug, A. (2008). Assessment of pain. British journal of anaesthesia, 101(1), 17-24.
- Vadivelu, N., Mitra, S., & Narayan, D. (2010). Recent advances in postoperative pain management. The Yale journal of biology and medicine, 83(1), 11.
- Window, M. and Plot, P. G. Power.
- Milan, Z. B., Duncan, B., Rewari, V., Kocarev, M., & Collin,R. (2011, September). Subcostal transversus abdominis plane block for postoperative analgesia in liver transplant recipients. In Transplantation proceedings (Vol. 43, No. 7, pp. 2687-2690). Elsevier.
- Kitik, A., Erdogan, M. A., Ozgul, U., Aydogan, M. S., Ucar,M., Toprak, H. I., ... & Durmus, M. (2017). Ultrasound- guided transversus abdominis plane block for postoperative analgesia in living liver donors: a prospective, randomized, double-blinded clinical trial. Journal of Clinical Anesthesia, 37, 103-107.
- Berthoud, H. R. (2004). Anatomy and function of sensory hepatic nerves. The Anatomical Record Part A: Discoveries in Molecular, Cellular, and Evolutionary Biology: An Oficial Publication of the American Association of Anatomists,280(1), 827-835.
- Breazu, C. M., Ciobanu, L., Hadade, A., Bartos, A., Mitre, C., Mircea, P. A., & Ionescu, D. (2016). The efficacy of oblique subcostal transversus abdominis plane block in laparoscopic cholecystectomy–a prospective, placebo controlled study. Romanian journal of anaesthesia and intensive care, 23(1), 12.
- Parikh, B. K., Waghmare, V. T., Shah, V. R., Mehta, T., Butala,B. P., Parikh, G. P., & Vora, K. S. (2013). The analgesic efficacy of ultrasound-guided transversus abdominis plane block for retroperitoneoscopic donor nephrectomy: a randomized controlled study. Saudi journal of anaesthesia, 7(1), 43-47.
- Hasan, M. S., Ling, K. U., Vijayan, R., Mamat, M., & Chin,K. F. (2011). Open gastrostomy under ultrasound-guided bilateral oblique subcostal transversus abdominis plane block: a case series. European Journal of Anaesthesiology| EJA, 28(12), 888-889.
- Li, K., Li, L., Gao, M., Zhu, Z., Chen, P., Yang, L., & Zhao,G. (2015). Application of ultrasound-guided subcostal transversus abdominis plane block in gastric cancer patients undergoing open gastrectomy. International journal of clinical and experimental medicine, 8(8), 13976.
- Jindal, S., Sidhu, G. K., Baryha, G. K., Singh, B., Kumari, S., & Mahajan, R. (2020). Comparison of efficacy of thoracic paravertebral block with oblique subcostal transversus abdominis plane block in open cholecystectomy. Journal of Anaesthesiology Clinical Pharmacology, 36(3), 371-376.
- Ibrahim, M., & El Shamaa, H. (2014). Efficacy of ultrasound- guided oblique subcostal transversus abdominis plane block after laparoscopic sleeve gastrectomy: a double blind, randomized, placebo controlled study. Egyptian Journal of Anaesthesia, 30(3), 285-292.
- Hebbard, P. D., Barrington, M. J., & Vasey, C. (2010). Ultrasound-guided continuous oblique subcostal transversus abdominis plane blockade: description of anatomy and clinical technique. Regional Anesthesia & Pain Medicine, 35(5), 436-441.
- Houben, A. M., Moreau, A. S. J., Detry, O. M., Kaba, A., & Joris, J. L. (2019). Bilateral subcostal transversus abdominis plane block does not improve the postoperative analgesia provided by multimodal analgesia after laparoscopic cholecystectomy: a randomised placebo-controlled trial. European Journal of Anaesthesiology| EJA, 36(10), 772-777.
- El-Dawlatly, A. A., Turkistani, A., Kettner, S. C., Machata,M., Delvi, M. B., Thallaj, A., ... & Marhofer, P. (2009). Ultrasound-guided transversus abdominis plane block: description of a new technique and comparison with conventional systemic analgesia during laparoscopic cholecystectomy. British journal of anaesthesia, 102(6), 763- 767.
- Shin, H. J., Oh, A. Y., Baik, J. S., Kim, J. H., Han, S. H., &Hwang, J. W. (2013). Ultrasound-guided oblique subcostal transversus abdominis plane block for analgesia after laparoscopic cholecystectomy: a randomized, controlled, observer-blinded study. Minerva anestesiologica, 80(2), 185- 193.
- Swati, S., Shagufta, N., Erum, O., Adil, A., & Urvashi,Y. (2020). Ultrasound-guided intercostal nerve block and subcostal transversus abdominis plane block for postoperative analgesia in patients posted for open cholecystectomy: a randomized controlled trial. Anesthesia Essays and Researches, 14(3), 376-383.
- Altiparmak, B., Toker, M. K., Uysal, A. I., Kuscu, Y., & Demirbilek, S. G. (2019). Ultrasound-guided erector spinae plane block versus oblique subcostal transversus abdominis plane block for postoperative analgesia of adult patients undergoing laparoscopic cholecystectomy: Randomized, controlled trial. Journal of clinical anesthesia, 57, 31-36.
- Oksar, M., Koyuncu, O., Turhanoglu, S., Temiz, M., & Oran, M. C. (2016). Transversus abdominis plane blockas a component of multimodal analgesia for laparoscopic cholecystectomy. Journal of Clinical Anesthesia, 34, 72-78.
- Zhao, X., Tong, Y., Ren, H., Ding, X. B., Wang, X., Zong,J. Y., ... & Li, Q. (2014). Transversus abdominis plane block for postoperative analgesia after laparoscopic surgery: a systematic review and meta-analysis. International journal of clinical and experimental medicine, 7(9), 2966.
- Kehlet, H., Rung, G. W., & Callesen, T. (1996). Postoperative opioid analgesia: time for a reconsideration?. Journal of clinical anesthesia, 8(6), 441-445.
- Vrsajkov, V., Mancic, N., Mihajlovic, D., Milicevic,S. T., Uvelin, A., & Vrsajkov, J. P. (2018). Subcostal transversus abdominis plane block can improve analgesia after laparoscopic cholecystectomy. Revista Brasileira de Anestesiologia, 68, 149-153.



