Research Article - (2024) Volume 9, Issue 3
Comparative Effectiveness of Transcatheter Aortic Valve Replacement (TAVR) in Nonagenarians Compared with Younger Patients
2St. Joseph’s Hospital, USA
3University of South Florida, Morsani College of Medicine, USA
Received Date: Sep 27, 2024 / Accepted Date: Oct 23, 2024 / Published Date: Oct 30, 2024
Copyright: ©Â©2024 Pasquale Marotta, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Marotta, P., Vasaiwala, S., Lacombe, P., Klingel, K., Buchanan, S., et al. (2024). Comparative Effectiveness of Transcatheter Aortic Valve Replacement (TAVR) in Nonagenarians Compared with Younger Patients. Cardio Open, 9(3), 01-05.
Abstract
Background: TAVR has garnered worldwide acceptance as a suitable alternative to surgical AVR in many clinical situations, particularly in the elderly. Our goal was to study whether some of the known benefits from TAVR might be superseded by risks in the nonagenarian population [1].
Methods: Using Cox proportional hazards method, we retrospectively analyzed 1246 patients age > 50 years undergoing TAVR at our institution from the STS/ACC TVT database between 2010-2020. Patients age > 90 were compared with younger patients with coprimary endpoints of inpatient mortality and major bleeding requiring transfusion, 1-yr mortality, and 30-day all cause readmission.
Results: Baseline demographic, clinical characteristics, and unadjusted outcomes in primary endpoints are presented in Table 1. Primary endpoints did not differ across the two groups. Inpatient mortality (Odds Ratio 2.23 [0.62, 8.00]; p=0.22), 1-year mortality (HR 1.64 [0.78, 3.44]; p =0.19), and 30-day hospital readmission rates (HR 0.84 [0.39, 1.81]; p=0.66) were similar prior to and after adjustment for baseline differences.
Conclusions: In our study, no differences in hard clinical endpoints were detected between a younger and advanced aged population of patients treated with TAVR. Our study highlights that TAVR can be safely performed in patients of extreme age with clinical outcomes similar to a younger patient population when properly selecting patients for this procedure.
Keywords
TAVR, Nonagenarian, Aortic Stenosis, Heart Team, Quality of Life
Introduction
Transcatheter aortic valve replacement (TAVR) was initially introduced to treat patients with severe aortic valve stenosis (AS) at high risk for surgical aortic valve replacement (SAVR). TAVR has been shown to significantly reduce death rates from any cause in patients with severe aortic stenosis [1]. Results derived from randomized trials and observational studies proved TAVR as a reliable alternative to conventional SAVR in not only high-risk but also intermediate-risk patients with respect to the primary endpoint of death or disabling stroke [2,3]. Furthermore, TAVR has been found to extend beyond the scope of high and intermediate-risk surgical patients and is at the very least equivalent to SAVR in the treatment of low-risk surgical candidates when using a transfemoral approach in patients without bicuspid aortic valves [4].
TAVR has garnered worldwide acceptance as a suitable alternative to surgical AVR in many clinical situations, particularly in the elderly. As TAVR technology and techniques have improved, there has been a slow creep in the application of this therapy to patients of extreme age, those defined as age > 90 years. TAVR in the nonagenarian population has been shown to be performed safely under conscious sedation [5]. Randomized clinical trials evaluating TAVR versus SAVR were limited in the number of extreme elderly patients, especially those over the age of 90 years. Nevertheless, data from the younger subset are extrapolated to the very elderly population. We sought to compare the safety and effectiveness of TAVR in the nonagenarian age group compared to the younger subset of patients within the STS database at our institution. Our goal was to help clarify the current divergence in data regarding safety and efficacy of TAVR in the nonagenarian population.
Methods
Patient Population and Data Collection
Our study is a retrospective cohort study reviewing up to 2000 patients over age 50 contained within the STS/ACC TVT database from prior TAVR procedures performed at Maine Medical Center between the years 2010-2020. Cohorts (greater than or equal to 90 years old vs. less than 90 years old) included ultimate enrolment of 1246 patients. Patients who received alternative access via non-transfemoral approach were excluded.
Study Endpoints
End points were selected using the Standardized Aortic Valve Clinical Research Endpoints as determined by the Valve Academic Research Consortium (VARC) [6]. The primary endpoints of our study were inpatient mortality, one-year mortality, inpatient major bleeding events requiring transfusion, and 30-day hospital readmission rate. QOL was assessed with the 12-item Kansas City Cardiomyopathy Questionnaire (KCCQ- 12), a 12-item condensed version of the full KCCQ [7].
Statistical Analysis
Baseline characteristics of the study population as well as in-hospital outcomes were presented according to the age. Categorical variables were summarized as percentages and continuous variables as medians with interquartile ranges (IQRs). The baseline characteristics and in- hospital outcomes of patients ≥ 90 and < 90 years of age were then compared using the Pearson chi-square test for categorical variables and the Wilcoxon rank sum test or Student t-test as appropriate for continuous variables. Data and primary endpoints were analysed using Cox proportional hazards method via STATA 16 (StataCorp. 2019. Stata Statistical Software: Release 16. College Station, TX: StataCorp LLC).
Results
Patient Cohort
From January 2012 through December 2020, 1,242 patients underwent transfemoral TAVR in this single centre study, of which 86 were nonagenarians. The median age was 91 years in nonagenarians and 80 years in the younger cohort. Compared to patients under age 90, nonagenarians were more likely to be non-smokers and overweight and less likely to have co-morbid conditions including hypertension and diabetes (Table 1). Otherwise, clinical profiles including known CAD, pre-operative cardiomyopathy or recent heart failure, NYHA functional class and quality of life as assessed by KCQ-12 were comparable.
|
|
Age <90 (n= 1,160) |
Age ≥90 (n=86) |
P value |
|
Gender (male) |
671 (53.9) |
55 (64.0) |
0.268 |
|
Height, cm |
167.2 ± 10.9 |
165.5 ± 9.5 |
0.1725 |
|
Weight, kg |
83.4 ± 20.6 |
70.5 ± 12.3 |
a<0.001 |
|
Race (White) |
1,156 (99.6) |
85 (98.8) |
0.247 |
|
Patient History |
|||
|
Smoker |
65 (5.6) |
0 (0.0) |
a0.024 |
|
Hypertension |
1,059 (91.3) |
72 (83.7) |
a0.019 |
|
Diabetic |
480 (41.4) |
18 (20.9) |
a<0.001 |
|
Pre-operative dialysis |
26 (2.2) |
0 (0.0) |
0.161 |
|
Coronary Artery Disease |
|
|
0.819 |
|
Asymptomatic |
4 (0.3) |
0 (0.0) |
|
|
Stable Angina |
990 (85.3) |
75 (87.2) |
|
|
Unstable Angina |
123 (10.6) |
8 (9.3) |
|
|
Non-ST Elevation MI |
31 (2.7) |
3 (3.5) |
|
|
ST Elevation MI |
12 (1.0) |
0 (0.0) |
|
|
Pre-op Cardiomyopathy |
19 (1.6) |
1 (1.2) |
0.733 |
|
Heart Failure (HF) prior 2 weeks |
653 (56.3) |
51 (59.3) |
0.587 |
|
Clinical Profile |
|||
|
New York Heart Association functional class |
|
|
0.782 |
|
I |
52 (4.5) |
5 (5.8) |
|
|
II |
420 (36.2) |
28 (32.6) |
|
|
III |
532 (45.9) |
39 (45.4) |
|
|
IV |
156 (13.5) |
14 (16.3) |
|
|
Kansas City Questionnaire-12 (KCQ-12) |
50.84 ± 23.81 |
52.99 ± 22.18 |
0.4290 |
|
Values are n (%), mean ± SD, or median (IQR), unless otherwise indicated. aP <0.05. |
|||
Table 1: Baseline Clinical Variables
Primary Endpoints
Primary endpoints did not differ across the two groups. (Table 2). Inpatient mortality (Odds Ratio 2.23 [0.62, 8.00]; p=0.22), 1-year mortality (Hazard Ratio 1.64 [0.78, 3.44]; p =0.19), and 30-day hospital readmission rates (Hazard Ratio 0.84 [0.39, 1.81]; p=0.66) were similar prior to and after adjustment for baseline differences. Nonagenarians also experienced similar rates of inpatient major bleeding events requiring transfusion compared to those under the age of 90 years old.
|
|
Age <90 (n= 1,160) |
Age ≥90 (n=86) |
P value |
|
Primary Endpoints |
|||
|
Inpatient Mortality |
17 (1.5) |
3 (3.5) |
0.15 |
|
1-year Mortality |
83 (7.2) |
8 (9.3) |
0.46 |
|
Inpatient Major Bleeding Event |
51 (4.4) |
2 (2.33) |
0.36 |
|
30-day hospital readmission rate |
130 (11.2) |
7 (8.1) |
0.38 |
|
Values are n (%), mean ± SD, or median (IQR), unless otherwise indicated. aP <0.05. |
|||
Table 2: Unadjusted Clinical Outcomes
Post-Discharge Outcomes
Observed stroke rate/aortic valve re-intervention/myocardial infarction at 30-days and one-year were similar between groups. NYHA class improved to Class I for 72.6% of nonagenarians compared to 64% of their younger counterparts although not statistically significant. (p=0.144) (Table 3). Nonagenarians were more likely to be discharged to extended care/TCU/ rehabilitation or nursing home facilities. (p<0.001) (Table 3).
|
|
Age <90 |
Age ≥90 |
P value |
|
Discharged to Facility (N=1,242) |
174 (15.1%) |
27 (31.4%) |
<0.001 |
|
NYHA class (N= 1,219) |
|
|
0.144 |
|
HF Class I |
720 (63.4%) |
61 (72.6%) |
|
|
HF Class II |
353 (31.1%) |
17 (20.2%) |
|
|
HF Class III |
55 (4.9%) |
6 (7.1%) |
|
|
HF Class IV |
7 (0.62%0 |
0 (0.0%) |
|
|
Values are n (%), mean ± SD, or median (IQR), unless otherwise indicated. aP <0.05. |
|||
Table 3: Post Discharge and NYHA Class 30-Day Follow-up
Quality of Life
Nonagenarians had a lower mean 30-day KCQ-12 score compared with younger patients (69.6 vs. 73.4) although not statistically significant. (p=0.192) This score recovered for those over 90 by 1-year follow-up. (76.5 vs. 74.2, p=0.957) (Table 4).
|
|
Age <90 |
Age ≥90 |
P value |
|
KCQ-12 |
|
|
|
|
Score 30 days |
73.5 ± 22.3 |
69.6 ± 24.3 |
0.192 |
|
Score 1 year |
74.2 ± 23.2 |
76.5 ± 17.62 |
0.957 |
|
Values are n (%), mean ± SD, or median (IQR), unless otherwise indicated. aP <0.05 |
|||
Table 4: KCQ-12 Scores at Follow-Up
Discussion
Several studies have looked at the long-term mortality and quality of life outcomes in these patients, which demonstrate that older age does not predict poor clinical outcomes after TAVR and may improve quality of life for non-frail patients [8- 11]. Contrary to this, a Swiss study detailed a linear relationship between age and mortality, stroke, and pacemaker implantation following TAVR. However, standardized mortality ratios were found to be lower for those patients greater than 90 years old [12]. Furthermore, another recent study showed higher 30- day and one-year mortality in nonagenarians compared to their younger counterparts, but again found lower observed to expected mortality with similar improvements in quality of life. (QOL) [13].
Based on the limited TAVR data available in nonagenarians, there appears to be an acceptable survival benefit along with improvement in quality of life despite higher burden of comorbidities and frailty. Our study seeks to add to this collection through a single set of retrospective data from Maine Medical Center within the STS (Society for Thoracic Surgeons (STS) / ACC (American College of Cardiology) TVT (Transcatheter Valve Therapy) registry focused on the years 2010-2020. This retrospective study analysing TAVR procedures performed at our centre in recent years included roughly 7% nonagenarians sought to compare short and mid-term outcomes between age groups. Nonagenarians included in this study had fewer comorbidities than their younger counterparts, highlighting the underlying meticulous selection process for those to undergo the procedure. Outside of extremely advanced age, nonagenarians included had similar rates of underlying coronary disease, heart failure, and indices of quality of life prior to TAVR placement. Our findings show these carefully chosen non-frail nonagenarians exhibited similar rates of adverse outcomes regarding inpatient major bleeding events, 30-day hospital re-admission rate, as well as inpatient, 30-day and 1-year follow-up mortality. This further confirms TAVR is a viable option in nonagenarians with severe aortic stenosis using a multi-disciplinary collaborative approach to individualized patient decision making.
There have been multiple single centre studies with small patient cohorts reported over the last 10 years [11,14-17]. Given limited insights available due to scant data, larger studies were conducted including outcomes reported post-hoc from the PARTNER-1 trial, the international French National Transcatheter Aortic Valve Implantation Registry (FRANCE-2) and American STS/ TVT database. The post hoc PARTNER-1 analysis reported a 4.0% 30-day mortality rate in nonagenarians receiving TAVR via transfemoral approach [10]. The FRANCE-2 dataset demonstrated an 11.2% 30-day mortality rate in nonagenarians, which after adjustment for baseline differences, yielded no significant difference with early or late octogenarians [5]. Of note, the STS/TVT registry analysis between 2011-2014 reported worse 30-day mortality rates in nonagenarians (≥90 vs. <90 years: 30-day: 8.8% vs. 5.9%, p<0.001), although were similar when adjusted for observed to expected mortality ratios given elevated nonagenarian STS Predicted Risk of Mortality (PROM) (10.9% vs. 8.1%; p<0.001) [13].
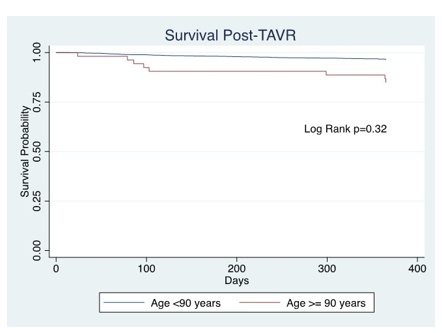
Figure 1: Survival Post-TAVR "When adjusted for baseline differences, Kaplan-Meier curve showed no significant difference in mortality at 1 year"
Our study showed inpatient mortality to be similar between nonagenarians compared to their younger counterparts (3.5% vs. 1.5%) as well as 30-day mortality (4.65% vs. 1.90%). Compared to aforementioned studies, lower 30-day mortality rates were observed which may reflect selective patient decision making as well as optimization of procedural methods/device development over time. Despite improved nonagenarian mortality, absolute rates remain higher than those in their younger counterparts receiving TAVR. Nonetheless, a continued decreasing trend in mortality within nonagenarians is reassuring, even surpassing previously published mortality rates for octogenarians from FRANCE-2 as well as German TAVI registries [5,17]. Therefore, given derived benefits including improved NYHA class and quality of life, observed mortality rates may be acceptable within the nonagenarian population eligible for TAVR.
Longer term survival in our patient cohort yielded no statistical significance in 1-year mortality rates between nonagenarians and their younger peers (9.3% vs. 7.2%). Notably, the 2015 STS/ TVT study did show a statistical difference in mortality between groups (10.9% vs. 8.1%), which normalized after adjustment for observed to expected mortality ratios. Similarly, the FRANCE-2 dataset also demonstrated no significant difference in one year mortality after adjustment for baseline differences between octogenarians age 80-84 (19.8%) or 85-89 (26.1%) with nonagenarians (27.7%) Notably, the lower mortality rates seen at 30-days in our patient cohort sustained through 1-year follow-up, highlighting decreased mortality rates compared to those reported in prior studies and a larger gap between the same age general population mortality (median age 91; male 20.3%; female 16.4%) [18,19]. This confirms prior reported acceptable outcomes in select nonagenarians highlighting that raw differences in mortality compared to younger patients may not be of clinical significance.
Of note, there were various in-hospital complications noted to be more prominent in the nonagenarian group in the 2015 STS/ TVT study which included major bleeding events and need for blood transfusion. Our study showed no statistical difference regarding haemorrhagic events between age groups however, nonagenarians remained more likely to require discharge to an extended care or rehabilitation facility. Nonetheless, an important factor to consider in TAVR outcomes remains overall effect on functional capacity and quality of life. The 2015 STS/TVT study found a significant increase in KCQ scores by 30 days but noted significantly lower nonagenarian results. These differences in quality of life vanished between groups by 1-year post-TAVR. The post hoc review of the PARTNER trial also demonstrated improvement of QOL, reported to stabilize by 6 months after TAVR in nonagenarians [10]. Our study corroborated these findings, with initially lower KCQ-12 scores improving by 1-year post procedure. Overall, this verifies the previously reported observation regarding longer nonagenarian recovery time, however with adequate time suggests those of extreme age make significant gains back to meaningful functional status.
Limitations
As this is a retrospective study, our ability to obtain complete there was some loss to follow-up. Additionally, the retrospective nature of this analysis had inherent unmeasured confounding, which was adjusted for in statistical analysis as described above.
Conclusions
In our study, no differences in hard clinical endpoints were detected between a younger and advanced aged population of patients treated with TAVR. Our study highlights that TAVR can be safely performed in patients of extreme age with clinical outcomes similar to a younger population when properly selecting patients for this procedure.
Disclosure Statement
Samip Vasaiwala, MD reports a consulting and advisory relationship with Abbott Vascular Inc and Boston Scientific Corp as well as is on the speaker’s bureau at Shockwave Medical Inc and AbioMed Inc. Scott Buchanan, MD reports a relationship with Edwards as an alternative access proctor. All other authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper. No grant support for this research was provided.
References
- Mack, M. J., Leon, M. B., Smith, C. R., Miller, D. C., Moses,J. W., Tuzcu, E. M., ... & Akin, J. (2015). 5-year outcomes of transcatheter aortic valve replacement or surgical aortic valve replacement for high surgical risk patients with aortic stenosis (PARTNER 1): a randomised controlled trial. The Lancet, 385(9986), 2477-2484.
- Winter, M. P., Bartko, P., Hofer, F., Zbiral, M., Burger, A., Ghanim, B., ... & Goliasch, G. (2020). Evolution of outcome andcomplications in TAVR: a meta-analysis of observational and randomized studies. Scientific reports, 10(1), 15568.
- Leon, M. B., Smith, C. R., Mack, M. J., Makkar, R. R.,Svensson, L. G., Kodali, S. K., ... & Webb, J. G. (2016). Transcatheter or surgical aortic-valve replacement in intermediate-risk patients. New England Journal of Medicine, 374(17), 1609-1620.
- Mack, M. J., Leon, M. B., Thourani, V. H., Makkar, R., Kodali,S. K., Russo, M., ... & Smith, C. R. (2019). Transcatheter aortic-valve replacement with a balloon-expandable valve in low-risk patients. New England Journal of Medicine, 380(18), 1695-1705.
- Yamamoto, M., Mouillet, G., Meguro, K., Gilard, M., Laskar, M., Eltchaninoff, H., ... & FRANCE-2 Registry Investigators. (2014). Clinical results of transcatheter aortic valve implantation in octogenarians and nonagenarians: insights from the FRANCE-2 registry. The Annals of thoracic surgery, 97(1), 29-36.
- VARC-3 Writing Committee, Généreux, P., Piazza, N., Alu,M. C., Nazif, T., Hahn, R. T., ... & Leon, M. B. (2021).Valve Academic Research Consortium 3: updated endpoint definitions for aortic valve clinical research. JACC, 77(21), 2717-2746.
- Spertus, J. A., & Jones, P. G. (2015). Development and validation of a short version of the Kansas City Cardiomyopathy Questionnaire. Circulation: Cardiovascular Quality and Outcomes, 8(5), 469-476
- Kleczynski, P., Dziewierz, A., Bagienski, M., Rzeszutko, L., Sorysz, D., Trebacz, J., ... & Dudek, D. (2016). Long-Term Mortality and Quality of Life After Transcatheter Aortic Valve Insertion in Very Elderly Patients. The Journal of invasive cardiology, 28(12), 492-496.
- Saito, Y., Lewis, E. E., Raval, A., Gimelli, G., Jacobson, K. M., & Osaki, S. (2021). The prognosis of elderly patients with aortic stenosis after transcatheter aortic valve replacement. Internal Medicine, 60(4), 517-523.
- Thourani, V. H., Jensen, H. A., Babaliaros, V., Kodali, S. K., Rajeswaran, J., Ehrlinger, J., ... & Mack, M. (2015). Outcomes in nonagenarians undergoing transcatheter aortic valve replacement in the PARTNER-I trial. The Annals of thoracic surgery, 100(3), 785-793.
- Mack, M. C., Szerlip, M., Herbert, M. A., Akram, S., Worley,C., Kim, R. J., ... & Holper, E. M. (2015). Outcomes of treatment of nonagenarians with severe aortic stenosis. The Annals of thoracic surgery, 100(1), 74-80.
- Attinger-Toller, A., Ferrari, E., Tueller, D., Templin, C., Muller, O., Nietlispach, F., ... & Stortecky, S. (2021). Age- related outcomes after transcatheter aortic valve replacement: insights from the SwissTAVI registry. Cardiovascular Interventions, 14(9), 952-960.
- Arsalan, M., Szerlip, M., Vemulapalli, S., Holper, E. M., Arnold, S. V., Li, Z., ... & Mack, M. J. (2016). Should transcatheter aortic valve replacement be performed in nonagenarians? Insights from the STS/ACC TVT Registry. Journal of the American College of Cardiology, 67(12), 1387-1395.
- Kayatta, M. O., Thourani, V. H., Jensen, H. A., Condado, J. C., Sarin, E. L., Kilgo, P. D., ... & Babaliaros, V. C. (2015). Outcomes for transcatheter aortic valve replacement in nonagenarians. The Annals of Thoracic Surgery, 100(4), 1261-1267.
- Noble, S., Frangos, E., Samaras, N., Ellenberger, C., Frangos, C., Cikirikcioglu, M., ... & Roffi, M. (2013). Transcatheter aortic valve implantation in nonagenarians: effective and safe. European journal of internal medicine, 24(8), 750-755.
- Akin, I., Kische, S., Paranskaya, L., Schneider, H., Rehders, T. C., Turan, G. R., ... & Ince, H. (2012). Morbidity and mortality of nonagenarians undergoing CoreValve implantation. BMC cardiovascular disorders, 12, 1-6.
- Yamamoto, M., Meguro, K., Mouillet, G., Bergoend, E., Monin, J. L., Lim, P., ... & Teiger, E. (2012). Comparison of effectiveness and safety of transcatheter aortic valve implantation in patients aged≥ 90 years versus< 90 years. The American journal of cardiology, 110(8), 1156-1163.
- Buellesfeld, L., Gerckens, U., Erbel, R., Zahn, R., Linke, A., Sievert, H., ... & Grube, E. (2012). Age-stratified baseline and outcome characteristics of patients undergoing transcatheter aortic valve implantation: results from the German multicenter registry. The Journal of invasive cardiology, 24(10), 531-536.
- Administration SS. Period life table for the Social Security area population. 2020.




