Research Article - (2024) Volume 2, Issue 1
Assessment of Knowledge, Attitude and Practice of Antibiotic Resistance among Medical Student at Al-Zaiem Al-Azhari University, December 2021-July 2022
2Department of microbiology, Faculty of Medicine, Al-Zaiem AlAzhari University, Sudan
Received Date: Dec 22, 2023 / Accepted Date: Jan 10, 2024 / Published Date: Jan 24, 2024
Copyright: ©Ã?©2024 Mustafa Magbol, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Magbol, M., Osman, M. F. M., Ahmed, M. A. A. M., Alneama, M. A. B., Hassieb, M. A. A. (2024). Assessment of Knowledge, Attitude and Practice of Antibiotic Resistance among Medical Student at Al-Zaiem Al-Azhari University, December 2021-July 2022. Int Internal Med J, 2(1), 01-06.
Abstract
Background: The issue of antibiotic resistance has become a global public health concern, with an extensive clinical and economic burden. In this context, health professionals play a key role in the fight against antibiotic resistance because they play a part in prescribing antibiotics during routine clinical practice.
Objectives: to study assessing knowledge, attitude and practice of antibiotic resistance among medical students.
Methods: An observational cross-sectional facility-based study was done during period from December 2021 to June 2022 on medical students of AAU. The sample size of the study was 285 By Stratified random sampling technique, according to their academic year then the sample selected randomly from each strata. The data was collected by using electronic structured questionnaire by Google form. Then after collected the data we analysis by SPSS version 25.
Result: A total sample of 285 participants were collected. 93% of participants heard about antibiotic resistance. Regarding knowledge, and 91, 9% of participants defined antibiotic resistance as the ability of bacteria & other microorganisms to resist the effects of an antibiotic to which they were once sensitive and about spread of resistance, only 26.7% agree that antibiotic resistance bacteria can spread from animals to human. Regarding the attitude, 84.2% considered that antibiotic resistance is a problem and 89.5% stated that taking antibiotic correctly reduce the risk of antibiotic resistance. Regarding the practice, 51. 6% of students sometimes stop taking antibiotic course after improvement of symptoms and 56,1% get a prescription before starting antibiotics.
Conclusion: This study showed that medical students had good knowledge concerning antibiotic resistance with exception about spread of antibiotic resistance, good attitude and moderate practice. So improvements in antibiotic usage and prescribing must be made in the medical curriculum for undergraduate students to reduce the emergence of antibiotic resistance.
Keywords
Antibiotic, Antimicrobial Resistance.
Abbreviations
AAU: Al-Zaiem Al-Azhari University
AB: Antibiotic; ABR: Antibiotic resistance
AMR: Antimicrobial resistance
AMU: Antimicrobial use
Background
Antibiotics are medicines used to prevent and treat bacterial infections that infect humans and animals. Bacteria change in response to antibiotics use is called antibiotic resistance (ABR) which eliminate or restrict the therapeutic actions of antibiotics [1]. Which currently became a global health problem not merely increased morbidity and mortality but also affecting economic situations. The percentage of acquiring ABR infections is increasing day by day worldwide with 2.8 million people infected annually in U.S.A. With 35.000 death per year [2,3].
Naturally microorganisms have the capability of being antimicrobial resistance (AMR). Which mean that generation of a microorganism that no longer responds to antimicrobials. In appropriate prescriptions of antibiotics, substandard medications, poor infections control, being within the reach of all people (over the market) , mixing bacterial and viral infections, self-medication by the patient, patients demand and lack of awareness about AMR and its consequences among health-care workers and the general population for antibiotics are all found to be the determining factor for development and expansions of antibiotics resistance. . All health-care professionals have a pivotal role to play in controlling AMR and preserving the efficacy of antibiotics. The World Health Organization's Global Action Plan on AMR highlights the importance of training health professions. Therefore, educational training to both health professions and public regarding AMR and its consequences, rational use of antibiotics, and control measures of AMR must be promoted. Hence the medical students, who are the future doctors and key stakeholders of the health- care system. The major move toward the training of health-care professionals is at the undergraduate level. They must be made fully aware of challenges posed by AMR, responsible use and prescription of antibiotics, and various preventive measures to combat AMR. It is important to scrutinize the baseline knowledge of medical students for proper development and implementation of a highly effective training program on antibiotic use and controlling measures of AMR [4].
Hence, the present study aimed at evaluating knowledge, attitude and practice of Antibiotic resistance among medical students. Antibiotic resistance is one of the public health problem in a low income setting in Africa. This study is intended to be part of raising awareness and education about antibiotic resistance in Sudan by assessing the knowledge of medical students towards it. Extensive studies were published around the world. However, in Sudan, there is a little published papers of awareness about antibiotic resistance. Our study is aim to reduce the major health problems resulting from the unaware activities of the medical field and the study can be a reference for future research.
Study Design and Population
A descriptive cross sectional study was conducted in Alzaeim Alazhari University in Khartoum state, Sudan during the period from November 2021 to June 2022 The sample size calculated by the following formula at the confidence level of 95% and degree of precision 0.05. n=N÷1+N(d)²,n-> sample size ,N->population size ,d-> level of precision.
The total population (N) = 985, so when we applied the formula the sample size (n) was equal to 285 undergraduate medical students of Alzaeim Alazhari University selected By Stratified random sampling technique. The medical students were divided into 5 strata (according to their academic year) then the sample was selected randomly from each strata. So after dividing (n) on the 5 strata we studied this study on 57 students from batch [24] ,65 from batch [25], 60 from batch [26] ,54 from batch [27] and 49 from batch [28] total sample size equal 285 students data was collected through electronic self-structured Questionnaire by Google form
Statistical Analysis
We used SPSS version 25 to analyze the collected data, and print it in graphs and frequency tables, and then statistical test was done to examine knowledge, attitude, and practice about antibiotic resistance
The Results
A total sample of 285 participants were collected. 20% were batch 24, 22.8% were batch 25, 21.1% were batch 26 while 18.9% batch 27 and 17.2% batch 28.
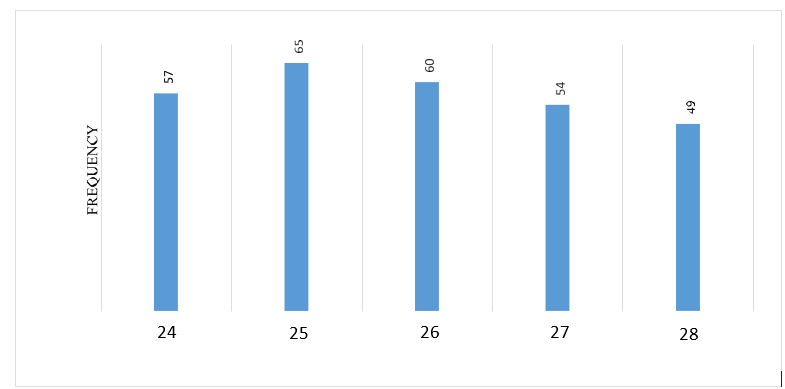
Figure 1: Participants Batch
7% of participants did not know about antibiotics resistance while 93% of participants did know about it
Participant’s Knowledge
91.9% of participants believe that biotic resistance is the ability of bacteria & other microorganisms to resist the effects of an antibiotic to which they were once sensitive while 3.5% is the ability of viruses to resist the effect of an antibiotic to which they were once sensitive and 4.6% do not know. 26% of participants believe the cause is the Use of antibiotic without medical prescription, 0.7% is the stop the medication suddenly, and 4.2% is the uncompleted course while 65.3% is all of mentioned reasons. 94.7% of participants believe that Bacteria can become resistant to antibiotics while 1.1% do not think that, and 4.2% do not know. 59.6% of participants believe that people can become resistant to antibiotics, 16.1% do not, 24.2% do not know. 26.7% of participants believe that antibiotic resistance bacteria can spread from animals to human while 27.7% don’t believe that and 45.6% don’t know.34.7% of participants believe that Antibiotic resistance bacteria can spread from person to person while 37.5% don’t believe that and 27.7% don’t know. 91.6% of participants believe that increasing the use of antibiotic in the society, is associated with increasing the risk of developing antibiotic resistance, while 3.9% do not believe that and 4.6% do not know.
|
Variables |
Frequency |
Percent |
|
What is antibiotic resistance |
||
|
The ability of bacteria & other microorganisms to resist the effects of an antibiotic to which they were once sensitive. |
262 |
91.9 |
|
The ability of viruses to resist the effect of an antibiotic to which they were once sensitive. |
10 |
3.5 |
|
I don't know |
13 |
4.6 |
|
What is the cause of antibiotic resistance |
||
|
Use of antibiotic without medical prescription |
74 |
26.0 |
|
Stop the medication suddenly |
2 |
0.7 |
|
Uncompleted the course |
12 |
4.2 |
|
All of them |
186 |
65.3 |
|
I do not know |
11 |
3.9 |
|
Bacteria can become resistant to antibiotics. |
||
|
Yes |
270 |
94.7 |
|
No |
3 |
1.1
|
Participant’s Attitude
10.9% of participants agree that antibiotic resistance is not a big problem while 84.2% disagree and 4.9% are neutral. 89.5% of participants agree that Taking antibiotic correctly may reduce the risk of antibiotic resistance while 4.9% disagree and 5.9% are neutral. 25.3% of participants agree that noncompliance dose not contribute to the development of antibiotics resistance while 47% disagree and 27.7% are neutral. 21.4% of participants agree that antibiotic should be stopped immediately when the Patient clinically improved while 68.4% disagree and 10.2% are neutral. 88.1% of participants agree that students and medical have a role to play in decreasing the prevalence of antibiotics resistance while 1.8% disagree and 10.2% are neutral.
|
variable |
Frequency |
Percent |
|
Do you think antibiotic resistance is not a problem |
||
|
Agree |
31 |
10.9 |
|
Disagree |
240 |
84.2 |
|
Neutral |
14 |
4.9 |
|
Taking antibiotic correctly may reduce the risk of antibiotic resistance |
||
|
Agree |
255 |
89.5 |
|
Disagree |
14 |
4.9 |
|
Neutral |
16 |
5.6 |
|
Noncompliance dose not contribute to the development of antibiotics resistance |
||
|
Agree |
72 |
25.3 |
|
Disagree |
134 |
47.0 |
|
Neutral |
79 |
27.7 |
|
Antibiotic should be stopped immediately when the Patient clinically improved |
||
|
Agree |
61 |
21.4 |
|
Disagree |
195 |
68.4 |
|
Neutral |
29 |
10.2 |
|
As a student in the medical field and also member of society do you think you have a role to play in decreasing the prevalence of antibiotics resistance |
||
|
Agree |
251 |
88.1 |
|
Disagree |
5 |
1.8 |
|
Neutral |
29 |
10.2 |
According to Participant’s Practice
93% of participants have taking antibiotic while 7% have not taking antibiotic.
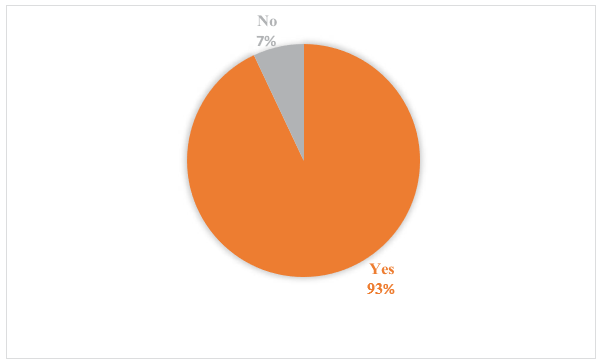
Figure 3: Taking Antibiotic
16.1% of participant's always stopping antibiotic course after improvement of symptoms while 51.6% sometimes and 32.3% never.
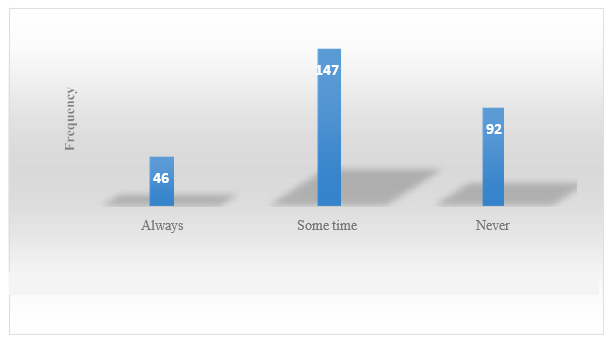
Figure 4: Stopping Antibiotic Course
32.6% of participants always-getting prescription before starting antibiotics while 56.1% sometimes and 11.2% never.
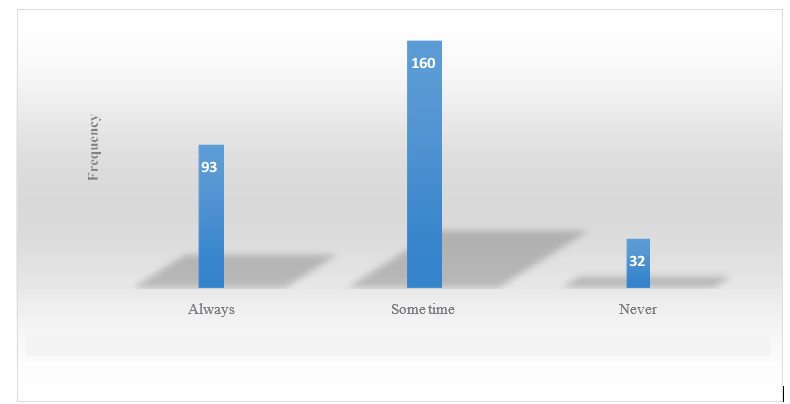
Figure 5: Getting Prescription before Starting Antibiotics
50.2% of participants always complete the course of prescribed antibiotic while 43.2% sometimes and 6.7% never.
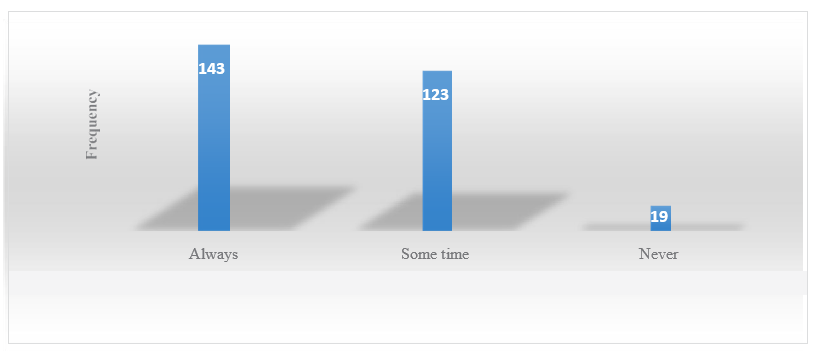
Figure 6: Complete the Course of Prescribed Antibioti
Discussion
The present study assessed knowledge, attitude and practice of antibiotic resistance among medical students. The students in AAU generally have good knowledge with some exceptions, good attitude and Poor practice. These can be seen in the main findings, which are summarized into the following points:
Regarding knowledge of antibiotic resistance: In our study, 93% of participants have heard of antibiotic resistance. This finding is similar to study in medical students in Georgia by H Phagave et al in which 83.02% heard of antibiotic resistance. On the other hand, this finding differ from study in medical students in Colombia by Luis Felipe et al in Colombia. In which only 18.2% had heard of antibiotic resistance. Regarding definition of antibiotic resistance our students show good knowledge in which 91.9% of participants agree that it is the ability of bacteria to resist the effect of an antibiotic to which they were once sensitive. This is similar to study in medical students in India done by Gupta MK et al. In which 93% of participants agree that antibiotic resistance is a phenomenon in which bacterium loses it is sensitivity to an antibiotic [5-7].
In our study, 65.3% of participants agree that the cause of antibiotic resistance is: use of antibiotic without medical description, stop the medication suddenly and un complete the course. Therefore, the present study reported good knowledge about the causes of antibiotic resistance, which is similar to study in Jordan by Saurian G. et-al [8].
In the matter "what can become resistance to antibiotic" 94.7% of our participants correctly answered that the bacteria can become resistant to antibiotics. This is similar to study in medical students in Sudan done by Musnad MA et-al [9].
However, in concern with "people can become resistance to antibiotic" our participants show average knowledge in which 59.6% of students agree with that. This is slightly differ from previous study in which 63.2% agree with us.
In concern with "Spread of resistance", only 26.7% of our participants agree that antibiotic resistance bacteria can spread from animals to humans. This finding slightly contrast study in Sudan done by Musnad MA et-al, which show 37.4% agree that. Also only 34.7% of our participants agree that resistance can spread from person to person. The present study thus reported an overall low knowledge about Spread of antibiotic resistance, which is similar to study in Sudan done by Musnad MA et-al [9].
In our study 91.6% of students know that increasing the use of antibiotic, is associate with increasing the risk of developing antibiotic resistance. In this part, our students have good knowledge, similar to studies in Zambia done by Zulu et-al [10]. And in Sudan by Musnad MA et-al. in which respectively 93.1%, 82.2% of students agree that the frequency use of antibiotic can lead to antibiotic resistance [9].
Overall, the results of the study show that the students have good knowledge, but have wrong believes about Spread of antibiotic resistance.
Concerning the attitude of participants toward antibiotics resistance: In our study, 10.9%of participants agree that antibiotic resistance in not a big problem while 84.2% disagree and 4.9% are neutral. These results are similar to the results obtained in Georgia H Phagava et_al [5]. Which 83.96% of medical students agree that antibiotics resistance has become a problem. Also in our study, 21.4% of participants agree that antibiotic should be stopped immediately when the Patient clinically improved while 68% disagree and 10.2% are neutral. On other, hand a study done in Bangladesh Mahfuza Marzan et_al [11]. Reported that 48.67% of student stop taking antibiotics when symptoms disappeared.
Also regarding attitude 88.1% of participants agree that students have a role to play in decreasing the prevalence of antibiotics resistance while 1.8% disagree and 10.2% are neutral comparing it while a study conducted in Sudan Musand MA et_al [9]. That 83.2% of students think have a role to play in decreasing the prevalence of antibiotics resistance while 7.4% disagree and 9.4% neutral.
Overall, the results of the study showed that the students had good attitude towards antibiotic resistance.
Regarding Practices of students towards antibiotic resistance: Our study reported that 93% of the participants Agreed with the statement that they take antibiotics when they were sick. The findings are similar to that in India by Manoj k. et-al [12]. In which 83.3% students have consumed antibiotics in previous year of the survey.
Regarding the participants’ practice on whether they asked doctors to prescribe antibiotics, 32.6% of participants always getting prescription before starting antibiotics while 56.1% sometimes and 11.2% never. The majority of the students disagreed but there was a minority who believed that antibiotics are used with prescription. This is similar to a study done in India by Manoj k. et-al. shows that83.3% students have consumed antibiotics in previous year of the survey. Around 45% of medical students accepted that they buy antibiotics without a prescription [12].
In the present study, 16.1% of participants always stopping antibiotic course after improvement of symptoms while 51.6% sometimes and 32.35 never. The findings of our study are different to the findings of study was performed in Bangladesh by Mahfuza marzan et-al show that students admitted to stop-taking antibiotics when symptoms disappeared (48.67%) [11].
Overall, the results of the study showed that the students had moderate practices towards antibiotic resistance.
Conclusion
This study highlight that medical students had good knowledge concerning definition of antibiotic resistance and causes of it, but low knowledge about spread of resistance. The study also declare that medical students had a good attitude about that taking antibiotic correctly reduce the risk of antibiotic resistance and as they, students have a role in decreasing prevalence of antibiotic resistance. The study also revealed that students had moderate practice in which they sometimes stop taking antibiotic after improvement of the symptoms and get prescription before starting antibiotic. The study reported a high score in attitude than knowledge and practices. We recommend introducing courses or workshops for medical students of our university describing the importance of idealized use of antibiotics, the side effects of improper use, and antibiotic resistance dangers. In addition, we recommend organizing awareness campaigns about antibiotic in different social groups to understand the overall through different ways like workshops, mass media and so.
Acknowledgments
We would like to acknowledge the student and doctors of Al- Zaiem Al-Azhari University who helped us through this study.
Funding
The research was fully funded by the authors.
Authors Contribution
MM, MFMO, MAAM, MABA; Designed and implemented the research. MABA, MFMO, MAAM conducted the data collection. MM, MFMO, MAAM, MABA conducted the data analysis .MAAH supervised the research. All authors revised the manuscript and approved it for publication.
Ethical Consideration
Ethical approval was obtained from the community department of Alzaiem Alazhari University, and after explanation of the purpose of the research to all participants; the informed consent was obtained from them.
Consent for Publication
Not applicableCompetiting Interest
The authors declare that they have no competing interests
References
- Antibiotic resistance [Internet]. Who.int. 31 July 2020 [cited2022 Jun 25]. Available from: https://www.who.int/news- room/fact-sheets/detail/antibiotic-resistance
- Antibiotic/Antimicrobial Resistance. [Internet]. www.cdc. gov. Reviewed: December 13, 2 0 2 1 [ c i t e d25 June 2022]. Available from: https://www. cdc.gov/drugresistance/about.html
- Thriemer, K., Katuala, Y., Batoko, B., Alworonga, J. P., Devlieger, H., Van Geet, C., ... & Jacobs, J. (2013). Antibiotic prescribing in DR Congo: a knowledge, attitude and practice survey among medical doctors and students. PloS one, 8(2), e55495.
- Sannathimmappa, M. B., Nambiar, V., & Aravindakshan, R. (2021). A cross-sectional study to evaluate the knowledge and attitude of medical students concerning antibiotic usage andantimicrobial resistance. International Journal of AcademicMedicine, 7(2), 113-119.
- Phagava, H., Balamtsarashvili, T., Pagava, K., & Mchedlishvili,(2019). SURVEY OF PRACTICES, KNOWLEDGE AND ATTITUDE CONCERNING ANTIBIOTICS AND ANTIMICROBIAL RESISTANCE AMONG MEDICALUNIVERSITY STUDENTS. Georgian Medical News, (294),77-82.
- Gustavo Eduardo et_al.Knowledge, attitude, and practice regarding antibiotic use and resistance among medical students in Colombia. BMC Public Health.2020;(20).1861.
- Gupta, M. K., Vohra, C., & Raghav, P. (2019). Assessment of knowledge, attitudes, and practices about antibiotic resistance among medical students in India. Journal of family medicine and primary care, 8(9), 2864.
- Suaifan, G. A. R. Y., Shehadeh, M., Darwish, D. A., Al-Ijel, H., Yousef, A. M., & Darwish, R. M. (2012). A cross-sectional study on knowledge, attitude and behavior related to antibiotic use and resistance among medical and non-medical university students in Jordan. Afr J Pharm Pharmacol, 6(10), 763-770.
- Mousnad Mohamed Awad et_al. Assessment of Knowledge and Attitude toward AntibioticUse and Resistance among Students of InternationalUniversity of Africa, Medical complex, Sudan. 2019 ;(4) :2399-9098.
- Zulu, A., Matafwali, S. K., Banda, M., & Mudenda, S. (2020). Assessment of knowledge, attitude and practices on antibiotic resistance among undergraduate medical students in the school of medicine at the University of Zambia. Int J Basic Clin Pharmacol, 9(2), 263-270.
- Marzan, M., Islam, D. Z., Lugova, H., Krishnapillai, A., Haque, M., & Islam, S. (2021). Knowledge, attitudes, and practices of antimicrobial uses and resistance among public university students in Bangladesh. Infection and drug resistance, 519-533.
- Gupta, M. K., Vohra, C., & Raghav, P. (2019). Assessment of knowledge, attitudes, and practices about antibiotic resistance among medical students in India. Journal of family medicine and primary care, 8(9), 2864.




