Case Report - (2025) Volume 10, Issue 7
A Small Perianal Lesion Revealing a Large Hemolymphangioma in a Pediatric Patient-The Hidden Iceberg Phenomenon: Case Report
Received Date: May 02, 2025 / Accepted Date: Jul 15, 2025 / Published Date: Jul 30, 2025
Copyright: ©Copyright: ©2025 Fouzia Hali. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation: Hali, F, Boujloud, S., & Chiheb, S. (2025). A Small Perianal Lesion Revealing a Large Hemolymphangioma in a Pediatric Patient-The Hidden Iceberg Phenomenon: Case Report. J Clin Rev Case Rep, 10(7), 01-05.
Abstract
Background: Hemolymphangioma is a rare vascular and lymphatic malformation that poses diagnostic and therapeutic challenges. Treatment depends on the severity and location. Electrocoagulation and other physical modalities may offer temporary relief for superficial lesions. Hemolymphangioma management requires a multidisciplinary approach due to its complexity. Given its rarity, each case contributes valuable insights into optimal management strategies.
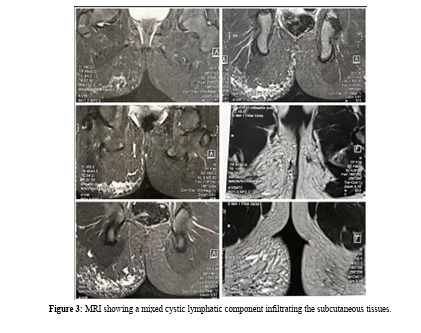
Case Presentation: A North African 10-year-old girl was presented with congenital right-sided gluteal asymmetry, which progressively evolved with the appearance of a painful, bleeding perianal lesion. Clinical examination revealed lymphangiectasias overlying a port-wine stain, prone to bleeding upon minor irritation. Ultrasonography and MRI confirmed a hemolymphangioma with a mixed cystic lymphatic component. Electrocoagulation was performed to control superficial bleeding while preserving the infiltrative subcutaneous component for ongoing clinical monitoring. To date, an eight-month follow-up has shown no recurrence of superficial lymphangiectasias and no clinically significant increase in gluteal volume.
Conclusion: Hemolymphangioma is a rare and challenging entity that necessitates individualized management strategies. A multidisciplinary approach is essential to optimize treatment outcomes, prevent complications, and improve the patient’s quality of life.
Keywords
Hemolymphangioma, Tumor, Lymphatic malformation, Perianal, Pediatric, Case report
Abbreviations
MRI: Magnetic Resonance Imaging ; ISSVA : International Society for the Study of Vascular Anomalies
Introduction
Hemolymphangioma is a rare benign tumor resulting from the abnormal development of lymphatic and vascular structures, typically present at birth [1]. Although most commonly found in the head, neck, and extremities, perianal involvement is exceptionally rare, with limited epidemiological data available. According to the latest ISSVA (International Society for the Study of Vascular Anomalies) classification guidelines (2023), hemolymphangiomas fall under the spectrum of combined vascular malformations.
The clinical presentation varies widely, often leading to diagnostic challenges. Perianal hemolymphangiomas may mimic other vascular anomalies such as angiokeratomas, lymphangiomas, hemorrhagic papillomas, and Klippel-Trénaunay syndrome, necessitating thorough imaging studies. MRI remains the gold standard for diagnosis, providing detailed assessment of lesion extent and tissue involvement. Due to the complexity of its management, treatment strategies are determined through a multidisciplinary approach.
Case Report
A North African 10-year-old female patient presented with rightsided gluteal asymmetry since birth. The condition progressively worsened, with the emergence of a vesicular, bleeding, and painful perianal lesion six months before consultation. The patient experienced significant discomfort, particularly during flare-ups, with recurrent episodes of bleeding triggered by minor mechanical irritation, further impacting her daily activities. The psychological burden extended to her mother, her distress led to an overprotective attitude, limiting her daughter’s outdoor playtime with friends to prevent potential trauma to the lesion. However, the child’s academic performance remained unaffected, with no disruptions in school attendance.
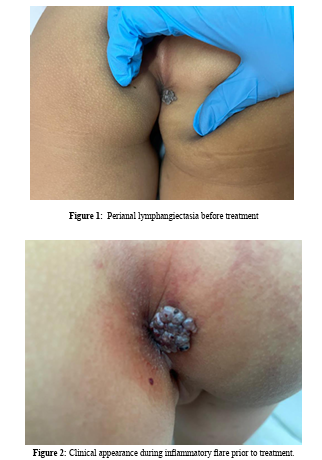
The patient had no significant past medical history and had never undergone any prior interventions or treatments for the lesion. Clinical examination revealed multiple lymphangiectasias overlying a port-wine stain in the right perianal region. The lesions had a characteristic vesicular appearance, with a marked tendency to bleed upon minimal friction (Figure 1 and 2). There were no signs of secondary infection or systemic involvement.
antigen, CA19-9, and CA-125, were within normal limits, ruling out malignant involvement. A biopsy was deferred due to the risk of excessive bleeding and because imaging findings were sufficient for diagnosis. The differential diagnosis included hemorrhagic papillomas, vascular malformations, angiokeratomas, and Klippel- Trénaunay syndrome, which were excluded based on clinical and imaging findings.
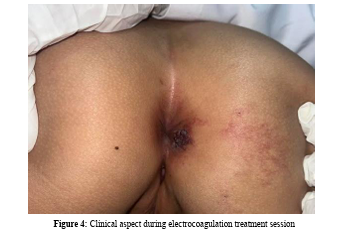
Given the patient’s symptoms and the high risk of recurrent bleeding, electrocoagulation was performed to manage the superficial lymphangiectasias (figure 4), ensuring effective local hemostasis while preserving the infiltrative subcutaneous component of the hemolymphangioma, which remains under clinical surveillance.
Postoperative care included wound monitoring, infection prevention, and pain management. Electrocoagulation was chosen over alternative modalities such as COâ?? laser therapy or sclerotherapy due to its accessibility, and suitability for treating localized superficial lesions.
At the eight-month follow-up, no recurrence of superficial lymphangiectasias was observed, and there was no clinically significant increase in gluteal volume. Initial surveillance consists of clinical evaluations every three months, with an MRI planned at one year of evolution to monitor lesion progression and assess the need for further intervention. No adverse or unexpected events occurred during follow-up.
Discussion
Hemolymphangioma is a rare tumor characterized by developmental anomalies of the lymphatic system associated with vascular malformations. Superficial lymphatic malformations are often visible at birth but may become apparent later, typically within the first two years of life, often triggered by inflammatory episodes or minor trauma [2]. Macrocystic lymphatic malformations manifest as subcutaneous, round masses. These lesions, covered by normal skin. Microcystic components may present as subcutaneous masses beneath normal-colored skin or as lymphangiectasias which are more prone to bleeding upon irritation.
In this case, the hemolymphangioma manifested as a perianal lesion, a rare site for such malformations. To our knowledge, no similar cases have been described in the literature. Common locations for lymphangiectasias include the neck, proximal limbs extending to axillary and inguinal regions, gluteal area, external genitalia, and the tongue [3].
Dermoscopic examination typically reveals pink, red, brown, or violaceous lacunae separated by pale septa. Histologically, hemolymphangioma consists of dense fibrous tissue forming bands between numerous vascular spaces, involving blood or lymphatic vessels, and infiltrating subcutaneous fat [4].
Imaging interpretation must consider clinical findings to aid diagnosis. Ultrasound is crucial for initial assessment, allowing the exclusion of differential diagnoses. MRI remains the preferred modality for evaluating anatomical extension, particularly in cases with deep involvement, and is essential for therapeutic planning.
Macrocystic lymphatic malformations may pose a life-threatening risk due to airway compression in cervicofacial locations and may also cause functional impairments depending on their site.
Treatment is tailored according to the severity, location, and characteristics of the condition [5]. When abstention is not an option, first-line therapy for macrocystic lymphatic malformations is sclerotherapy. The management of microcystic or mixed malformations is more complex, relying on a multidisciplinary therapeutic strategy, which may include sclerotherapy, physiotherapy, surgery, sirolimus, or targeted therapy, either sequentially or in combination [6].
In the present case, electrocoagulation of the superficial lymphangiectasias was performed while preserving the infiltrative subcutaneous component. Other physical modalities, such as CO2 laser or radiofrequency, may be employed but require repeated sessions and provide only temporary relief. These treatments are primarily indicated for cutaneous and mucosal lymphangiectasias, as they effectively reduce lesion size and control bleeding.
This case highlights the complexities of managing perianal hemolymphangiomas, where treatment strategies must be carefully tailored to the lesion’s location and characteristics. The multidisciplinary approach, including electrocoagulation, was chosen as it offered the best balance between efficacy and preservation of the deeper tissue components. Given the absence of significant complications during the follow-up period, this intervention appears effective, although further research and longer follow-up are necessary to confirm its long-term outcomes.
Limitations
The case represents a single-center experience, which restricts the generalizability of the findings. Furthermore, the follow-up period of eight months, while showing promising results, is too short to assess the long-term recurrence and effectiveness of the treatment. A longer follow-up and further clinical trials are needed to refine treatment protocols of this rare condition.
Conclusion
Hemolymphangioma is a congenital vascular malformation. Due to its rarity, only a limited number of cases have been documented in the literature. Imaging modalities, including ultrasound and MRI, play a crucial role in the comprehensive assessment of tumors and the confirmation of diagnosis. Due to its complexity, treatment strategies are established through a multidisciplinary consensus, ensuring individualized care for each patient. This case is notable for the rare localization of the hemolymphangioma, which manifested as a perianal lesion, and it highlights the importance of careful management and the need for a therapeutic approach adapted to the resources available and tailored to the specific needs of each patient. The goal remains to lead to favorable outcomes and improved quality of life for patients.
Declarations
Consent for Publication
Written informed consent was obtained from the patient's legal guardian for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Ethical Approval and Consent to Participate
Ethical approval was not required for this case report. Consent was obtained from the legal guardians of the patient.
Availability of Supporting Data
Not applicable.
Competing Interests
The authors declare that they have no competing interests.
Funding
No funding was received for this study.
Authors’ Contributions
All authors contributed to the clinical diagnosis, management, and decision-making for the patient. They all reviewed and approved the final version of the manuscript.
Acknowledgments
The authors would like to thank the patient and her family for their cooperation.
Informed Consent
Informed consent was obtained from the patient’s mother before initiating any diagnostic and therapeutic procedures. The risks, benefits, and alternatives to electrocoagulation and other treatment options were thoroughly discussed, and the family agreed to proceed with the recommended management plan.
References
- https://www.issva.org/classification
- Li, Y., Pang, X., Yang, H., Gao, C., & Peng, B. (2015). Hemolymphangioma of the waist: A case report and review of the literature. Oncology letters, 9(6), 2629–2632.
- Lerat, J., Bisdorff-Bresson, A., Borsic, M., Chopinet, C., Couloignier, V., Fakhry, N., ... & de travail de la SFORL, G. (2019). Recommandations de la SFORL (version courte) sur les malformations lymphatiques cervicales de l’adulte et de l’enfant: le diagnostic. Annales françaises d'Oto-rhino- laryngologie et de Pathologie Cervico-faciale, 136(2), 110- 114.
- Kosmidis, I., Vlachou, M., Koutroufinis, A., & Filiopoulos, K. (2010). Hemolymphangioma of the lower extremities in children: two case reports. Journal of Orthopaedic Surgery and Research, 5(1), 56.
- Savas, J. A., Ledon, J., Franca, K., Chacon, A., Zaiac, M., & Nouri, K. (2013). Carbon dioxide laser for the treatment of microcystic lymphatic malformations (lymphangioma circumscriptum): a systematic review. Dermatologic surgery, 39(8), 1147-1157.
- Heit, J. J., Do, H. M., Prestigiacomo, C. J., Delgado- Almandoz, J. A., English, J., Gandhi, C. D., ... & Jayaraman, M. V. (2017). Guidelines and parameters: percutaneous sclerotherapy for the treatment of head and neck venous and lymphatic malformations. Journal of neurointerventional surgery, 9(6), 611-617.



