Case Report - (2024) Volume 2, Issue 2
Cage Extrusion after Cervical Discectomy and Fusion: Case Report
2Department of Neurosurgery, Hopital des Specialites, Faculty of Medicine and Pharmacy, Mohammed V University, Rabat, Morocco
Received Date: Jun 28, 2024 / Accepted Date: Jul 30, 2024 / Published Date: Aug 02, 2024
Copyright: ©©2024 Yao Christian Hugues Dokponou, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Mohcine, S., El Kacemi, I., Dokponou, Y. C. H., Obame, F. O., El Asri, C., et al. (2024). Cage Extrusion after Cervical Discectomy and Fusion: Case Report. J Neuro Spine, 2(2), 01-04.
Abstract
Anterior cervical discectomy and fusion (ACDF) with cages has become the standard treatment for cervical disc hernia- tion. Several surgical techniques have been developed that have proven effective, but the results are not without serious and sometimes fatal complications. Symptoms can vary in severity, from mild to severe, and even life-threatening. We report a rare case of delayed cervical cage migration in a 54-year-old patient admitted for cervical pain associated with dysphagia. A cervical x-ray showed implant ejection at the C6-C7 level. In this case report, we discuss the clinical and radiological features of this unusual complication and attempt to identify technical reasons and ultimately raise awareness of this complication.
Keywords
Anterior Cervical Discectomy and Fusion, ACDF, Dysphagia, Implant Migration, Cage ExtrusionIntroduction
A herniated disc is a common cause of neck pain in adults. The severity of the disease can range from mild to severe and even life-threatening. Medical treatment is generally limited to mild cases. However, more severe or progressive symptoms require surgical treatment [1,4]. Several technical modifications have been developed. Anterior cervical discectomy and fusion (ACDF), introduced in 1955, offered promising results for the treatment of this pathology [2,3]. The procedure aims to decompress the nervous components, restore lordosis, and achieve bone fusion. Over the years, this procedure has been continuously improved and is now a highly reliable treatment modality that provides pain relief, improvement in neurological symptoms, and high patient satisfaction in both short- and long¬term follow-up [5-7]. Complications after anterior cervical spine surgery are rare, particularly cage migration. In this interesting report, we present a 54-year-old man who presented with delayed dysphagia 9 months after an anterior cervical discectomy and fusion. To our knowledge, this case report of delayed migration has not been reported.
Case Presentation
The patient is a 54-year-old man with no significant medical history who presented with progressive neck pain and worsening symptoms of myeloradiculopathy for several years. On examination, he demonstrated full motor strength and objective sensation in both the upper and lower extremities. Hyperreflexia was observed diffusely in the bilateral upper extremities. No other upper or lower motor neuron signs were noted.
Magnetic resonance imaging (MRI) suggested a herniated disc with bilateral foraminal stenosis at the C6–C7 level. Surgical intervention was chosen and the patient underwent anterior cervical discectomy and cage fusion. His postoperative period was uneventful. Nine months later, he was admitted with delayed dysphagia and intermittent breathing difficulties without neurological deficits.
ENT examination with laryngoscopy revealed no lesions or swelling in the nasopharynx, hypopharynx, or larynx. Cervical radiographs showed migration of the cervical cage at the C6-C7 level (Figure 1). The patient had a surgical removal of the migration cage, which was then replaced with a new one (Figure 2). The patient did well postoperatively, remained in the hospital for a few days for immediate postoperative follow-up, and was discharged home asymptomatic a week later.
Figure 1: Cervical Spine X-ray showing Migration of C6C7 Arthrodesis Material
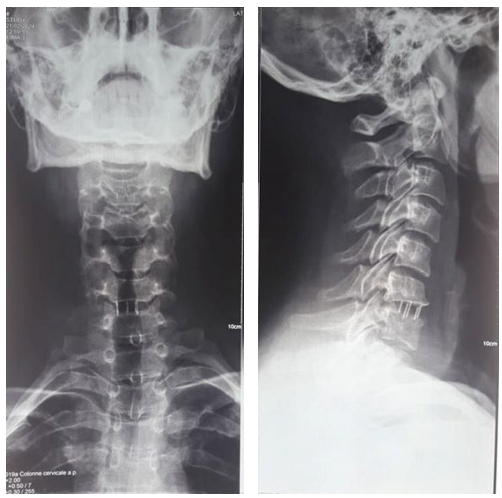
Figure 2: Cervical Spine X-ray showing Replacement of C6C7 Arthrodesis Material
Discussion
Anterior interbody fusion of the cervical spine (ACDF) with cages has become the gold standard for the treatment of intervertebral disc disease. ACDF cage extrusion is a rare complication, and the incidence of which is estimated to be less than 1% [8]. The consensus is that implant migration is due to implant malpositioning and/or poor fixation. Smith et al. identified 11 cases of implant extrusion out of 8,887 cases studied and attributed them to long complex constructs spanning three or more levels and located at the cervicothoracic junction, placing high stress on the implants and resulting in displacement [9]. In our case, we believe that both the cage height and its proximity to the cervicothoracic junction contributed to cage migration despite immobilization with a cervical collar.
Anterior displacement of the implant can cause dysphagia and difficulty breathing due to the mass effect. In addition, the chronic pressure of the implants can lead to pressure necrosis and erosion of the implants into the pharynx, as other authors reported [10]. This may be considered to place this patient at risk of catastrophic respiratory compromise or the development of a severe infection with acute decompensation. Fountas et al. reported a patient who underwent C5–C6 ACDF and presented with severe dysphagia 16 months postoperatively [11]. Imaging showed implant pullout. The patient then had the hardware removed; However, the fourth locking expansion screw was not found during surgery but was located later on abdominal imaging. Another case described a patient who presented with acute-onset odynophagia three years after C5–C6 ACDF and was found to have extruded a lower locking screw into the hypopharynx, which was removed with forceps under anesthesia. Oral expectoration by anterior cervical discectomy and fusion cage or screws was also reported [1]. Nevertheless, there were more serious and life-threatening complications in some cases: Fujibayashi et al. reported a suspected migration of the cervical plate and its screws through the gastrointestinal tract, which occurred unknowingly after extrusion, as there was no imaging evidence of the inserted implants and the patient never underwent surgical removal [12].
However, Riew et al. report a patient who suffocated due to respiratory impairment after coughing up the anterior cervical plate and died three days after the operation [13]. Therefore, radiological intraoperative and postoperative follow-up is of undeniable importance. It is not clear how many months patients must wear the cervical collar to avoid postoperative material extrusion.
Conclusion
Implant ejection is a rare and uncommon but serious complication that may involve pain, swelling, and difficulty swallowing. Obtaining orthogonal radiographs is crucial for the routine follow-up of postoperative ACDF patients, especially if dysphagia persists or suddenly worsens. Significant morbidity can be prevented through early detection of implant displacement.
Disclosures
The authors have nothing to disclose.
Funding
No funding was received for this research.
Conflict(s) of Interest
The authors report no conflicts of interest.
Acknowledgments
None
Authors' Contributions
Yao Christian Hugues Dokponou: Conceptualization, writing draft, reviewing and editing, visualization, supervision, validation, methodology.
Salami Mohcine: Writing, review & editing.
Fresnel Ontsi Obame: Writing, review & editing.
Inas El Kacemi: Writing & editing.
Abad Cherif El Asri: Writing & editing.
Miloud Gazzaz: Supervision, Validation, & review.
References
- Prusick, P. J., Sabri, S. A., & Kleck, C. J. (2021). Expectoration of anterior cervical discectomy and fusion cage: a case report. Journal of Spine Surgery, 7(2), 218.
- Kalsi-Ryan, S., Karadimas, S. K., & Fehlings, M. G. (2013). Cervical spondylotic myelopathy: the clinical phenomenon and the current pathobiology of an increasingly prevalent and devastating disorder. The Neuroscientist, 19(4), 409-421.
- Toledano, M., & Bartleson, J. D. (2013). Cervical spondylotic myelopathy. Neurologic clinics, 31(1), 287-305.
- Sadasivan, K. K., Reddy, R. P., & Albright, J. A. (1993). The natural history of cervical spondylotic myelopathy. The Yale journal of biology and medicine, 66(3), 235.
- Smith, G. W., & Robinson, R. A. (1958). The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. JBJS, 40(3), 607-624.
- HERZBERGER, E. E., CHANDLER, A., BEAR, N. E., &KINDSCHI, L. G. (1962). Anterior interbody fusion in the treatment of certain disorders of the cervical spine. Clinical Orthopaedics and Related Research®, 24, 83-93.
- Ra, R. (1955). Anterolateral cervical disc removal and interbody fusion for cervical disc syndrome. Bull Johns Hopkins Hosp, 96, 223-224.
- Buttermann, G. R. (2018). Anterior cervical discectomy and fusion outcomes over 10 years: a prospective study. Spine, 43(3), 207-214.
- Smith, G. A., Pace, J., Corriveau, M., Lee, S., Mroz, T. E., Nassr, A., ... & Steinmetz, M. P. (2017). Incidence and outcomes of acute implant extrusion following anterior cervical spine surgery. Global spine journal, 7(1_suppl), 40S-45S.
- Geyer, T. E., & Foy, M. A. (2001). Oral extrusion of a screw after anterior cervical spine plating. Spine, 26(16), 1814-1816.
- Fountas, K. N., Kapsalaki, E. Z., Machinis, T., & Robinson,J. S. (2006). Extrusion of a screw into the gastrointestinal tract after anterior cervical spine plating. Clinical Spine Surgery, 19(3), 199-203.
- Fujibayashi, S., Shikata, J., Kamiya, N., & Tanaka, C.(2000). Missing anterior cervical plate and screws: a case report. Spine, 25(17), 2258-2261.
- Riew, K. D., Sethi, N. S., Devney, J., Goette, K., & Choi,K. (1999). Complications of buttress plate stabilization of cervical corpectomy. Spine, 24(22), 2404.