Research Article - (2023) Volume 8, Issue 1
Dual Contraceptive Utilization and Associated Factors among Women Attending Antiretroviral Therapy Clinics in Central Ethiopia, 2022: The Need for a Better Control of Ever-Increasing New Strain of HIV Infection and its Transmission
Received Date: May 15, 2023 / Accepted Date: Jun 07, 2023 / Published Date: Jun 28, 2023
Copyright: ©Ã??Ã?©2023 Sisay Motuma Debela, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Debela, S. M., Adinew, Y. M., Geleta, L. A., Guye, A. H. (2023). Dual Contraceptive Utilization and Associated Factors among Women Attending Antiretroviral Therapy Clinics in Central Ethiopia, 2022: The Need for a Better Control of Ever-Increasing New Strain of HIV Infection and its Transmission. Int J Women
Abstract
Background: Dual contraceptive utilization can reduce the transmission of many sexually transmitted infections and is recommended by the World Health Organization. Even though recent times advise the use of dual contraception as a potent instrument in the control of unintended pregnancy and sexually transmitted infections including HIV/AIDS, there are considerable contraceptive use gaps among women living with HIV globally.
Methods: A facility-based cross-sectional study was conducted from March 22 to June 22/2022 among HIV-positive reproductive age women on Antiretroviral Therapy in the North Shewa Zone, central Oromia health facility. A total of 611 women were selected using a multi-stage sampling technique. A pre-tested structured questionnaire was used to collect data. Both bivariable & multivariable logistic regression analysis was used to find predictors for dual contraceptive utilization.
Result: The overall magnitude of dual contraceptive method utilization among the respondent was 38.1% (95% CI: 34.80-42.02). After adjusting for other variables; who residing in urban [AOR = 0.23 [95% CI: 0.09-0.56]; respondent who married [AOR = 3.32 [95% CI: 1.03-10.94]; husband with formal education [AOR = 7.38[95% CI: 1.52-35.94], respondents who thoughts one of the advantages to disclose HIV serostatus is protecting sexual partner from HIV [AOR = 3.68[95% CI: 1.42-9.43] were significantly associated with dual contraceptive utilization.
Conclusion: The overall magnitude of dual contraceptive utilization among women on ART was found to be low and factors like; place of residence, marital status, educational status of the partner, and participant who utilize due to the reason to protect the sexual partner from acquiring HIV were identified. Efforts have to be made by local governments and other concerned bodies to increase utilization of dual contraceptive method.
Keywords
Contraception, Dual Contraceptive Utilization, Ethiopia, HIV Infection, Women
Abbreviations
AIDS: Acquired Immune Deficiency Syndrome
ART: Antiretroviral Therapy
CD4: Cluster of Differentiation
EDHS: Ethiopian Demographic Health Survey
FP: Family Planning
HIV: Human Immune Deficiency Virus
IUCD: Intra Uterine Contraceptive Device
PLHIV: People Living with Human Immune Deficiency Virus
PMTCT: Prevention of Mother to Child Transmission
STI: Sexually Transmitted Infection
WHO: World Health Organization
Introduction
An estimated 34 million people are living with HIV/AIDS worldwide, with more than 2 million HIV-positive women becoming pregnant each year, the majorities (67.1%) occur in Sub-Saharan Africa [1]. Unintended pregnancy, contraction of new strains of HIV, and pediatric HIV have become challenging issues [2]. It is worth mentioning that, by the end of 2018, more than half (55.9%) of the pregnancies among People living with Human Immune Deficiency Virus (PLWHIV) were unintended, which was mainly due to poor contraceptive utilization [3,4]. The effect of unintended pregnancy among HIV seropositive is well known throughout the world. According to World Health Organization (WHO) report, 21.3% of new pediatric HIV infections are caused by unintended pregnancy among HIV seropositive women [5].
Allowing HIV-positive women to prevent unintended pregnancy can help to reduce vertical HIV transmission, as well as morbidity and mortality among mothers and children [6]. Increasing access to Family Planning (FP) services in Sub-Saharan Africa would result in a significant drop in unintended pregnancies and unsafe abortions, as well as a 69% reduction in maternal deaths and a 57% reduction in neonatal deaths [7]. If Prevention of Mother to Child Transmission (PMTCT) of HIV focused on boosting contraception, it will prevent more than 29% of HIV infections at birth [8]. In addition, the WHO settled on preventing unintended pregnancy by providing safe and effective contraception to HIV-infected women who desire it as a primary strategy for the prevention of pediatric infections [9].
Dual contraceptive method utilization can reduce the risks of both unintended pregnancy and sexually transmitted infections (STIs) including HIV [10]. The protection from unintended pregnancy and STI varies depending on the form of contraception used [2]. Condom use alone as a contraceptive choice does not substantially reduce the risk of pregnancy and in general, it is not an accurate method for women on Antiretroviral Therapy (ART) [11]. Only about 85% of unintended pregnancies may be avoided [12]. On the other hand, hormonal contraception, intrauterine contraceptive devices (IUCD) and permanent methods such as sterilization are more successful than condoms in preventing unintended pregnancy, but they do not prevent Sexually Transmitted Infections (STIs) such as HIV [13]. Because the problem and risk of unprotected sex, such as unintended pregnancy and sexually transmitted infections, are intrinsically linked, the WHO recommended that all HIV-positive individuals should practice safer sex utilizing dual methods as protection against STIs, including HIV and unplanned pregnancy [13,14]. Studies have shown that HIV serodiscordant and sero concordant couples, who continue to engage in unprotected sex will increase their risk of contracting mutant or multiple strains of the human immunodeficiency virus, as well as other STIs and unintended pregnancy if they do not use dual method for disease and pregnancy prevention [1,15].
Despite its advantage, several studies found a low level of magnitude of the utilization of the dual contraception method [16,17]. Even though various attempts have been made in Ethiopia to measure the magnitude of dual contraceptive utilization among women on ART and the factor associated with it, it is essential to keep updated with the current knowledge, since dual contraceptive utilization is unique to the context and is influenced by cultural change. Therefore, this research was intended to determine the magnitude of dual contraceptive utilization and associated factors among women on ART, moreover, to produce evidence on which to lay on to propose a reinforcement of existing strategies for better control of ever-increasing new strains of HIV infection and its transmission.
Plain Language Summary: Dual Contraceptive Utilization among Women Attending ART Clinic
Studies estimated that 75% of HIV-positive people are of reproductive age worldwide. Sixty-four percent of new HIV infections were from Sub-Saharan Africa with 43% women and 2 million children. Currently, in Ethiopia, HIV transmission is still high and many HIV-positive women are still encountering unintended pregnancies with a concomitant risk of mother-to-child transmission (MTCT) of HIV, pregnancy-related morbidity and mortality, and transmission of HIV and a new strain of HIV virus to their sexual partners due to low dual contraceptive method utilization.
Hence, a facility-based cross-sectional study design was conducted on reproductive-age women attending ART clinics in central Ethiopia from March 22 to June 22/2022 to asses dual contraceptive utilization and associated factors to give evidence-based information. A total of 590 women of reproductive age (15 to 49 years) who attend ART clinics participated. The mean age of the respondents was 33.82 ± 6.46 years. Almost half 290(49.2%) of the respondents were in the age group 35-49.
The mean knowledge score of the respondents on modern family planning was 9.023 ± 3.09. Greater than half 273(53.6%) had good knowledge. The overall magnitude of current dual contraceptive utilization in this study was 38.10%. The utilization of dual contraceptive methods was more among participant’s who reside in rural area, who married, husband with formal education, and respondents who thought one of the advantages to disclose HIV serostatus is protecting sexual partners from HIV. Therefore, it needs governmental and non-governmental organizations, and researcher’s involvement to improve dual contraceptive utilization.
Methods
Study Design, Setting, and Participants
A facility-based cross-sectional study design was conducted on reproductive-age women attending ART clinics in North Shewa Zone health facilities, Oromia region, Ethiopia from March 22 to June 22/2022. The study was carried out in randomly selected public health facilities that provide HIV/ AIDS care and treatment services, owning anti-retroviral therapy clinics in North Shewa Zone, Central Ethiopia. Currently, eighteen health institutions
in the city provide ART services (Thirteen health centers, 1 comprehensive Specialized Hospital, 1 General Hospital, and 3 primary hospitals), and the service is linked with family planning services in all of them. In North Shewa Zone, there were 1,695,183 people; 847,591 females, of which 27, 292 were of reproductive age.
Population
Source Population
All HIV-positive reproductive-aged women (15 to 49 years) who are enrolled in chronic HIV care service and are in active follow-up at ART clinics in North Shewa Zone health facilities.
Study Population
HIV-positive reproductive-aged women (15 to 49 years) who are enrolled in chronic HIV care service and are in active follow-ups at ART clinics in randomly selected North Shewa Zone health facilities during the study period.
Inclusion and Exclusion Criteria
Inclusion Criteria
All sexually active reproductive age women who were on ART care service. HIV positive reproductive aged women at least one visit attended before this study.
Exclusion Criteria
HIV positive reproductive age women who are mentally unable to respond. Pregnant women at the time of data collection.
Sample Size Determination and Sampling Procedure
The sample size was determined using the single population proportion formula by taking the prevalence of dual method of contraceptive use (p) to be 59.5% from a previous study done in west Shewa [18]. Ethiopia with the following assumptions: 95% confidence level(Zα/2=1.96), 5% marginal error. Thus, after adding 10% of the non-response rate, and considering the design effect of 1.5, the required sample size was found to be 611.
To reach the study participant multi-stage sampling techniques were applied. Initially, thirty percent of health facility that provides ART service was selected randomly by lottery method, and then the sample size was proportionally allocated for each health facility by the formula ![]()
Where N is the total number of HIV-positive reproductive-aged women (15 to 49 years) who are enrolled in chronic HIV care service at all health institutions (N=2008), Nj is the total number of HIV-positive reproductive-aged women (15 to 49 years) who are enrolled in chronic HIV care service at each health institution then, nj is the proportional sample of HIV-positive reproductive-aged women (15 to 49 years) who are enrolled in chronic HIV care service to be taken from each health institution, and finally n is the calculated sample size At the level of the health facilities, participants were selected using systematic random sampling of every K-interval, while K-interval was calculated by the formula ![]()
Where Nj is the total number of HIV-positive people at each health institution then, nj is the proportional sample of HIV-positive people to be taken from each health institution, K the interval size, and then randomly select an integer between 1 to K, let us denote this number by a, then starting at a take ever Kth unit using the individual identification number of women. The selected list will be a+k, a+2k, and a+3k…, Care that was taken to prevent the double interview from one respondent in the occurrence of cyclic repetition was by keeping the identification number of women that was already interviewed.
Data Collection Procedures
The structured pretested questionnaire was used to collect the required data through a face-to-face interview. The questionnaire was adapted from the ones used by other authors and modified following a literature review of articles [19-24]. The questionnaire contains information on socio-demographic characteristics, socioeconomic status of the respondents, knowledge of family planning methods, dual contraceptive utilization related issues, fertility intention, HIV/STI clinical variable. Chart review was also done on medical records of participants. Data were collected by trained five clinical nurses and were supervised by two public health officers. Data collectors were assigned to data collection at each ART clinic and an exit interview was conducted during routine health facility visits.
Measurement of the Variables
Dual contraceptive utilization is measured by the respondent who answered Yes to the question: simultaneous utilization of any modern contraceptive method with a barrier method (i. e., male condom) during sexual intercourse consistently in the last three months before the study period. Knowledge of family planning methods was measured by nine knowledge questions. The first six questions include numerous answers, and each response was added to create a composite score from no answer to all alternatives. The remaining three questions are based on a Yes/No system, with 1 indicating Yes and 0 indicating No [24]. The wealth index was measured by a simplified and updated Ethiopian wealth index equity tool. The tool contains 15 simplified household assets questions available from www.equitytool.org. The tool has an 84.2% agreement and 0.755 kappa statistics with the full Ethiopian Demographic Health Survey wealth index measurement tool. In this study, households were categorized into three groups: lower, middle, and higher using household factor scores obtained from the principal component analysis [25].
Operational Definitions and Definition of Terms
Dual Contraceptive Utilization
Current utilization of any hormonal, IUCD, or permanent modern contraceptive method along with a male condom for the last three months before the study period consistently [26].
Good Knowledge
A respondent who answered mean and above knowledge question with a response of Yes, while poor knowledge was A respondent who answered below mean [24].
Data Quality Control
The questionnaire was prepared first in English and translated into the local language (Amharic and Afaan Oromo) language by a language expert, then back to English to check for consistency. Training for data collectors for half day on the importance of research, method of data collection, and ethical issues. The supervisors were also trained on how to monitor the data collection procedures. The questionnaire was pretested on 10% of the total sample size out of the study area to check to insure clarity, wording, logical sequence, skip pattern, and acceptability of the questionnaire. Checking collected questionnaires for consistency, completeness, and accuracy was held daily by the supervisor and principal investigators on the spot. The identified errors were corrected after revising the original questionnaires. Mobile data collection using Kobo toolbox software was used for data collection and entry after creating the platform. Checking double data entry was controlled by the must-enter command, skip logic, and validation criteria on kobo toolbox software before deploying the form to Mobile devices and collecting data .
Data Processing and Analysis
All data were coded on mobile-based data collection and exported to SPSS version 25 for analysis. Data exploration was carried out to assess completeness and descriptive statistics were used to describe the study participants’ data based on its nature. A principal component analysis was done to quantify the wealth index. Accordingly, four components were created with varimax rotation and Eigenvalue greater than 1 where the total variance of 67.8% was explained by the model. The study employs binary logistic regression to identify the predictor’s variables. The candidate explanatory variables from the bivariable analysis were selected at P-Value=<0.25. For multivariable analysis, backward: LR was done for dual contraceptive utilization including after adjusting for other characteristics of the study participants considered to be potential confounders. Multi-collinearity was checked by examining the standard errors for the β- coefficients (a standard error larger than 2 indicated its presence). Model fitness was also checked by Hosmer and Lemeshow goodness of fit test (With P-value>0.05, fit model). Finally, the significance was declared based on the adjusted odds ratio with a 95% confidence interval and a p-value less than 0.05.
Result
Sociodemographic Characteristics of the Respondent
A total of 590 women of reproductive age (15 to 49 years) participated in this study with a response rate of, 96.6%. The mean age (SD) of the respondents was 33.82 ± 6.46 years. Almost half 290(49.2%) of the respondents were in the age group 35-49. The marital status of the participants indicated that the majority, 423(71.7%) were unmarried, while the remaining 167(28.3%) were married. Regarding the educational status of the participant almost the majority, 512(86.8%) attended formal education, while the remaining 78(13.2%) had no formal education (Table 1).
|
Variable |
Category |
Frequency |
% |
|
Age |
15-24 |
40 |
6.8 |
|
25-34 |
260 |
44 |
|
|
35-49 |
290 |
49.2 |
|
|
Residence |
Urban |
271 |
45.9 |
|
Rural |
319 |
54.1 |
|
|
Marital status |
Married |
167 |
28.3 |
|
Unmarried/Uncohabited |
423 |
71.7 |
|
|
Educational status of participant |
No formal education |
78 |
13.2 |
|
Attended formal education |
512 |
86.8 |
|
|
Educational status of husband |
No formal education |
78 |
24.2 |
|
Attended formal education |
244 |
75.8 |
|
|
Occupational status of the participant |
Daily laborer |
192 |
32.54 |
|
Merchant |
151 |
25.59 |
|
|
Housewife |
119 |
20.18 |
|
|
Government Employ |
70 |
11.86 |
|
|
Farmer |
37 |
6.27 |
|
|
Others** |
53 |
3.56 |
|
Occupational status of husband |
Daily laborer |
147 |
45.9 |
|
Merchant |
69 |
21.6 |
|
|
Government Employ |
61 |
19.1 |
|
|
Farmer |
40 |
12.5 |
|
|
Others*** |
3 |
0.9 |
|
|
Household wealth index |
Lowest wealth index |
183 |
31.1 |
|
Middle wealth index |
197 |
33.4 |
|
|
Highest wealth index |
209 |
35.5 |
|
|
*Other: Muslim, Catholic **Others: Farmer, waitress, sex worker. ***Others: Driver, contractor |
|||
Table 1: Sociodemographic Characteristic of the Respondent among Reproductive Age Women Attending ART Clinic in Central Oromia, Ethiopia, 2022(n=590)
Sexual and Reproductive Characteristics
About 503(85.3%) heard about family planning, while the remaining 87(14.7%) did not hear about family planning. Concerning the source of information about family planning, 500(99.2%) from a health professional, 434(86.3%) from mass media such as radio, and television, 84(16.7%) were heard from their husband, 348(69.2%) were from peers. Related to the type of modern female contraceptive they knew, the largest portion was Injectable followed by pills which accounted for 500(99.4%), and 487(96.8%) respectively.
Of the 503 respondents who heard about family planning almost greater than half 372(74.0%) knew that there is family planning for men, of this almost all knew condoms as the main type of male contraceptive method. Of the 503 respondents who heard about family planning, 469(93.2%) replied advantages of family planning they knew as avoiding unwanted pregnancy followed by 487(77.46%) were replied to space childbirth, 456(90.7%) were replied as to limit the family size, 457(90.9%) were to space childbirth, and 387(76.8%).
Concerning appropriate space of interval between two consecutive childbirth out of 503 who heard about family planning almost half 263(44.6%) reported three to five years, followed by 157(26.6%) reported one to two years.
Of the 503 women who heard about family planning majority of them, 486(96.6%) knew where to get modern contraceptive methods, and, health centers were the primary place mentioned which accounted for 480(98.8%) followed by Hospital 476(97.9%), private clinics 363(74.7%). The mean knowledge score of the respondents was 9.023 ± 3.09. Concerning knowledge scores greater than half 273(53.6%) had good knowledge (Figure 1).
Figure 1: Knowledge Distribution of Reproductive Age Women Attending ART Clinic in Central Oromia, Ethiopia, 2022(n=590).
Nearly two-thirds, 380(64.4%) of the participant had more than one live child, while the remaining 210(35.6%) had either one or no live child. Almost greater than half, 308(52.3%) of study participants and 224 (52.3%) of women’s sexual partners had no desire to have more children in the future
Clinical and HIV-Related Characteristics
Concerning knowing sexual partners’ HIV status, more than two-thirds, 386 (84.8%) of them reported being aware of their partners’ HIV status, of this, the majority 312(80.8%) were HIV positive. Of all participants, only 67 (11.4%) of them had a history of symptom of other STIs, 62 (92.5%) of whom received treatment. The mean (±SD) duration since they tested HIV positive was 9.05 ± 4.62 years. The majority, 495(83.9%) of study participants tested HIV positive in the past three years, and 56 (9.5%) had multiple sexual partners. The majority, 375(82.6%) of women disclosed their HIV status to their sexual partners, and greater than two-thirds, 515 (87.3%) of study participants thought that disclosure of HIV status to a sexual partner is important due to the advantage of (to discuss freely, to avoid unintended pregnancy, to rotect the sexual partner from acquiring HIV/AIDs, to attend better care, to practice safe sex, and to support each other; 485(94.4)%, 443(86.0%), 442(85.7%), 374(72.3%), 367(71.3%), and 468 (90.8%) respectively.
The mean (±SD) duration of since starting ART was 8.48 ±4.36. The median CD4 cell count of the respondents was 550(IQR; 396, 726), and only 117(19.8%) of them had a current CD4 cell count = of <350. The median viral load count was 49(IQR; 23, 97) with only 54(9.2%) Target not detected range (Table 2).
|
Variable |
Category |
Frequency |
% |
|
Other STI history/syptoms |
Yes |
67 |
11.36 |
|
No |
520 |
88.14 |
|
|
I can't remember |
3 |
0.5 |
|
|
If yes for the above, have been treated |
Yes |
62 |
92.5 |
|
Not |
5 |
7.5 |
|
|
Reason for not being treated |
No access of treatment |
2 |
40 |
|
No need of treatment |
3 |
60 |
|
|
No of sexual partner |
One or no |
534 |
90.5 |
|
Greater than one |
56 |
9.5 |
|
|
Duration since tested for HIV positive |
Less than or equal to 3 years |
95 |
16.1 |
|
|
Greater than 3 years |
495 |
83.9 |
|
Knowing HIV status of regular partner |
Yes |
386 |
84.8 |
|
|
No |
69 |
15.2 |
|
HIV status of regular partner |
Positive |
265 |
68.7 |
|
|
Negative |
121 |
31.3 |
|
Disclosure status of HIV to your sexual partner |
Yes |
361 |
79.5 |
|
No |
93 |
20.5 |
|
|
If not disclosed, what was/were the reason |
Fear of divorce |
23 |
28.75 |
|
Fear of violence by partner |
45 |
56.25 |
|
|
Fear of stigma and discrimination |
41 |
51.25 |
|
|
Others* |
2 |
2.5 |
|
|
Thought disclosure of HIV status to sexual partner is important |
Yes |
505 |
85.6 |
|
No |
85 |
14.4 |
|
|
Duration of ART after start |
Less than or equal to 3 years |
101 |
17.1 |
|
Greater than 3 years |
489 |
82.9 |
|
|
Current CD 4 cell count |
<250 |
47 |
8 |
|
250-350 |
70 |
11.8 |
|
|
>350 |
473 |
80.2 |
|
|
Current Viral Load |
TND |
536 |
90.8 |
|
Not in range of TND |
54 |
9.2 |
|
|
*Others: break relationship tie, chance of missing financial support |
|||
Table 2: Clinical and HIV Related Characteristics among Reproductive Age Women Attending ART Clinic in Central Oromia, Ethiopia, 2022(n=590).
Dual Contraceptive Utilization
The magnitude of current dual contraceptive utilization in this study was 38.10%; 95% CI: 34.80-42.02 (Figure 2).
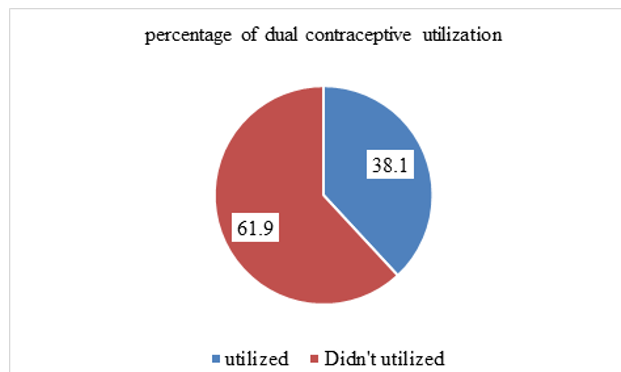
Figure 2: The percentages of Dual Contraceptive Utilization among Reproductive Age Women Attending ART Clinics in Central Oro- mia, Ethiopia, 2022(n=590).
Among the 225 current dual contraceptive utilization users; the main modern contraceptive methods used along with condom was, injectable 140 (61.67%), followed by implant 65(28.63%). Among the 590 participants, 430(73%) and 417(96.8%) have also reported ever use of any modern contraceptive method and ever use of a condom during sexual intercourse since they were aware of HIV serostatus, respectively.
Most of the respondents choose the current dual contraceptive method used, to prevent unintended pregnancy 201(89.3%), prevent acquiring other STIs 195(86.3%), prevent HIV transmission to a sexual partner 184(81.7%), protect from acquiring a new strain of the virus 152(67.5%) and to avoid the occurrence of high viral load 131(58.2%). The most common reason not to use the current dual contraceptive method was the side effect of contraceptives 18(51.9 %).
Factor Associated with Dual Contraceptive Utilization
Bivariable analysis indicated that sociodemographic variables (place of residence, educational status of the woman, and educational status of the partner), Socioeconomic status (wealth index class), client-related factors (knowledge about family planning, protecting sexual partner from acquiring HIV, avoiding unintended pregnancy, and current viral load), showed P-value of less than or equal to 0.25 (Table 4).
In multivariable logistic regression analysis, factors that were independently associated with dual contraceptive utilization were place of residence, marital status, educational status, thought of serostatus disclosure. Accordingly, respondents who resided in urban areas were less likely [AOR = 0.23 [95% CI: 0.09-0.56] utilize dual contraceptive methods when compared to a respondent who residing in rural areas; marital status of the respondent, respondents who were married was more than 3 times more likely [AOR = 3.32 [95% CI: 1.03-10.94] utilize a dual method of contraceptive when compared to their counterparts.
The educational status of the partner was also found to be a factor associated with dual contraceptive utilization. Respondent's partners who have formal education were more than 7 times [AOR = 7.38[95% CI: 1.52-35.94] more likely to utilize the dual contraceptive method when compared to their counterparts. Again, respondents who thoughts one of the advantages of disclosing HIV serostatus is protecting their sexual partner from HIV were more than 3 times more likely [AOR = 3.68[95% CI: 1.42-9.43] utilize dual contraceptive methods when compared to their counterpart. (Table 3).
Discussion
This study aimed to assess the magnitude and factors associated with dual contraceptive utilization among HIV-positive women. The magnitude of dual contraceptive utilization in this study was, 38.1% (95% CI: 34.8–42.02). Place of residence, marital status of the respondent, educational status of the respondent, educational status of partner, and protect the sexual partner from acquiring HIV were the independent predictors of dual contraceptive utilization.
This research found dual contraceptive utilization (38.1%) to be consistent with the previous study in Bungoma Country, Kenya where dual contraceptive utilization among HIV-infected women attending ART clinics was (38.5%), Cameroon (33.3%), Tanzania (33%), and Soweto, South Africa (40%) [13,27-29].
However, the result in this study was higher than study conducted in Gebretsadik Shawo hospital (19.8%) Ethiopia, Adwa, Northern Ethiopia (13.8%), Bahir Dar, Northern Ethiopia (26.1%), Nekqement Western Ethiopia (22.4%), Tigray, Northern Ethiopia (21.6%), Lusaka (17.7%) Zambia, Nigeria(27.2%) [20,30-33]. The observed variation between the studies might be due to the differences in the socio-demographic characteristics of the participants included. Again, the inconsistency noted with studies from other countries may be attributable to the difference in the cultural characteristics of study participants, study period settings, and sample size.
Additionally, it is lower than the studies done in West Shoa, Oromia (59.5%), Mekelle Town (45.2%) Ethiopia, India (72%), USA(59%) [18,34-36]. The high dual contraceptive magnitude might be a result of the vigorous attempt to scale-up dual contraception uses by involving service providers and change in dual-protection counseling.
In this study respondents who resided in urban areas were less likely to utilize dual contraceptive methods when compared to a respondent who resided in rural areas. This finding is in line with a study conducted in Malawi [37]. However, this finding is typically different from the study conducted in the southern part of Ethiopia and Gonder, northern Ethiopia, and West Shoa, Central Ethiopia which revealed that HIV-positive urban women were more likely to use dual contraceptive methods than rural women [19,26,31]. Even if FP knowledge was evenly distributed in all residential areas, women who reside in rural areas show apparently positive behavioral change when counseled frequently by health professionals about the advantage of using dual contraceptive methods, in turn, making them use the method. In addition, there might be reluctance among women residing in urban areas to promote the use of dual contraceptive methods in their community, even though they are knowledgeable about the advantage of FP utilization.
This study also revealed the marital status of the women was one of the independent predictors to utilize the dual contraceptive method, respondents who had married were more than 3 times more likely to utilize a dual method of contraceptive when compared to their counterparts. This finding is comparable with finding from West Shoa, Central Ethiopia, Addis Ababa, Southwestern Uganda, Kenya, and Lusaka Zambia [26,38-41]. This may be because married women find it simpler to talk about contraception-related issues than single women. Moreover, WHO recommends male involvement, which is one of the health promotion strategies that can increase the utilization of maternal and child health services [42].
Educational status has been described as a key factor to utilize a dual method of contraceptive. A husband (partner) with formal education (primary and above) were more than 7 times more likely to utilize a dual method of contraceptive when compared to their counterparts. The finding is supported by studies done among HIV-positive women conducted in Gondar City, northwest Ethiopia; Borana, Southeast Ethiopia, EDHS, and also in Brazil [19,36,43,44]. This could be explained by highly educated women partners might appreciate the advantages of dual contraceptive use, have higher levels of HIV/AIDS, STI, and risky sexual practice knowledge, and able to discuss freely with their sexual partners and are less likely to have a stigma towards HIV/AIDS, which, in turn, assists them to easily change their risky sexual behavior.
Additionally, respondents who thoughts one of the advantages to disclose HIV serostatus is protecting sexual partners from HIV were significantly associated with dual contraceptive utilization. The possible explanation might be due to the reason on the degree of counseling provided by a health professional at the health facility level. This finding agrees with those reported in studies conducted in Hosanna Hospital, Southern Ethiopia; Gebretsadik Shawo Hospital, Ethiopia, and India [12,31,45].
Conclusion
The overall magnitude of dual contraceptive utilization among women on ART was found to be low when compared to WHO recommendation. Factors like Place of residence, marital status, husband's educational status, and respondents who thoughts one of the advantages to disclose HIV serostatus is protecting sexual partners from HIV were found to be significantly associated with dual contraceptive method utilization. Therefore, health facilities should emphasize the value of dual contraceptive use to all sexually active HIV-positive women to remove obstacles to dual method use and effort had to be taken to strengthen formal education (primary and above) attainment of a client partners who was HIV-positive. Furthermore, promoting thoughts on one of the advantages to disclose HIV serostatus is protecting sexual partners from HIV. Besides, conducting further exploratory research in the future study in this regard will be beneficial to provide a comprehensive understanding and how the way to most effectively promote the use of a dual contraceptive method.
Strength and Limitation of this Study
As to the strengths of this study, the respondents have been selected by random sampling technique with a relatively large sample size; therefore, the results of this study can be generalized to women attending health institutions inside the study area. Additionally, precautions have been taken in the selection of experienced data collectors. This study had a few limitations: As an interview survey, social desirability bias cannot be eliminated, and recall bias for some events might happen.
Declaration
Ethical Consideration
The letter of approval was obtained from the Salale University College of health science ethical review committee. Permission and support letter were written to a health facility that gives ART service. Then, heads of hospitals and health centers were communicated through formal letters from the North Shoa Zone health office in addition to personal communication by the investigator. Written consent was obtained from study participants for protecting autonomy and ensuring confidentiality. In the case of minors (participants below 18 years old), written assent was obtained from the minors themselves and their parents or guardians. Confidentiality was maintained by omitting their names and personal identification. Participant were told that they could decline at any time if they feel uncomfortable, even after the interview has started.
Acknowledgment
We would like to thank North Shoa Zone ART clinics site staff for their precious support in the provision of baseline vital information and their collaboration during the study conduct. We would also, like to thank the data collectors, supervisors and study participants.
Authors’ Contributions
Sisay Motuma Debela, Yohannes Mehretie Adinew, Leta Adugna Geleta, and Ararso Hordofa Guye designed the study. Sisay Motuma Debela obtained the data, analyzed and interpreted the data and obtained funding. Sisay Motuma Debela, Yohannes Mehretie Adinew, and Leta Adugna Geleta involved in analysis, reviewed and commented the entire of the paper from inception to end for its intellectual content. SM prepared the first draft of this manuscript. Finally, all authors have read and approved the final version of the manuscript to be published.
Availability of Data and Materials
All data generated and/or analyzed during the study are available from the corresponding author on reasonable request.
References
- World Health Organization. (2014). Hormonal contraceptive methods for women at high risk of HIV and living with HIV: 2014 guidance statement.
- Agboghoroma, C. O. (2011). Contraception in the Context of HIV/AIDS: A Review. African Journal of Reproductive Health, 15(3), 15-24.
- UNFPA. Preventing HIV and unintended pregnancies: strategic framework. 2015.
- Feyissa, T. R., Harris, M. L., Melka, A. S., & Loxton, D. (2019). Unintended pregnancy in women living with HIV in Sub-Saharan Africa: a systematic review and meta-analysis. AIDS and Behavior, 23, 1431-1451.
- UNAIDS. PREVENTION GAP REPORT [Internet]. 2016
- Stuart, G. S. (2009). Fourteen million women with limited options: HIV/AIDS and highly effective reversible contraception in sub-Saharan Africa. Contraception, 80(5), 412-416.
- Harvard Chan School Center of Excellence in Maternal and Child Health. Family Planning and Maternal Health –Maternal Health Task Force [Internet]. 2016
- Kaida, A., Laher, F., Strathdee, S. A., Money, D., Janssen, P. A., Hogg, R. S., & Gray, G. (2010). Contraceptive use and method preference among women in Soweto, South Africa: the influence of expanding access to HIV care and treatment services. PloS one, 5(11), e13868.
- WHO. PMTCT STRATEGIC VISION 2010–2015: PREVENTING MOTHER-TO-CHILD TRANSMISSIONOF HIV [Internet]. 2010
- Wilson, T. E., Koenig, L. J., Walter, E., Fernandez, I., & Ethier,K. (2003). Dual contraceptive method use for pregnancy and disease prevention among HIV-infected and HIV-uninfected women: the importance of an event-level focus for promoting safer sexual behaviors. Sexually transmitted diseases, 809-812.
- Hladik, W., Stover, J., Esiru, G., Harper, M., & Tappero, J. (2009). The contribution of family planning towards the prevention of vertical HIV transmission in Uganda. PloS one, 4(11), e7691.
- Chakrapani, V., Kershaw, T., Shunmugam, M., Newman, P. A., Cornman, D. H., & Dubrow, R. (2011). Prevalence of and barriers to dual-contraceptive methods use among married men and women living with HIV in India. Infectious diseases in obstetrics and gynecology, 2011.
- Schwartz, S. R., Rees, H., Mehta, S., Venter, W. D. F., Taha,T. E., & Black, V. (2012). High incidence of unplanned pregnancy after antiretroviral therapy initiation: findings from a prospective cohort study in South Africa. PloS one, 7(4), e36039.
- Munsakul, W., Lolekha, R., Kowadisaiburana, B., Roongpisuthipong, A., Jirajariyavej, S., Asavapiriyanont, S.,... & Martin, M. (2015). Dual contraceptive method use and pregnancy intention among people living with HIV receiving HIV care at six hospitals in Thailand. Reproductive health, 13, 1-11.
- Poudel, K. C., Tandukar, K. P., Nakahara, S., Yasuoka, J., & Jimba, M. (2011). Knowing the consequences of unprotectedsex with seroconcordant partner is associated with increased safer sex intentions among HIV-positive men in Kathmandu, Nepal. Journal of Health, Population, and Nutrition, 29(3), 191.
- Reta, M. M., Tessema, G. A., & Shiferaw, G. (2019). Prevalence of dual contraceptive use and associated factors among HIV positive women at University of Gondar Hospital, Northwest Ethiopia. BMC research notes, 12, 1-7.
- Demissie, D. B., Girma, T., & Abdissa, G. (2015). Dual contraceptive utilization and associated factors among people living with HIV attending ART clinic in Fitche Hospital, Ethiopia. J Health Med Nurs, 2015, 20.
- Demissie, D. B., & Gudisa, T. (2019). Dual contraceptive use and associated factors among women living with HIV attending art clinics in West Zone Health Facilities Oromia, Ethiopia. EC Gynaecol, 8(4), 143-55.
- Abay, F., Yeshita, H. Y., Mekonnen, F. A., & Sisay, M. (2020). Dual contraception method utilization and associated factors among sexually active women on antiretroviral therapy in Gondar City, northwest, Ethiopia: a cross sectional study. BMC Women's Health, 20(1), 1-9.
- Kebede, H. G., Ababa, A., Ababa, A., & Ababa, A. (2015). Assessment of contraceptive use and associated factors among HIV positive women in Bahir-Dar Town, Northwest Ethiopia. Open Access Library Journal, 2(10), 1.
- Molla, A. A., & Gelagay, A. A. (2017). Risky sexual practice and associated factors among HIV positive adults attending anti-retroviral treatment clinic at Gondar University Referral Hospital, Northwest Ethiopia. PloS one, 12(3), e0174267.
- Berhane, Y., Berhe, H., Abera, G. B., & Berhe, H. (2013). Utilization of modern contraceptives among HIV positive reproductive age women in Tigray, Ethiopia: a cross sectional study. International Scholarly Research Notices, 2013.
- Ginindza, T. G., Stefan, C. D., Tsoka-Gwegweni, J. M., Dlamini, X., Jolly, P. E., Weiderpass, E., ... & Sartorius, B. (2017). Prevalence and risk factors associated with sexually transmitted infections (STIs) among women of reproductive age in Swaziland. Infectious agents and cancer, 12(1), 1-12.
- Dejene, H., Abera, M., & Tadele, A. (2021). Unmet need for family planning and associated factors among married women attending anti-retroviral treatment clinics in Dire Dawa City, Eastern Ethiopia. PloS one, 16(4), e0250297.
- Chakraborty, N. M., Fry, K., Behl, R., & Longfield, K. (2016). Simplified asset indices to measure wealth and equity in health programs: a reliability and validity analysis using survey data from 16 countries. Global Health: Science and Practice, 4(1), 141-154.
- Tilahun, Y., Bala, E. T., Bulto, G. A., & Roga, E. Y. (2021). Dual contraceptive utilization and associated factors among reproductive-age women on anti-retroviral therapy at hospitals in central Ethiopia. Risk Management and Healthcare Policy, 619-627.
- Damian, D. J., George, J. M., Martin, E., Temba, B., & Msuya,S. E. (2018). Prevalence and factors influencing modern contraceptive use among HIV-positive women in Kilimanjaro region, northern Tanzania. Contraception and reproductive medicine, 3, 1-9.
- Mulongo, A. M., Lihana, R. W., Githuku, J., Gura, Z., & Karanja, S. (2017). Factors associated with uptake of dual contraception among HIV-infected women in Bungoma County, Kenya: a cross-sectional study. The Pan African Medical Journal, 28(Suppl 1).
- Tsafack, M. (2020). Dual contraception use and associated factors among HIV positive women follow-up at Treatment Center Unit of Yaounde Central Hospital, Cameroon. Open Access Library Journal, 7(05), 1.
- Lawani, L. O., Onyebuchi, A. K., & Iyoke, C. A. (2014). Dual method use for protection of pregnancy and disease prevention among HIV-infected women in South East Nigeria. BMC women's health, 14(1), 1-6.
- Erashi MWM. Dual-Contraceptive Method Utilization and Associated Factors among HIV Positive Women Attending Art Clinic in Gebretsadik Shawo Hospital. J Women’s Heal Care. 2015;4(6):1–5.
- Teklu, T., & Davey, G. (2008). Which factors influence North Ethiopian adults' use of dual protection from unintended pregnancy and HIV/AIDS?. The Ethiopian Journal of Health Development, 22(3).
- Sufa, A., Abera, M., & Admasu, B. (2013). Utilization of family planning methods and associated factors among women living with HIV attending ART clinics in Nekemte Public Health Facilities, East Wollega Zone, Ethiopia. Science, Technology and Arts Research Journal, 2(4), 71-77.
- Kalayu, H. (2017). Dual Contraceptive Use and Associated Factors among HIV Positive Women on Art Follow up In Mekelle Town Tigray, Ethiopia.
- Sutton, M. Y., Zhou, W., & Frazier, E. L. (2018). Unplanned pregnancies and contraceptive use among HIV-positive women in care. PloS one, 13(5), e0197216.
- Tsuyuki, K., Barbosa, R. M., & de Araujo Pinho, A. (2013). Dual protection and dual methods in women living with HIV: the Brazilian context. Journal of sexually transmitted diseases, 2013.
- Habte, D., & Namasasu, J. (2015). Family planning use among women living with HIV: knowing HIV positive status helps-results from a national survey. Reproductive health, 12(1), 1-11.
- Chibwesha, C. J., Li, M. S., Matoba, C. K., Mbewe, R. K., Chi, B. H., Stringer, J. S., & Stringer, E. M. (2011). Modern contraceptive and dual method use among HIV-infected women in Lusaka, Zambia. Infectious diseases in obstetrics and gynecology, 2011.
- Asfaw, H. M., & Gashe, F. E. (2014). Contraceptive use and method preference among HIV positive women in Addis Ababa, Ethiopia: a cross sectional survey. BMC Public Health, 14(1), 1-10.
- Muyindike, W., Fatch, R., Steinfield, R., Matthews, L. T., Musinguzi, N., Emenyonu, N. I., ... & Hahn, J. A. (2012). Contraceptive use and associated factors among women enrolling into HIV care in southwestern Uganda. Infectious diseases in obstetrics and gynecology, 2012.
- Njuguna, E., Ilovi, S., Muiruri, P., Mutai, K., Kinuthia, J., & Njoroge, P. (2017). Factors influencing the utilization of family planning services among HIV infected women in a Kenyan health facility. Int J Reprod Contracept Obstet Gynecol, 6(5), 1746-52.
- WHO. WHO recommendations on health promotion interventions for maternal and newborn health. 2015
- Amare, G., Cherie, N., & Mekonen, A. M. (2021). Dual contraceptive use and associated factors among reproductive age group on antiretroviral therapy in Borena District, Northeast Ethiopia: a cross-sectional study. HIV/AIDS-Research and Palliative Care, 107-114.
- Central Statistical A. Ethiopia demographic and health survey. 2016
- Jifar MS, Handiso TB MT and IS. (2017). Dual Contraceptive Utilization and Associated Factors among Human Immunodeficiency Virus (HIV) Positive Women Attending Anti Retro Viral Therapy (ART) Clinic in Hossana Hospital, Southern Ethiopia. SM J Gynecol Obs, 3(2):1–8


