Research Article - (2025) Volume 3, Issue 6
An Evaluation of the Effectiveness of Refractive Loupes as an Intervention to Prevent Chronic Neck and Back Pain in Undergraduate Dental Students - A Longitudinal Study
Received Date: Oct 21, 2025 / Accepted Date: Nov 21, 2025 / Published Date: Nov 25, 2025
Copyright: ©2025 N. Raghava. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Raghava, R., Kulkarni, T., Cantiveros, M. B. (2025). An Evaluation of the Effectiveness of Refractive Loupes as an Intervention to Prevent Chronic Neck and Back Pain in Undergraduate Dental Students - A Longitudinal Study. Int Internal Med J, 3(6), 01-07.
Abstract
Chronic neck and back pain is prevalent among dental professionals, stemming from the static and often awkward positions required during clinical practice. This longitudinal study investigates the effectiveness of Refractive loupes, an ergonomic intervention, in mitigating such musculoskeletal issues among undergraduate dental students. Despite being advocated for posture improvement, traditional loupes may exacerbate neck pain due to prolonged static neck positions. However, the impact of ergonomic loupes, designed to maintain neutral neck positions, remains unexplored.
This study enrolled undergraduate dental students from the UK and Australia, provided them with Refractive loupes, and tracked their neck and back pain scores over two years. Participants completed pre- and post-intervention questionnaires assessing pain levels, posture, and loupe use history. Results indicate a significant reduction in pain incidence (15.5%) post-refractive use, with 30.6% of participants reporting pain at the study's end compared to 46.1% at the beginning of the study. Notably, 92.3% reported improved posture ratings despite 39.1% experiencing increased pain, suggesting additional factors contributing to pain development beyond posture alone.
Further analysis reveals that later adoption of Refractive loupes correlates with increased pain, suggesting a potential preventive benefit if initiated earlier in dental education. Additionally, a comparison of traditional loupe users with their non-loupe-using counterparts indicates more significant pain reduction among the loupe-using cohort post-refractive use, highlighting the need for more extensive studies in this area.
In conclusion, Refractive loupes effectively reduce musculoskeletal pain among undergraduate dental students. Nevertheless, challenges persist, warranting continued research into optimal intervention timing and the role of the loupe type used in pain mitigation.
Introduction
Chronic back and neck pain is one of the most commonly reported occupation-related health hazards experienced by dentists across the globe [1]. This is most closely related to the static2 and often contorted positions that dentists adopt to obtain direct vision while working. This musculoskeletal pain often begins at dental school with a systematic literature review suggesting that the prevalence of this pain in graduated dentists varies between 64% and 93%, with the most commonly cited regions of pain being back (36.3– 60.1%) and neck (19.8–85%), when compared with, compared with 79% of dental students prior to graduation6 with worsening proportions of students complaining of pain as the dental school year of participants increased [3-5].
Traditional loupes have long been promoted as a way to improve spinal position and prevent chronic back pain; however, chronic neck pain is the second most reported musculoskeletal pain by dentists and dental students. HodaÄová et al. found that the statistically significant increase in pain was in neck pain, not back pain, as dental students progressed from 1st to 5th year [7].
Traditional loupes do not propose an ergonomic solution for the neck, and traditional loupe use increases the time users spend with their necks in a static position- a key contributor to the development of chronic pain. Although the relationship between traditional loupe use and neck pain has not been explored extensively, Sivak- Callcott, Jennifer. A et al. showed that traditional loupes did not prevent neck pain but were associated with an increased risk of neck pain in the oculoplastic surgeons they surveyed. This finding was supported by the more extensive study by Wu et al., also in oculoplastic surgeons, in which 11% of their participants stated that neck and cervical spinal issues were associated with loupe use [8,9].
To our knowledge, no study has shown the effects of using ergonomic loupes, here defined as loupes that use prisms or deflective mechanisms to keep the neck in a neutral position during work. Moreover, none of the studies we encountered during our literature review included any interventional element and were typically observational. Our study was designed to study the effect of ergonomic loupes in a population of dental students across the UK and Australia who had been provided with ergonomic loupes to compare their neck and back pain scores at the end of their studies to the values reported in the literature in students who used traditional loupes or no loupes.
Methods
We enrolled all undergraduate dental students who purchased 2.9x, 3.8x or 5.7x Refractive loupes with a headlight into our longitudinal study, which began in 2021. Participants were enrolled throughout the year, at which point they completed a questionnaire prior to receiving their ergonomic loupes. This questionnaire was designed to assess their posture prior to using Refractives. It was based on the Nordic back pain assessment, modified to account for prior loupe use, and tailored to dentistry
Our study design was assessed using the NHS Research Ethics Committee (REC) review tool. Following a comprehensive evaluation, it was determined that the study does not meet the criteria for requiring NHS ethical review. Our first questionnaire asked participants to: • Rate their posture out of 10 to assess perceived posture during clinical work, with ten being the highest and 0 being the lowest.
• Whether they currently suffer from neck or back pain
• To rate their neck and back pain out of 10, with 10 being the highest and zero the lowest. We also collected information on their clinical year when they started using Refractives and their history of loupe use. We then asked participants to complete a follow-up study 2 years later, which asked them once again to:
•Rate their posture out of 10 to assess perceived posture during clinical work, with ten being the highest and 0 being the lowest.
• Whether they currently suffer from neck or back pain
• To rate their neck and back pain out of 10, with 10 being the highest and zero the lowest.
Students from all year groups were included in the study, and no participants were excluded.
Of the 907 students who enrolled throughout the two years, 233 completed both questionnaires, with the remaining scheduled to complete the second survey over the next two years.
Results
In total, 907 participants completed the first survey, and we collected information from all of these participants on whether they suffered neck or back pain - we have included these values below to assess the baseline percentage of neck and back pain compared to values in the literature. Of our participants, 57% reported neck and back pain, which is consistent with values reported in the literature 1,2,3,4 - although on the lower side, which we attribute to the early stage of dental school, 46% of participants are in.
Figure 1: Graph Showing all Participants' Reported Back and Neck Pain before Receiving
Refractives
Figures 2,3 and 4 show the baseline back and neck pain percentage in the 233 who completed both surveys and their initial posture and pain rating before receiving Refractives.
Figure 2: A Graph Showing the Percentage of Participants Who Reported Pain Prior to Refractive Use Compared to Those Who Reported No Pain
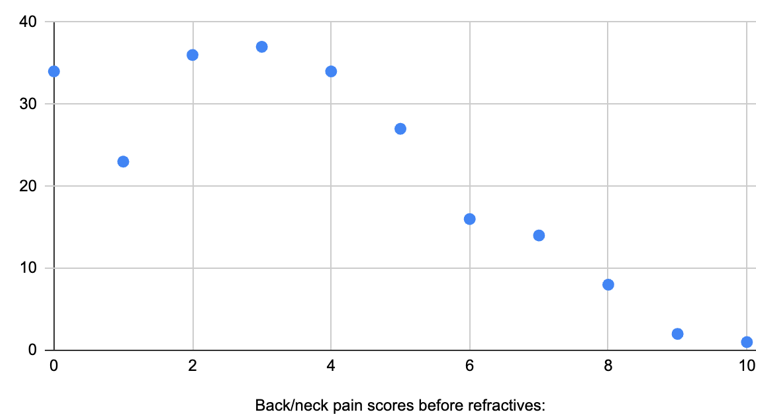
Figure 3: Showing the Back and Neck Pain Scores in Participants Who Completed Both Surveys Before Using Refractives
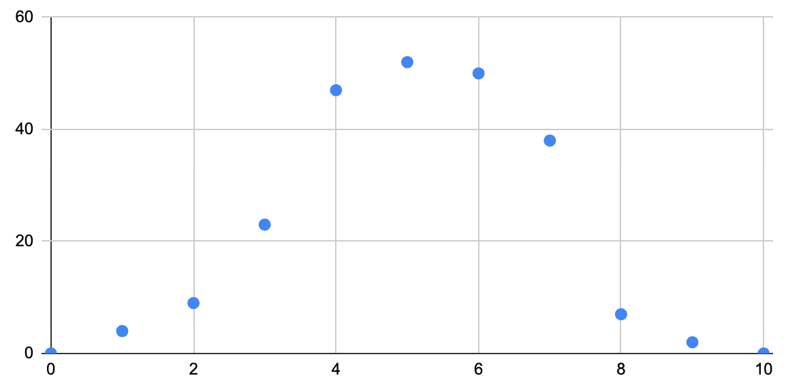
Figure 4: Showing the Posture Rating Scores in Participants Who Completed Both Surveys Before Refractive Use
The highest percentage of participants started to wear Refractives in their second year of dental school, which allowed us to monitor the progress of their pain without the effects of daily clinical work confounding the results.
Figure 4: The Year Group Split into 233 Participants Who Completed Both Surveys
We also considered the reasons students gave us for choosing to use Refractives, which could be broadly split into four categories: to improve posture, increase magnification, reduce pain, and others. Most participants chose to wear Refractives to improve their posture, which shows an increasing awareness of the importance of neck and back posture during dental practice.
Figure 5: Graph Showing the Main Reasons for Enrolling in our Study Split by Year Group
We then evaluated the change in posture and pain rating across this 233-participant cohort compared to their overall pain incidence and pain and posture ratings before using Refractives. Results are shown in Figures 6, 7 and 8 below.
Figure 6: Graph Showing the Pain Incidence in Participants Who Completed Both Surveys After Using Refractives
Figure 7: Graph Showing the Pain Rating Changes in Participants Who Completed Both Surveys After Using Refractives
When Figure 7 is compared with results in Figure 2, taken prior to Refractive use, it shows a decrease of 15.6% in pain among respondents.
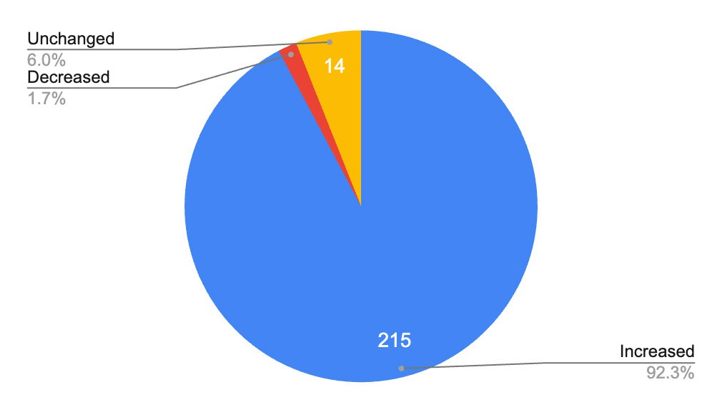
Figure 8: Graph Showing the Posture Rating Changes in Participants Who Completed Both Surveys After Using Refractives
The figures above show an overall reduction in pain incidence of 49.4% and prevention of further pain in 11.6% of the participants. However, 39.1% showed an increase in musculoskeletal pain. Conversely, despite the 39.1% who reported increased pain, 92.3% of all participants reported an increase in perceived posture, with 6% reporting unchanged posture and 1.7% reporting a reduction in perceived posture rating.
For participants whose pain rating increased post-refractive use, we evaluated the year of dental school they were in before starting the study to assess the effect of later adoption on the efficacy of the intervention. Table 9 shows that as a proportion of the total participants from each year group who started the study, there was a general increase in the percentage of those with increased pain per year group as the year groups increased. This is consistent with literature findings reporting increased pain during the dental degree [3].
|
|
Increased pain rating participants by year group at commencement |
% of the total enrolled participants in that year group |
|
Year 2 |
39 |
36.11% |
|
Year 3 |
14 |
38.88% |
|
Year 4 |
16 |
43.24% |
|
Year 5 |
20 |
39.21% |
Figure 9: Table Showing the Incidence of Increased Pain Post Refractives Split by Year Group Upon Commencement of the Study
We also compared pain incidence in participants who had previously worn loupes prior to wearing Refractives with those who had not worn loupes prior to Refractives and then evaluated the incidence of pain in these populations post-refractive use. This can be seen in Figures 10 and 11 below.
Figure 10: Graph Showing the Percentage Change in Pain in Non-Loupe Users Before and After Refractive Use
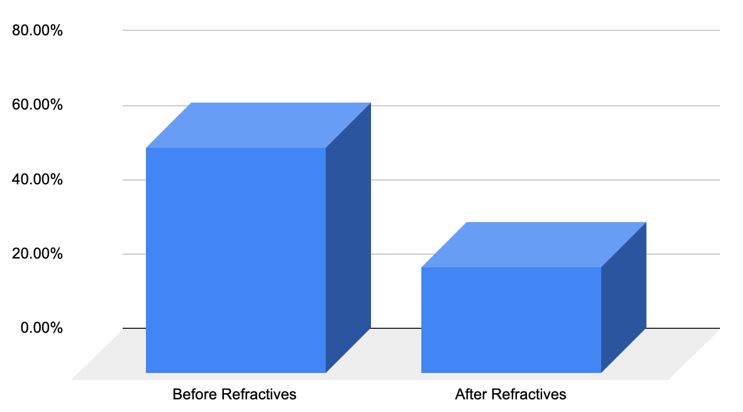
Figure 11: Graph Showing the Percentage Change in Pain Incidence in Traditional Non-Refractive Loupe Users Before and After Refractive Use
Our comparison showed that not only was the percentage reduction in pain greater in traditional loupe users when compared with never users, but the pain incidence was also higher in these populations prior to Refractive use, which aligns with findings in work in oculoplastic surgeons in the effect of traditional loupes on musculoskeletal pain [8,9].
Discussion
Our results show that using Refractives led to a statistically significant reduction in neck and back pain incidence in undergraduate dental students, with an overall decrease in reported pain of 15.6%. At the end of two years of Refractive use, our cohort showed a 30.6% pain incidence, which is significantly lower than our baseline and significantly lower than reported values in the literature [1-4].
We would also posit that the reasons for our baseline pain incidence percentages being lower than reported values - which in cases ranged up to 91.2%3- may be related to an increased awareness amongst dental students in these cohorts of the importance of posture, with 64.8% of participants enrolling in order to correct their posture, as well as an increased uptake amongst second-year students who have not yet practised dentistry for extended hours with bad posture. Of those who reported pain, 49.4% reported a decreased pain rating, 11.6% reported no worsening with an unchanged score, and 39.1% reported an increased pain score despite using the Refractives for two years.
When evaluating this result, we assessed it alongside our postural findings. Compared to perceived posture rating pre-refractives, 92.3% of all participants reported increased posture ratings.
This is a significant increase, with only 1.7% reporting decreased perceived posture ratings. Given that participants who reported increased pain also reported an improvement in their posture, increased pain ratings suggest that there may be other confounding factors contributing to pain development that are not attributable to posture alone.
One such factor may be pre-existing pain conditions or the practice of dentistry without loupes for extended periods. This is supported by our findings in Table 9, which show that of those participants who reported increased pain, they were more likely to have adopted Refractive use at a later stage in their dental education.
Interestingly, when evaluating traditional loupes and how their users experienced pain before and after using Refractives, we found that traditional loupe users experienced higher pain incidence before Refractives and reported a more significant pain reduction post-use of Refractives. One limitation of our work here in this aspect is the small sample size of loupe users in this cohort, and we would welcome further, more extensive studies in this area.
Conclusions
Our findings suggest that using Refractive loupes significantly reduces musculoskeletal pain development and worsening in undergraduate dental students. However, we aim to repeat this study with the remaining participants scheduled to complete the survey in the next two years. We aim to repeat this study, with the modification of enrolling all participants at the beginning of their clinical careers - by the second year of their programme- to prevent bad habits from developing that may not be completely rectifiable.
Furthermore, our results report that 60.7% of previous loupe users reported pain before Refractive use, 32.13% of whom showed a reduction in pain rating after two years of Refractive use. We urge further studies to focus on the longitudinal impact of prismatic loupe use on posture and chronic pain and whether they are an ergonomic solution or part of the problem. Finally, we would also welcome studies investigating the effects of other confounding factors, such as the dental stools students use, to assess this impact on the overall ergonomic position.
References
- SL; MELR. Musculoskeletal symptoms in New South Wales dentists [Internet]. U.S. National Library of Medicine; [cited 2024 Feb 1].
- Rundcrantz, B. L., JohnSSon, B., & MoritZ, U. (1990). Cervical pain and discomfort among dentists. Epidemiological, clinical and therapeutic aspects. Part 1. A survey of pain and discomfort. Swedish dental journal, 14(2), 71-80.
- Felemban, R. A., Sofi, R. A., Alhebshi, S. A., Alharbi, S. G., Farsi, N. J.,Abduljabbar, F. H., & Farsi, J. M. (2021). Prevalence and predictors of musculoskeletal pain among undergraduate students at a dental school in Saudi Arabia. Clinical, cosmetic and investigational dentistry, 39-46.
- O; RDBK. Reports of body pain in a dental student population [Internet]. U.S. National Library of Medicine; [cited 2024 Feb 1].
- Vijay, S., & Ide, M. (2016). Musculoskeletal neck and back pain in undergraduate dental students at a UK dental school—a cross-sectional study. British dental journal, 221(5), 241-245.
- DR; HMD. A systematic review of musculoskeletal disorders among Dental professionals [Internet]. U.S. National Library of Medicine; [cited 2024 Feb 1].
- HodaÄová, L., Pilbauerová, N., Ä?ermáková, E., MachaÄ, S., Schmidt, J., HodaÄ, J., & Kapitán, M. (2022). The Prevalence and Development of Neck and Lower Back Pain and Associated Factors in Dentistry Students—A Long-Term Prospective Study. International Journal of Environmental Research and Public Health, 19(14), 8539.
- Sivak-Callcott, J. A., Diaz, S. R., Ducatman, A. M., Rosen,C. L., Nimbarte, A. D., & Sedgeman, J. A. (2011). A survey study of occupational pain and injury in ophthalmic plastic surgeons. Ophthalmic Plastic & Reconstructive Surgery, 27(1), 28-32.
- AY; WC. Surgical loupe usage among oculoplastic surgeons in North America [Internet]. U.S. National Library of Medicine; [cited 2024 Feb 1].




