Research Article - (2025) Volume 3, Issue 2
Antimicrobial Resistance Profiles of Bacterial Pathogens Causing Surgical Site Infections among Post-Operative Mothers at Kawempe National Referral Hospital, Uganda
Received Date: Sep 09, 2025 / Accepted Date: Oct 30, 2025 / Published Date: Nov 07, 2025
Copyright: ©2025 Muyingo Yusuf, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Yusuf, M., Jawuhala, N., Eluma, O. I., Muhammad, H., Koma, A. A., et al. (2025). Antimicrobial Resistance Profiles of Bacterial Pathogens Causing Surgical Site Infections among Post-Operative Mothers at Kawempe National Referral Hospital, Uganda. J Emerg Med OA, 3(2), 01-06.
Abstract
Surgical site infections (SSIs) significantly contribute to maternal morbidity and mortality, with antimicrobial resistance (AMR) complicating effective management. This study assessed the bacterial profiles and antimicrobial susceptibility patterns, emphasizing AMR, among post-operative mothers at Kawempe National Referral Hospital. Swab samples from infected surgical sites were cultured and tested against a panel of antibiotics using the Kirby-Bauer disk diffusion method. Results revealed predominant pathogens, notably Staphylococcus aureus and Escherichia coli, with varying susceptibility profiles. Notably, multidrug-resistant strains, including methicillin-resistant Staphylococcus aureus (MRSA), exhibited resistance to commonly used antibiotics such as penicillins and aminoglycosides, but remained susceptible to vancomycin and imipenem. These findings underscore the urgent need for antimicrobial stewardship and routine susceptibility testing to curb AMR in this setting.
Introduction
Antimicrobial resistance (AMR) poses a global health threat, undermining the efficacy of antibiotics and complicating the treatment of infections, including surgical site infections (SSIs). In Uganda, the prevalence of SSIs post-cesarean delivery remains high, with bacterial pathogens demonstrating diverse susceptibility patterns. Understanding the local antimicrobial resistance profiles is vital for guiding empirical therapy and implementing effective infection control measures [1].
Materials and Methods
Swab specimens from post-operative maternal surgical sites were cultured on Blood, Chocolate, and MacConkey agar plates. Incubation was performed at 37°C for 24-48 hours. Bacterial identification involved colony morphology, Gram staining, and biochemical tests, including catalase, coagulase, indole, urease, citrate utilization, and triple sugar iron tests. Antimicrobial susceptibility testing was conducted using the Kirby-Bauer disk diffusion method on Mueller-Hinton agar, with antibiotics selected based on local guidelines: Imipenem, Vancomycin, Clindamycin, Ciprofloxacin, Gentamicin, Ceftriaxone, and Ceftazidime. Zones of inhibition were measured and interpreted following CLSI standards.
Results
Prevalence of Surgical Site Infection in Post-Operative Mothers at Kawempe National Referral Hospital
This data was obtained from the culture plates which showed growth of significance during the study as in table 1 below
|
Sepsis (n=202) |
Freq. |
Percent(%) |
|
No Growth |
140 |
69.3 |
|
Growth |
62 |
30.7 |
|
Gram stain reaction (n=62) |
|
|
|
Positive(only) |
51 |
82.2 |
|
Negative(only) |
4 |
6.5 |
|
Mixed Growth |
7 |
11.3 |
Table 1: Showing the Prevalence of Surgical Site Infection in Post-Operative Mothers at Kawempe National Referral Hospital
In the study comprising 202 participants, 30.7% were diagnosed with post-Caesarean wound sepsis with gram positive, gram negative, and mixed gram reaction having the prevalence of 82.2%, 6.5% and 11.3% respectively.
Possible Bacterial Species from Exudates on Wounds of Post-Operative Mothers at Kawempe National Referral Hospital
This data was obtained from the culture plates which showed growth of significance during the study and isolates identified as shown In Table 2.
|
Isolated Organism (n=70) |
Freq. |
Percent(%) |
|
Staphylococcus aureus |
30 |
42.9 |
|
Coagulase Negative Staphylococuss |
29 |
41.4 |
|
Escherichia coli |
3 |
4.3 |
|
Klebsiella species |
3 |
4.3 |
|
Others |
5 |
7.1 |
Table 2: Showing Possible Bacterial Species from Exudates on Wounds of Post-Operative Mothers at Kawempe National Referral Hospital
A total of 70 bacterial isolates were identified from SSIs, with Staphylococcus aureus (42.9%) and coagulase-negative Staphylococci (41.4%) being the most prevalent. Gram-negative bacteria included E. coli (4.3%) and Klebsiella spp. (4.3%).
Antimicrobial Activity of Isolated Bacterial Profiles Causing Surgical Site Infections among Postoperative Mothers at Kawempe National Referral Hospital
Figure 1: Bar graph showing gram negatives susceptibility testing to antibiotics in post ceasarean wound infections among mothers attending Kawempe National Referral Hospital (Number of organisms against Antibiotics)
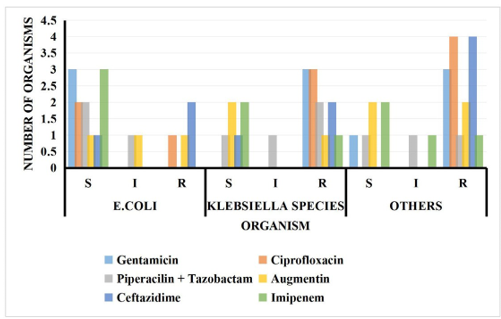
Figure 2: Bar graph showing gram negative isolates susceptibility testing to antibiotics in post ceasarean wound infections among mothers attending Kawempe National Referral Hospital (Number of organisms against Antibiotics)
• E. coli and Klebsiella spp.: Demonstrated high susceptibility to Imipenem (92-100%) but showed resistance to Ceftriaxone and Ceftazidime (resistance rates >50%), indicating extended- spectrum beta-lactamase (ESBL) production.
Figure 3: A Radar Chart showing Staphylococcus aureus susceptibility testing to antibiotics in post ceasarean wound infections among mothers attending Kawempe National Referral Hospital (Number of organisms against Antibiotics)
Staphylococcus Aureus: High susceptibility to Vancomycin (100%) and Clindamycin (86.7%), but notable resistance to Ciprofloxacin (40%) and Gentamicin (33.3%). MRSA strains exhibited resistance to beta-lactams, with susceptibility retained to Vancomycin and Imipenem.
The resistance patterns indicate a rising prevalence of multidrug- resistant organisms, particularly MRSA and ESBL-producing gram-negatives.
Discussion
In the study, coliforms showed high susceptibility to Imipenem and this is comparable to a study done in Mbale Regional Referral Hospital, Eastern Uganda, as well as in the study conducted from Hoima Regional Referral Hospital [1,2]. In the same study, Staphylococcus aureus showed high susceptibility to Clindamycin and Vancomycin which is contrally to other studies from Hoima and Mbale regional Refferal hospital which showed high sensitivity to Ciprofloxacin [3]. Furthermore, the study also showed that Staphylococcus aureus was resistant to Ciprofloxacin, Gentamycin, and Cefoxitin while coliforms were resistant to Ciprofloxacin, Ceftazidime, and Gentamicin. This could be attributed to the fact that these drugs were the most erroneously prescribed medications among the study population in Kawempe National Referral Hospital. These findings are similar to those found in Hoima [1].
The detection of MRSA and ESBL-producing gram-negative bacteria underscores the growing challenge of AMR in the hospital setting. Resistance to first-line antibiotics such as penicillins and cephalosporins limits empirical treatment options, necessitating reliance on last-resort drugs like Vancomycin and Imipenem. These findings align with regional studies indicating high resistance rates among Staphylococcus aureus and Enterobacteriaceae. The persistence of susceptibility to Vancomycin and Imipenem offers some therapeutic options but raises concerns over potential future resistance development. The high prevalence of multidrug- resistant organisms necessitates strengthening antimicrobial stewardship programs, routine susceptibility testing, and infection control measures to prevent transmission.
Conclusion
AMR among bacterial pathogens causing SSIs at Kawempe National Referral Hospital is increasingly problematic, characterized by resistance to commonly used antibiotics. There is an urgent need to implement routine microbial susceptibility testing, enforce antimicrobial stewardship, and adopt infection prevention strategies to mitigate the impact of resistant organisms [4-41].
Recommendations
1. Routine antimicrobial susceptibility testing for all SSI isolates to guide targeted therapy.
2. Strengthen infection prevention and control protocols.
3. Promote antimicrobial stewardship programs to optimize antibiotic use.
4. Continuous surveillance of resistance patterns to inform empirical treatment guidelines.
5. Capacity building for laboratory personnel in advanced diagnostic and susceptibility testing techniques.
References
- Muhumuza, I., Lavingia, A. Z., Tayebwa, B., Ahmed, A. A., Koriow, F. M., Tetty, V. O., ... & Ssebuwufu, R. (2020). Post Caesarean Wound sepsis and associated factors among patients attending a rural regional referral hospital in Western Uganda: A cross-sectional study.
- Matinyi, S., Enoch, M., Akia, D., Byaruhanga, V., Masereka, E., Ekeu, I., & Atuheire, C. (2018). Contamination of microbial pathogens and their antimicrobial pattern in operating theatres of peri-urban eastern Uganda: a cross-sectional study. BMC infectious diseases, 18(1), 460.
- George, M., Iramiot, J. S., Muhindo, R., Olupot-Olupot, P., & Nanteza, A. (2018). Bacterial aetiology and antibiotic susceptibility profile of post-operative sepsis among surgical patients in a tertiary hospital in rural Eastern Uganda. Microbiology research journal international, 24(2), MRJL-41690.
- Aboud, S., Ali, S. S., & Kibwana, U. O. (2022). Bacterial Profile and Antibiogram of Pathogens Causing Surgical Site Infections at Mnazi Mmoja Hospital in Zanzibar, Tanzania.
- Adaji, J. A., Akaba, G. O., Isah, A. Y., & Yunusa, T. (2020). Short versus long-term antibiotic prophylaxis in cesarean section: A randomized clinical trial. Nigerian Medical Journal, 61(4), 173-179.
- Adane, F., Mulu, A., Seyoum, G., Gebrie, A., & Lake, A. (2019). Prevalence and root causes of surgical site infection among women undergoing caesarean section in Ethiopia: a systematic review and meta-analysis. Patient safety in surgery, 13(1), 34.
- Anguzu, J. R., & Olila, D. (2007). Drug sensitivity patterns of bacterial isolates from septic post-operative wounds in a regional referral hospital in Uganda. African health sciences, 7(3).
- Azeze, G. G., & Bizuneh, A. D. (2019). Surgical site infection and its associated factors following cesarean section in Ethiopia: a cross-sectional study. BMC research notes, 12(1), 288.
- Carshon-Marsh, R., Squire, J. S., Kamara, K. N., Sargsyan, A., Delamou, A., Camara, B. S., ... & Kenneh, S. (2022). Incidence of surgical site infection and use of antibiotics among patients who underwent caesarean section and herniorrhaphy at a regional referral hospital, Sierra Leone. International Journal of Environmental Research and Public Health, 19(7), 4048.
- Cheesbrough, M. (1999). Parasitological tests. District laboratory practice in tropical countries, part, 1, 220-1.
- Curcio, D., Cane, A., Fernández, F., & Correa, J. (2019). Surgical site infection in elective clean and clean-contaminated surgeries in developing countries. International Journal of Infectious Diseases, 80, 34-45.
- Dayo-Dada, T. O., Ojo, A. A., & Akpor, O. A. (2022).Prevalence of surgical site infection among caesarean section patients in a teaching hospital in Ekiti State, Nigeria: An eight-year review. Scientific African, 16, e01216.
- Farret, T. C. F., Dallé, J., Monteiro, V. D. S., Riche, C. V. W., & Antonello, V. S. (2015). Risk factors for surgical site infection following cesarean section in a Brazilian Women's Hospital: a case-control study. Brazilian Journal of Infectious Diseases, 19(2), 113-117.
- Gelaw, K. A., Aweke, A. M., Astawesegn, F. H., Demissie,B. W., & Zeleke, L. B. (2017). Surgical site infection and its associated factors following cesarean section: a cross sectional study from a public hospital in Ethiopia. Patient safety in surgery, 11(1), 18.
- Getaneh, T., Negesse, A., & Dessie, G. (2020). Prevalence of surgical site infection and its associated factors after cesarean section in Ethiopia: systematic review and meta- analysis. BMC pregnancy and childbirth, 20(1), 311.
- Harrison, M. S., & Goldenberg, R. L. (2016). Cesarean section in sub-Saharan Africa. Maternal health, neonatology and perinatology, 2(1), 6.
- Irani, M., & Deering, S. (2015). Challenges affecting access to cesarean delivery and strategies to overcome them in low- income countries. International Journal of Gynecology & Obstetrics, 131(1), 30-34.
- Isanga, J., Emmanuel, B., Musa, K., Julius, M., Tibaijuka, L., Ronald, M., & Ngonzi, J. (2020). The prevalence, risk factors, and bacterial profile of cesarean surgical site infections at a University Teaching Hospital in South Western Uganda.
- Isanga, J., Emmanuel, B., Musa, K., Julius, M., Tibaijuka, L., Ronald, M., & Ngonzi, J. (2020b). The prevalence, risk factors, and bacterial profile of cesarean surgical site infections at a University Teaching Hospital in South Western Uganda. 1, 5-10.
- John, C., & Omoruyi, S. (2021). Prevalence and Pattern of Post Caesarean Section Wound Sepsis at The University of Port Harcourt Teaching Hospital: A 5 Year Review. Gazette of Medicine, 9 (1).
- Amulioto, J., Muturi, M. W., Mathenge, S., & Mutua, G.M. (2020). Antibiotic susceptibility patterns of bacteria isolates from post-operative wound infections among patients attending Mama Lucy Kibaki Hospital, Kenya. African Journal of Microbiology Research, 14(8), 420-425.
- Kawakita, T., & Landy, H. J. (2017). Surgical site infections after cesarean delivery: epidemiology, prevention and treatment. Maternal health, neonatology and perinatology, 3(1), 12.
- Lukabwe, H., Kajabwangu, R., Mugisha, D., Mayengo, H., Munyanderu, B., Baluku, A., ... & Ngonzi, J. (2022). Effectiveness of preoperative bath using chloroxylenol antiseptic soap on the incidence of post emergency cesarean section surgical site infection at Mbarara Regional Referral hospital, Uganda: a randomized controlled trial. Pan African Medical Journal, 41(1).
- Lukakamwa, D. (2012). Risk of post caesarean wound infection among women managed by open versus closed dressing in Mulago Hospital: A randomised controlled trial (Doctoral dissertation, Makerere University).
- Manyahi, J. (2012). Bacteriological spectrum of post operative wound infections and their antibiogram in a Tertiary Hospital, Dar Es Salaam, Tanzania (Doctoral dissertation, Muhimbili University of Health and Allied Sciences).
- McKibben, R. A., Pitts, S. I., Suarez-Cuervo, C., Perl, T. M., & Bass, E. B. (2015). Practices to reduce surgical site infections among women undergoing cesarean section: a review. infection control & hospital epidemiology, 36(8), 915- 921.
- Devi, S. L., & Durga, D. V. K. (2018). Surgical site infections post cesarean section. International Journal of Reproduction, Contraception, Obstetrics and Gynecology, 7(6), 2486-2490.
- Mitchell, M. D., Peiris, H. N., Kobayashi, M., Koh, Y. Q., Duncombe, G., Illanes, S. E., ... & Salomon, C. (2015). Placental exosomes in normal and complicated pregnancy. American journal of obstetrics and gynecology, 213(4), S173-S181.
- Morrison, J. J., Rennie, J. M., & Milton, P. J. (1995). Neonatal respiratory morbidity and mode of delivery at term: influence of timing of elective caesarean section. BJOG: An International Journal of Obstetrics & Gynaecology, 102(2), 101-106.
- Nansikombi, S. (2015). Risk factors for post cesarean wound infection among mothers at Mulago national referral hospital- Uganda (Doctoral dissertation, International Health Sciences University.).
- Onken, A., Said, A. K., Jørstad, M., Jenum, P. A., & Blomberg,B. (2015). Prevalence and antimicrobial resistance of microbes causing bloodstream infections in Unguja, Zanzibar. PloS one, 10(12), e0145632.
- Ostovar, R., Rashidian, A., Pourreza, A., Rashidi, B. H., Hantooshzadeh, S., Ardebili, H. E., ... & members of the panel of the Cesarean Section RAM Study. (2010). Developing criteria for cesarean section using the RAND appropriateness method. BMC pregnancy and childbirth, 10(1), 52.
- Seni, J., Bwanga, F., Najjuka, C. F., Makobore, P., Okee, M., Mshana, S. E., ... & Kateete, D. P. (2013). Molecular characterization of Staphylococcus aureus from patients with surgical site infections at Mulago Hospital in Kampala, Uganda. PloS one, 8(6), e66153.
- Sway, A., Nthumba, P., Solomkin, J., Tarchini, G., Gibbs, R., Ren, Y., & Wanyoro, A. (2019). Burden of surgical site infection following cesarean section in sub-Saharan Africa: a narrative review. International journal of women's health, 309-318.
- Temming, L. A., Raghuraman, N., Carter, E. B., Stout, M. J., Rampersad, R. M., Macones, G. A., ... & Tuuli, M. G. (2017). Impact of evidence-based interventions on wound complications after cesarean delivery. American journal of obstetrics and gynecology, 217(4), 449-e1.
- Victor, D., Revathi, G., Sam, K., Abdi, H., Asad, R., & Andrew, K. (2013). Pattern of pathogens and their sensitivity isolated from surgical site infections at the Aga Khan University Hospital, Nairobi, Kenya. Ethiopian journal of health sciences, 23(2), 141-149.
- Wekesa, Y. N., Namusoke, F., Sekikubo, M., Mango, D. W., & Bwanga, F. (2020). Ceftriaxone-and ceftazidime-resistantKlebsiella species, Escherichia coli, and methicillin-resistant Staphylococcus aureus dominate caesarean surgical site infections at Mulago Hospital, Kampala, Uganda. SAGE Open Medicine, 8, 2050312120970719.
- Wodajo, S., Belayneh, M., & Gebremedhin, S. (2017). Magnitude and factors associated with post-cesarean surgical site infection at Hawassa University teaching and referral hospital, southern Ethiopia: a cross-sectional study. Ethiopian journal of health sciences, 27(3), 283-290.
- Worjoloh, A., Manongi, R., Oneko, O., Hoyo, C., Daltveit, A.K., & Westreich, D. (2012). Trends in cesarean section ratesat a large East African referral hospital from 2005-2010. Open Journal of Obstetrics and Gynecology, 2(03), 255.
- Yerba, K., Failoc-Rojas, V., Zeña-Ñañez, S., & Valladares- Garrido, M. (2020). Factors associated with surgical site infection in post-cesarean section: a case-control study in a Peruvian hospital. Ethiopian journal of health sciences, 30(1).
- Zuarez-Easton, S., Zafran, N., Garmi, G., & Salim, R. (2017). Postcesarean wound infection: prevalence, impact, prevention, and management challenges. International journal of women's health, 81-88.



